What Are The Long
As discussed above, tamoxifen works by blocking estrogen activity in the breasts. However, it can have the opposite effect on the internal reproductive organs. Researchers believe this may contribute to other types of cancer.
For example, some studies have found that people who take tamoxifen long-term are more likely to develop cancer in the lining of the uterus known as endometrial cancer or other uterine tumors.
Tamoxifen can also affect bone density a measure of the strength of the bone. But your risk of this side effect may depend on whether youve gone through menopause yet.
One study followed a group of people who hadnt gone through menopause yet and were taking tamoxifen. The study showed that tamoxifen caused more bone loss in people who continued to menstruate during and after tamoxifen treatment. However, it actually helped to prevent bone loss in those who stopped menstruating during treatment.
Another study of people who had gone through menopause and took tamoxifen found that it helped stop bone loss in the spine. Its important to note that neither of these studies looked at whether these people had a higher or lower risk of broken bones because of tamoxifen.
Lastly, studies have shown that tamoxifen can raise your risk for a pulmonary embolism a life-threatening condition where a blood clot forms and travels to the lungs. If you have a history of blood clots, make sure your healthcare provider is aware of this before you start taking tamoxifen.
What Are Hormone Inhibitors And How Do They Work
Hormone inhibitors also target breast cancer cells with hormone receptors, but unlike hormone blockers, they work by reducing the bodys hormone production. When breast cancer cells are cut off from the food supply the tumor begins to starve and die.Generally, the benefits of using hormone therapy and chemotherapy together have a much greater combined effect than using either alone. If your breast cancer is positive for hormone receptors, your doctor may recommend both therapies.
Less Common Types Of Hormone Therapy
Some other types of hormone therapy that were used more often in the past, but are rarely given now include:
- Megestrol acetate , a progesterone-like drug
- Androgens
- High doses of estrogen
These might be options if other forms of hormone therapy are no longer working, but they can often cause side effects.
Recommended Reading: Baking Soda And Honey For Cancer
Prognostic Values Of Nrf2 Abcc1 Abcc3 And Nqo1 In Human Cancer Patients Treated With Tamoxifen
To determine the validity of our findings from the cell culture and the syngeneic mouse model to responses in human patients, we used a collection of human breast tumors included in the Breast Cancer Relapsing Early Determinants study. This collection included 176 patients diagnosed with primary breast cancer who had their tumors resected before treatment . Of these patients, 64% had ER-positive tumors and ~84% of these patients were treated with tamoxifen. The ER-positive patients who were not treated with tamoxifen were mainly postmenopausal and they received aromatase inhibitors. Other treatments included trastuzumab for those with Human Epidermal growth factor Receptor 2 positive tumors, or anthracycline for high-risk node-negative disease and adjuvant cytotoxic chemotherapy for those with high-risk features. Additional information about the clinical and pathological features of the breast cancer cases used in this study is provided in the .
The gene expression profiles of Nrf2, ABCC1, ABCC3 and NQO1 serve as a good prognostic marker for the survival of human breast cancer patients treated with tamoxifen.
Patients stratified as high and low expressers of Nrf2, ABCC1, ABCC3, NQO1 and NQO1 and ABCC3 together. The survival data were plotted from patients who received tamoxifen treatment or patients with NO tamoxifen treatment .
What Is Hormone Therapy
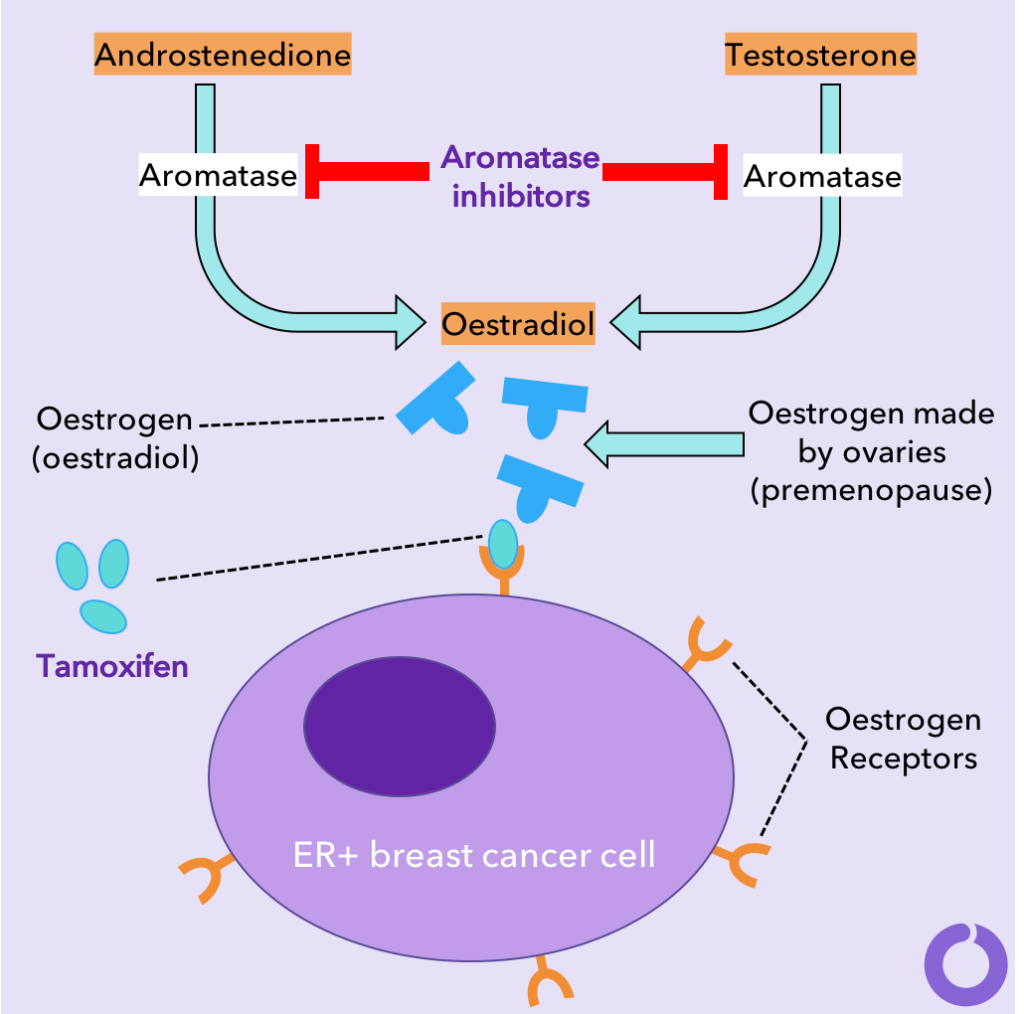
Hormone therapy slows or stops the growth of hormone-sensitive tumors by blocking the bodys ability to produce hormones or by interfering with effects of hormones on breast cancer cells. Tumors that are hormone insensitive do not have hormone receptors and do not respond to hormone therapy.
Hormone therapy for breast cancer should not be confused with menopausal hormone therapy treatment with estrogen alone or in combination with progesterone to help relieve symptoms of menopause. These two types of therapy produce opposite effects: hormone therapy for breast cancer blocks the growth of HR-positive breast cancer, whereas MHT can stimulate the growth of HR-positive breast cancer. For this reason, when a woman taking MHT is diagnosed with HR-positive breast cancer she is usually asked to stop that therapy.
Don’t Miss: Baking Soda For Breast Cancer
What Other Information Should I Know
- Keep all appointments with your doctor and the laboratory. Your doctor will order certain lab tests to check your body’s response to tamoxifen.
- Before having any laboratory test, tell your doctor and the laboratory personnel that you are taking tamoxifen.
- Do not let anyone else take your medication. Talk to your pharmacist if you have any questions about refilling your prescription.
It is important for you to keep a written list of all of the prescription and nonprescription medicines you are taking, as well as any products such as vitamins, minerals, or other dietary supplements. You should bring this list with you each time you visit a doctor or if you are admitted to a hospital. It is also important information to carry with you in case of emergencies.
How Does Tamoxifen Work In The Body
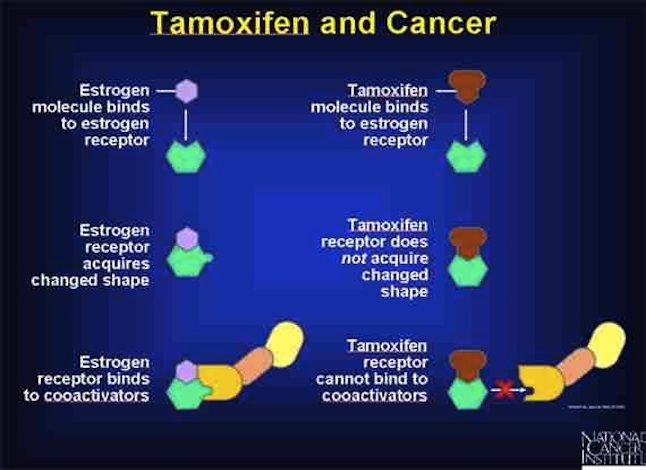
Tamoxifen belongs to a class of medications known as selective estrogen receptor modulators . It works in two ways it lowers estrogen activity in some areas of the body and acts similarly to estrogen in other areas.
For example, tamoxifen prevents estrogen from attaching to receptors in the breast tissue, slowing down the growth of cancer cells. At the same time, tamoxifen acts like estrogen does on the bones, helping to lower the risk of bone-related side effects in some people .
Recommended Reading: Is Stage 3 Breast Cancer Curable
What Other Breast Cancer Treatments Are Often Used Together With Tamoxifen
Your treatment plan with tamoxifen depends on the type of cancer you have or how high your risk of developing breast cancer is. For example, metastatic breast cancer may require more aggressive treatment to prevent the spread of the cancer, whereas tamoxifen alone may be an option for lowering your breast cancer risk.
The following treatments are often used with tamoxifen:
- Targeted therapies This is a treatment that targets certain proteins or genes that help cancer cells grow and survive. An example of a targeted therapy medication is Kisqali .
- Ovarian suppression This is either surgery or medication that prevents the ovaries from producing estrogen. Medications used for this include leuprolide and goserelin .
- Mastectomy This surgical procedure aims to remove the cancerous tissue. As mentioned earlier, this could include removing part or all of the breast.
- Chemotherapy or radiation therapy These are strong treatments designed to kill cancer cells.
How Do People Typically Take Tamoxifen
Tamoxifen comes as an inexpensive generic tablet available in 10 mg and 20 mg strengths. Its also available as a brand-name oral liquid called Soltamox for people who have trouble swallowing pills. However, the liquid is much more expensive than the tablets because it currently has no generic alternative.
Tamoxifen is FDA-approved to treat ER+ breast cancer at both early and advanced stages, including metastatic breast cancer cancer that started in the breast but has spread to other parts of the body. Its also approved to help prevent breast cancer in high-risk people, such as those with a strong family history of breast cancer and those with certain genetic changes.
For people with non-metastatic breast cancer, the recommended dose is 20 mg once a day for 5 years after a mastectomy surgery that removes part or all of the breast. However, some sources suggest continuing the medication for a total of 10 years may help lower the risk of breast cancer recurrence .
For people with metastatic breast cancer, the recommended dose is 20 mg to 40 mg per day for at least 5 years. The 20 mg dose can be taken once a day, but the 40 mg dose should be taken as 20 mg twice a day . Some studies suggest taking 40 mg per day may be no more effective than taking 20 mg per day, but healthcare providers may still choose to prescribe the higher dose for some people.
People taking tamoxifen to prevent breast cancer are recommended to take 20 mg daily for 5 years.
Don’t Miss: Don Harrington Breast Cancer Center
Tamoxifen As Breast Cancer Treatment
Tamoxifen lowers the risk of :
- Breast cancer recurrence
- Breast cancer in the opposite breast
- Death from breast cancer
Tamoxifen is a pill taken every day for 5-10 years. For premenopausal women, tamoxifen may be combined with ovarian suppression.
The benefits from tamoxifen last long after you stop taking it.
Find a list of questions on hormone therapy for your health care provider.
|
For a summary of research studies on tamoxifen for early breast cancer, visit the Breast Cancer Research Studies section. |
How Does Tamoxifen Work For Pct
When you run anabolic steroids, the body receives signals that too many hormones are produced so it stops producing them naturally. Depending on the type, amount, dosage of steroids as well as cycle length there are different levels of suppression.
But any anabolic steroid cycle suppresses the production of testosterone thats why it is important to run a PCT plan to help your body recover HPTA. Tamoxifen does exactly that.
TamoxifenCitrate is stimulating the hypothalamus for releasing more gonadotropins the protein hormones that are secreted by the pituitary gland which are responsible for a faster and higher release of FSH and LH. As a result, you get more testosterone since Tamoxifen helps increase LH.
Therefore, you are capable of getting a boosted testosterone level, a smooth PCT and wont get typical symptoms of getting off a steroid cycle.
- You wont lose muscles, gain fat, lose energy, lose sex drive, motivation etc.
As mentioned, Tamoxifen selectively binds to estrogen receptors blocking their activity thats how it works here too. It prevents estrogen from reaching the pituitary gland and therefore, this leads to higher production of LH. The Luteinizing Hormone offers signals to the Leydig cells for producing testosterone.
Tamoxifen is extremely effective studies prove that users of Tamoxifen who used to have LH levels of almost 0 they managed to reach over 10 iu and thats even more than the normal reference range for an adult man.
Also Check: Is Breast Cancer Curable
Effectiveness In Premenopausal Women
In premenopausal women, the majority of estrogen in the body is produced by the ovaries. After menopause, the conversion of androgens to estrogen is the primary source of estrogen. Aromatase inhibitors work by blocking this conversion, hence reducing estrogen levels.
Since aromatase inhibitors do not address estrogen produced by the ovaries, they are ineffective before menopause unless a woman has received ovarian suppression therapy. This, however, is not the case with tamoxifen.
What Are The Side Effects Of Hormone Therapy
The side effects of hormone therapy depend largely on the specific drug or the type of treatment . The benefits and harms of taking hormone therapy should be carefully weighed for each person. A common switching strategy used for adjuvant therapy, in which patients take tamoxifen for 2 or 3 years, followed by an aromatase inhibitor for 2 or 3 years, may yield the best balance of benefits and harms of these two types of hormone therapy .
Hot flashes, night sweats, and vaginal dryness are common side effects of all hormone therapies. Hormone therapy also may disrupt the menstrual cycle in premenopausal women.
Less common but serious side effects of hormone therapy drugs are listed below.
Tamoxifen
- Breathing problems, including painful breathing, shortness of breath, and cough
- Loss of appetite
Recommended Reading: Anne Hathaway Breast Implants
Preventing Breast Cancer In The Opposite Breast
About 1 in 20 women diagnosed with breast cancer will develop breast cancer in the opposite breast within the 10 years after first breast cancer diagnosis. A 2017 study in the prestigious medical journal JAMA found that taking tamoxifen can reduce the percentage of those women from developing cancer in the opposite breast within 10 years, from about 5% to 2%. Unfortunately, the study authors did not report on breast cancer deaths or deaths for any other reason. Therefore, we do not know whether tamoxifens reduction of cancer in the opposite breast had any impact on the womens longevity.
If You Have Ongoing Side Effects
Most of the time side effects can be controlled or managed. But for a few people, they can be more difficult to manage. If this happens, talk to your doctor or nurse. They can usually suggest ways to improve your side effects. If things do not improve, go back to your doctor or nurse. They may suggest you try something else.
It is important not to stop taking tamoxifen without telling your doctor. Stopping may affect the success of your treatment. If side effects cannot be managed, your doctor may suggest you take a different type of hormonal therapy.
Read Also: Is Breast Cancer Curable In The 3 Stage
Are There Any Health Risks Associated With Taking Tamoxifen
Aside from the common side effects, tamoxifen can cause some more serious health problems that you should be aware of. They include:
- Higher risk of blood clots
- Eye problems, such as cataracts
- Higher risk of uterine cancer
- Bone loss in people who havent gone through menopause
Call 911 or seek immediate medical care if you experience any of the following:
- Leg swelling or tenderness, leg thats red or warm to touch, shortness of breath, chest pain
- Unusual monthly bleeding or severe pains around the hips and groin
Cancers Of The Uterus
Because tamoxifen acts like estrogen in the uterus, it can increase your risk of endometrial cancer and uterine sarcoma . It also is linked to a higher risk of endometrial pre-cancers. Raloxifene does not act like estrogen in the uterus and is not linked to an increased risk of uterine cancer.
Although tamoxifen does increase the risk of uterine cancer, the overall increase in risk is low . The risk of uterine cancer goes back to normal within a few years of stopping the drug.
The increased risk seems to affect women over 50, but not younger women.
If you have been diagnosed with uterine cancer or pre-cancer you should not take tamoxifen.
If you have had a hysterectomy , you are not at risk for endometrial cancer or uterine sarcoma and do not have to worry about these cancers.
If you are taking tamoxifen, tell your doctor if you have any abnormal vaginal bleeding or spotting, especially after menopause, as these are possible symptoms of uterine cancer.
You May Like: Did Anne Hathaway Have Breast Cancer
Side Effects And Risks Of Treatment
Tamoxifen increases the chances of developing endometrial cancer and blood clots in the legs and lungs. In a Danish study, the 5-year risk of developing blood clots was about 1.2% in breast cancer patients taking tamoxifen compared to 0.5% in breast cancer patients who were not taking tamoxifen. Tamoxifen often causes side effects similar to those experienced in menopause, including hot flashes and irregular periods. In one study, 41% of women taking tamoxifen experienced hot flashes, and 10% experienced abnormal periods .
Tamoxifen Treatment Induces Oxidative Stress
Tamoxifen is hydrophobic and it accumulates rapidly in phospholipid bilayers of membranes where it is postulated to induce oxidative stress. To investigate this, we pretreated 4T1 breast cancer cells with the superoxide indicator, dihydroethidium , which is oxidized to produce a bright fluorescent red color when it interacts with superoxide. Treatment with 10M tamoxifen for 24h significantly increased the red staining in 4T1 cells, indicating a higher level of superoxide generation . Since this could lead to lipid peroxidation, we measured the production of 4-hydroxynonenal , which results from the oxidation of membrane lipids. 4HNE conjugates with cell proteins and this effect can be visualized by Western blotting with an anti-4HNE antibody. Treatment of 4T1 cells with 10M 4HT for 24h significantly increased the conjugation of proteins at 65kDa with 4HNE and this effect was partially blocked with the antioxidants, vitamin E and/or PMC . Increased conjugation of cell proteins with 4HNE was also observed in MCF-7 cells treated for 312h with 20M 4HT . Hence, treatment of breast cancer cells with 4HT increased in the oxidation of membrane lipids .
Tamoxifen treatment induces oxidative stress.
Don’t Miss: How To Remove Breast Cancer Naturally
Can Other Drugs Interfere With Hormone Therapy
Certain drugs, including several commonly prescribed antidepressants , inhibit an enzyme called CYP2D6. This enzyme plays a critical role in the body’s use of tamoxifen because CYP2D6 metabolizes, or breaks down, tamoxifen into molecules, or metabolites, that are much more active than tamoxifen itself.
The possibility that SSRIs might, by inhibiting CYP2D6, slow the metabolism of tamoxifen and reduce its effectiveness is a concern given that as many as one-fourth of breast cancer patients experience clinical depression and may be treated with SSRIs. In addition, SSRIs are sometimes used to treat hot flashes caused by hormone therapy.
Many experts suggest that patients who are taking antidepressants along with tamoxifen should discuss treatment options with their doctors, such as switching from an SSRI that is a potent inhibitor of CYP2D6, such as paroxetine hydrochloride , to one that is a weaker inhibitor, such as sertraline or citalopram , or to an antidepressant that does not inhibit CYP2D6, such as venlafaxine . Or doctors may suggest that their postmenopausal patients take an aromatase inhibitor instead of tamoxifen.
Other medications that inhibit CYP2D6 include the following:
- Quinidine, which is used to treat abnormal heart rhythms