Is Chemo Necessary Before Or After Surgery
Is Chemotherapy Necessary Before or After Breast Cancer Surgery, or At All? Chemotherapy is an effective way to treat and prevent the spread of breast cancer, but new research suggests it is not always necessary. A recent study found that breast cancer has been highly over treated with chemotherapy and doctors can now confidently provide an
What You Can Expect
- Timing and frequency of chemotherapy sessionsChemotherapy for breast cancer is given in cycles. The cycle for chemotherapy can vary from once a week to once every three weeks. Each treatment session is followed by a period of recovery. Typically, if you have early-stage breast cancer, youll undergo chemotherapy treatmen
- Common drug combinationsThere are many chemotherapy drugs available. Because each person is different, your doctor will tailor the type and dose of medications often a combination of two or three chemotherapy drugs to your type of breast cancer and medical history.
Criteria For Considering Studies For This Review
Types of studies
Randomised controlled clinical trials.
Types of participants
Women with operable breast cancer: TNM stage T1c, T2, T3, N0 to 2, and M0 . We applied no restrictions to age or menopausal status.
TNM classification is the global standard in cancer staging
Types of interventions
Preoperative chemotherapy versus postoperative chemotherapy. Preoperative and postoperative chemotherapy versus postoperative chemotherapy.
See Table 1 for a list of chemotherapeutic agents.
You May Like: How To Determine Breast Cancer
Side Effects Of Radiation Therapy
External beam radiation therapy is a non-invasive treatment with some short term and some longer-term side effects. Patients undergoing some weeks of treatment usually experience fatigue caused by the healthy tissue repairing itself and aside from this there can be no side effects at all. However many breast cancer patients develop a suntan-like change in skin color in the exact area being treated. As with a suntan, this darkening of the skin usually returns to normal in the one to two months after treatment. In some cases permanent changes in color and texture of the skin is experienced. Other side effects sometimes experienced with radiation can include:
- muscle stiffness
- tenderness in the area
After surgery, radiation and other treatments have been completed, many patients notice the affected breast seems smaller or seems to have shrunk. This is basically due to the removal of tissue during the lumpectomy operation.
The use of adjuvant radiation has significant potential effects if the patient has to later undergo breast reconstruction surgery. Fibrosis of chest wall skin from radiation negatively affects skin elasticity and makes tissue expansion techniques difficult. Traditionally most patients are advised to defer immediate breast reconstruction when adjuvant radiation is planned and are most often recommended surgery involving autologous tissue reconstruction rather than breast implants.
Will The Nhs Fund An Unlicensed Medicine
Itâs possible for your doctor to prescribe a medicine outside the uses itâs licensed for if theyâre willing to take personal responsibility for this âoff-licenceâ use of treatment.
Your local clinical commissioning group may need to be involved, as it would have to decide whether to support your doctorâs decision and pay for the medicine from NHS budgets.
Page last reviewed: 28 October 2019 Next review due: 28 October 2022
You May Like: What Chemotherapy Is Used For Metastatic Breast Cancer
For Metastatic Breast Cancer
Chemo can be used as the main treatment for women whose cancer has spread outside the breast and underarm area to distant organs like the liver or lungs. Chemo can be given either when breast cancer is diagnosed or after initial treatments. The length of treatment depends on how well the chemo is working and how well you tolerate it.
Who Is A Good Candidate For Neoadjuvant Therapy
Patients should meet a few requirements to be a candidate for neoadjuvant therapy. The size of the tumor, the type of breast cancer they have, and whether lymph nodes are involved are all things a doctor will consider before suggesting this form of treatment. Some forms of breast cancer are more likely to respond well to neoadjuvant therapy.
Read Also: Where Does Metastatic Breast Cancer Spread To
How Is Chemotherapy For Breast Cancer Given
Chemo drugs for breast cancer are typically given into a vein , either as an injection over a few minutes or as an infusion over a longer period of time. This can be done in a doctors office, infusion center, or in a hospital setting.
Often, a slightly larger and sturdier IV is required in the vein system to administer chemo. These are known as central venous catheters , central venous access devices , or central lines. They are used to put medicines, blood products, nutrients, or fluids right into your blood. They can also be used to take out blood for testing.
There are many different kinds of CVCs. The most common types are the port and the PICC line. For breast cancer patients, the central line is typically placed on the side opposite of the breast cancer. If a woman has breast cancer in both breasts, the central line will most likely be placed on the side that had fewer lymph nodes removed or involved with cancer.
Chemo is given in cycles, followed by a rest period to give you time to recover from the effects of the drugs. Chemo cycles are most often 2 or 3 weeks long. The schedule varies depending on the drugs used. For example, with some drugs, chemo is given only on the first day of the cycle. With others, it is given one day a week for a few weeks or every other week. Then, at the end of the cycle, the chemo schedule repeats to start the next cycle.
What Is Targeted Therapy For Her2
When a cancer is HER2-positive, it means that the cancer cells make too much HER2 protein, which can cause tumors to grow more rapidly than with other forms of breast cancer.
Drugs that target the HER2 proteins are the primary treatment for this type of breast cancer, given along with chemotherapy. Your oncology team may refer to these medications as targeted therapy or HER2-directed therapy.
Trastuzumab and pertuzumab are the most commonly used drugs used to treat HER2-positive breast cancer. Neratinib is another drug that is sometimes given after trastuzumab.
Some other targeted therapy drugs, such as lapatinib or ado-trastuzumab emtansine , are mainly used to treat more advanced HER2-positive breast cancers.
Herceptin and Perjeta are given at the same time as chemotherapy through an IV. HER2-directed therapy is usually given over a longer period of months than chemotherapy.
Herceptin alone is usually continued after chemotherapy has finished, every three weeks for a total of one year.
Side effects for HER2-targeted therapies may include:
- redness at the IV site
You May Like: Does Chemo Make You Lose Your Hair
Also Check: How To Get Checked For Breast Cancer
When Is Chemotherapy Generally Needed
If needed, chemotherapy is most commonly given after surgery for invasive breast cancer. It is a more intense cancer treatment than hormonal therapy. Only a minority of breast cancer patients will ever need chemotherapy. These complex decisions are ones you will make with your medical oncologist and breast surgeon. You will make better treatment choices when you are well informed about chemotherapy before you meet your breast surgeon and medical oncologist. To learn more about chemotherapy, view our short video lesson entitled Will I need chemotherapy?.
Questions For Your Breast Surgeon And Medical Oncologist:
- Do you know now, before surgery, if I will need chemotherapy?
- If yes, should we consider Neoadjuvant Chemo before surgery?
- What are the benefits of Neoadjuvant Chemotherapy?
- Isnt Neoadjuvant Chemo recommended more now?
- Do my receptors suggest I will need chemotherapy?
- Do I have cancer in my axillary nodes?
- Will you ultrasound my axillary lymph nodes today?
Recommended Reading: Does Cheese Cause Breast Cancer
Is Radiation Therapy Safe
Some patients are concerned about the safety of radiation therapy. Radiation has been used successfully to treat patients for more than 100 years. In that time, many advances have been made to ensure that radiation therapy is safe and effective.
Before you begin receiving radiation therapy, your radiation oncology team will carefully tailor your plan to make sure that you receive safe and accurate treatment. Treatment will be carefully planned to focus on the cancer while avoiding healthy organs in the area. Throughout your treatment, members of your team check and re-check your plan. Special computers are also used to monitor and double-check the treatment machines to make sure that the proper treatment is given. If you undergo external beam radiation therapy, you will not be radioactive after treatment ends because the radiation does not stay in your body. However, if you undergo brachytherapy, tiny radioactive sources will be implanted inside your body, in the tumor or in the tissue surrounding the tumor, either temporarily or permanently. Your radiation oncologist will explain any special precautions that you or your family and friends may need to take.
Chemotherapy Before Surgery But I Want My Cancer Gone Part Ii
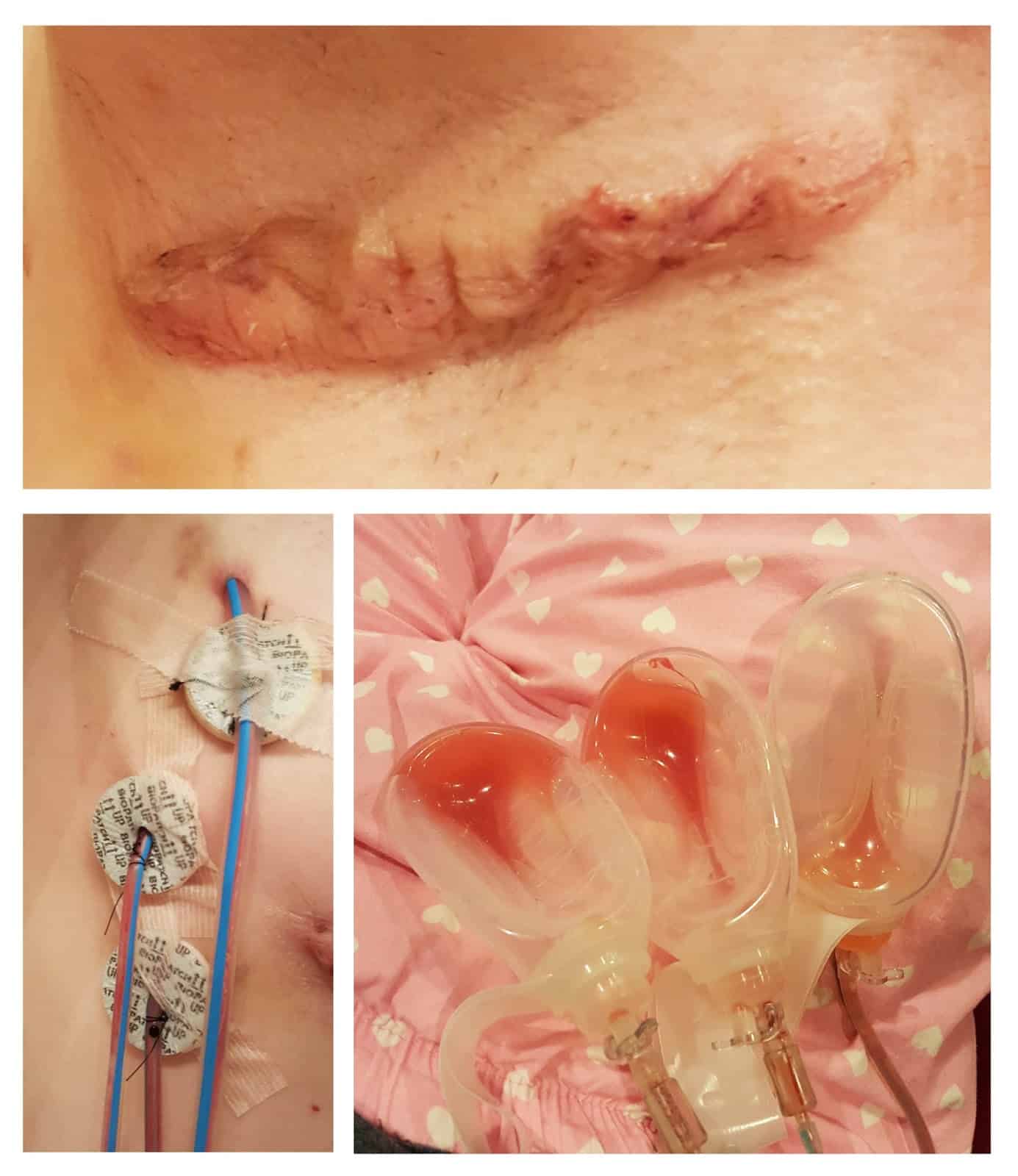
Chemotherapy prior to surgery can tell us whether your tumor responded to chemotherapy. If your tumor is gone after chemotherapy, then we can feel good that any tumor cells hiding elsewhere in your body were killed.
There are 3 chemotherapy agents that are typically administered for breast cancer. Adriamycin , also known as the Red Devil, cyclophosphamide, and Taxol or Taxotere . We refer to these drugs by their initials, A, C or T.
The main regimens we use to kill breast cancer are:
AC Adriamycin and cyclophosphamide once every three weeks for four cycles.
TC Taxotere and cyclophosphamide once every three weeks for four cycles.
AC => T is Adriamycin and cyclophosphamide once every three weeks for four cycles followed by a Taxol every week for 12 weeks.
TAC is Adriamycin, cyclophosphamide, and Taxotere given together once every three weeks for six cycles and is generally an aggressive regimen with more side effects.
ddAC => T is another aggressive regimen, called dose-dense because Adriamycin and cyclophosphamide are given once every two weeks for four cycles followed by Taxol every week for 12 weeks.
But which chemotherapy regimen do we choose for you? Which regimen will give us the best chance of killing the cancer? The biology of the cancer will guide us.
Recommended Reading: Radiation Seeds For Breast Cancer
Summary Of Surgery Timing
Though we donât have a solid answer on how soon surgery should be done after a diagnosis of breast cancer , it would seem earlier surgery is ideal .
Delaying for a lengthy period of time can be dangerous, with studies finding that those who delay over six months are twice as likely to die from the disease. This is important to keep in mind for those who have breast lumps they are âobservingâ without a clear diagnosis. Any breast lump needs to be explained.
Why Doctors Sometimes Recommend Chemo Before A Mastectomy
Why is chemo given before a mastectomy? originally appeared on Quora: the place to gain and share knowledge, empowering people to learn from others and better understand the world.
Answer by David Chan, MD from UCLA, Stanford Oncology Fellowship, on Quora:
There are certain breast cancer situations where treatment is routinely given before surgery. That treatment could be chemotherapy or it could be endocrine therapy.
Typically the sequence of breast cancer treatment doest effect the ultimate outcome with regards to cancer control rate or survival. Doing surgery first doesnt give an advantage in cure rate.
Sometimes chemotherapy is given before mastectomy if the cancer is large and/or if there are significant size and number of lymph nodes already involved. This allows for a better operation if cancer shrinkage is needed to close the skin flaps and also better timing if immediate reconstruction is planned. Getting a breast surgeon and a plastic surgeon and 34 or more hours of operating room time that isnt scheduled quickly, given that the best surgeons are also the ones in greatest demand and usually booked out a number of weeks and even months, could be costly.
Certain kinds of breast cancer usually get chemotherapy before surgery. HER2 positive breast cancers get an immunotherapy with chemotherapy. Triple negative breast cancers usually get chemotherapy before surgery. This statement does not apply if the cancers are small and lymph nodes appear normal.
You May Like: What Does Breast Cancer Feel Like
Saving Karas Breasts And Her Life
During surgery, Dr. Moo didnt find any lingering tumor cells and was able to conserve Kéaras breasts, just as she had hoped. Kéara then completed four weeks of radiation therapy to further make sure the cancer was gone for good. It was the easiest part of her therapy, she says: I was in my car more than in the treatment room!
Celebrating little victories kept her motivated. A dancer since childhood, Kéara marked treatment milestones with the same concept of dancing. It was step-by-step-by-step, she says. We got a good CT scan? We take that win. We learn the cancer isnt in my lymph nodes? We take that win.
Kéara completed active treatment December 2021 and has regular follow-up appointments with her MSK care team. She recently took a trip with her friends to Costa Rica, and shes still running the passion company she founded, KOR Values, which encourages teens and young adults to make positive lifestyle choices. Knowing her selfless spirit, it comes as no surprise that Kéara wants to pay it forward by sharing her story. I havent publicly had the conversation, but this puts it out there, she says. The goal is to help someone else.
It can be hard for many patients to see beyond treatment, says Dr. Moo. But I tell them, Ive taken care of hundreds of people with breast cancer, and I know a year from now youre going to come in smiling and happy.
What Are My Mastectomy Breast Cancer Treatment Options
Some surgeons believe that using chemotherapy to shrink the tumor before surgery is the most effective method. This approach is known as Neoadjuvant Therapy.
Experts suggest that neoadjuvant therapy can not only improve surgical options for breast cancer patients, but it can also allow for a better assessment of the patientâs overall response to chemotherapy. This process can provide the doctors and specialists with more information and help them decide which is the best option for follow-up treatment for the patient after the mastectomy. While the approach may not work for all patients, it is worth discussing neoadjuvant therapy with your doctor to determine if you are a good candidate.
Read Also: Radiation Therapy Side Effects Breast Cancer
Why Do Chemotherapy Before Breast Cancer Surgery
The treatment plan Dr. Moo recommended was different from what Kéara was expecting. At the first institution, she was told she would need surgery, then chemotherapy, then radiation. But at MSK, Dr. Moo told her that having chemotherapy before surgery could shrink the tumor, and as a result, Kéara would probably not need a mastectomy.
We knew based on the type of tumor she had that she would need chemotherapy as a part of her breast cancer treatment, says Dr. Moo. If we used it ahead of surgery, wed be more likely to preserve her breasts.
Chemotherapy given before surgery is known as neoadjuvant chemotherapy. Its an exciting advance in treatment one that MSK is able to offer more and more women with breast cancer these days, Dr. Moo says.
Chemotherapy regimens have been getting better and better, she says. We know that in some cases neoadjuvant chemotherapy can get rid of all of the tumor in the breast and lymph nodes, so when its time for surgery, were not doing as big a procedure.
When Kéara started chemo, she had a remarkable response in just a week or two. After my first treatment, she says, I could no longer feel the lump.
How Does Chemo Work For Breast Cancer
Chemotherapy for Breast Cancer. Chemotherapy uses anti-cancer drugs that may be given intravenously or by mouth. The drugs travel through the bloodstream to reach cancer cells in most parts of the body. Occasionally, chemo may be given directly into the spinal fluid which surrounds the brain and spinal cord.
Recommended Reading: Do Bras Cause Breast Cancer
Sentinel Lymph Node Biopsy
Another way to decide whether cancer is present in the lymph nodes is to perform a sentinel lymph node biopsy. During surgery to remove your cancer, a radioactive tracer and/or a blue dye is injected into the region of the tumor. The surgeon then watches to see which lymph node is the first to receive the dye or tracer as it is carried away from the tumor site by the lymphatic vessels. The surgeon then removes this “sentinel” node. If it is free of cancer, your doctor may not need to remove any other lymph nodes.
This procedure is still quite new, but many doctors believe that it will prove to be as effective as axillary dissection in at least some patients. This could be important because removal of the lymph nodes produces a condition called lymphedema in 10 percent to 20 percent of women with breast cancer. It is hoped that decreasing the amount of surgery performed in the armpit will decrease lymphedema and other side effects.
Surgery To Remove Breast Cancer
There are two main types of surgery to remove breast cancer:
- Breast-conserving surgery is surgery to remove the cancer as well as some surrounding normal tissue. Only the part of the breast containing the cancer is removed. How much breast is removed depends on where and how big the tumor is, as well as other factors. This surgery is also called a lumpectomy, quadrantectomy, partial mastectomy, or segmental mastectomy.
- Mastectomy is a surgery in which the entire breast is removed, including all of the breast tissue and sometimes other nearby tissues. There are several different types of mastectomies. Some women may also have both breasts removed in a double mastectomy.
Also Check: Where Does Breast Cancer Spread To Most Often