How Is Breast Cancer Treated
There are six standard types of treatment for breast cancer: surgery, radiation, chemotherapy, hormone therapy, targeted therapy, and immunotherapy.¹ Your doctor might suggest combinations of these therapies or “adjuvant” therapies, which are used after the primary therapy to help reduce the chances of the cancer coming back. Your doctor may also suggest that you participate in a clinical trial, which is a research study that tests new cancer treatments.
The options for treating men with breast cancer are similar to those for women. A man will typically have surgery followed by hormone therapy, chemotherapy, or radiation.
It is important to mention here that some groups have a harder time accessing breast cancer care than others. Disparities in care negatively affect people who are Black and Latinx, poor, uninsured, LGBTQ+, older, or living in rural areas.²
Is A Preventative Double Mastectomy For Me
A woman newly diagnosed with breast cancer will often say, when discussing her surgical options, Why not just take them both off? These patients often express a desire to never have to worry about my breasts again, particularly those women who have had difficulty with screening procedures in the past or have a history of multiple breast biopsies. Women in whom the primary cancer was initially missed often lose faith in mammography and other screening methods and may feel that the only way to be sure this will not happen to them in the future is to remove both breasts.
Double mastectomies have been featured more in the mainstream media, increasing awareness of this option. Furthermore, the option of immediate reconstruction serves to make this route more appealing than in the past. But what is the real risk of developing a new cancer in the other breast? Do double mastectomies really save lives or improve quality of life? The answer is different for every woman. This article seeks to address these issues and assist individuals in making the most informed decision.
Breast Cancer Survivor 40 Who Got Implants After Double Mastectomy Details Excruciating Three
- Rachel Garlinghouse, 40, from Missouri, has been candid about her experience on TikTok, where she shares topless videos of herself to raise awareness
- The writer was first diagnosed with breast cancer in 2017, and she opted to get a double mastectomy and implants during the same surgery
- Garlinghouse explained in an essay published by Insider that her ‘breast implants looked perfect,’ but she immediately suffered from shoulder pain
- Two years later, she developed a total of 29 other unexplained symptoms, including brain fog, depression, hair loss, purple toes, and digestive issues
- After meeting with ten different doctors who were unable to find out what was wrong with her, she started researching breast implant illness
- Breast implant illness is an unofficial term for the varying health issues that are believed to be caused by breast implants
- Garlinghouse noted that she ‘faced medical gaslighting’ from a few doctors who tried to convince her the symptoms were all in her head
- The mother of four was diagnosed with breast cancer a second time in 2019, and she had both a mass in her chest and her implants removed at the same time
- Garlinghouse, who is now cancer free, credits her explant surgery with her symptoms subsiding, saying she felt better battling cancer than she did before
Read Also: How To Support Breast Cancer
Types Of Mastectomy The Following Types Of Mastectomy May Be Offered
Total mastectomy
A total mastectomy, or simple mastectomy, removes all of the breast and the tissue that covers the chest muscles . The lymph nodes, nerves and muscles in the chest are left in place. The nipple may or may not be removed.
If you plan to have a breast reconstruction, your doctors may try to do a skin-sparing mastectomy when they remove the cancer. A skin-sparing mastectomy is like a total mastectomy except that the surgeon doesnât remove the skin that covers the breast. This approach means that breast reconstruction can be done with very little scarring that can be seen.
Modified radical mastectomy
A modified radical mastectomy removes all of the breast, the nipple, most or all of the lymph nodes in the armpit and the tissue that covers the chest muscles . Nerves and muscles are usually left in place.
This type of mastectomy is used for breast cancer that has spread to lymph nodes. It is also used to treat inflammatory breast cancer.
A radical mastectomy is an operation that removes more muscle, lymph nodes and other tissues than a modified radical mastectomy. It is now very rarely used to treat breast cancer.
You Can Still Live A Long Life
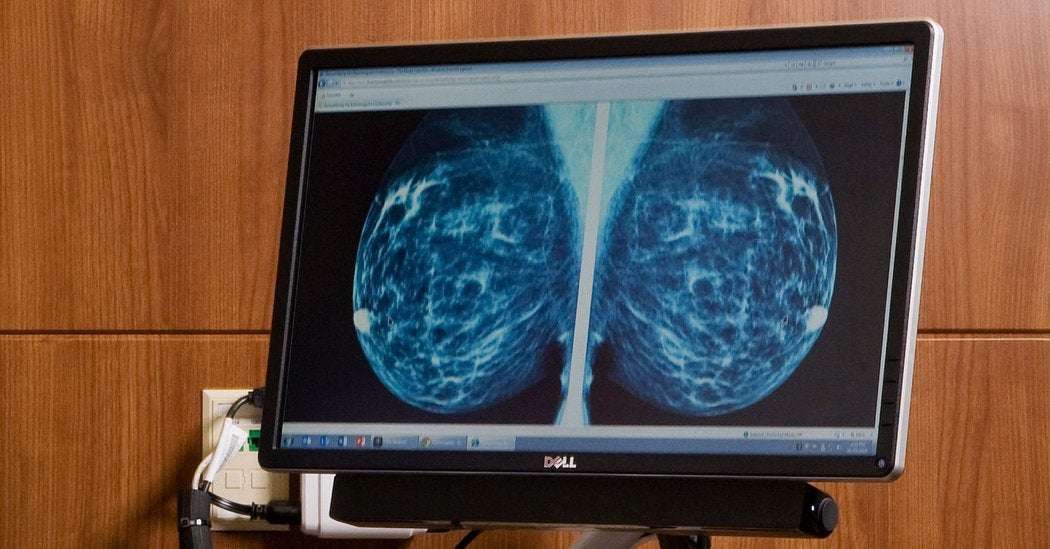
Talk to your doctor about ways to reduce your risk of recurrent or opposite breast cancer. The risks are probably less than you think but completing recommended treatment including radiation following a lumpectomy and any recommended systemic treatment is essential. For more information or two find a breast health provider, click here.
Geisinger Health Plan may refer collectively to Geisinger Health Plan, Geisinger Quality Options Inc., and Geisinger Indemnity Insurance Company, unless otherwise noted. Geisinger Gold Medicare Advantage HMO, PPO, and HMO D-SNP plans are offered by Geisinger Health Plan/Geisinger Indemnity Insurance Company, health plans with a Medicare contract. Continued enrollment in Geisinger Gold depends on annual contract renewal. Geisinger Health Plan Kids and Geisinger Health Plan Family are offered by Geisinger Health Plan in conjunction with the Pennsylvania Department of Human Services . Geisinger Health Plan is part of Geisinger, an integrated health care delivery and coverage organization.
Also Check: How Effective Is Chemotherapy For Breast Cancer
What Can You Expect From Treatment
If it is possible to completely remove the tumor and there are no distant metastases, even recurrent breast cancer can be cured.
The odds of being able to get recurrent breast cancer under control depend on a lot of factors, including the following:
- The size of the tumor
- Whether it is confined to the breast tissue and where in the breast it is located
- Whether the tumor growth is affected by hormones
- Whether the cancer cells have growth factor receptors on them
- How much the cancer cells have mutated
- How many cancerous growths there are
- Whether the cancer cells have spread through the lymph vessels in the skin
- Whether all of the tumor tissue can be removed
- Whether it has already spread to other parts of the body
- How long ago breast cancer was first diagnosed
Talking To Family And Friends About Your Illness
Women who have breast cancer are often concerned about how the disease will affect their relationship with their partner and if they are mothers their children. The stress of treatment often makes sexual needs a lower priority for a while. It can affect your daily routine and require a lot of decisions and planning. All this can give rise to conflicts. It’s important to keep talking to your partner. If you have reached your limits you can get psychological counseling or support, either individually, or as a couple.
Whether children are still very young or already grown up, many mothers find it difficult to talk to their children or grandchildren about their disease. It might stir up memories of the first time they were diagnosed and the same fears may resurface, along with new worries as well. But even if you would rather protect your children from this situation, children do sense when something is wrong. So it is a good idea to speak openly with them about the cancer coming back and about the fact that there may be more treatment to come, and that you may once again need to rest more often.
Recommended Reading: What Tests Detect Breast Cancer
Factors That Affect The Risk Of Breast Cancer Recurrence Following A Mastectomy
Your individual risk for breast cancer recurrence after receiving a mastectomy will depend on several factors, including the type of breast cancer you have and whether it is affected by hormones, the size and location of your tumor, how quickly the cancer cells grew and the stage of cancer at the time of treatment. In particular, if breast cancer has spread to nearby lymph nodes, such as those in the underarm area, the likelihood of recurrence may be higher.
How Do Surgeons Reconstruct The Nipple And Areola
After the chest heals from reconstruction surgery and the position of the breast mound on the chest wall has had time to stabilize, a surgeon can reconstruct the nipple and areola. Usually, the new nipple is created by cutting and moving small pieces of skin from the reconstructed breast to the nipple site and shaping them into a new nipple. A few months after nipple reconstruction, the surgeon can re-create the areola. This is usually done using tattoo ink. However, in some cases, skin grafts may be taken from the groin or abdomen and attached to the breast to create an areola at the time of the nipple reconstruction .
Some women who do not have surgical nipple reconstruction may consider getting a realistic picture of a nipple created on the reconstructed breast from a tattoo artist who specializes in 3-D nipple tattooing.
A mastectomy that preserves a woman’s own nipple and areola, called nipple-sparing mastectomy, may be an option for some women, depending on the size and location of the breast cancer and the shape and size of the breasts .
Don’t Miss: Where Can Breast Cancer Spread To
If Cancer Comes Back In The Same Breast
If the breast cancer comes back in the same breast it’s called local recurrence. The cancer might be picked up at one of your follow up scans or appointments. Or you might notice your breast or scar looks or feels different.
Symptoms of local recurrence can include:
- a small pink or red lump called a nodule on the breast or scar
- change in shape or size of the breast
- a swelling in your arm or hand on the side of your breast surgery
- changes in the shape or position of the nipple
- redness or a rash on the skin on or around the breast area
- a lump or thickening in the breast
Let your doctor know as soon as you can if you notice any changes. You usually have tests to check if the cancer has come back.
Keeping Health Insurance And Copies Of Your Medical Records
Even after treatment is finished, its very important to keep your health insurance. Tests and doctor visits cost a lot, and even though no one wants to think their cancer might come back, this could happen.
At some point after your treatment, you might find yourself seeing a new doctor who doesnt know about your medical history. Its important to keep copies of your medical records so you can give your new doctor the details of your diagnosis and treatment. Learn more in Keeping Copies of Important Medical Records.
Recommended Reading: How Long Can You Live With Inflammatory Breast Cancer
How Can You Cope With Negative Feelings
New fears and disappointment about this setback to your health, anger about the unfairness of your situation or being envious of healthy people are all perfectly natural reactions and are nothing to feel bad about. In the long run, however, it might be better for your general wellbeing to learn how to deal with negative feelings and thoughts so that you still have space for other things as well.
Many women say that it comes as a relief to accept feelings of anxiety, worries and despair and to talk about them with people close to them. As well as talking to your partner, family and friends, professional counseling might also help. Religious organizations and hospitals also offer pastoral or spiritual support. Sharing your experiences with other women in a self-help group is another option.
It can sometimes help to put anxieties and worries aside for a while. Concentrating on pleasant things or activities can help reduce fears and tension to a manageable level.
What Can I Do To Reduce The Chances Of Breast Cancer Recurrence
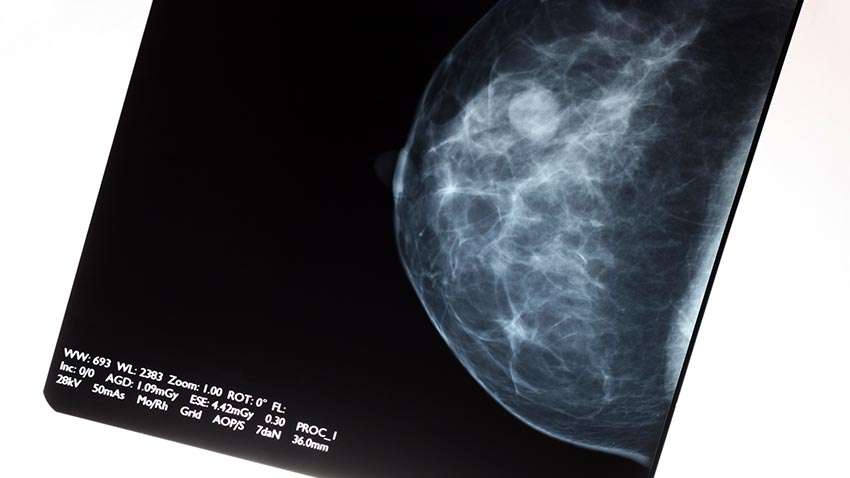
The best thing you can do following your breast cancer treatment is to take care of yourself. Dont smoke, and try to exercise and maintain a healthy diet as best as you can. You should also be sure to follow your schedule for follow-up appointments closely, and continue to perform monthly self-exams on your own. If anything seems out of the ordinary, dont be afraid to consult with your physician. As with other cancers, breast cancer recurrence is best treated when caught early.
In the event you do experience breast cancer recurrence, we invite you to come to the Don & Erika Wallace Comprehensive Breast Program at Moffitt Cancer Center, where our physicians will develop a treatment plan that is tailored to meet the challenges of your unique cancer. Other reasons to come to Moffitt for breast cancer treatment include:
- The unparalleled knowledge and experience of our multispecialty team
- Our robust clinical trials program
- Our supportive care specialists
If you are experiencing breast cancer recurrence after receiving a total mastectomy, you can schedule a consultation to speak with a Moffitt physician by calling or submitting a new patient registration form online.
Read Also: Can Guys Have Breast Cancer
How Long After Breast Cancer Treatment Do Recurrences Occur
The risk of recurrence for all breast cancers was highest in the first five years from the initial cancer diagnosis at 10.4%. This was highest between the first and second years after the initial diagnosis. During the first five years after the initial diagnosis, patients with oestrogen receptor positive breast cancer had lower rates of recurrence compared with those with ER negative disease. However, beyond five years, patients with ER positive disease had higher rates of recurrence.
The late recurrence or relapse of breast cancer refers to cancers that come back after five years, but may not return for 10 years, 20 years, or even more. For people who have estrogen receptor-positive tumours, the cancer is actually more likely to recur after five years than in the first five years.
In contrast to the common belief that surviving for five years after cancer treatment is equivalent to a cure, with hormone-sensitive breast tumours there is a steady rate of recurrence risk for at least 20 years after the original diagnosis, even with very small node-negative tumours.
An awareness of the risk of late recurrence is important for a number of reasons. People are often shocked to learn that their breast cancer has come back after say, 15 years, and loved ones who dont understand this risk are often less likely to be supportive as you cope with the fear of recurrence.
Bone Metastases
- Spine
- Pelvis
- The long bones of the arms and legs
Symptoms and Detection
Treatment
Liver Metastases
Can Breast Cancer Recur After A Mastectomy
A mastectomy is a surgical procedure that removes an entire breast. This procedure may be used as a treatment for breast cancer or a preventative measure for individuals at high risk of developing breast cancer. If your physician has recommended a mastectomy as part of your treatment plan, you may be wondering if this procedure will prevent breast cancer recurrence. Although a mastectomy removes all of the breast tissue, there is still a chance that breast cancer can return.
Read Also: What Percent Of Guys Get Breast Cancer
What Are The Types Of Breast Cancer Recurrence
If you develop cancer in the opposite, untreated breast , you receive a new breast cancer diagnosis. This isnt the same as breast cancer recurrence.
When breast cancer returns, it may be:
- Local: Cancer returns in the same breast or chest area as the original tumor.
- Regional: Cancer comes back near the original tumor, in lymph nodes in the armpit or collarbone area.
- Distant: Breast cancer spreads away from the original tumor to the lungs, bones, brain or other parts of the body. This is metastatic cancer, often referred to as stage 4 breast cancer.
Where Can You Get Support
Coping with a of local or locoregional recurrence, and working through the existential fears and worries that it may trigger, is anything but easy. Starting cancer treatment again can also take a heavy physical and emotional toll. Nowadays, good-quality treatment will also include the option of psycho-oncological counseling. Psycho-oncologists have special training in psychology, medicine and/or social work and are there to support patients and their family and friends in dealing with the illness.
In hospitals, psycho-oncological support is mainly provided by doctors and nurses. They may work together with psycho-oncological services. Psycho-oncological support is also offered as part of rehabilitation. Outpatient psycho-oncological help is available as well.
Various forms of psychotherapy may also be offered to help you if you are experiencing longer-term fears or other negative feelings. You can have therapy or counseling either individually, together with your partner, or in a group with others affected by breast cancer.
In Germany, you are entitled to a variety of services and financial support, including sickness benefit and help with nursing care, as well as home help and childcare. There are a number of places you can go to for advice and help if you want to apply for support. Experts can assist you with personal decisions as well as with financial and legal matters. Individual advice either over the telephone or in person is available from
Read Also: Julia Louis Dreyfus Breast Cancer
Will I Need Chemotherapy After A Total Mastectomy
A total mastectomy is the surgical removal of the entire breast to treat breast cancer. A physician may recommend this treatment on its own or in combination with another therapy, such as chemotherapy. When chemotherapy is provided after surgery, it is called adjuvant chemotherapy. Whether or not chemotherapy is recommended following a total mastectomy will depend on many different factors, including the patients overall health, age and medical history as well as the type, stage and nature of the breast cancer.