Wyoming Highway Patrol Scanner
Secondary brain cancer is cancer that starts somewhere else in the body and spreads to the brain. It may also be called brainmetastases or secondary brain tumour. It is a type of advanced cancer. Some types of primary cancer are more likely to spread to the brain. The primary cancer is where the cancer first started. These include: lung cancer. The “distant” category is equivalent to stage 4 metastatic cancer. Using the SEER database, statistics show that people with a soft tissue sarcoma have an average 5-year survival rate of 65%. But this differs depending on where the cancer was first found: Localized sarcoma: 81%. Regional: 56%. Distant: 15%. Tumor metastasis into the liver may cause weight loss, nausea, a swollen liver, and abnormal blood tests. Tumor in lymph nodes may cause swelling of the extremities and enlarged glands. Tumor in the lungs may cause shortness of breath, cough, and bloody sputum. Tumor in the brain may cause headaches, dizziness, and seizures. Lung cancer is the number one cause of cancer-related death in the United States, and it is the most common cancer diagnosis behind prostate cancer for men and breast cancer in women. Lung cancer or cancer in general can spread to other parts of the body. This is called metastasis. The brain is one of the most common sites of metastasis.
Research Into Advanced And Metastatic Breast Cancer
As metastatic breast cancer remains the leading cause of death from breast cancer, NBCF is committed to funding a broad spectrum of research that helps to further understand breast cancer metastasis, develop improved treatment options and enhance patient quality of life for those with metastatic breast cancer.
H& O How Has Our Understanding And Management Of Brain Metastases Changed Over The Past5 Years
CA We are seeing advances in both local and systemic therapy. The ability of neurosurgeons to locate and resect brain metastases has improved, and radiation oncology has improved as well. Traditional radiation treatment of brain metastases involved whole-brain radiation therapy, which includes low doses of radiation to the brain over the course of approximately 10 to 15 days. This approach irradiates a large amount of normal brain in addition to the brain metastases, which can lead to a decline in neurocognition and performance status.
More recently, the use of stereotactic radiosurgery has revolutionized the care of patients with brain metastases who have a limited number of lesionsusually no more than four. With stereotactic radiosurgery, the radiation oncologist delivers beams of high-dose radiation to tumors with extreme accuracy over 1 or 2 days, so that the remainder of the brain remains untouched by radiation.
When stereotactic radiotherapy is not possible, another option is whole-brain radiation. Newer strategies spare the hippocampus, the region of the brain that is our seat of memory. We have seen some very promising clinical trial results with hippocampus-sparing whole-brain radiation to preserve neurocognitive function.
Read Also: How Many Deaths From Breast Cancer
Read Also: How To See If You Have Breast Cancer
Inpatient Or Outpatient Status At The Time Of Brain Metastasis Diagnosis
We observed no significant difference based on patient age with respect to inpatient or outpatient status at the time of the brain metastasis diagnosis . When the cohort was stratified by inpatient or outpatient status, survival was significantly longer for outpatients less than 40 years of age than for outpatients 40 or more years of age . No significant difference was observed for inpatients less than 40 years of age and those 40 or more years of age .
Influencing Factors Of Brain Metastasis Free Survival
Univariate analysis showed that clinical stage, molecular subtypes, bone metastases, and lung metastases were significantly associated with BMFS . Patients with TNM stage IV had a shorter BMFS . For patients with stage II or III, their BMFS were not statistically different from that of stage I. Univariate analysis showed shorter BMFS for HER2-positive and triple-negative breast cancers, but multivariate analysis showed that only triple-negative subtypes were independent risk factors for BMFS . In addition, univariate analysis suggested that patients with bone metastases and lung metastases had longer BMFS, but after multivariate analysis, only patients with bone metastases showed significantly longer BMFS than patients without bone metastases .
Table 2. Univariate and multivariate analysis of Brain-metastasis free survival.
Figure 1. Survival curve of BMFS grouped by TNM stage , molecular subtypes , and bone metastasis status . BMFS, brain metastases free survival.
Recommended Reading: Is There Pain With Breast Cancer
Where Do These Numbers Come From
The American Cancer Society relies on information from the SEER* database, maintained by the National Cancer Institute , to provide survival statistics for different types of cancer.
The SEER database tracks 5-year relative survival rates for breast cancer in the United States, based on how far the cancer has spread. The SEER database, however, does not group cancers by AJCC TNM stages . Instead, it groups cancers into localized, regional, and distant stages:
- Localized: There is no sign that the cancer has spread outside of the breast.
- Regional: The cancer has spread outside the breast to nearby structures or lymph nodes.
- Distant: The cancer has spread to distant parts of the body such as the lungs, liver or bones.
Dont Miss: What Is The Treatment For Inflammatory Breast Cancer
Metastasis Patterns And Prognosis Of Octogenarians With Metastatic Breast Cancer: A Large
- Zhenye Lv,
Roles Conceptualization, Methodology, Writing original draft
Affiliation Division of Breast Surgery, Department of General Surgery, Cancer Center, Zhejiang Provincial Peoples Hospital, Affiliated Peoples Hospital, Hangzhou Medical College, Hangzhou, Zhejiang, China
- Wendan Zhang,
Roles Writing review & editing
Affiliation Department of Gynaecology and Obstetrics, The 903 Hospital of the Joint Logistics Support Force of the Chinese Peoples Liberation Army, Hangzhou, Zhejiang, China
- Yingjiao Zhang,
Roles Writing review & editing
Affiliation Department of Gastroenterology, The 903 Hospital of the Joint Logistics Support Force of the Chinese Peoples Liberation Army, Hangzhou, Zhejiang, China
-
Roles Methodology, Software
Affiliation Department of Breast Surgery, College of Medicine, The First Affiliated Hospital, Zhejiang University, Hangzhou, Zhejiang, China
Also Check: Stage 4 Breast Cancer Mammogram
H& o Are We Getting Any Better At Preventing Brain Metastases
CA We do not have any agents that have been shown to prevent brain metastases. As we get better at treating extracranial metastases and preventing breast cancer from entering the lymphatic system, however, the likelihood that breast cancer will reach the central nervous system decreases. We are seeing significant advances in immunotherapy and molecularly targeted therapy in both melanoma and lung cancer, so that holds true for other solid tumors as well.
Is Stage 4 Breast Cancer Curable
Theres currently no cure for stage 4 breast cancer, but with treatments it can be kept under control, often for years at a time.
People with metastatic breast cancer need to receive treatments for the rest of their lives. If a certain treatment stops being effective, another treatment regimen may be tried.
Read Also: Do All Breast Cancer Patients Lose Their Hair
Stage 4 Cancer Life Expectancy
The life expectancy of stage 4 cancer is different depending on the type of cancer. However, there is a 5 years rule, which is the average maximum survivability of stage 4 cancer patients. Within those 5 years, the cancer case could worsen and lead to death. On the other hand, with proper treatment, a patient also can survive more than those 5 years limit.
For example, a breast cancer patient in the last stage will receive a similar diagnosis by using that 5 years limit. However, according to the research, 28% of people can pass through that 5 years limit. Thus, the life expectancy of a breast cancer patient in the late stage is 28%. To help you understand this part, we have already categorized the cancer life expectancy based on the cancer type.
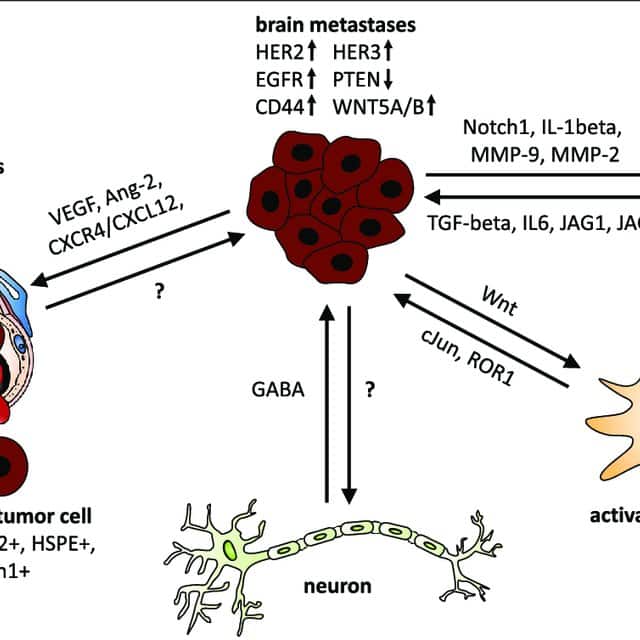
Crosstalk Between Tumor And Brain Microenvironment
Breast cancer cells also adapt to the local microenvironment in the brain and co-opt neurons, astrocytes and microglial cells to proliferate and establish metastases.
Metastatic breast cells have been shown to develop neuronal characteristics, expressing the GABAA receptor, GABA transporter, GABA transaminase, parvalbumin, and reelin, allowing them to take up GABA, shunt it to nicotinamide adenine dinucleotide phosphate production and facilitate proliferation of the tumor cells in the brain microenvironment . Kim et al. showed that murine astrocytes co-cultured in direct cell-to-cell contact with human breast cancer cells caused up-regulation of survival genes in the tumor cells, thus protecting them from the toxic effects of chemotherapy.
Zhang et al. demonstrated that microRNAs from astrocytes cause human and mouse tumor cells with normal expression of PTEN, to downregulate PTEN expression in the brain environment. The loss of this tumor suppressor gene expression allows proliferation of brain metastases. Subsequent blockade of astrocyte secretion restored PTEN and suppressed brain metastasis in vivo. Loss of PTEN is associated TNBC subtype and portends a shorter survival time. Hohensee et al. showed that upregulation of PTEN in a TNBC cell line led to reduced migration and invasion to the brain. Autocrine and paracrine activation of GM-CSF/CSF2RA and AKT/PTEN pathway on both astrocytes and tumor cells mediated this crosstalk.
Also Check: Can Stage 4 Breast Cancer Be Cured
Additional File : Figure S3
Cumulative incidence curves of deaths to show the probability of each competing event in the entire cohort and according to metastatic sites . The real line represents breast cancer-specific mortality and the dotted line represents competing mortality. Cumulative incidence curves of deaths to show the probability of death due to breast cancer according to metastatic sites .
Gm Card Redemption Allowances By Vehicle
Once it spreads, or metastasizes, the disease is known as metastatic melanoma . This type of melanoma may typically occur during stage 3 or stage 4. Common melanoma metastasis sites include the lymph nodes, lungs, liver, bones and brain . About 99,780 adults in the United States will be diagnosed with melanoma> in 2022, according to the American Society of Clinical.
Read Also: Can You Have Breast Cancer At 17
Razorback Basketball Recruiting 2022
Goldberg and colleagues 3 found that pembrolizumab works as well in the central nervous system as in the rest of the body. “We were really encouraged by this,” says Goldberg. “It shows us. Nov 10, 2020 ·Cancer that spreads from where it started to a distant part of the body is called metastatic cancer. For many types of cancer, it is also called stage IV cancer. The process by which cancer cells spread to other parts of the body is called metastasis.
H& o Is The Number Of Women Living With Breast Cancer That Has Metastasized To The Brain Increasing
CA We do not know for certain the answer to that question, although our Brain Metastases Specialty Clinic is working with our partners at the Dana-Farber Cancer Institute to examine how the incidence is changing over time. It is logical that the incidence of brain metastases would increase as patients live longer, thanks to medications that work outside of the brain but are unable to reach the brain. For example, trastuzumab is a big, bulky monoclonal antibody that has a difficult time permeating the blood-brain barrier but does an excellent job treating HER2-positive breast cancer elsewhere in the body.
Recommended Reading: How Do You Know If You Have Breast Cancer
Much Worse Breast Cancer Survival When First Metastasis In Brain
M. Alexander Otto, PA, MMS
This study was published on Research Square as a preprint and has not yet been peer reviewed.
Key Takeaway
-
Patients with HER2-positive breast cancer whose first metastatic event is an isolated brain lesion have worse overall survival than patients with concurrent extracranial disease who develop brain metastases later in their metastatic course.
Why This Matters
-
Current first-line systemic therapies for advanced HER2-positive breast cancer, including pertuzumab and trastuzumab, control metastases outside of the central nervous system, but do not readily cross the bloodbrain barrier and can allow for metastatic escape into the central nervous system.
-
The finding of worse overall survival with isolated brain metastases highlights the need for more agents that are effective against both intracranial and extracranial lesions.
-
The investigators said that clinical trials of HER2-targeted therapies that can cross the bloodbrain barrier, such as the oral tyrosine kinase inhibitor tucatinib , are warranted.
Study Design
Key Results
Limitations
Impact Of Ti On Os After Bm Surgery
There are several acknowledged prognostic markers for postoperative survival after BC BM surgery like the preoperative KPS, BC subtype, age, number of BM and extracranial metastases. As to the possible impact of BM timing on the postoperative course, there are several publications addressing this association, but with conflicting results . Several reasons might underlie this discrepancy such as the differences in baseline characteristics and used TI cutoffs. According to the survival trends in the present cohort, we defined 5 years as the outcome-relevant TI cutoff. Of note, a previous study has already investigated the impact of the 5-year TI on OS in a heterogeneous cohort of BC BM patients, but could not show significant associations .
Don’t Miss: How Serious Is Grade 3 Breast Cancer
Life Expectancy For Brain Metastases
Life expectancy in patients with brain metastases depends upon the variety of factors. It depends upon the stage at which the cancer is diagnosed. It also depends upon the type of primary cancer and its spread in other body parts. The life expectancy also depends upon the number of brain metastatic sites.
The complications related to brain metastases further depends upon the neurological damage due to tumor. Although various treatments are available for the management of brain metastases but none of the treatment completely cure the disease due to various reasons. Chemotherapy is rarely effective due to the fact that most of the chemotherapeutic drugs unable to cross the blood brain barrier at required concentration. Surgery of brain tumor is highly complicated and requires precision. Also, the patient and relative fears with surgery due to significant risk involved. Even if the risk of brain surgery is taken, most of the times the tumor cannot be completely removed due to its inaccessibility.
Survival Rate With Metastatic Breast Cancer
Many people wonder about the life expectancy for stage 4 breast cancer . It’s important to note that everyone is different and survival rates vary widely. There are some people who survive many years and even decades with stage 4 disease. At the same time, it’s important to understand that stage 4 breast cancer isn’t curable.
It can be helpful to look at current statistics and consider the many variables that affect life expectancy. While it’s important not to raise false hope, it may help to know the reality that there are some long-term survivors.
Some people want to know the statistics, but many don’t. If you’re living with stage 4 breast cancer, there is absolutely no requirement that you know the prognosis. The information provided here is only for those who truly wish to know what the current research iseven this research has many limitations.
Also Check: What Percentage Of Breast Cancer Is Metastatic
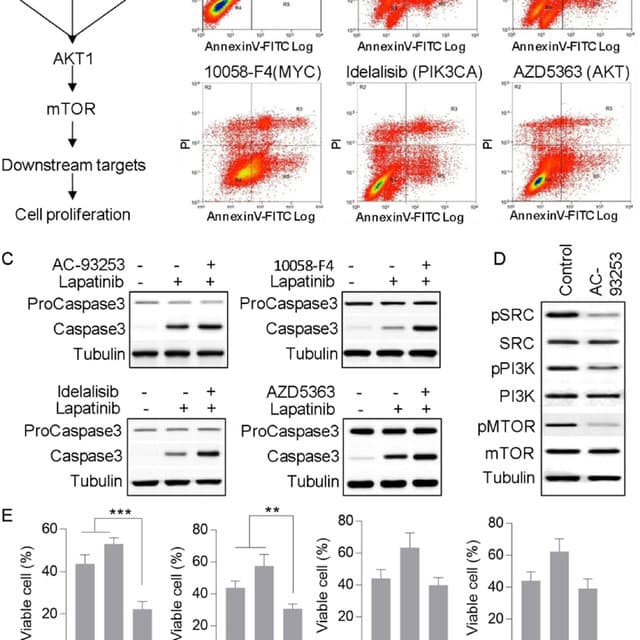
Special/molecular Considerations For Therapy Selection
HER 2 positive breast cancer
Approximately 25% of patients with HER2-positive breast cancer will develop brain metastases. Those with HER2-positive disease have demonstrated a significant survival benefit with the use of systemic anti-HER2 therapy. One proposed mechanism behind the propensity of HER2-positive disease to metastasize to the brain is the inability of trastuzumab to cross the BBB.
HER2-directed therapies for breast cancer can be classified into three subgroups: monoclonal antibodies such as trastuzumab and pertuzumab, small-molecule tyrosine kinase inhibitors such as lapatinib and neratinib, and the antibody-drug conjugate ado-trastuzumab emtansine . The American Society of Clinical Oncology has recommendations on disease management for advanced HER2-positive breast cancer and brain metastases, which we have outlined in Table 1.
Lapatinib with capecitabine is considered a treatment option for progressive brain metastasis and when local therapy has failed, or re-radiation is not feasible, especially when an oral systemic treatment option is preferred. More recently, the TKI neratinib was studied in a phase II trial among 40 patients with HER2-positive breast cancer with brain metastases who had progressed after at least one line of therapy. The intracranial response rates were modest at 8% with this agent.
Metastatic Cancer Life Expectancy
Metastatic cancer life expectancy is an issue for all patients. They are interested to know the survival rate of this cancer because their lives are at stake.
Metastatic Cancer Life Expectancy
Knowing the percentage to survive from this metastatic stage would surely give hopes for patients to strive keeping on.
Metastatic cancer life expectancy breast cancer and ovarian are somewhat among the most critical conditions you should know. The reason is because both cancers are very extreme. Cancerous cells at these diseases have already spread to other parts of the body. Increasing metastatic cancer life expectancy ovarian and breast cancer is surely important.
In our world today, there are lots of diseases that affect the race of human. Metastatic cancer or also known as metastasis is the most dreadful one. This is serious medical condition wherein cancerous cells have already reached to other tissues or organs of the body. For example, metastatic colon cancer may have affected the appendix and other nearby body parts. Having an idea about metastatic cancer life expectancy colon could be very helpful so patients can have the option to take proper treatments.
Recommended Reading: How Many Different Kinds Of Breast Cancer Are There
Brca Mutated Breast Cancer
BRCA mutations, particularly BRCA1, increase the likelihood of developing brain metastases. Up to 5% of patients with breast cancer harbor a germline BRCA mutation. Poly polymerase inhibitors that disrupt DNA repair mechanisms have been developed as an effective therapy in germline BRCA-mutated breast cancers. The OlympiAD and EMBRACA trials for PARP inhibition in patients with germline BRCA mutation demonstrated a significant survival advantage with olaparib and talazoparib, respectively. Olaparib was studied in first or second progression, compared with standard therapy. Median PFS benefit was 2.8 months with a decrease of 42% in disease progression and a more favorable safety profile. Similarly, talazoparib was shown to have a 3-month PFS benefit compared to standard therapy. Another indication for PARP inhibition in most malignancies includes a germline deficiency or somatic loss of function of genes responsible for DNA repair. Repair of both single-strand and double-strand DNA breaks can be blocked using PARP inhibitors, making them particularly useful in those with homologous recombination deficiency.