Hypoxia In The Reconstructed Breast
Hypoxia is a process simultaneous with breast reconstruction. Flaps which are supplied solely by their anastomoses have graft borders which are not immediately supplied by native, ingrowing vessels . Implants and expanders exert pressure on the breast boundaries, which decreases microvasculature efficiency, leading to hypoxia . Adipocyte viability based on oxygen diffusion, independent of local HIF pathway activation, reaches 0.2 cm into the grafted tissue from its periphery . In this hypoxic environment, there are multiple aspects which cancer may take advantage of. It is commonly accepted that tumor hypoxia correlates positively with increased invasiveness and metastatic ability . As a baseline, breast cancer biopsies have been shown to contain increased levels of HIF-1, and that the overexpression is connected with increased metastatic risk and mortality . HIF1 expression is directly upstream of L1CAM and angiopoeitin-like 4, which are responsible for lung metastasis of breast adenocarcinoma cells . Using microarrays on biopsy samples from 512 patients, a clear upregulation of HIF-2, as opposed to HIF-1 is present in breast cancer. This offers a specific molecule which the authors propose as a prophylactic target to decrease harmful effects of hypoxia . In terms of extracellular impact, HIF1 hydroxylates and stiffens collagen matrices. Matrix mechanical hardening has been proposed as a histopathologic prognosticator of recurring cancer .
How Do Surgeons Use Implants To Reconstruct A Woman’s Breast
Implants are inserted underneath the skin or chest muscle following the mastectomy.
Implants are usually placed as part of a two-stage procedure.
- In the first stage, the surgeon places a device, called a tissue expander, under the skin that is left after the mastectomy or under the chest muscle . The expander is slowly filled with saline during periodic visits to the doctor after surgery.
- In the second stage, after the chest tissue has relaxed and healed enough, the expander is removed and replaced with an implant. The chest tissue is usually ready for the implant 2 to 6 months after mastectomy.
In some cases, the implant can be placed in the breast during the same surgery as the mastectomythat is, a tissue expander is not used to prepare for the implant .
Surgeons are increasingly using material called acellular dermal matrix as a kind of scaffold or sling to support tissue expanders and implants. Acellular dermal matrix is a kind of mesh that is made from donated human or pig skin that has been sterilized and processed to remove all cells to eliminate the risks of rejection and infection.
Locally Advanced Breast Cancer
If breast cancer has spread to the chest wall or skin of the breast, or the lymph nodes around the chest, neck and under the breast bone, but has not spread to other areas of the body, its called locally advanced breast cancer. Sometimes breast cancer is locally advanced when it is first diagnosed.
People who have locally advanced breast cancer are thought to have an increased risk of cancer cells spreading to other areas of the body, compared to those with stage 1 or 2 breast cancers.
Also Check: Can You Get Breast Implants After Having Breast Cancer
Fears Of Cancer Recurrence Affecting Decisions
According to recent studies, women with breast cancer have been increasingly choosing to have this aggressive surgery because they are worried about recurrence. About three-quarters of patients reported being very worried about their cancer recurring.
But a diagnosis of cancer in one breast does not increase the likelihood of cancer recurring in the other breast for most women, according to the researchers.
Lead study author Sarah Hawley, Ph.D., associate professor of internal medicine at the University of Michigan Medical School, said in a press statement that women appear to be using worry over cancer recurrence to choose contralateral prophylactic mastectomy, This does not make sense, because having a non-affected breast removed will not reduce the risk of recurrence in the affected breast, said Hawley.
The study also found that women with higher education levels and women who had undergone an MRI test before surgery were more likely to choose double mastectomy. Concern about recurrence was one of the biggest factors driving the decision to have this surgery.
How Is A Local Recurrence After Lumpectomy Diagnosed
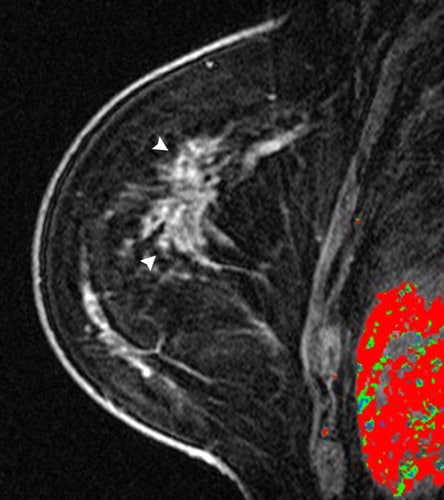
After a diagnosis of early stage breast cancer, any remaining breast tissue should be evaluated annually with scans .
Most local recurrences within the breast after lumpectomy are detected on routine annual breast imaging, which usually takes the form of mammography and ultrasound, and on occasions MRI.
If you have a local recurrence or new primary breast cancer, you may find symptoms similar to an initial breast cancer. This includes:
- A new lump in the breast, armpit area or around the collarbone
- A change in breast size or shape
- Changes to the nipple, such as sores or crusting, an ulcer or inverted nipple
- Clear or bloody nipple discharge
- Changes to the skin including redness, puckering or dimpling
- Breast tenderness or pain
Once a local recurrence has been diagnosed, we do tests to see whether there are signs of cancer elsewhere in the body. These may include a chest X-ray, CT scan, bone scan or PET scan, and blood tests , then we have to figure out how best to treat the tumour in the breast. Usually in these cases we do a mastectomy, as the prior less drastic surgery and radiation didnt take care of it.
Read Also: What Month Is Breast Cancer Awareness Month
Request An Appointment At Moffitt Cancer Center
Please call for support from a Moffitt representative. New Patients and Healthcare Professionals can submit an online form by selecting the appropriate button below. Existing patients can call . for a current list of insurances accepted at Moffitt.
NEW PATIENTS To request a new patient appointment, please fill out the online form or call 1-888-663-3488.
REFERRING PHYSICIANS Providers and medical staff can refer patients by submitting our online referral form.
Moffit now offers Virtual Visits for patients. If you are eligible for a virtual appointment, our scheduling team will discuss this option further with you.
Moffitt Cancer Center is committed to the health and safety of our patients and their families. For more information on how were protecting our new and existing patients, visit our COVID-19 Info Hub
How Common Is Breast Cancer Recurrence
Most local recurrences of breast cancer occur within five years of a lumpectomy. You can lower your risk by getting radiation therapy afterward. You have a 3% to 15% chance of breast cancer recurrence within 10 years with this combined treatment. Based on genetic testing, your provider may recommend additional treatments to further reduce your risk.
Recurrence rates for people who have mastectomies vary:
- There is a 6% chance of cancer returning within five years if the healthcare providers didnt find cancer in axillary lymph nodes during the original surgery.
- There is a one in four chance of cancer recurrence if axillary lymph nodes are cancerous. This risk drops to 6% if you get radiation therapy after the mastectomy.
You May Like: Breast Cancer Treatment When Lymphovascular Invasion Is Present
What Type Of Follow
Any type of reconstruction increases the number of side effects a woman may experience compared with those after a mastectomy alone. A womans medical team will watch her closely for complications, some of which can occur months or even years after surgery .
Women who have either autologous tissue or implant-based reconstruction may benefit from physical therapy to improve or maintain shoulder range of motion or help them recover from weakness experienced at the site from which the donor tissue was taken, such as abdominal weakness . A physical therapist can help a woman use exercises to regain strength, adjust to new physical limitations, and figure out the safest ways to perform everyday activities.
Dermal Reservoir Of Cancer Cells
The skin has been quoted as an immune privilege area, in ways not dissimilar to the brain. Hair follicle Antigen Presenting Cells lack MHCII. Potent immunosuppressive factors like TGFB1 and a-melanocyte stimulating hormone are present in the dermis . These factors create an environment which provides shelter for cancer cells during treatment . A separate aspect inherent to preserving skin margins , is also the potential remaining breast tissue adherent to the hypodermis, allowing cancerous breast tissue to remain unintentionally .
Don’t Miss: What Stage Is Grade 3 Breast Cancer
Breast Cancer Recurrence After Mastectomy
Breast cancer is one of the most common cancers among women nowadays. Many female patients that have been diagnosed with breast cancer decide to get a mastectomy. But what happens after the mastectomy can the breast cancer return? Here well discuss some important must-knows about breast cancer and mastectomies.
Symptoms Of Local Breast Cancer Recurrence
Local recurrence could cause one or more of the following symptoms:
- Dimpling of the skin in the breast.
- Pain in the shoulder, upper arm, or chest area.
- Breast lump or thickening.
- Nipple discharge
- Loss of milk production.
In some cases, cancer has spread to other parts of the body. In this case, breast lump or swelling occurs on one side while the other is normal. Once you discover the symptoms, get the opinion of the top oncologist in India at Medicover Hospital Vizag.
Also Check: Is Zinc Good For Breast Cancer
What Is Breast Reconstruction
Many women who have a mastectomysurgery to remove an entire breast to treat or prevent breast cancerhave the option of having the shape of the removed breast rebuilt.
Women who choose to have their breasts rebuilt have several options for how it can be done. Breasts can be rebuilt using implants . They can also be rebuilt using autologous tissue . Sometimes both implants and autologous tissue are used to rebuild the breast.
Surgery to reconstruct the breasts can be done at the time of the mastectomy or it can be done after the mastectomy incisions have healed and breast cancer therapy has been completed . Delayed reconstruction can happen months or even years after the mastectomy.
In a final stage of breast reconstruction, a nipple and areola may be re-created on the reconstructed breast, if these were not preserved during the mastectomy.
Sometimes breast reconstruction surgery includes surgery on the other, or contralateral, breast so that the two breasts will match in size and shape.
Risk Factors For Distant Recurrence
There are several risk factors that raise the risk of recurrence overall . These include:
- Tumour size: Larger tumours are more likely to recur than smaller ones both early and late.
- Positive lymph nodes: Tumours that have spread to lymph nodes are more likely to recur at any time than those that have not.
- Age at diagnosis: Breast cancer recurrence is more common in younger women.
- Treatments received and response to treatments: Both chemotherapy and hormonal therapy reduce the risk of recurrence
- Tumour Characteristics: More aggressive cancers are more likely to recur than less aggressive tumours , especially in the first five years. We also take into account the receptor status and an estimate of proliferation .
There are also factors that do not appear to affect the risk of recurrence. Recurrence rates are the same for women who have a mastectomy or lumpectomy with radiation and are also the same for women who have a single vs. double mastectomy.
You May Like: Treating Triple Negative Breast Cancer
Risk Factors For And Patient Outcomes After Local Recurrence
On univariate Cox regression analysis, the risk factors for local recurrence following implant-based breast reconstruction were lymphatic vessel invasion and positive or< 2 mm vertical margin . Multivariate Cox regression analysis also showed lymphatic vessel invasion and positive or< 2 mm vertical margin to be significant independent risk factors for local recurrence .
Table 3 Risk factors for local recurrence by Cox proportional hazard regression analysis
The 5-year local recurrence free survival rate for the entire patient population was 97.5% . The median local recurrence free survival of the 12 patients with local recurrence was 27.5 months . There was no significant difference in OS between patients with versus without local recurrence .
Fig. 3
a Local recurrence free survival rate for the entire patient population. b Overall survival rate according to with or without local recurrence
Symptoms Elsewhere In The Body
Sometimes breast cancer cells can spread from the breast to other parts of the body. This is known as secondary breast cancer.
Some symptoms to be aware of include:
- unexpected weight loss and a loss of appetite
- severe or ongoing headaches
Find out more about the symptoms of secondary breast cancer.
You May Like: How Does Chemotherapy Work For Breast Cancer
Surgical Adjustments And Complications After Reconstruction
Ipsilateral adjustment surgery after DIEP flap reconstruction was performed in 175 patients procedures per patient). This included shaping of the breast, liposuction, lipofilling and scar revision. Contralateral surgery was performed in 147 patients procedures per patient), including mastopexy, breast reduction, implant-based augmentation, implant replacement or capsulectomy. Nipple reconstruction was undertaken in 212 patients and flap revision owing to suspected surgical complications in 22 . Partial or total flap necrosis occurred in 16 and two patients respectively. Complications after DIEP flap reconstruction did not have a signficant effect on DFS, BCSS or OS rates.
How Do Surgeons Use Tissue From A Womans Own Body To Reconstruct The Breast
In autologous tissue reconstruction, a piece of tissue containing skin, fat, blood vessels, and sometimes muscle is taken from elsewhere in a womans body and used to rebuild the breast. This piece of tissue is called a flap.
Different sites in the body can provide flaps for breast reconstruction. Flaps used for breast reconstruction most often come from the abdomen or back. However, they can also be taken from the thigh or buttocks.
Depending on their source, flaps can be pedicled or free.
- With a pedicled flap, the tissue and attached blood vessels are moved together through the body to the breast area. Because the blood supply to the tissue used for reconstruction is left intact, blood vessels do not need to be reconnected once the tissue is moved.
- With free flaps, the tissue is cut free from its blood supply. It must be attached to new blood vessels in the breast area, using a technique called microsurgery. This gives the reconstructed breast a blood supply.
Abdominal and back flaps include:
Flaps taken from the thigh or buttocks are used for women who have had previous major abdominal surgery or who dont have enough abdominal tissue to reconstruct a breast. These types of flaps are free flaps. With these flaps an implant is often used as well to provide sufficient breast volume.
Recommended Reading: Can Asbestos Cause Breast Cancer
Recommended Reading: Where Is Breast Cancer Usually Located
Does Breast Reconstruction Affect The Ability To Check For Breast Cancer Recurrence
Studies have shown that breast reconstruction does not increase the chances of breast cancer coming back or make it harder to check for recurrence with mammography .
Women who have one breast removed by mastectomy will still have mammograms of the other breast. Women who have had a skin-sparing mastectomy or who are at high risk of breast cancer recurrence may have mammograms of the reconstructed breast if it was reconstructed using autologous tissue. However, mammograms are generally not performed on breasts that are reconstructed with an implant after mastectomy.
A woman with a breast implant should tell the radiology technician about her implant before she has a mammogram. Special procedures may be necessary to improve the accuracy of the mammogram and to avoid damaging the implant.
More information about mammograms can be found in the NCI fact sheet Mammograms.
Imaging Surveillance Of The Reconstructed Breast In A Subset Of Patients May Aid In Early Detection Of Breast Cancer Recurrence
- Received:
How to cite this article: Adrada BE, Karbasian N, Huang M, Rauch GM, Woodtichartpreecha P, Whitman G. Imaging surveillance of the reconstructed breast in a subset of patients may aid in early detection of breast cancer recurrence. J Clin Imaging Sci 2021 11:58.
Read Also: Stage 2 Er Positive Breast Cancer
Recovery From Breast Reconstruction Surgery
You may have some discomfort for the first few days afterward. Youll get pain medication as needed. Throughout your hospital stay, the staff will closely watch you.
Soon after surgery, youll be encouraged to move your arms, but not for any forceful activity like pulling yourself up, getting out of bed, or lifting heavy objects. Nurses will help you in and out of bed. The day after surgery, you may be able to sit in a chair beside the bed. On the second day, most patients are walking without help.
Youll probably get IV fluids for a day or two. You may have a urinary catheter overnight or until you can walk to the bathroom. And where the surgeon made cuts , youll have drains. If you go home with these drains in place, youll get instructions on how to care for them.
The length of your hospital stay depends on the type of operation and how your recovery goes. If you got implants, the average hospital stay is 1 to 2 days. Flap procedures may require a stay of 5 to 6 days.
What Can I Do To Reduce The Chances Of Breast Cancer Recurrence
The best thing you can do following your breast cancer treatment is to take care of yourself. Dont smoke, and try to exercise and maintain a healthy diet as best as you can. You should also be sure to follow your schedule for follow-up appointments closely, and continue to perform monthly self-exams on your own. If anything seems out of the ordinary, dont be afraid to consult with your physician. As with other cancers, breast cancer recurrence is best treated when caught early.
In the event you do experience breast cancer recurrence, we invite you to come to the Don & Erika Wallace Comprehensive Breast Program at Moffitt Cancer Center, where our physicians will develop a treatment plan that is tailored to meet the challenges of your unique cancer. Other reasons to come to Moffitt for breast cancer treatment include:
- The unparalleled knowledge and experience of our multispecialty team
- Our robust clinical trials program
- Our supportive care specialists
If you are experiencing breast cancer recurrence after receiving a total mastectomy, you can schedule a consultation to speak with a Moffitt physician by calling or submitting a new patient registration form online.
Also Check: Does Breast Cancer Cause Bruising