The Emotional Aspects Of Risk
Every women reacts differently to the idea of risk-reducing surgery. It is a big decision to have your breasts and/or your ovaries and fallopian tubes removed to reduce the risk of cancer.
Some women who carry a gene fault have seen lots of women in the family die of breast or ovarian cancer and feel they would like to do whatever they can to minimise their own risk.
Others feel that the thought of losing their breasts is worse than the thought of developing cancer. These women may prefer to take medication to reduce the risk of cancer or to have close monitoring.
Some women find a combination of both approaches suitable, for example having surgery to remove their ovaries and fallopian tubes, but close monitoring of their breasts.
All of these approaches are perfectly reasonable. It is important that you make a decision you feel comfortable with.
Remember, you can take all the time you need to get information and consider the choices available to you. You may reconsider and have the surgery in a few years if it doesnt feel right for you now.
Familial Atypical Multiple Mole Melanoma Syndrome
FAMMM is a syndrome that increases your risk of developing melanoma skin cancer. People with FAMMM tend to have large numbers of moles or moles that are unusual. They also have at least one close relative with a diagnosis of melanoma. A close relative is a parent, brother or sister, or child.
Scientists think that FAMMM is linked to a fault in the CDKN2A gene. It may also increase your risk of developing pancreatic cancer. But doctors need more research to find out for sure.
You May Like: What Does Invasive Breast Cancer Mean
Ovarian Cancer Treatment Options
Typically, treatment for ovarian cancer involves surgery to remove the tumor or tumors, and chemotherapy to kill remaining cancer cells. Additional therapies may include Avastin , which starves the tumor of its blood supply, and PARP inhibitors, a type of targeted therapy that may improve survival rates.
Women diagnosed with mutations prior to the onset of cancer can undergo procedures to lower their risk, Dr. Zaid says.
Some women at very strong risk undergo preventive surgery to help avoid future cancers, Dr. Arentz explains. For example, a preventive mastectomy may lower future breast cancer risk as much as 90%. Oophorectomy may reduce ovarian cancer risk as much as 80-90% in women with a BRCA mutation.
Read Also: Is Breast Cancer Curable
Epidemiology And Risk Factors
Epithelial ovarian cancer is the leading cause of death among the gynecologic cancers and the fourth leading cause of cancer death in women in the United States . Incidence rates vary considerably but are highest in industrialized countries with the exception of Japan. Ovarian cancer is one-tenth as common as breast cancer but three times as lethal. The high mortality rate is generally attributed to its occult development, resulting in advanced, widespread disease occurring in approximately 75% of women at diagnosis. The overall 5-year survival rate of ovarian cancer is about 30%. However, in about 25% of women, disease is confined to the ovary , and 5-year survival is more than 90%, compared with 10% for women with advanced disease . The incidence of epithelial ovarian cancer is age related and is generally a disease of postmenopausal women. Malignant epithelial tumors are most common between the ages of 40 and 60 years.
Having A Family History Of Ovarian Cancer Breast Cancer Or Colorectal Cancer
Ovarian cancer can run in families. Yourovarian cancer risk is increased if your mother, sister, or daughter has ovarian cancer. The risk also gets higher the more relatives you have with ovarian cancer. Increased risk for ovarian cancer can also come from your father’s side.
A family history of some other types of cancer such as colorectal and breast cancer is linked to an increased risk of ovarian cancer. This is because these cancers can be caused by an inherited mutation in certain genes that cause a family cancer syndrome that increases the risk of ovarian cancer.
Recommended Reading: 2cm Breast Cancer
Breast Cancer And Ovarian Cancer: Understanding The Connection
Ovarian cancer and breast cancer share some risk factors. This means that some people have a higher risk of developing both types of cancer. In some cases, these risk factors can be controlled, allowing a person with ovarian cancer to lower their chances of developing breast cancer. People who have a very high risk of breast cancer may also be able to use medication, surgery, and screening tests to reduce the risk or catch cancer early.
Inherited Genes And Cancer Types
-
Most cancers are not linked to inherited faulty genes.
-
If you have an inherited faulty gene it increases your risk of developing certain types of cancer.
-
Some faulty genes increase the risk of more than one cancer type.
-
Faulty BRCA1 and BRCA2 genes increase the risk of developing breast, ovarian, pancreatic and prostate cancer.
Most cancers are not linked to inherited faulty genes . Only around 5 in every 100 cancers diagnosed are linked to an inherited faulty gene.
This information is aboutsome of the inherited faulty genes that can increase your risk of developing cancer. Faulty genes are also called gene mutations.
Its important to remember that these conditions are rare. Most cancers develop because of a combination of chance and our environment, not because we have inherited a cancer gene fault. Talk to your GP if you have a strong family history of cancer. Or if you think you could have inherited any of these faulty genes.
Don’t Miss: Side Effects Of Hormone Blockers For Breast Cancer
Leaving The Primary Tumor: The First Step To Successful Ovarian Cancer Metastasis
Serous ovarian carcinoma metastasis. Normal human peritoneum . A: H& E staining. MC , Fib . B: Trichrome staining to detect collagen. C: Photograph of peritoneal surface implants in a patient with disseminated ovarian carcinoma on a background of normal peritoneum . D: Implant in C. E: Peritoneal implant with neoangiogenesis. Other smaller implants in the background . F: H& E picture of normal omentum. G: Very early serous ovarian carcinoma metastasis on the omentum. Cancer cells proliferating on the surface of f the omentum without invading. H: Later phase: cancer cells invading into the omentum.
Genetic Testing And Ovarian Cancer
Just 3 percent of people with breast cancer have inherited mutations in BRCA genes. This means that most people diagnosed with breast cancer dont have a gene change that puts them at risk for ovarian cancer. However, you may be more likely to have one of these inherited mutations if you were diagnosed with breast cancer before the age of 50, developed breast cancer in both breasts, or have multiple family members including male family members who were diagnosed with breast cancer.
If your doctor thinks you may have a genetic mutation that leads to a higher risk of cancer, they may recommend genetic counseling and genetic testing. In this case, you will meet with a genetic counselor to talk about your cancer risk, and you may undergo tests that help determine whether you have certain gene changes. These tests are very simple and involve either a blood or saliva test. When one person within a family finds out they have an inherited gene change, other family members should be informed and may also want to be tested to determine their risk levels.
You May Like: Stage 3 A Cancer
Talking About Family Health History With Your Health Care Provider
Your family history of breast cancer and other health conditions is important to discuss with your health care provider. This information helps them understand your risk of breast cancer.
|
Susan G. Komen®s My Family Health History Tool |
|
My Family Health History tool is a web-based tool that makes it easy for you to record and organize your family health history. It can help you gather information thats useful as you talk with your doctor or genetic counselor. |
Dont Miss: What Organs Are Affected By Breast Cancer
Personal History Of Breast Cancer
If you have already had breast cancer, you might have a greater chance of also developing ovarian cancer. Some of the same risk factors that can impact ovarian cancer can affect breast cancer. That might include the age you first started your period, and if and when you started menopause. Any pregnancies and fertility treatments could also make a difference.
The good news is that even with family risk factors like breast cancer, the chance of developing ovarian cancer is still small. It is rarer than breast cancer. Most women with a family or personal history of ovarian or breast cancer will never get the disease.
Make sure to tell your doctor if you or a family member have a history of breast cancer. You can work together to prevent breast and ovarian cancer if you have an increased genetic risk.
Show Sources
Recommended Reading: Mbc Metastatic Breast Cancer
Inherited Genetic Changes In Breast And Ovarian Cancer
Breast and ovarian cancer can both be caused by some of the same inherited gene mutations. Many of these cancers are caused by changes in the BRCA1 or BRCA2 genes. In normal cells, these genes allow the cell to fix damage, preventing them from turning cancerous. When cells have mutated BRCA genes, DNA damage cannot easily be fixed, so they are more likely to start growing abnormally.
Inherited gene changes are present at birth, and they can be found in every cell within the body. When a person has inherited BRCA mutations, doctors refer to the condition as hereditary breast and ovarian cancer syndrome.
Changes in BRCA1 or BRCA2 can increase the risk of both breast and ovarian cancers:
- About 1.6 percent of women without BRCA mutations develop ovarian cancer at some point in their lives.
- Women with BRCA1 mutations have a 40 percent to 60 percent chance of being diagnosed with ovarian cancer. Those with BRCA2 mutations have a 20 percent to 35 percent lifetime risk.
- Around 13 percent of women without BRCA mutations are diagnosed with breast cancer.
- BRCA1 mutations lead to a 55 percent to 72 percent risk of developing breast cancer. The lifetime risk for women with BRCA2 mutations is 45 percent to 69 percent.
BRCA mutations, and in particular mutations in BRCA1, are more likely to lead to triple-negative breast cancer. Triple-negative breast cancer is an aggressive type of breast cancer that often comes with a poor outlook.
Risk Factors You Can Change

- Not being physically active. Women who are not physically active have a higher risk of getting breast cancer.
- Being overweight or obese after menopause. Older women who are overweight or obese have a higher risk of getting breast cancer than those at a normal weight.
- Taking hormones. Some forms of hormone replacement therapy taken during menopause can raise risk for breast cancer when taken for more than five years. Certain oral contraceptives also have been found to raise breast cancer risk.
- Reproductive history. Having the first pregnancy after age 30, not breastfeeding, and never having a full-term pregnancy can raise breast cancer risk.
- Drinking alcohol. Studies show that a womans risk for breast cancer increases with the more alcohol she drinks.
Research suggests that other factors such as smoking, being exposed to chemicals that can cause cancer, and changes in other hormones due to night shift working also may increase breast cancer risk.
Read Also: What Happens If You Get Hit In The Breast
Second Cancers After Breast Cancer
Breast cancer survivors can be affected by a number of health problems, but often a major concern is facing cancer again. Cancer that comes back after treatment is called a recurrence. But some cancer survivors develop a new, unrelated cancer later. This is called a second cancer.
Women whove had breast cancer can still get other cancers. Although most breast cancer survivors dont get cancer again, they are at higher risk for getting some types of cancer, including:
- A second breast cancer
- Salivary gland cancer
- Melanoma of the skin
- Acute myeloid leukemia
The most common second cancer in breast cancer survivors is another breast cancer. The new cancer can occur in the opposite breast, or in the same breast for women who were treated with breast-conserving surgery .
Not Everyone Needs Genetic Testing
If there is a strong family history and you have an ethnic background that puts you at risk for a particular mutation, then it may be worth your while to be tested, says Ross. But testing all your genes to find out all your mutation may not be such a good idea. They say that a third of cancers are inherited but we only know about 5 to 10 percent of cancers with specific genes. Without knowing where to look, the results are hard to interpret.
Also Check: Breast Cancer Secondary Cancer
The Genetic Link Between The Ovaries And The Breasts
The ovaries and the breasts are also connected through a genetic component. Most notably, researchers have established that BRCA1 and BRCA2 gene mutations can increase the risk of both breast cancer and ovarian cancer. Therefore, genetic testing and counseling may be recommended for a woman who is diagnosed with ovarian cancer in order to help her manage her breast cancer risk. Likewise, genetic testing and counseling may be recommended for a woman who is diagnosed with breast cancer and has a known family history of breast or ovarian cancer in order to help her manage her ovarian cancer risk.
If you would like to learn more about the connection between breast cancer and ovarian cancer, you can rapidly connect with a specialist in the renowned Don & Erika Wallace Comprehensive Breast Program Moffitt Cancer Center. To request an appointment, call or complete our new patient registration form online. You can benefit from our extensive cancer expertise within one day.
What Are The Estimated Cancer Risks Associated With Hboc
Cancer risks for women with HBOC
-
Lifetime risk of breast cancer 45% to 75%
-
Lifetime risk of ovarian cancer
-
BRCA1 gene mutation 25% to 40%
-
BRCA2 gene mutation 10% to 20%
-
Developing a second breast cancer 20% to 40%
Cancer risks for men with HBOC
-
Lifetime risk of breast cancer
-
BRCA1 gene mutation 1% to 2%
-
BRCA2 gene mutation 6%
-
BRCA1 gene mutation some increased risk
-
BRCA2 gene mutation 20%
-
Men with a BRCA2 gene mutation have a significantly increased risk of developing more aggressive prostate cancer before age 65 and therefore screening should begin at age 40.
Also Check: Stage Iiii Cancer
Lowering Risk Of Ovarian Cancer
People with breast cancer who are concerned about their ovarian cancer risk should talk to their doctor to learn more about potential next steps. You may be able to change certain habits in order to lower your risk of developing ovarian cancer in the future. Additionally, you may be a candidate for genetic testing to determine whether you have any inherited gene changes.
Where Does Metastatic Ovarian Cancer Spread To
Metastatic ovarian cancer is an advanced stage malignancy that has spread from the cells in the ovaries to distant areas of the body. This type of cancer is most likely to spread to the liver, the fluid around the lungs, the spleen, the intestines, the brain, skin or lymph nodes outside of the abdomen.
Read Also: Cancer Stage 3a
Surgery To Remove The Ovaries And Fallopian Tubes
- Surgery to remove the ovaries and fallopian tubes reduces the risk of:
- cancer of the ovaries and fallopian tubes by up to 95%
- breast cancer by 50% if done before the menopause
Surgery to remove these organs is only done when you have finished having a family. It is not possible to have children after this surgery.
The timing of surgery differs depending on the type of gene fault in your family and also on your own personal and family history.
- In families that carry a BRCA1 gene fault, cancer of the ovaries and fallopian tubes usually develops after the age of 40. Surgery is therefore recommended after the age of 35 and by the age of 40.
- In families that carry a BRCA2 gene fault, cancer of the ovaries and fallopian tubes usually develops at a later age.
Surgery is therefore recommended after the age of 40 and by the age of 45, but can be considered earlier.
Surgery to remove the ovaries and fallopian tubes can often be done by laparoscopic surgery which allows the operation to be done through a few tiny cuts in the tummy. The recovery from this surgery is usually quick, taking less than a week.
If you have had previous abdominal surgery or if you choose to have a hysterectomy at the same time, the operation may be done through a larger cut in the bikini line area.
A hysterectomy can sometimes be done through keyhole surgery depending on the size of the uterus and whether or not you have had previous surgery.
Environmental And Lifestyle Risk Factors
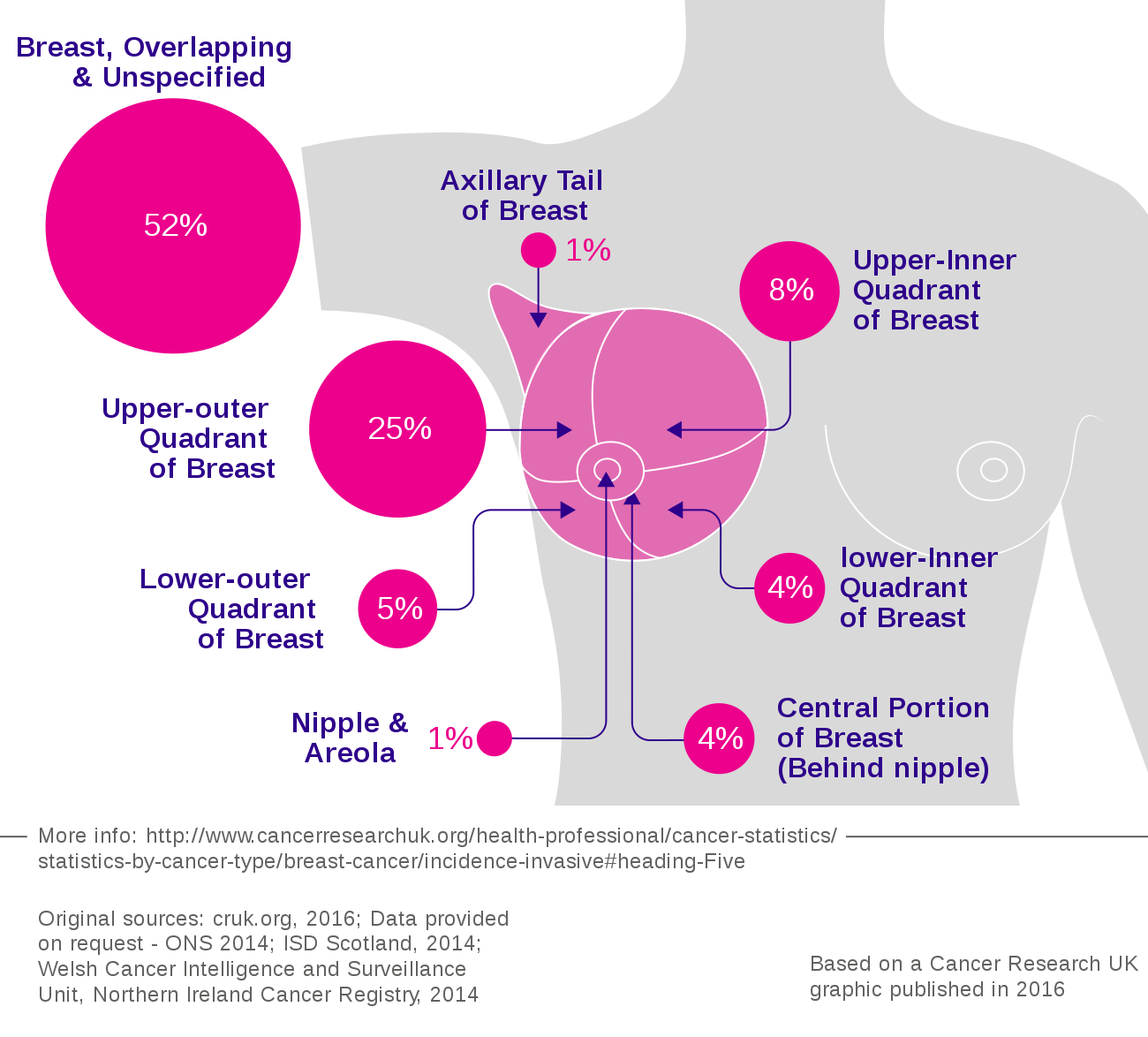
Acquired gene changes may develop after exposure to substances that damage DNA, like ultraviolet light or radiation. Some environmental and lifestyle factors can increase the chances that genes mutate and change. These factors make people more likely to be diagnosed with multiple types of cancer. Gene changes may also develop randomly as a cell grows and divides.
Factors that raise the risk of ovarian cancer or breast cancer include:
- Older age
- Heavier body weight
- Never having had children
- Having your first child at a later age
- Using hormone replacement therapy during or after menopause
If you have any of these shared risk factors, you are slightly more likely to develop ovarian cancer and breast cancer.
You May Like: Breast Cancer Stage 1 Survival Rate