Pten And Cowden Syndrome
Cowden syndrome is a rare autosomal dominant predisposition to both benign and malignant neoplasms. Breast cancer develops in 20%30% of carrier women. Other tumors seen among patients with Cowden syndrome include adenomas and follicular cell carcinomas of the thyroid gland, polyps and adenocarcinomas of the gastrointestinal tract, and ovarian cysts and carcinoma . Cowden syndrome is caused by germline mutations in the PTEN gene . PTEN, a tumor suppressor gene on 10q23.3 , is a dual-specificity phosphatase .
What Does Estrogen Do For Your Health
Before diving into its role in breast cancer, lets begin by looking at all the beautiful things estrogen does for us. Aside from all the ways it impacts reproductive health, from your monthly cycle to pregnancy, estrogen plays a positive role in functions like:
- Libido, fertility, and sexual health
- Healthy stress response
- Cognitive function
How Do Hormone Therapies Work
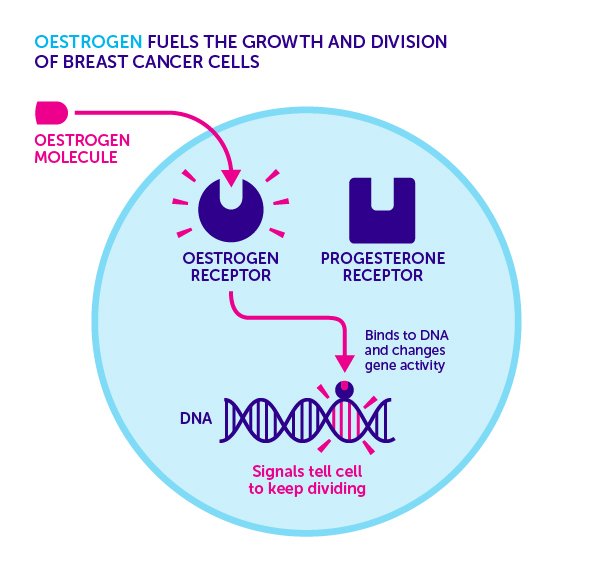
Hormone therapies slow or stop the growth of hormone receptor-positive tumors by preventing the cancer cells from getting the hormones they need to grow.
They work in a few ways:
- Some hormone therapies, such as tamoxifen, attach to the hormone receptor in the cancer cell and block estrogen from attaching to the hormone receptor.
- Some hormone therapies, such as aromatase inhibitors and ovarian suppression, lower the level of estrogen in the body so the cancer cells cant get the estrogen they need to grow.
Recommended Reading: What Are The Odds Of Surviving Breast Cancer
What Causes Her2 Positive Breast Cancer
The exact cause of HER2 positive breast cancer is not yet known, though researchers believe that environment, lifestyle and genetics may all play a role in the development of this malignancy. That said, HER2 positive breast cancer is not hereditary you cant inherit a bad HER2 gene from a parent or pass one on to a child.
You Have More Power Than You Have Been Told
You have more power over your risk of breast cancer than you think. There are many steps you can take to protect yourself. Each one of them has other positive domino effects for your hormonal balance and overall health:
1. Help with Estrogen Metabolism
If theres one trio of supplements I recommend for preventing breast cancer and promoting overall hormone health, its the combination of DIM, sulforaphane, and calcium d-glucarate. Heres a breakdown of these major estrogen metabolizers.
DIM: Also known as diindolylmethane, DIM is a compound generated when the body breaks down cruciferous vegetables such as broccoli, cabbage, and cauliflower. It is best known as a nutrient that supports healthy estrogen metabolism as well as the prevention of hormone-related cancers by its anti-estrogenic and anti-androgenic effects. It supports:
- Phase 1 liver detoxification
- The breakdown of estrogen into clean estrogens, not the antagonistic dirty ones
- A healthy balance of testosterone and estrogen by acting as an aromatase inhibitor, blocking some testosterone from converting to estrogen
- The cells from the damaging effects of oxidation
I personally use and recommend our DIM. The recommended dose is 100 mg to 200 mg per day.
I personally use and recommend our Brocco Power . The recommended dosage is 500 mg a day.
I personally use and recommend our Calcium-D-Glucarate. Recommended dosage of calcium d-glucarate ranges from 150 mg to 300 mg per day, taken with meals.
For Breast Protection:
Don’t Miss: Stage 3 Breast Cancer
Breast Cancer Research At Moffitt Cancer Center
Moffitt Cancer Center has been designated a Comprehensive Cancer Center by the National Cancer Institute, an achievement that speaks directly to our commitment to advancing research and treatment for this malignancy. We are researching the causes of HER2 positive breast cancer every day, and we wont be satisfied until there is a cure. To advance the treatment of this malignancy, Moffitt spearheads a robust clinical trials program where eligible patients can receive the latest breakthroughs in treatment before they are available elsewhere.
If you would like to learn more about the causes of HER2 positive breast cancer, or if you have been diagnosed with this malignancy and would like to explore the treatment options available to you at Moffitt, we encourage you to request an appointment. To do so, call or submit a new patient registration form. We accept patients with or without referrals.
- BROWSE
Pregnancy Childbearing And Breastfeeding
Lower age of first childbirth, compared to the average age of 24, having more children , and breastfeeding have all been correlated to lowered breast cancer risk in premenopausal women, but not postmenopausal women, in large studies. Women who give birth and breast-feed by the age of 20 may have even greater protection. In contrast, for instance, having the first live birth after age 30 doubles the risk compared to having first live birth at age less than 25. Never having children triples the risk. The studies have found that these risk factors become less material as a woman reaches menopause, i.e. that they affect risk of breast cancer prior to menopause but not after it. In balancing premenopausal reductions in risk from childbirth and lactation, it is important also to consider the risks involved in having a child.
Also Check: Effects Of Breast Cancer On A Person
Estrogen Exposure Over Time Is Linked To Breast Cancer
The longer your body is exposed to estrogen throughout your life, the more it appears to increase your risk for estrogen-related breast cancer. This helps explain why most breast cancer diagnoses occur later in life, after a lifetime of exposure to estrogen.
But it gets more interesting. Even though breast cancer risk generally increases as you get older, if you start your period later in life , your risk goes down simply because you had a few extra years without estrogen. The opposite seems true for women who go through menopause later, as more years of estrogen exposure may actually increase the risk for breast cancer.
See the connection? More estrogen equals more risk, according to current research.
What Is Her2 And What Does It Mean
HER2 is a protein that helps breast cancer cells grow quickly. Breast cancer cells with higher than normal levels of HER2 are called HER2-positive. These cancers tend to grow and spread faster than breast cancers that are HER2-negative, but are much more likely to respond to treatment with drugs that target the HER2 protein.
All invasive breast cancers should be tested for HER2 either on the biopsy sample or when the tumor is removed with surgery.
Also Check: Hormone Based Breast Cancer
How Is Hormone Therapy Used To Treat Breast Cancer
There are three main ways that hormone therapy is used to treat hormone-sensitive breast cancer:
Adjuvant therapy for early-stage breast cancer:Tamoxifen is FDA approved for adjuvant hormone treatment of premenopausal and postmenopausal women with ER-positive early-stage breast cancer, and the aromatase inhibitorsanastrozole, letrozole, and exemestane are approved for this use in postmenopausal women.
Research has shown that women who receive at least 5 years of adjuvant therapy with tamoxifen after having surgery for early-stage ER-positive breast cancer have reduced risks of breast cancer recurrence, including a new breast cancer in the other breast, and reduced risk of death at 15 years .
Until recently, most women who received adjuvant hormone therapy to reduce the chance of a breast cancer recurrence took tamoxifen every day for 5 years. However, with the introduction of newer hormone therapies , some of which have been compared with tamoxifen in clinical trials, additional approaches to hormone therapy have become common .
Some premenopausal women with early-stage ER-positive breast cancer may have ovarian suppression plus an aromatase inhibitor, which was found to have higher rates of freedom from recurrence than ovarian suppression plus tamoxifen or tamoxifen alone .
Men with early-stage ER-positive breast cancer who receive adjuvant therapy are usually treated first with tamoxifen. Those treated with an aromatase inhibitor usually also take a GnRH agonist.
Obesity And Lack Of Exercise
Gaining weight after menopause can increase a woman’s risk. A 2006 study found that putting on 9.9 kg after menopause increased the risk of developing breast cancer by 18%. Lack of exercise has been linked to breast cancer by the American Institute for Cancer Research.
Obesity has been linked to an increased risk of developing breast cancer by many scientific studies. There is evidence to suggest that excess body fat at the time of breast cancer diagnosis is associated with higher rates of cancer recurrence and death. Furthermore, studies have shown that obese women are more likely to have large tumors, greater lymph node involvement, and poorer breast cancer prognosis with 30% higher risk of mortality.
Weight gain after diagnosis has also been linked to higher rates of breast cancer recurrence or mortality although this finding is not consistent. Weight gain is often less severe with newer chemotherapy treatments but one study found a significant risk of breast cancer mortality in women who gained weight compared to those who maintained their weight. However, other cohort studies and recent clinical trials have not shown a significant relationship between weight gain after diagnosis and breast cancer mortality.
Don’t Miss: Terminal Breast Cancer Symptoms
Not All Estrogens Are Bad
Let me not vilify all estrogens, as they are not the same. There are 16 forms of estrogens but todays science has only gone deeper into understanding three estrogens: estrone , estradiol and estriol . Out of these three, estradiol tends to be the most aggressive estrogen that has been linked to breast cancer multiplication. In fact, estriol is a protective estrogen that is often prescribed for women with estrogen dominance.
Another thing I need you to know is that it is also certain metabolites that are broken down in the liver that can be antagonistic. In fact, one of the breast cancer risk tests used is a blood test called 2:16 hydroxy-estrone which measures the relationship between estrones metabolites to determine the risk factor. In my practice, I like to look at three markers to identify the risk factor of a women :
The first test can be ordered by your physician, while you can order the saliva test online from Canary Club. The urine tests need to be ordered by an integrative physician, one of whom you can find near you from the listing here .
How Her2 Status Affects Treatment
For more than 30 years, researchers have been studying HER2-positive breast cancer and ways to treat it.
Targeted therapies have now changed the outlook of stage 1, 2, and 3 breast cancers from poor to good.
While targeted therapies are part of the standard treatment for HER2-positive breast cancer, theyre only used occasionally in HER2-negative breast cancer.
Another difference between HER2-positive treatments and HER2-negative treatments is that HER2-negative treatments are often oral medications. HER2-positive treatments are usually administered intravenously or by injection.
For HER2-positive or HER2-negative breast cancers that are estrogen-positive or progesterone-positive, treatment with hormonal therapy may also be recommended.
Medications that may be used to treat HER2-negative breast cancers that are hormone-negative include:
- sacituzumab govitecan , an IV treatment
- talazoparib
Medications that may be used to treat HER2-negative breast cancers that are hormone-positive include:
- abemaciclib
- palbociclib
- ribociclib
Some of these medications are taken on their own, while others must be administered with other medications. Factors that affect your treatment regimen include whether:
- youve gone through menopause
- youve already received hormone therapy or chemotherapy
- you have certain gene mutations
Trastuzumab is a biologic therapy thats administered intravenously.
Other treatments for HER2-positive breast cancer include:
Recommended Reading: Estrogen Positive Her2 Negative Breast Cancer
Can You Reduce Your Risk Of Breast Cancer Related To Estrogen
The connection between estrogen and breast cancer is clear, so optimal levels are vital. I wish I could tell you exactly what to do to avoid a breast cancer diagnosis altogether, but of course, I cant because it’s an issue that’s too complex to offer that type of advice.
That said, there are things you can do to keep your estrogen in check:
Remember that estrogen helps us feel healthy and sexy. The key is maintaining balance with other hormones. Here are my top lifestyle habits that promote healthy estrogen metabolism.
- Maintain a healthy body weight. Remember that your fat tissue can make estrogen by converting androgens into estrogens. This means that as body fat increases, so does the amount of estrogen produced and circulated throughout your tissues.
Scientists estimatee that your risk for developing breast cancer jumps by 30% after menopause if your BMI is above 30. And being overweight appears to be linked to ER+ breast cancers, likely related to the increased estrogen production. While its much easier said than done to maintain body weight, the number one tip I advise for healthy weight is a healthy fiber intake. Try swapping your mindset from how many calories did I eat today to how much fiber from real, whole vibrant foods did I enjoy today?
- Keep xenoestrogens out of your kitchen. Chemicals like BPA, phthalates, and BHT all mimic estrogen in the body. They sneak into our kitchen via canned goods, plastic containers, and other food storage items.
What Happens If My Test Is Positive For Hereditary Breast Cancer Risk
If testing confirms you are at risk, your care provider can work with you on a plan to safeguard your health, which could include:
- High-risk evaluation and monitoring
- Screening schedules, including digital mammography and clinical breast exams
- Hormonal therapy medications designed to prevent the development of breast cancer
Preventive surgery, such as mastectomy with breast reconstruction, is necessary only for patients at very high risk for aggressive breast cancer.
A comprehensive breast center offers a safe and supportive environment where you can ask questions and get the best answers for you, Ninan says. Every patients decision about how to handle their risk of developing breast cancer is managed with sensitivity and an understanding about the complexity of these decisions.
Read Also: Cancer Stages 3
How Well Do Different Guidelines Identify Women With Inherited Mutations
The American Society of Breast Cancer Surgeons
ASBrS recommends testing for all women with breast cancer. An XRAY review of the ASBrS recommendations can be found here. Using ASBrS guidelines:
- According to these guidelines, in this study, all participants with mutations would be identified.
Pro: All women with mutations would be identified none would be missed.
Con: 3,666 women who did not have an inherited mutation were tested, which may have caused unnecessary cost, stress and anxiety.
The National Comprehensive Cancer Network
NCCN has a complex set of guidelines for genetic testing recommendations . Using current NCCN guidelines:
- 169 of the 3,907 participants had a genetic mutation in one of 9 actionable breast cancer genes and would qualify for genetic testing under NCCN guidelines.
- These 169 women represented 70% of 241 women with an inherited mutation.
Pro: Fewer women without inherited mutations were tested than under ASBrS guidelines and did not unnecessarily face the potential stress and anxiety of genetic testing.
Con: A large portion women with an inherited mutation were not identified, which prevented them from using this information to guide their treatment and surgical decisions.
Expanded NCCN guidelines
Signs Of Breast Cancer
Take time to get to know the normal look and feel of your breasts while showering, dressing or looking in the mirror so you can detect any changes that may indicate cancer such as:
- A lump, lumpiness or thickening.
- Changes to the nipple such as a change in shape, crusting, a sore or an ulcer, redness or a nipple that turns in when it used to stick out.
- Changes to the skin of the breast such as dimpling of the skin, unusual redness or other color changes.
- Change in the shape or size of the breast either an increase or decrease.
- Unusual discharge from the nipple without squeezing.
- Swelling or discomfort in the armpit.
- Persistent, unusual pain not related to your normal monthly cycle, which remains after a menstrual period and occurs in one breast only.
Though not necessarily cancer, these signs should be checked by your doctor without delay.
Other resources Ive put together for you:
Don’t Miss: Hormone Receptor Positive Metastatic Breast Cancer
Load Up On Fruits And Vegetables
The fiber, antioxidants and other phytonutrients in fruits and vegetables have the potential to reduce cancer growth, although research results have been mixed on their role in breast cancer. In fact, data from the Womens Healthy Eating and Living trial, a study of more than 3,000 women with a history of early-stage breast cancer, failed to show a diet rich in these foods reduced the rate of recurrence.
However, data from the Womens Health Observational Study , a trial of nearly 94,000 postmenopausal women with a history of early-stage breast cancer, linked a higher intake of carotenoid-rich fruits and vegetables, such as leafy greens, carrots, sweet potatoes and nectarines, to a lower recurrence of ER-positive breast cancer.
In addition, a 2008 study in the Journal of Clinical Oncology of nearly 1,500 women with early-stage breast cancer found those who ate at least five daily servings of fruits and vegetables and exercised 30 minutes daily cut their risk of death in half over a 10-year period. This benefit was greatest among women with ER-positive breast cancer.
Eating a diet rich in fruits and vegetables can do more than cut cancer risk. A plant-centered, high-fiber diet can also reduce the risk of other health problems that breast cancer patients may face, such as obesity and cardiovascular disease. Consequently, women with breast cancer are encouraged to include a variety of colorful fruits and vegetables in their daily diets.