Key Points Of Breast Histology After Cnb
There are some key points regarding breast histology on CNB:
Lobular neoplasia or in-situ lobular neoplasia are the preferred terms for core needle biopsy reports the use of atypical lobular hyperplasia or lobular carcinoma in situ are recommended for excision specimens.
Grading of breast cancer on core needle biopsy can be performed and is reasonably accurate. Concordance between grade on CNB and in the definitive excision specimen has been reported to be seen in approximately 75% of cases. However, the grade may differ, usually by one level, from that in the subsequent resection specimen.
Tumors in CNB may be identified according to the most common breast tumor categories ductal or lobular carcinoma.
Assessment of predictivefactors in CNB have been shown to correlate with their expression in subsequent breast excision specimens and include ER, PR and HER2.
Pathologic Complete Response To Neoadjuvant Therapy
Sometimes, the pathologists exam shows no sign of cancer in the breast or axillary lymph nodes. This is called a pathologic complete response and means the neoadjuvant therapy eradicated all of the breast cancer. If you have a pCR, it will be noted on your pathology report.
Although a pCR is encouraging, it doesnt mean the cancer will never return, and many people who dont have a pCR will still do very well.
pCR rates after neoadjuvant chemotherapy are highest among women with tumours that are:
- Hormone receptor-negative
- HER2-positive, when the neoadjuvant treatment plan includes trastuzumab and pertuzumab
The standardized definition of pathological complete response includes residual preinvasive disease/DCIS
The most widely accepted definition of pathologic complete response includes absence of residual invasive disease in the breast and the sampled axillary nodes , but includes residual preinvasive disease/DCIS. Patients who achieve a pCR have lower rates of systemic and local recurrence, and pCR predicts for excellent survival, regardless of subtype.
Tumour Size After Surgery
A pathologist will study the tissue removed during breast cancer surgery and take measurements. Some samples of the tissue may need to be studied under a microscope to check for small amounts of cancer. The largest length of the tumour is the tumour size.
On your pathology report, the post-neoadjuvant treatment tumour size will be indicated with ypT followed by numbers and sometimes, letters. The y notes the measurement was taken after neoadjuvant therapy. The p means a pathologist took the measurement from the tissue removed during surgery.
Sometimes, theres more than one area of cancer in the breast. The largest continuous area will be reported as the tumour size. Youll see the letter m to note there were multiple areas of cancer in the breast.
Also Check: Metastatic Breast Cancer Symptoms And Signs
How Is Tissue Obtained For Examination By A Pathologist
The pathologist examines cells or tissues obtained during a biopsy or surgery or from bodily fluids.
A biopsy specimen can be obtained in several ways, such as by
- taking a tissue sample from the surface of the skin
- using a needle inserted through the skin to withdraw tissue or fluid
- inserting a thin, lighted tube called an endoscope through the mouth, , urethra, or a small incision in the skin to look at areas inside the body and remove a sample using special tools that pass through the tube
If surgery is used to remove part or all of a tumor, some or all of the removed tumor specimen will be examined by the pathologist. If the entire tumor is removed, typically the surgeon will attempt to remove some normal tissue around the tumor for examination by the pathologist to make sure that it doesnt contain tumor cells.
For some cancer types, especially breast cancer and melanoma, the surgeon may also remove nearby lymph nodes, called the sentinel lymph nodes, so the pathologist can see if these contain cancer cells. The Sentinel Lymph Node Biopsy fact sheet describes this procedure and its use in determining the extent, or stage, of cancer in the body.
A pathologist may also examine cells that are present in bodily fluids, such as urine, cerebrospinal fluid , sputum , peritoneal fluid, pleural fluid, cervical/vaginal smears, and bone marrow.
Is It A Cancer
A breast abnormality isnt always cancer. Sometimes, it is simply a collection of normal cells. In other cases, it is made up of cells that fall somewhere between normal and cancerous. These are called atypical cells.
To determine if the abnormality is cancer, the pathologist will look at how the cancer cells grow and travel. Cancer cells grow in an uncontrolled way. They may grow into the tissue nearby or travel to other areas of the body.
You May Like: Nipple Retraction Breast Cancer Staging
Breast Cancer Pathology Report And Lymph Node Specimens
Lymph node metastasis is an important part of cancer Staging and will affect future treatment.
Metastatic tumor clusters in lymph nodes that measure< 0.2 mm are designated as isolatedtumor cells.
Discontinuous clusters of metastatic tumor cells are measured as one focus in a definable part of a lymph node. Unevenly dispersed, clustered tumor cells are characterized by the largest cluster.
What If My Report Says Radial Scar Or Complex Sclerosing Lesion
These findings are benign . If these findings are seen in an excision biopsy, no further action is needed. However, if they are found on a needle biopsy, it isnt so simple. If the lesion is small, entirely removed by the needle biopsy, or unrelated to what was seen on the mammogram, then no further treatment may be needed. However, for lesions that are larger or not entirely removed by the needle biopsy, more tissue from that area may need to be removed because sometimes they are found near something more serious that may need to be treated. You should talk with your doctor about what is best in your case.
Recommended Reading: Can Breast Cancer Start In The Armpit
Ductal Carcinoma In Situ
Ductal carcinoma in situ is concomitantly present in as many as 80% of IBC cases and is associated with increased risk of local recurrence after breast-conserving surgery .
Extensive intraductal component -positive carcinoma is present when DCIS is a major component of the area of invasive carcinoma and also is present outside the area of invasive carcinoma or there is extensive DCIS associated with a small invasive carcinoma .
Extensive intraductal component-positive invasive carcinoma. Ductal carcinoma in situ constitutes 25% of the area of invasive carcinoma and also is present outside the area of invasive carcinoma. A small invasive carcinoma is present in background of extensive DCIS.
The histological features of DCIS associated with increased risk of recurrence are large lesion size, high nuclear grade, certain architectural patterns, central necrosis, and positive surgical margin . It is essential to report the features of DCIS, including nuclear grade, presence of necrosis, and extent of DCIS, in cases of EIC-positive carcinoma .
Nuclear grade is determined according to pleomorphism, nuclear size, chromatin, nucleoli, mitoses, and orientation and is predictive of clinical outcome . Central necrosis is easily detected at low magnification within the central portion of ducts affected by DCIS. Focal necrosis means necrosis in small foci or single-cell necrosis and is indistinct at low magnification.
How Long Do Pathology Results Take
Results usually take between one and two weeks.
Some tests take longer than others and may be done in a different hospital to the one where youre being treated.
Occasionally pathologists get a second opinion about the results which can also delay them.
Your specialist or breast care nurse should be able to tell you when your results will be ready.
Most people feel anxious waiting for their results. How long you wait depends on the type of biopsy or surgery you had and where youre being treated.
Read Also: Lower Back Pain After Chemo For Breast Cancer
Understanding Your Breast Cancer Pathology Report
5 min read
Learning you have been diagnosed with breast cancer can be scary and overwhelming. Suddenly, youre faced with a multitude of doctor appointments and tests, and trying to interpret the results can add extra stress. But knowing how to read pathology reports can give you a better understanding of your cancer and help you feel more in control.
Your Surgeons Operative And History & Physical Notes:
You should also ask for a copy of your surgeons Operative note and History and Physical note. These documents provide an excellent summary of your breast cancer care. Keep for your own health records and share this information with new physicians in the future. You will likely not remember all of the details of your care years later. As time passes, these records are difficult to obtain from retired physicians or cumbersome hospital medical record departments.
This outline What is a Pathology Report? explains why it is important to have copies of your pathology report. The Susan G. Komen organization is a leading advocacy group dedicated to assisting patients, funding research, and ensuring quality breast cancer care.
Review their page Interpreting Your Initial Pathology Report to better understand your breast biopsy report. This site was created for patients by the American Society of Breast Surgeons.
Their page on Your Pathology Report has information about the specifics of tumor type, receptors, and other important information. Living Beyond Breast Cancer is a non-profit organization dedicated to providing quality information about breast cancer to patients.
Teaching everyone to be an expert in their own breast cancer care.
Read Also: What Does Cancer Feel Like In Breast
Lymphatic Or Lymphovascular Space Invasion
Within the breast there is a network of tiny vessels that help circulate fluid and cells that help fight infections and remove waste products. Sometimes cancer cells are seen within these vessels and use these vessels as a mechanism to escape from the breast. If these cells are seen there is an increased risk of more aggressive behaviour by the cancer.
What Other Information Might Be Included On A Surgical Pathology Report

In the comments section of the pathology report, the pathologist may note unusual features of the sample, such as information about the cytogenetic and/or molecular characteristics of a tumor, or provide additional information. The comments section is often used by the pathologist to provide more details about the disease and its diagnosis and to recommend additional tests that might be needed. It may include relevant clinical history or test results, abnormal findings that could change a typical diagnosis, previous samples or diagnoses for the patient, and other possible diagnoses. It will also mention tests that are still in process .
Recommended Reading: Does Breast Cancer Hurt Before Diagnosis
S Of A Pathology Report
Different pathologists may use different words to describe the same findings. Pathology reports from different labs may be organized differently. But most pathology reports include these sections:
This part of a pathology report includes your name, birth date, and the date you had surgery or a blood draw. Make sure all this information is correct. This section also may include a number assigned to you to help keep your identity safe.
This section includes the pathologists and clinicians contact information, as well as the lab where the testing was done.
This part of a pathology report includes details about the tissue sample, which doctors call a specimen. This section includes the date the specimen was removed, the type of biopsy or surgery that was done, and the type of tissue it is. In many cases, tissue will be taken from the breast and/or the lymph nodes. If its suspected that the cancer has spread to parts of the body away from the breast, tissue may come from other areas, such as the liver or bones.
This section includes information about how the cancer was found and may include other information about your medical history.
This part of a pathology report describes what the pathologist can see with their naked eyes before they look at the removed tissue with a microscope. This usually includes:
The final diagnosis usually describes the type of cancer and will likely include information about:
-
anatomic location
Types of invasive carcinoma:
What Is The Microscopic Description On A Surgical Pathology Report
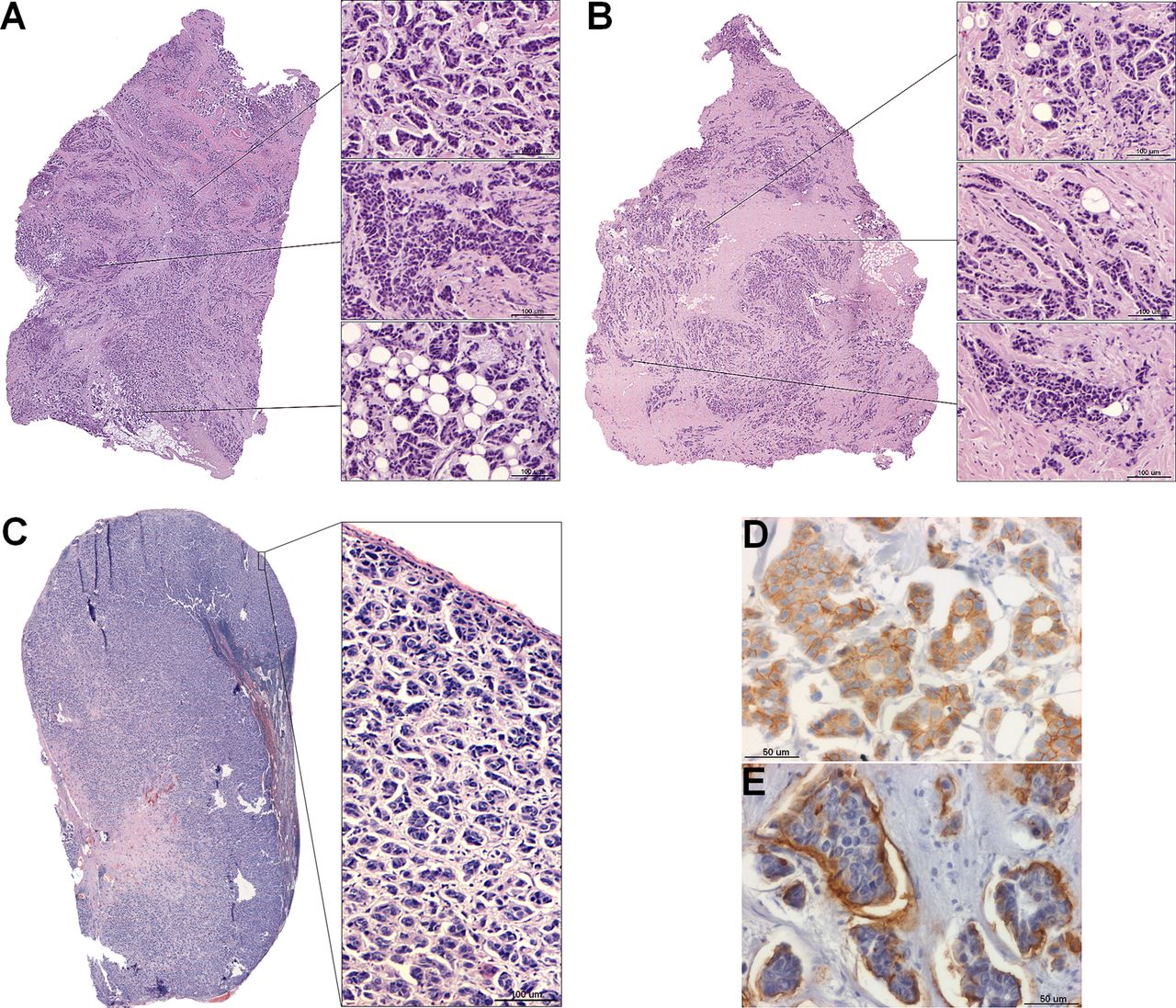
The microscopic description in a pathology report includes information about the appearance of the cells after they have been stained with routine stains such as hematoxylin and eosin and viewed under the microscope. H& E staining helps identify different types of cells and tissues and provides important information about the pattern and shape of cells and the structure of the tissue. With H& E staining, hematoxylin shows the ribosomes, chromatin within the nucleus, and some other structures in the nucleus as a deep blue-purple color. Eosin shows the cytoplasm, collagen, connective tissue, and other structures that surround and support the cell as an orange-pink-red color.
This description may also include the type and number of cells seen in the tissue sample, how abnormal the cells look , and whether there are notable cell features .
The microscopic description section will also indicate whether abnormal cells are found in the or in lymph nodes. Margins are described as negative when the pathologist finds no cancer cells at the edge of the tissue, suggesting that all of the cancer has been removed. A margin is described as positive when the pathologist finds cancer cells at the edge of the tissue, suggesting that some of the cancer has not been removed. Lymph nodes are called positive if they have cancer cells and negative if they do not.
Also Check: What Increases Risk For Breast Cancer
Residual Breast Cancer After Neoadjuvant Therapy
Any breast cancer that remains in the breast or axillary lymph nodes after neoadjuvant therapy is called residual breast cancer. Many people have some residual breast cancer after neoadjuvant therapy. Your pathology report will include whether or not residual breast cancer was found in the breast and/or lymph nodes.
What Happens After The Pathology Report
If you got a breast cancer diagnosis, your doctor will likely refer you to a breast specialist.
âThe breast specialist will be able to put the whole picture together, including a physical exam, the mammogram, the ultrasound, and an MRI to formulate a plan for treatment,â says Stephanie Bernik, MD, chief of breast surgery at Mount Sinai West. âIt varies from person to person more than it did in the past.â
If you have surgeries or biopsies later on, each one will generate a new pathology report.
Show Sources
Don’t Miss: What Is Stage 1 Triple Negative Breast Cancer
What Information Does My Pathology Report Contain
The pathology report contains detailed information about your breast cancer and is essential in helping to guide your treatment. This includes information on the size of the tumour, whether the lymph nodes in the armpit are involved, how aggressive the tumour is and also whether or not the tumour has hormone receptors. These features will help the treating doctors decide on what additional treatment you may or may not need.
What Does It Mean If My Report Mentions Microcalcifications Or Calcifications
Microcalcifications or calcifications are calcium deposits that can be found in both non-cancerous and cancerous breast lesions. They can be seen both on mammograms and under the microscope. Because certain calcifications are found in areas containing cancer, their presence on a mammogram may lead to a biopsy of the area. Then, when the biopsy is done, the pathologist looks at the tissue removed to be sure that it contains calcifications. If the calcifications are there, the doctor knows that the biopsy sampled the correct area .
You May Like: How Do Men Get Breast Cancer
Breast Core Needle Biopsy Specimen
The first report you are likely to encounter is your breast core needle biopsy report. Parts of a breast core needle biopsy pathology report and a breast operative pathology report are very similar, with one important difference: the biopsy pathology report will not have information about the size of the cancer, because a biopsy only removes a small piece of tissue. It should be noted, that although the size of the individual core biopsy specimens will often be listed in the CNB pathology report, that measurement does not reflect the actual size of the breast cancer, which cannot be determined until the whole cancer is removed by surgical excision.
Fine needle aspiration biopsy is a simple, inexpensive, reliable and rapid technique for obtaining cells from a targeted area of breast tissue, whereas a core biopsy involves obtaining single or multiple tissue cores from the breast. Fine needle aspiration removes cells from the tumour which are then examined under a microscope, and the cytology report will confirm whether they are malignant or benign . Fine needle aspiration can be used to establish/support a diagnosis of malignancy, but cytological preparations do not provide a reliable distinction between ductal carcinoma in situ and invasive carcinoma and also generally do not allow for the determination of hormone receptor and HER2 status.
Core biopsy device, needle and sample
What To Ask Your Doctor
When you talk with your doctor to go over your pathology report, you should ask them to clarify anything that you donât understand about the report, your diagnosis, or your treatment plan.
âMany patients come in with their pathology report marked up with circles and highlights because they want to make sure that they understand everything there,â says Lauren Nye, MD, a medical oncologist at the University of Kansas Cancer Center.
You may want to have a friend or family member join the phone call or visit to discuss your pathology report, so you have good support and record of everything discussed. Itâs often hard to take the notes yourself.
You May Like: Can You Get Your Breasts Removed Without Cancer
Other Information In A Report
In some cases, your doctor may order additional tissue testing. Some tissue testing happens after the original pathology report is created. Results from those tests are added to the report later, in an addendum. One example of a test result you may see on an addendum is the Ki-67 proliferation index. Test results for estrogen and progesterone receptors and HER2 also often appear on an addendum.
The Ki-67 proliferation index, also known as MIB-1, reports what percentage of invasive cancer cells are growing or multiplying. Ki-67 is a protein made by cells in the process of reproducing. This makes it a good measure of how many cancer cells are growing and multiplying.
- If the percentage of cancer cells making Ki-67 is low, it means the number of cells reproducing is also low.
- If the percentage of cells making Ki-67 is high, it means the number of cells reproducing is high.
- A percentage over 30 percent is considered to be high. This means that many cells are dividing and the cancer is more aggressive.
Ki-67 is not the same as mitotic rate. The mitotic rate is reported as part of the cancers grade. Not all pathologists perform this test, so you may not see it on your pathology report.