How Long Can You Live With Stage 3 Cancer
The five-year relative survival rate for these three types of tumors is 44 percent, according to the American Cancer Society. Early detection generally results in a better outlook. When diagnosed and treated in stage 1, the five-year relative survival rate is 92 percent.Outlook by stage.StageSurvival Rate365%435%2 more rows
Read Also: Stage Four Breast Cancer Treatment
For Microinvasive Dcis Breast Conserving Surgery With Radiation Is Usually Considered The Most Reasonable Approach
Because of the high rates of survival and freedom from distant metastases and because of the ability to salvage patients with local recurrence, breast-conserving surgery and definitive irradiation should continue to be considered as an alternative to mastectomy for appropriately selected and staged patients with microinvasive ductal carcinoma of the breast. However, virtually all microinvasive ductal carcinoma tumors which eventually metastasize are shown to be tumors with a T1 invasive status.
Is There A Breast Cancer Cure
There are many very good breast cancer treatments, which can often cure breast cancer. Treatment outcomes have also improved now that many are diagnosed at an early stage, due to mammogram screenings. Once breast cancer has spread, it becomes more difficult to cure. Certain types of breast cancer are more likely to be cured, such as infiltrative ductal carcinoma, the most common type of breast cancer, which is limited to the milk duct region and can almost always be cured if found before it has spread. Infiltrative lobular carcinoma is harder to cure as it often affects both breasts. Hormone receptor-positive cancer has a better prognosis than triple-negative cancer .
Read Also: What To Expect During Chemo For Breast Cancer
Common Risk Factors Of Invasive Breast Cancer
The most common form of breast cancer, invasive ductal carcinoma, is primarily associated with particular risk factors.
It is important to note that simply having the following risk factors does not 100% mean you will develop breast cancer. In fact, some women develop breast cancer with no known risk factors.
Risk factors include:
For example, women aged 50 to 59 have a 2.4% chance of developing breast cancer vs. women aged 70 and over who have a 7% chance.
Although breast cancer incidence increases with age, age-related differences based on the frequency of tumor subtypes depend on hormone receptor status and pathological grade.
So, younger and older patients have a higher frequency of estrogen receptor-negative, which reduces their chances of developing breast cancer more than middle-aged patients with estrogen receptor-positive and low-grade tumors.
Why Are Receptors Important
Receptors are tiny proteins on the surface of the cells that act like light switches that can turn on and off cancer cell growth. The Estrogen receptor , Progesterone receptor and HER2 receptor results are incredibly important for you to know and understand. There are great treatments available for all combinations of cancer receptor types. This information is critical in guiding you to therapies that may be needed before or after surgery, such as chemotherapy or hormonal therapy. You should try to understand this aspect of your cancer care from the outset. Take our lesson on My Tumor Receptors to learn the essentials.
Recommended Reading: Breast Cancer Final Stage Symptoms
What Is The Best Breast Cancer Treatment For Older Patients
In gauging which treatment might be best for an individual, Tran looks at the characteristics of the tumor. This can help identify tumors that are likely to respond to hormone-blocking therapy alone and those that may respond to other modes of treatment.
Genomic breast cancer tests can map the genome of the cancer cells and help reveal their sensitivity to hormone-blocking treatment, chemotherapy or both. Though Tran says oncotype tests are not appropriate for every patient, for some people with invasive cancers that are larger than 0.5 centimeters and estrogen positive, the tests can provide information on how likely a particular cancer is to return after therapy.
Tran says that in late 2019 and early 2020, genomic tests for breast cancer were improved, and they can now yield clues on more advanced breast cancers, even those that have infiltrated the lymph nodes. Using these data, your doctor is better prepared than ever to recommend a treatment plan to bring breast cancer under control.
When To Contact A Doctor
A person not diagnosed with cancer should see a doctor regularly for routine health checks. This can include cancer screenings to check for early signs of potential cancer.
A person diagnosed with non-invasive cancer should see a doctor more frequently for checks. A doctor can check to see if the cancer has progressed or come back.
A person in treatment for invasive cancer should work with a doctor to determine how often they need medical appointments. They should do their best to keep all appointments and follow treatments as prescribed.
A person should contact a doctor if they notice any side effects from treatment. A doctor may be able to help them cope with the side effects.
Recommended Reading: Stage 3 Breast Cancer Treatment
The Prognosis For Microinvasive Carcinoma Of The Breast Is Very Good
There is universal agreement that the prognosis for ductal carcinoma discovered and intervened at a microinvasive stage, is very good. Patients with microinvasive breast cancer can typically expect a cure rate very close to 100%, with local treatment alone. Most microinvasive breast cancers will be treated by breast conserving surgery or by radical mastectomy . Adjuvant treatment is still a bit controversial, but radiotherapy is very common , while chemical and endocrine treatments are much common and will likely depend on the hormone receptor status of individual patients.
Staging And Treatment Of Microinvasive Breast Cancer : Is Axillary Lymph Node Investigation Necessary
Staging of microinvasive ductal carcinoma in situ is somewhat of a controversial topic. The general consensus surrounding pure ductal carcinoma in situ is that axillary lymph node metastasis is so very improbable that lymph node staging or sentinel lymph node biopsy are not necessary.
The overall estimated rate of lymph node metastases in patients with microinvasive breast carcinoma is low, but not negligible. The statistics also tend to be quite inconsistent, adding to the dilemma. Some studies on lymph node metastasis of microinvasive DCIS place the rate from 0 to just over 5%. Other studies suggest a rate of lymph node metastasis as high as 10%-11%, while others place it as high as 28%.
Read Also: Effects Of Breast Cancer On A Person
Breast Radiotherapy At Genesiscare
Radiotherapy is the most commonly used treatment after breast cancer surgery. GenesisCare is at the forefront of developments in radiotherapy. We provide the latest-generation systems to deliver highly targeted radiotherapy for effective tumour treatments with fewer side effects.
Radiotherapy usually happens after surgery. Modern radiotherapy is very effective at treating cancer and reducing the risk of cancer recurrence in the breast and lymph nodes.
Not all radiotherapy is the same and there are many differences in the treatment given at GenesisCare that make it world class. Various state-of-the-art radiotherapy techniques are available for all patients.
External beam radiotherapy uses a machine called a linear accelerator to accurately deliver carefully planned beams of radiation to the breast and lymph node areas.
GenesisCare are leading experts in modern techniques called volumetric modulated arc radiotherapy for breast cancer and intensity modulated radiotherapy . These advanced therapies vary the radiation across the treatment area, making this very accurate.
Your consultant will assess your cancer to decide the best radiotherapy approach for you.
The aim is to treat the breast cancer and prevent it from coming back at a future date, so theyll also consider other treatments such as long-term hormone therapy, which will also lower the chance of this happening.
Hormone Therapy For Breast Cancer
Three out of every four invasive breast cancers are ER or PgR positive and you may have been told that your cancer is hormone sensitive. This means the cancer cells are triggered to grow by oestrogen, a female sex hormone that is made mostly by the ovaries, or by progesterone. If so, you will be offered hormone therapy, also known as endocrine therapy.
Hormone therapy drugs work in different ways. Some block oestrogen from attaching to cancer cells, whilst others reduce the amount of oestrogen your body makes. They can be very effective in preventing breast cancer recurrence or spread.
Your consultant will discuss the treatment options with you and the best time to start. Usually, hormone therapy is started after surgery and continues for several years to help prevent cancer returning. Sometimes it is given to help shrink a tumour before surgery.
Hormone therapies can cause side effects, many of which mimic the symptoms of menopause. If you havent yet reached the menopause, our breast care nurses will explain what to expect. We have a lot of support available to help you manage these symptoms and to provide emotional guidance throughout your therapy.
Chapter 4
Recommended Reading: Is Breast Cancer Curable At Stage 3
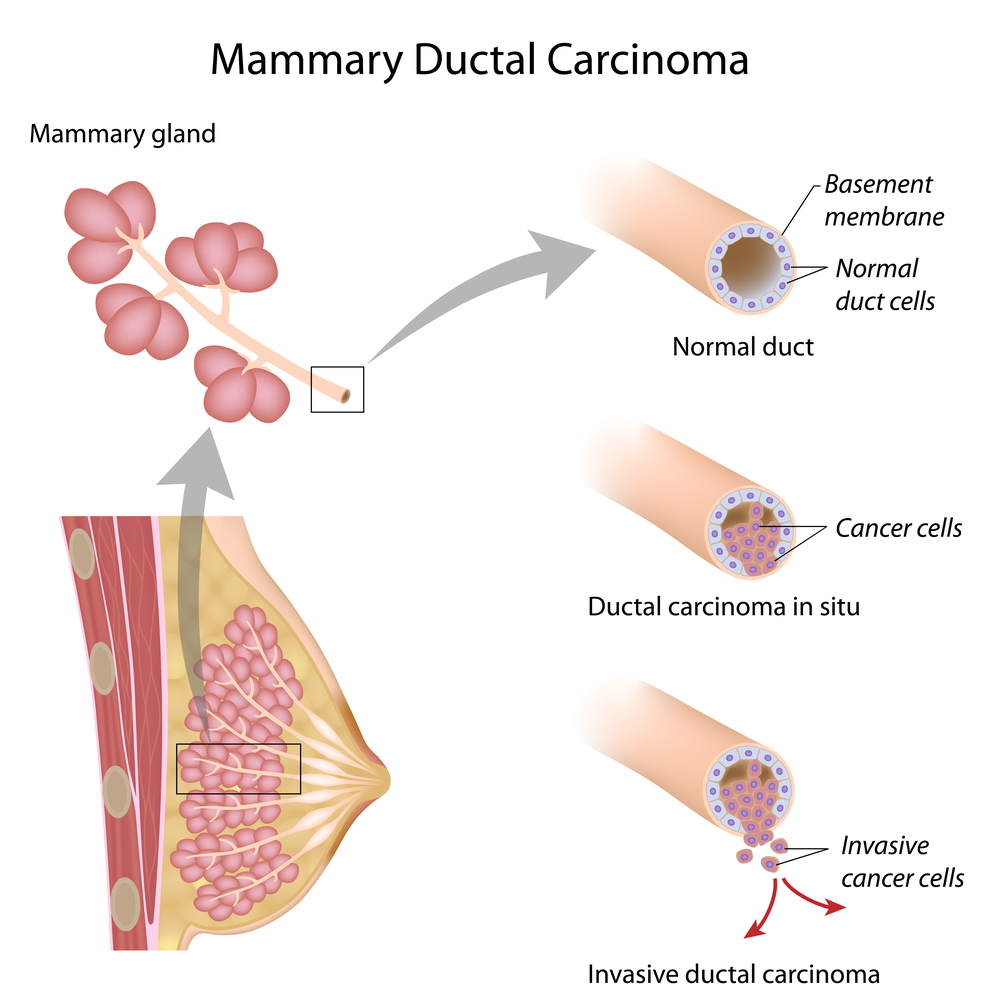
What Is Invasive Breast Cancer
Breast cancer most often begins in the milk producing glands or the milk ducts. When cancer cells spread outside of these areas and into healthy breast tissue, its called invasive breast cancer.
Most breast cancers are invasive. In fact, according to the American Cancer Society, of breast cancers are an invasive type.
Risk Of Lymph Node Metastasis Is Extremely Low In Micro
So, there is agreement that the risk of lymph node metastasis is very low, but the debate then turns to analyzing the various presenting factors in the microinvasive breast cancer tumor which might positively or negatively influence the incidence rate. Some studies have considered the difference in frequency of axillary node metastasis between tumors with measurable invasion, versus those of microfocal invasion. The rate of axillary lymph node metastasis for microinvasive tumors is estimated at around 4%, and about 8%-9% for measurable tumors. Whether or not the statistical difference is significant is still a matter of interpretation. However, the T1 threshold seems to be significant among physicians, and these larger tumors, even if 90% of the tumor is still DCIS, are thought to be more worrisome.
Recommended Reading: Breast Cancer Return Symptoms
A Team Approach To Breast Cancer Treatment
Tran says older patients or anyone diagnosed with breast cancer can benefit from getting care at a comprehensive center, such as the one where she performs surgery: the Sullivan Breast Center at Sibley Memorial Hospital in Washington, D.C.
Our team meets weekly to discuss individual patients cases, and that helps us bring the best thinking to each persons treatment plan, Tran says. Our combined experience supports every patient.
Breast Health Services
Ovarian Ablation Or Suppression
In women who have not yet experienced the menopause, oestrogen is produced by the ovaries.
Ovarian ablation or suppression stops the ovaries working and producing oestrogen.
Ablation can be done using surgery or radiotherapy. It permanently stops the ovaries from working and means you’ll experience the menopause early.
Ovarian suppression involves using a medicine called goserelin, which is a luteinising hormone-releasing hormone agonist .
Your periods will stop while you’re taking it, although they should start again once your treatment is complete.
If you’re approaching the menopause , your periods may not start again after you stop taking goserelin.
Goserelin comes as an injection you have once a month.
Recommended Reading: 3b Cancer
What Increases The Risk Of Invasive Breast Cancer
Thereâs no way to know if youâll develop an invasive form of breast cancer, but there are things that increase your chances, many of which you canât change.
Older women are at higher risk. About 10% of women diagnosed with invasive breast cancer are under age 45. And 2 out of every 3 women with invasive breast cancer are age 55 or older when theyâre first diagnosed.
Your genetics and family history of breast cancer play roles. Itâs more common among white women than black, Asian, or Hispanic women.
Also, youâre at higher risk if youâre obese, your breasts are dense, you didnât have children, or you became pregnant after the age of 35.
Rare Types Of Invasive Ductal Carcinoma
Medullary ductal carcinoma accounts for only 3%5% of breast cancers. It may appear on a mammogram, and it does not always feel like a lump rather, it can feel like an abnormally spongy area in the breast tissue.
Mucinous ductal carcinoma is also called colloid breast cancer. It occurs when cancer cells within the milk duct of the breast produce mucous, which also contains breast cancer cells. The cells and mucous combine to form a tumor. Pure mucinous ductal carcinoma tends to grow slowly, and has a better prognosis than some other types of IDCs.
Papillary carcinoma forms finger-like projections that can be seen under a microscope. Many papillary tumors are benign, but even those that become cancerous are usually very treatable with a good prognosis. Papillary carcinoma most commonly occurs in people older than 60.
Tubular ductal carcinoma is a rare diagnosis of IDC, comprising only 2% of breast cancer diagnoses. The name comes from how the cancer looks under the microscope like hundreds of tiny tubes. Tubular breast cancer has an excellent prognosis.
Read Also: Symptoms Of Stage 2 Breast Cancer
How Do You Prevent Invasive Ductal Carcinoma
There is no single way to prevent all cases of breast cancer but people can take steps to lower the risk.
- Lose weight or maintain a healthy weight
- Breastfeed for at least several months
- Use non-hormonal options to treat menopausal symptoms
- For women at increased risk of breast cancer :
- Genetic counseling and testing for breast cancer risk
- Close observation to look for early signs of breast cancer
- More frequent doctor visits for breast exams and ongoing risk assessment
- Start breast cancer screening with yearly mammograms at an earlier age
- Other screening tests, such as breast MRI
Histological Grade And Ki67
Histological grade information was available from the ICD-O-3 code and categorized as low , intermediate and high according to the Elston-Ellis modification of the Scarff-Bloom-Richardson grading system . Women with anaplastic carcinoma were excluded, leaving n=24,137 women for the analysis . Ki67 has been recorded routinely since 2011 and was categorized as low , intermediate or high according to cutoffs in the Norwegian treatment guidelines .
You May Like: What Is The Youngest Age To Have Breast Cancer
You May Like: Grade 3 Invasive Ductal Carcinoma
How Is It Diagnosed
There are a variety of tests to diagnose invasive breast cancer. These include:
- Breast exam: During a breast exam, a healthcare professional will carefully feel your breasts for signs of lumps or other changes.
- Mammogram: During a mammogram, a device presses your breasts between two plates. X-ray images of the breast tissue are then taken and evaluated for signs of cancer.
- Imaging tests: A healthcare professional may order additional imaging tests to help them better visualize breast tissue. Some examples include ultrasound or magnetic resonance imaging .
- Biopsy: During a biopsy, a sample of breast tissue is carefully removed and checked under a microscope for signs of cancer.
- Blood tests: Blood tests use a sample your blood to check for various markers of disease or illness.
If cancer is detected, additional tests can be used to help characterize the cancer and determine its stage. These tests can include things like:
- Receptor testing: Various tests can check for estrogen receptors, progesterone receptors, and HER2 status.
- Lymph node biopsy: A lymph node biopsy can determine if the cancer has spread to the nearby lymph nodes.
- Imaging tests: Imaging tests can look to see if cancer has spread to other areas. Some that may be used include bone scans, X-rays, CT scans, and positron emission tomography scans.
CE MM 4/8/2021: resolved
Treatment for invasive breast cancer depends on the stage of the cancer as well as other factors. Lets examine the most common treatment options.
How Often Does Stage 1 Breast Cancer Come Back After Treatment
If stage 1 cancer is treated comprehensively, it rarely comes back. A new, unrelated breast cancer is more likely to emerge after stage 1 breast cancer is treated than a recurrence. Your healthcare provider will recommend a surveillance schedule for you so that new breast cancer or a recurrence can be identified and treated as quickly as possible.
Recommended Reading: Can Breast Cancer Go Away
What Is The Chance I Will Die Of My Cancer
Most women just diagnosed with breast cancer have no idea how much of a risk to their life their unique situation poses. Any invasive breast cancer does impart some level of risk to your life. However, this risk is usually less than you would assume.
The average 5-year survival rate for all people with breast cancer is 89%. The 10-year rate is 83%, and the 15-year rate is 78%. If the cancer is located only in the breast , the 5-year survival rate is 99%. More than 70% of breast cancers are diagnosed at an Early Stage .
How Quickly Does Invasive Breast Cancer Spread
Cancer cells are similar to healthy cells in the body that grow through cellular division, whether non-invasive or invasive. According to the Robert W. Franz Cancer Research Center, breast cancer cells divide at least 30 times before being detected in a screening or physical exam. Each division may take between 1-2 months, suggesting a detectable tumor takes between 2-5 years in the body.
Since the period varies, breast cancer grading and staging come in handy to determine how quickly invasive breast cancer can spread. For instance, grade 3 breast cancer spreads much faster than grade 1 and 2. Stage IV invasive breast cancer spreads much faster since multiple cancer cells are dividing.
You May Like: Breast Cancer Growth Rate