Side Effects And Complications
All treatments have some side effects that range from mild to severe. Most clear up when treatment ends, but there can be some lasting complications.
Its important to tell your oncologist about all symptoms, even if they seem minor. Your healthcare team will work with you to ease side effects and deal with complications.
Will My Menstrual Flow Be Different After Chemotherapy
Menstrual cycles vary from woman to woman. Some women may experience less frequent cycles than they had prior to chemotherapy. They may skip a period or increase the number of days between periods. Other women may have more frequent periods.
Some women may not experience a change in the length of their menstrual cycles but the flow pattern may be different than it was before treatment . Mixed patterns are also common: some women may have shorter menstrual cycles with heavier bleeding, or infrequent cycles with many days of a very high flow.
Even though periods tend to be irregular around the time of menopause, it is important to be aware of bleeding that is not normal for you. It is very important to call your physician if you ever have very heavy bleeding that is associated with weakness or dizziness.
Feeling Sick And Being Sick
You may feel sick or be sick after chemotherapy. This will depend on the type and dose of drugs youre having. But this can usually be controlled.
You may start feeling sick straight after chemotherapy, a few hours after or up to several days later. For some people it may last for a few hours and for others it can continue for several days.
People who are very anxious or prone to travel sickness or morning sickness in pregnancy may be more likely to actually be sick.
Youll be given anti-sickness medication, as tablets or into a vein, before each cycle of chemotherapy. Youll also be given anti-sickness tablets to take at home.
Several types of anti-sickness drugs are available. You may need to take a combination of drugs to relieve your symptoms. This may include taking a low dose of steroids for a short time. If you keep feeling sick or are being sick, let someone in your treatment team know.
Contact your hospital if you keep being sick and have difficulty keeping fluids down, even if it happens at the weekend or during the night.
Recommended Reading: Don Harrington Breast Cancer Center
Other Drug Treatments For Cancer
The traditional drugs used for chemotherapy are an important part of treatment for many cancers. The drugs affect both cancer cells and healthy cells. But scientists have designed newer drugs that work more specifically to treat cancer. These treatments cause different side effects.
Doctors may use these newer cancer drugs as the only drug treatment. But they are often added to traditional chemotherapy. These types of treatment include:
Hormonal therapy. These treatments change the amount of hormones in your body. Hormones are chemicals your body makes naturally. They help control the activity of certain cells or organs. Doctors use hormonal therapy because hormone levels control several types of cancers. These include some breast and prostate cancers.
Targeted therapy. These treatments target and disable genes or proteins found in cancer cells that the cancer cells need to grow.
Immunotherapy. This type of treatment helps your body’s natural defenses fight the cancer. Immunotherapy is now an important part of treatment for several types of cancer and will play an increasingly important role in treatment in the future.
Inflammatory Breast Cancer Treatment
Inflammatory breast cancer is an uncommon and aggressive type of breast cancer caused by cancer cells blocking lymph vessels in the skin.
All IBC cases are classified as at least stage 3 breast cancer. If the cancer is metastatic , its considered stage 4.
Treatments for IBC depend on what stage the cancer is in.
Don’t Miss: Baking Soda For Breast Cancer
Radiation For Metastatic Breast Cancer
Sometimes breast cancer spreads to other parts of the body. When this happens, the breast cancer is called metastatic or stage IV.
If youve been diagnosed with metastatic breast cancer and are having symptoms, your doctor may recommend radiation therapy to:
- ease pain
- lower the risk of a cancer-weakened bone breaking
- open a blocked airway to improve breathing
- reduce pressure on a pinched spinal cord or nerve that might be causing pain, numbness, or weakness
- treat cancer that has spread to the brain
The radiation dose and schedule to treat metastatic breast cancer depends on a number of factors, including:
- the level of pain or amount of function lost
- the size of the cancer
- the location of the cancer
- the amount of previous radiation youve had
- the schedule for any other treatments
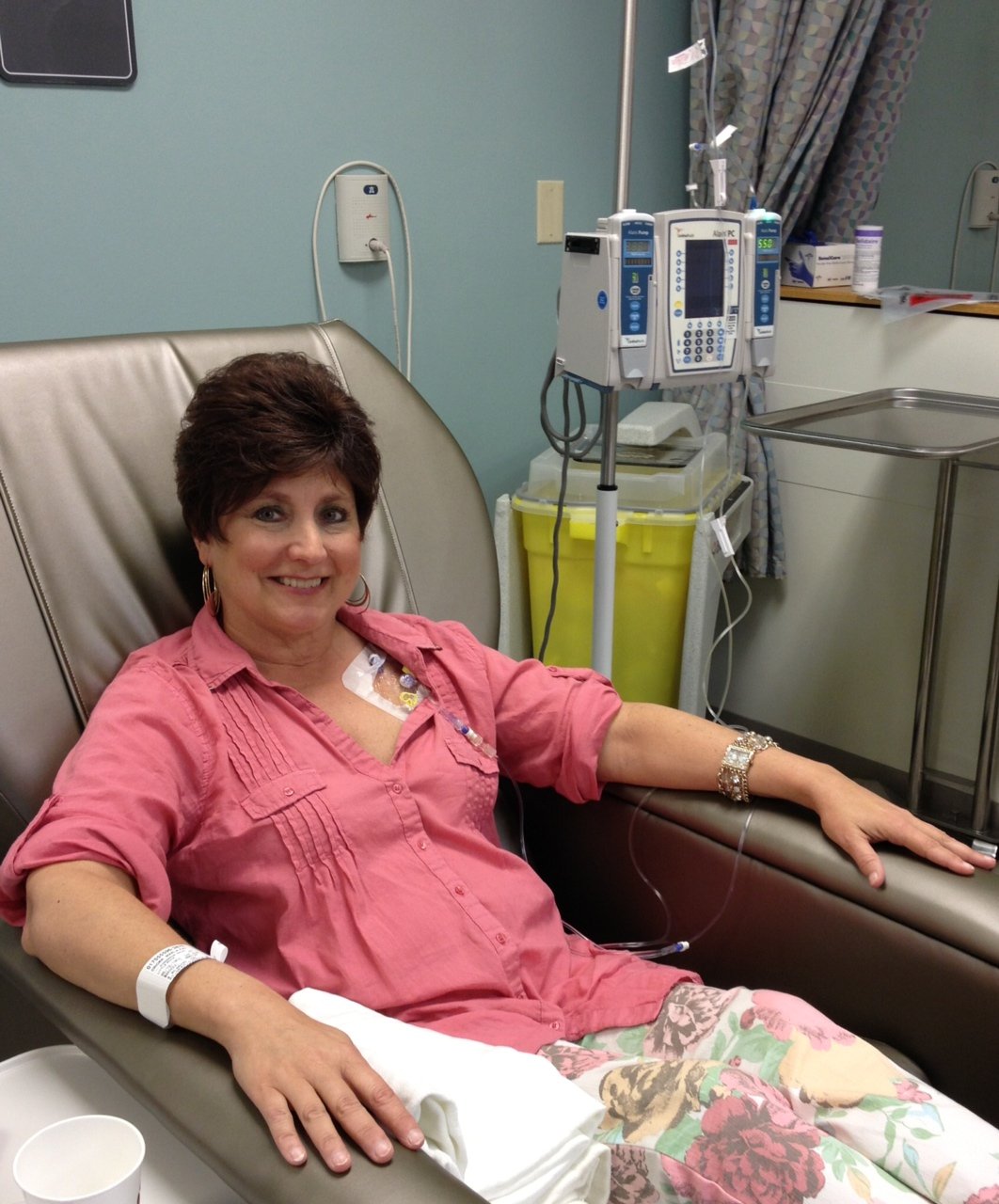
How Do You Get Chemotherapy For Breast Cancer
You get chemotherapy as a pill or in a vein daily, weekly, or every 2-4 weeks. You may get one drug or a combination of them. Your treatment plan is designed for your particular situation.
If your veins are hard to find, you may get a catheter in a large vein. These devices are inserted by a surgeon or radiologist and have an opening to the skin or a port under the skin, allowing chemotherapy medications to be given. They can also be used to give fluids or take blood samples. Once chemotherapy is finished, your catheter will be removed.
Read Also: What Is Stage 3a Breast Cancer
Trends In Research And Therapy
The therapeutic options for breast cancer patients have increased dramatically in the 21st century with increasing efforts towards the development of more efficient and effective screening, diagnosis and treatment options. The landscape of therapy for patients with metastatic breast cancer is also changing. For instance, many ongoing studies are exploring strategies to overcome endocrine resistance, target TNBC and develop new anti-HER2 therapies. There are promising advances in immunotherapy and new directions in inhibiting aberrant angiogenesis, one of the hallmarks of tumors . Our understanding of the molecular characteristics of tumors in general, coupled with better screening methods has helped shape the recent advances in breast cancer treatment. Neoadjuvant therapy, for example, has become a standard recourse. There are strategies not only for HER2- and ER-positive cancers, but also new options in the management and treatment of TNBC patients .
Sex Contraception And Pregnancy
You can still have sex during treatment. Its thought that chemotherapy drugs cant pass into vaginal fluids or semen, but this cant be completely ruled out as chemotherapy drugs can pass into the blood and some other body fluids. Most treatment teams will advise using barrier methods of contraception, such as condoms during treatment, and for a few days after chemotherapy is given.
If you havent been through the menopause, its important to use contraception because chemotherapy drugs can harm a developing baby in the first three months of pregnancy. Its still possible to become pregnant even if your periods become irregular or stop completely.
Your specialist will usually recommend barrier methods of contraception, such as condoms. The contraceptive pill is not usually recommended because it contains hormones. Emergency contraception such as the morning after pill can still be used.
An interuterine device can be used as long as its not the type that releases hormones. If you have a coil in place that does release hormones, such as the Mirena or Jaydess, when youre diagnosed, you may be advised to have this removed.
Find out more about how breast cancer and its treatment can affect sex and intimacy and read our tips on how to manage these changes.
Recommended Reading: What Are The Chances Of Getting Breast Cancer Twice
Whats An Oncotype Dx Test
To decide whether or not you need chemotherapy, youll likely take an Oncotype DX test, which evaluates your risk factors and arrives at a recurrence number , which then falls somewhere on an Oncotype sliding scale. Heres how to interpret the numbers if you are a younger woman with breast cancer:
-
Recurrence Score of 0-15: The cancer has a low risk of recurrence. The benefits of chemotherapy likely will not outweigh the risks of side effects.
-
Recurrence Score of 16-20: The cancer has a low to medium risk of recurrence. The benefits of chemotherapy likely will not outweigh the risks of side effects.
-
Recurrence Score of 21-25: The cancer has a medium risk of recurrence. The benefits of chemotherapy are likely to be greater than the risks of side effects.
-
Recurrence Score of 26-100: The cancer has a high risk of recurrence. The benefits of chemotherapy are likely to be greater than the risks of side effects.
Treating Stage Iii Breast Cancer
In stage III breast cancer, the tumor is large or growing into nearby tissues , or the cancer has spread to many nearby lymph nodes.
If you have inflammatory breast cancer: Stage III cancers also include some inflammatory breast cancers that have not spread beyond nearby lymph nodes. Treatment of these cancers can be slightly different from the treatment of other stage III breast cancers. You can find more details in our section about treatment for inflammatory breast cancer.
There are two main approaches to treating stage III breast cancer:
Recommended Reading: Does Getting Hit In The Breast Cause Cancer
Cancer Originates From Normal Tissue
Major advances in human pathology and safety during surgery as well as progress in oncology marked the 19th century. For instance, in 1838, German pathologist Johannes Muller proposed that cancer cells developed from the blastema between the normal tissues and not from the lymphatic system, and later Rudolph Virchow demonstrated that tumors were composed of cells . It was during this time that hand-washing was promoted and the pasteurization technique was invented as a precautionary measure during surgery. Joseph Lister introduced the concept of surgical antisepsis using carbolic acid spray aseptic techniques were adopted for the first time by the Baltic German surgeon Ernst von Bergmann and surgical masks and sterile rubber surgical gloves were also introduced . However, a major progress in surgery occurred on October 16, 1846 when William T. G. Morton pioneered and publicly demonstrated the use of ether as anesthesia for surgery .
When Is Radiation Therapy Used
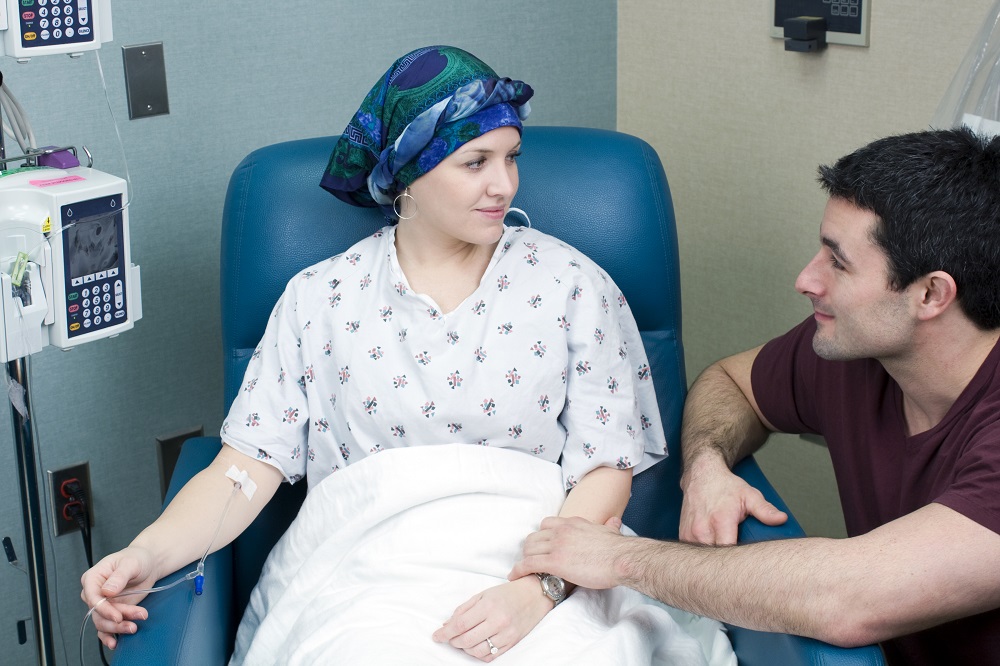
Radiation therapy can be used to treat all stages of breast cancer.
Pregnant women should not have radiation therapy because it can harm the unborn baby. Read about Treatment for Breast Cancer During Pregnancy.
Radiation therapy after lumpectomy
Radiation therapy is recommended for most people who have lumpectomy to remove breast cancer. Lumpectomy is sometimes called breast-conserving surgery. The goal of radiation after lumpectomy is to destroy any individual cancer cells that may have been left in the breast after the tumor was removed. This reduces the risk of the cancer coming back and the risk of passing away from breast cancer.
Heres a good analogy for understanding the role of radiation therapy after surgery:If you drop a glass on the kitchen floor, you must first sweep up all of the big pieces of glass and throw them away you can think of breast surgery in this way, says Marisa Weiss, M.D., founder and chief medical officer of Breastcancer.org and director of breast radiation oncology at Lankenau Medical Center. Radiation therapy is like vacuuming the area after you sweep, getting into the corners and under the furniture, to get rid of any tiny shards of glass that might be left behind.
Radiation therapy after mastectomy
Radiation therapy may be recommended after mastectomy to destroy any cancer cells that may be left behind after the surgery. During mastectomy, it’s difficult for surgeons to take out every cell of breast tissue.
Don’t Miss: How To Cure Breast Cancer With Baking Soda
Chemotherapy After Or Before Surgery
It’s fairly common for chemotherapy to be given after surgery, as soon as you recover. The time between surgery and chemotherapy depends on each person’s unique situation, so don’t worry if you start sooner or later than someone else. Doctors call this “adjuvant” chemotherapy because it’s given in addition to surgery, which is considered the primary treatment.
In some cases, chemotherapy is given before surgery to shrink the cancer so less tissue has to be removed. When chemotherapy is given before surgery, it’s called “neoadjuvant” chemotherapy. Only certain types of cancers respond well to chemotherapy before surgery.
Increased Risk Of Leukemia
Very rarely, certain chemo drugs can cause diseases of the bone marrow, such as myelodysplastic syndromes or even acute myeloid leukemia, a cancer of white blood cells. If this happens, it is usually within 10 years after treatment. For most women, the benefits of chemo in helping prevent breast cancer from coming back or in extending life are far likely to exceed the risk of this rare but serious complication.
Don’t Miss: Is Breast Cancer Curable In The 3 Stage
The Goals Of Chemotherapy
The goals of chemotherapy depend on the type of cancer and how far it has spread. Sometimes, the goal of treatment is to get rid of all the cancer and keep it from coming back. If this is not possible, you might receive chemotherapy to delay or slow cancer growth.
Delaying or slowing cancer growth with chemotherapy also helps manage symptoms caused by the cancer. Chemotherapy given with the goal of delaying cancer growth is sometimes called palliative chemotherapy.
The Bottom Line: Timely Treatment Is Better Than Delay
I realize that these two studies are about as close to Well, duh! studies as there are. Of course, delaying surgery for breast cancer is not a good thing. Of course, delaying chemotherapy when its indicated is also not a good thing. These are results that are not unexpected. However, these studies are still very important because they give us estimates of how much of a delay is safe and at what point delaying care starts to have a measurable impact on patient outcomes. Putting the results of these studies together suggests that its best to do surgery within about 60 days in patients not needing chemotherapy first, and that for patients with disease lacking the estrogen and progesterone receptor its best to start chemotherapy within 90 days of surgery.
We can thus reassure anxious patients who want their surgery tomorrow while at the same time tell patients balking at surgery or chemotherapy how long they can safely wait before the delay starts adversely affecting their chances of survival. Unfortunately, in my practice, due to the socioeconomic status of a lot of patients, by the time some of my patient see me its already been more than 30 days since their biopsy and diagnosis.
- Tagged in:alternative cancer cure testimonial, alternative medicine, breast cancer, chemotherapy, delay, disparities, quality improvement, surgery
Recommended Reading: Baking Soda And Breast Cancer
Breast Cancer Risk Factors
Although the Halsted operation was revolutionary, this surgical intervention was becoming controversial and losing popularity among some surgeons. In the mid-20th century there was greater awareness of the postoperative morbidity that included disfigurement of the chest, lymphedema of the arm and occasional irradiation-induced sarcomas. Some new breast cancer patients were inclined to choose alternative treatments and even some surgeons were becoming increasingly critical of radical mastectomy although it was considered to be far more successful than any other treatment at the time. The first half of the 20th century also saw an explosion of knowledge about the biology and epidemiology of breast cancer.
Survival Happens Every Day
These rough estimates for how long breast cancer takes to treat can be helpful to plan your life around treatment. More importantly, they provide a light at the end of the tunnel for you to focus on. However, for your daily sanity, it may be better to break down your treatment into smaller parts. Take it from one day to the next. Remember, every day you make it, youre already winning. These factors all affect how long breast cancer takes to treat.
Read Also: Did Anne Hathaway Have Breast Cancer
Survival And Time To Surgery
A 2016 study published in JAMA Oncology looked at data from over 115,000 people via the National Cancer Database . This study included people age 18 and older who were cared for at Commission on Cancer-accredited cancer centers across the United States.
All of the people had early stage breast cancer with surgery as their first treatment. They then looked at wait times to surgery and survival rates at five different intervals: a wait of less than 30 days, a wait time of 31 to 60 days, a wait time of 61 to 90 days, a wait time of 91 to 120 days, and a wait time of 121 to 180 days.
They found that for each 30-day interval of delay, survival rates decreased for people with stage I and stage II breast cancer. The conclusion was that although time is needed to discuss treatment options and prepare, earlier surgery is better.
Ancient Egypt And Greece

Origins of the medical papyri: Ancient Egyptians were the first to describe breast tumors around 3500 years ago in two distinct papyri: The Edwin Smith Surgical Papyrus and the Ebers Papyrus. The Edwin Smith Surgical Papyrus is regarded as one of the most important medical documents in the ancient Nile Valley. The papyrus document was produced in the Pyramid Age sometime between 3500 and 2500 BCE that is around the Stonehenge era . The Ebers Papyrus, was named after the Egyptologist George Ebers, who purchased it in 1872 and later published a facsimile with an English-Latin vocabulary of the document in 1875.
The Edwin Smith Papyrus: a) Case 39 of the original in hieratic. b) The corresponding modern scientific transcription into hieroglyphics. The images were cropped from the original publication by Breasted. They contain descriptions of tumors with prominent heads in the breast of the patient as transliterated in Harding’s publication in 2007. ).
Don’t Miss: Baking Soda And Honey For Cancer