Having Dense Breast Tissue
Breasts are made up of fatty tissue, fibrous tissue, and glandular tissue. Breasts appear denser on a mammogram when they have more glandular and fibrous tissue and less fatty tissue. Women with dense breasts on mammogram have a risk of breast cancer that is about 1 1/2 to 2 times that of women with average breast density. Unfortunately, dense breast tissue can also make it harder to see cancers on mammograms.
A number of factors can affect breast density, such as age, menopausal status, the use of certain drugs , pregnancy, and genetics.
To learn more, see our information on breast density and mammograms.
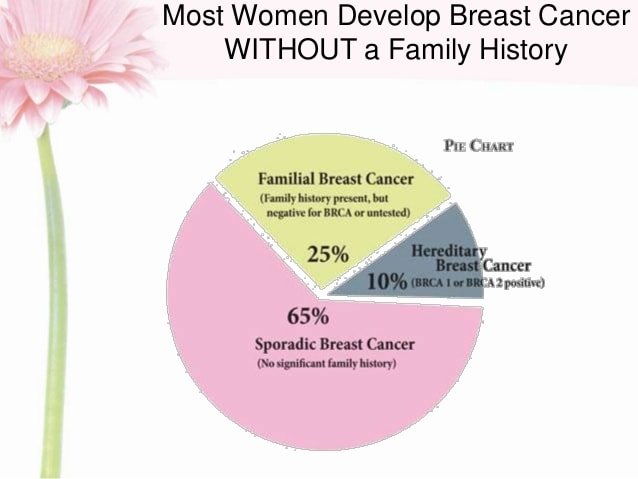
Those With No Family History Of Breast Cancer May Still Be At Risk
As common as breast cancer is about one in eight women will be diagnosed in their lifetime there still are misconceptions about the disease.
I do hear frequently, Im not concerned I dont have any family history, well neither did I, said 13-year survivor Laura Stottlemyer who is a mammographer at MedStar Montgomery Medical Center in Olney, Maryland.
About 75% of those diagnosed actually have no family history, she said.
Having close relatives with breast cancer means youre more likely to develop the disease.
The main things that we do look for are first-degree relatives, Stottlemyer said. And that would include your mother, your sisters or even daughters. And, it can extend to the male side of the families including father, brother or even sons.
Understanding Your Risk Of Breast Cancer
Several breast cancer risk assessment tools have been developed to help a woman estimate her chance of developing breast cancer. The best studied is the Gail model, which is available on the National Cancer Institutes website at www.cancer.gov/bcrisktool. After you enter some personal and family information, including race/ethnicity, the tool provides you with a 5-year and lifetime estimate of the risk of developing invasive breast cancer. Because it only asks for information about breast cancer in first-degree family members and does not include their ages at diagnosis, the tool works best at estimating risk in women without a strong inherited breast cancer risk. For some women, other ways of determining the risk of breast cancer may work better. For example, women with a strong family history of breast cancer risk should consider talking to a genetic counselor.
It is important to talk with your doctor about how to estimate your personal risk of breast cancer and to discuss risk-reducing or prevention options .
Also Check: Can Stage 3 Breast Cancer Be Cured
Breast And Ovarian Cancer And Family History Risk Categories
This table provides examples of average, moderate, and strong family health histories of breast and ovarian cancer. This may help you understand if you have an increased risk for these cancers based on your family health history.
Note: This table does not include all possible family health histories of breast and ovarian cancer. If you have concerns about your family health history of breast or ovarian cancer, please talk to your doctor. Your doctor may assess your risk based on your personal and family health history, using one of the following:
Results may vary, depending on the tool used, and may differ from the risk categories below, which are based largely on the guidelines from the National Comprehensive Cancer Network.1
First-degree = parents, brothers, sisters, children
Second-degree = aunts, uncles, nieces, nephews, grandparents, grandchildren
Triple negative cancers are a type of breast cancer that lack estrogen receptors, progesterone receptors, and human epidermal growth factor receptor 2.
Breast Cancer In Families
If you or one of your close relatives has been diagnosed with breast cancer, you may have concerns about whether breast cancer runs in the family .
A small number of people have an increased risk of breast cancer because of their family history. However, most breast cancers are not inherited and do not increase the lifetime risk for other family members.
Breast cancer is the most common cancer in the UK, so even if you have a relative with breast cancer, it doesnt necessarily mean youre more likely to develop it yourself.
Don’t Miss: Does Getting Hit In The Breast Cause Cancer
From Ancient To Modern Times
The first recorded reports of breast cancer and its treatment were discovered on ancient papyrus out of Egypt. The Edwin Smith papyrus is dated 1600 BCE, but was possibly a copy of an older document, maybe as old as 2500 or 3000 BCE.
The papyrus described several cases of tumors growing in the breast and how they were treated using a fire drilla tool that burnt the skin to destroy the cancerous tissue. The text describes the condition as untreatable.
The term cancer wasnt coined until 400 BCE by Hippocrates, who hypothesized it was an imbalance of humors .
Starting with Hippocratess humors, the road to understanding breast cancer is paved with many ideas which seem odd to modern minds:
Breast Cancer Screening For Women With A Strong Family History Of Breast Or Ovarian Cancer
There are special breast cancer screening guidelines for women with a strong family history of breast or ovarian cancer.
If you have a greater than 20 percent lifetime risk of breast cancer based mainly on your family history of breast or ovarian cancer, the National Comprehensive Cancer Network recommends you get a :
- Clinical breast exam every 6-12 months, but not before age 21
- Mammogram every year, starting 10 years younger than the youngest breast cancer case in your family, but not before age 30
- Breast MRI every year, starting 10 years younger than the youngest breast cancer case in your family, but not before age 25
Learn more about breast cancer screening recommendations for men at higher risk.
Don’t Miss: What Is The Prognosis For Stage 4 Breast Cancer
What Is Genetic Testing
There are several genes which may contain inherited faults linked to the development of breast cancer and ovarian cancer. You may have heard of these they are called BRCA1 and BRCA2. Faults in these genes can be detected using a blood test. Usually, a sample of blood is first taken from a woman in the family who has developed breast cancer or ovarian cancer. The DNA is searched for a gene fault. If a gene fault is detected, then other family members can be tested to see if they carry the same fault.
This testing is recommended in circumstances where there is a strong family history of breast cancer and/or ovarian cancer. The testing is only done under the supervision of a specialised clinic. There are pros and cons to genetic testing, and these will be discussed with you at a family cancer clinic.
Collecting Your Family History
Your mother is an important figure in your cancer risk profile if she has or has had breast cancer. But, given the above, it’s also helpful to find out if cancer has affected other family members, including grandparents, aunts, uncles, and cousins. Don’t assume that you know this informationit’s worth specifically asking.
For the purpose of building your own family history, you need to know:
- What type of cancer a relative had
- What age they were diagnosed
- If they were cured, still living with cancer, or have died
Other details, such as the grade, type, and stage of cancer are not as important for you to know. If you develop breast cancer, your medical team will identify your own grade, type, and stage rather than relying on your family history.
If your mother or father are alive and able to share your family’s background with you, filling out the Cancer Family History Questionnaire that was created by the American Society of Clinical Oncology can help you keep track of the information. Once you gather your family history, it would be useful to keep that record for yourself and for other family members who share some of your family medical history.
Also Check: Did Anne Hathaway Have Cancer
Guidelines For Elective Surgical Options
Women with BRCA1 or BRCA2 mutations face a significant risk of breast and ovarian cancer. Prophylactic removal of the fallopian tubes and ovaries is recommended by about age 40. Many women with BRCA1 or BRCA2 mutations will also elect to have their breasts removed. Nipple-sparing mastectomy is an effective option for these women.
Making the decision to have an elective preventive double mastectomy and removal of the ovaries is personal and should be based on many life factors. You must balance where you are in your childbearing years, what your future choices may be, and whether you would prefer to follow a rigorous screening schedule instead of making such a life-altering choice.
Whatever your decision, we encourage you to make an informed choice. If you do elect to have a preventive double mastectomy, our breast specialists will guide you in the appropriate breast surgery reconstruction to help restore your body image after treatment.
If you are interested in discussing ovary removal surgery , we will refer you to one of our gynecological oncologists.
Show me more…
How To Navigate Breast Cancer Screening Guidelines
In 2018, 47-year-old Adriana Ermter found a lump in her armpit. Her doctor referred her for a mammogram, but the clinic said it was likely just a calcification in her breast tissue. After months of requests for additional screening, the Toronto resident received a second mammogram, an ultrasound, an MRI and a biopsy. The biopsy confirmed the lump was cancer. If I hadnt advocated for myself, under the guidelines I wouldnt have had regular mammograms until I was 50, Ermter says. Who knows what stage of breast cancer I would have progressed to?
Although Ermter caught her cancer early enough, her story is familiar to Jennie Dale, executive director of Dense Breasts Canada, a non-profit that advocates for breast density awareness and better screening. Shes spoken with countless women who were diagnosed with later-stage cancer because they werent screened earlier.
With some MDs following guidelines that dont reflect widely established expert advice, women are finding cancer laterwhich can be deadly. Ermter, who has been cancer-free for three years, is an advocate of early testing. Kornecki agrees: I cannot tell you how frustrating it is to see cancer diagnosed at advanced stages, usually as a result of no screening.
Recommended Reading: Will My Breast Cancer Come Back
Having A Family History Of Breast Cancer
Its important to note that most women who get breast cancer do not have a family history of the disease. But women who have close blood relatives with breast cancer have a higher risk:
- Having a first-degree relative with breast cancer almost doubles a womans risk. Having 2 first-degree relatives increases her risk about 3-fold.
- Women with a father or brother who has had breast cancer also have a higher risk of breast cancer.
Overall, about 15% of women with breast cancer have a family member with this disease.
Family History And Inherited Genes

Some people have a higher risk of developing breast cancer than the general population because other members of their family have had particular cancers. This is called a family history of cancer.
Having a mother, sister or daughter diagnosed with breast cancer increases the risk of breast cancer. This risk is higher when more close relatives have breast cancer, or if a relative developed breast cancer under the age of 50. But most women who have a close relative with breast cancer will never develop it.
Some people have an increased risk of breast cancer because they have an inherited gene fault. We know about several gene faults that can increase breast cancer risk and there are tests for some of them. Having one of these faulty genes means that you are more likely to get breast cancer than someone who doesnt. But it is not a certainty.
Two of these faulty genes are known as BRCA1 and BRCA2. These are not common. Only about 2 out of every hundred of breast cancers are related to a change in the BRCA1 or BRCA2 genes.
Ionising radiation includes tests such as x-rays and CT scans and treatment such as radiotherapy.
Don’t Miss: Anne Hathaway Breast Cancer
So How Will You Know If Somethings Wrong
Women used to be advised to perform regular breast self-exams, but you would have to be very familiar with how your breasts usually feel in order to be aware of an irregularity. Younger women who menstruate regularly can feel differences in their breast tissue during different times in their menstrual cycle, because not all breast tissue is the same. For those reasons, conducting self-exams can cause a lot of stress and anxiety, so doctors have backed off on urging most women to conduct self-exams every month.
On the other hand, its a harmless task. You cant tell women not to do self-exams, Dr. Levine says. There are a lot of calls to the clinic when a woman identifies something that seems suspicious, but most of the time, an experienced examiner will tell you that theres nothing to worry about.
Its also more difficult to diagnose breast cancer in young women, not only because of the changes that can happen during a menstrual cycle, but because younger breast tissue is more dense. That density provides an opportunity for a malignancy to hide in the tissue, making it harder to identify on a mammogram or ultrasound.
Get Screened for Breast Cancer
Find out what you can do to catch breast cancer early.
How Do I Monitor My Breasts If I Have A Family History
The following recommendations apply to all women with or without a family history of breast cancer:
- Be breast aware this means examining your own breasts often enough to be familiar with how they normally feel. This will increase your chances of detecting a change. See the Breast Health brochure for more information.
- See a doctor promptly with any breast changes.
- Have a breast examination performed by a doctor every year.
- Begin having screening mammograms every two years from the age of 40-50.
The recommendations for extra monitoring depend on the risk category you are in.
Don’t Miss: Is Breast Cancer Curable In The 3 Stage
Breast Cancer Risk Factors You Cannot Change
A risk factor is anything that increases your chances of getting a disease, such as breast cancer. But having a risk factor, or even many, does not mean that you are sure to get the disease.
Some risk factors for breast cancer are things you cannot change, such as getting older or inheriting certain gene changes. These make your risk of breast cancer higher.
For information on other known and possible breast cancer risk factors, see:
Connections And More Information
If you would like to talk to young women affected by hereditary breast cancer, connect to our network of support through our Peer Mentor program.
For more information on hereditary breast cancer and tools for tracking your doctor visits and test results, download our Newly Diagnosed Navigator.
You can also:
Read Also: Do You Gain Weight With Breast Cancer
Are Women Under 40 At Risk For Breast Cancer
Younger women generally do not consider themselves to be at risk for breast cancer. However, breast cancer can strike at any age: 5% of breast cancer cases occur in women under 40 years of age. All women should be aware of their personal risk factors for breast cancer.
There are several factors that put a woman at higher risk for developing breast cancer, including:
- A personal history of breast cancer or a high risk lesion found by biopsy
- A family history of breast cancer, particularly at an early age
- A family history that is concerning for a genetic syndrome that may put them at a higher risk for breast cancer
- History of radiation therapy to the chest
- A known genetic mutation conferring a high risk for the development of breast cancer
- Ashkenazi Jewish ancestry
Breast Cancer And No Family History
I never worried about breast cancer. No one in my family ever had it, so I was sure that I was low risk. I got annual mammograms, and they were always clear. None of my physicians ever said anything to suggest that I should be concerned. After all, I was low risk. When I hit menopause and had horrible hot flashes that kept me from sleeping, my doctor suggested hormone replacement therapy . I knew that HRT increased the risk of breast cancer, but the doctor said I should try it. After all, I was low risk. Soon after starting HRT, the hot flashes stopped, and I was soon sleeping again, and able to function. I wasnt worried about HRTs impact on breast cancer because I was low risk. Two years passed on HRT, and I kept getting annual mammograms that were clear. I didnt worry, because I was low risk.
I tried to do some exercise and eat reasonably well as I got older. Then again, I live in a state known for deep-fried cheese and bratwurst. Even so, in May of 2010, when I was 54 years old, I decided to try jogging. I was surprised to note that every time my right foot hit the pavement, I felt a brief pain in my right breast. I wondered what it was, but because I was low risk and Id had a clear mammogram just five weeks earlier, I didnt worry about breast cancer.
Don’t Miss: Can Asbestos Cause Breast Cancer
Being Overweight Or Obese
Women who are overweight after their menopause have a higher risk of breast cancer than women who are not overweight. Men also have an increased risk of breast cancer if they are overweight or obese. For both men and women, the risk increases as more weight is gained.
Body mass index is a measure that uses your height and weight to work out whether you are a healthy weight. For most adults, an ideal is between 18.5 to 24.9. Being overweight means having a BMI of between 25 and 30. Obesity means being very overweight with a BMI of 30 or higher.
Try to keep a healthy weight by being physically active and eating a healthy, balanced diet.
Drinking alcohol increases the risk of breast cancer in women. The risk increases with each extra unit of alcohol per day. The number of units in a drink depends on the size of the drink, and the volume of alcohol.
The latest UK government guidelines advise drinking no more than 14 units of alcohol a week.