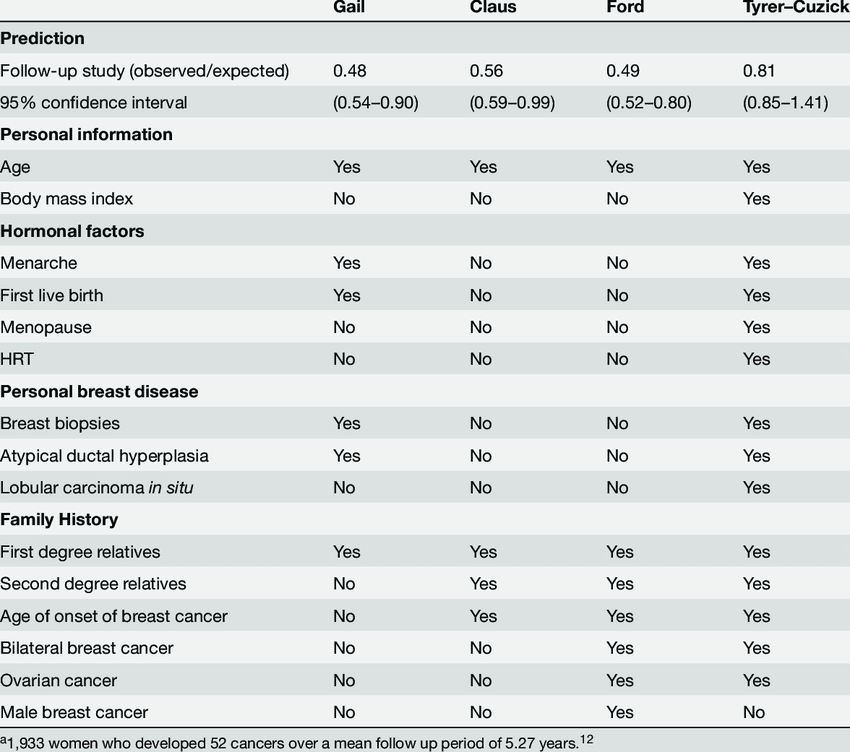
Differences In The Models
In instances of predicting risk in women who have a higher familial cancer history, the Tyrer-Cuzick is likely the most appropriate choice. This is because the Gail model has a tendency to underestimate risk of developing breast cancer in women with familial history of cancer. The findings of both models show a significant risk increase for individuals who are obese in any age group. For example, the risk rises from 0.8% for the 35-39 age group to 1.5% for 65-69 years. However, the Tyrer-Cuzick model presented the highest degree of accuracy for potentially developing breast cancer.
Pharmacologic Interventions For Breast Cancer Risk Reduction
Guidelines for pharmacologic intervention in women who are at increased risk for breast cancer, but do not have a personal history of breast cancer, have been issued by the American Society of Clinical Oncology and the U.S. Preventive Services Task Force . The guidelines differ in their classification of increased risk and in their inclusion of women with lobular carcinoma in situ .
Before Your Breast Imaging You Should Know:
When you arrive for your breast imaging, its essential that you have your script with you. If you dont have your script, please call the provider who ordered your imaging to ensure that one can be faxed to our office at 716.649.9005 before your appointment.
During your study, your technologist will position you, compress your breast, and take images from different angles. The technologist will view the images of your breasts at the computer workstation to ensure quality images have been captured for review. A radiologist will then examine the images and will send a copy of your results to the provider who ordered your breast imaging. In most cases, you will also be told of your imaging results while at our offices . If there is need for further testing, we will do our best to accommodate it while you are in for your scheduled appointment.
You May Like: What Is Ductal Breast Cancer
Include Breast Density As A Risk Factor
There is overwhelming evidence that breast density is an independent risk factor for the development of breast cancer.5, 6 In May of this year, the first validation paper was published showing the value breast density added to the Tyrer-Cuzick risk model.7 The results found that inclusion of breast density, with other classical risk factors, increased the number of women accurately identified at higher and lower risk of breast cancer.
Two clinically practical breast density measurements validated for use in TCv8 are:
1) % Volpara Volumetric Density
The validated density input for the use of VBD% is the average of the left and right breast VBD% as measured by VolparaDensity.
2) BI-RADS® ATLAS Density
The validated density input for the use of BI-RADS ATLAS Density is the visual assessment using BI-RADS 4th edition guidelines . The assessment should then be mapped to the BI-RADS 5th edition equivalent before entering the density grade into the model.
Using a validated measure of breast density adds significant value to the TCv8 risk assessment model.
Use Of Biomarkers To Guide Adjuvant Systemic Therapy
A 2016 guideline from the American Society of Clinical Oncology advises that the only biomarkers that can guide choices of specific treatment regimens in breast cancer are as follows :
- Estrogen receptor
- Human epidermal growth factor receptor 2
A 2022 update of the ASCO guideline regarding further biomarker use includes the following recommendations :
Also Check: Is Radiation For Breast Cancer Dangerous
What Is The Tyrer
This risk assessment tool is designed to provide women with figures related to their chances of developing breast cancer within the next ten years and throughout their lifetime. It figures the likelihood of having some specific gene mutations known for causing cancer development. Its important to note that this risk assessment tool cant predict if the patient develops cancer, only the potential chance by giving a percentage figure based on personal details including family history and lifestyle. The figures given at the test completion are the percentages of risk of development over a lifetime and within the next 10 years.
The average percentage for risk is currently less than a 15% score for the Tyrer-Cuzik model. Intermediate risk is between 15% and 19%. Anyone who is classified over 20% is considered to be at high risk of developing breast cancer. There is an online version of this risk assessment tool that provides this information conveniently.
Fernanda Sales Luiz Vianna
1 Programa de Pós-Graduação em Epidemiologia, UniversidadeFederal do Rio Grande do Sul, Porto Alegre, RS, Brazil
2 Programa de Pós-Graduação em Genética e Biologia Molecular,Universidade Federal do Rio Grande do Sul, Porto Alegre, RS, Brazil
3 Laboratório de Medicina Genômica, Centro de PesquisaExperimental do Hospital de Clínicas de Porto Alegre, Porto Alegre, Brazil
You May Like: What Is Er And Pr Positive In Breast Cancer
Additional File : Supplementary Materials
: Comparative validation of the BOADICEA and Tyrer- Cuzick breast cancer risk models incorporating classical risk factors and polygenic risk in a population-based prospective cohort of women of European ancestry.Additional details on the definition of study follow-up, sources of genotype data, risk factors in BOADICEA and Tyrer-Cuzick models, model validation methods are given. Supplementary Fig. 1. shows the study design in the validation cohort. Supplementary Fig. 2. shows a comparative validation of Tyrer-Cuzick model with and without PRS in the Generations Study. Supplementary Table 1 shows the risk factor distribution in the Generation Study. Figure . Calibration and discrimination of five-year risk predictions of breast cancer for women younger than 50years in the nested case-control sample of the Generations Study cohort with risk categories based on deciles of predicted five-year absolute risk. Figure . Calibration and discrimination of five-year risk predictions of breast cancer for women aged 50years or older in the nested case-control sample of the Generations Study cohort with risk categories based on deciles of predicted five-year absolute risk.
Dont Miss: Does Breast Cancer Spread To Thyroid
Understand How The Different Breast Density Measurements Impact Risk Scores
There are key differences in the two methods of breast density measurement validated for use in Tyrer-Cuzick risk model:
| Automated | VisualACR BI-RADS 4th Edition |
| Provides a precise measurement of density, on a continuous spectrum, that generates a risk score specific to an individuals unique density measurement. | Provides a 4-step measurement of density that may result in an under- or overestimation of an individuals breast density risk. |
| Is an objective, reproducible measurement of density that has excellent agreement with MRI.8 | Is a subjective visual measurement that is dependent on radiologist experience for accuracy.9 |
Example:
Three women walk into a breast screening clinic with exactly the same risk factors and a visual breast density of BI-RADS 3, which we would enter as C. What happens when their unique volumetric breast density % is entered into TCv8 as opposed to the BI-RADs score?
Risk factors
* > 20% lifetime risk indicates that this woman may benefit from additional supplemental screening.10
Volumetric breast density can give a more accurate reflection of risk because of the continuous nature of both the risk model and density calculation.
Read Also: Taking Collagen After Breast Cancer
Q3 What Does It Mean To Have Dense Breast Tissue And Why Does It Matter For My Tyrer
Breast cancer research and advances in risk assessment have shown that having dense breasts is a contributing factor in determining a womans risk of breast cancer. Dense breast tissue refers to the appearance of breast tissue on a mammogram and the makeup of supportive and fatty tissue in the breast. The more fatty tissue, the less dense the breast is. Dense breast are common and can be caused by simply being younger, having a lower body mass index, or taking hormone therapy for menopause researchers are still studying why some women have dense breast and other do not. Non-dense tissue appears dark and transparent, whereas dense breast tissue appears as solid white area on a mammogram the solid white area can make it hard for radiologists to accurately analyze the image with a mammogram, so your provider may recommend supplemental imaging, like a breast ultrasound or other recommendations, to ensure no cancers are missed. Having dense breast alone is not cause for concern, and you should speak with your doctor about your breast density and how it affects your risk status.
Family History And Genetic Factors
A family history of breast cancer in a first-degree relative is the most widely recognized breast cancer risk factor, but only 5-10% of women diagnosed with breast cancer have a known genetic predisposition. Women with a family history of breast cancer in a mother or sister have a 1.5-3 fold increase in the risk of developing breast cancer.
Family history of breast cancer is a heterogeneous risk factor that depends on the number of family members affected and the age at diagnosis, as well as the number of unaffected women in the pedigree. Even in the absence of a known genetic risk factor, the presence of a family history may suggest the presence of an unknown genetic risk, or a shared environmental risk.
A family history of ovarian cancer in a first-degree relative, especially if the disease occurred at an early age , has been associated with an increased risk of breast cancer risk.
The family history characteristics that suggest increased risk of cancer are summarized as follows :
- One or more relatives with breast or ovarian cancer
- Breast cancer occurring in an affected relative younger than 50 years
- Male relatives with breast cancer
- BRCA1 and BRCA2 mutations
- Ataxia-telangiectasia heterozygotes
- Ashkenazi Jewish descent (2 times greater risk independent of BRCA positivity
- Malignant melanoma
Other rare genetic disorders, such as Peutz-Jeghers syndrome and hereditary nonpolyposis colorectal carcinoma , are associated with an increased risk of breast cancer.
You May Like: Can You Get Breast Cancer From Breast Implants
Breast Cancer Risk Models That Include Breast Density
Breast Density Measures Improve Tyrer
Breast cancer risk-stratification models can help radiologists identify women who may benefit from additional imaging exams as well as screening mammography and implementing other preventive strategies. An international, multi-institutional team of breast imaging specialists hypothesized that adding breast density to an established risk-stratification model would increase its accuracy. Their research using the Tyrer-Cuzick tool, published online May 11, 2019 in the Journal of Breast Imaging, confirmed their hypothesis.
The Tyrer-Cuzick model is used to calculate the likelihood of carrying the BRCA1 or BRCA2 mutations, and estimates the likelihood of a woman developing invasive breast cancer within 10 years and over the course of her lifetime. It estimates risk based on age, body mass index, age at menarche, obstetric history, age at menopause, family history, use of hormone replacement therapy, and history of ovarian cancer and/or benign breast conditions that increase breast cancer risk, such as hyperplasia or atypical hyperplasia. A recent British study from the Centre for Cancer Prevention of Queen Mary University in London determined that this long-term risk assessment tool has been accurate for at least 19 years.1
They also verified that women in the highest Bi-RADS density category were three times more likely to develop breast cancer than were women with predominantly fatty breasts.
Also Check: What Percentage Of Triple Negative Breast Cancer Returns
How To Measure Your Risk Of Breast Cancer
Every woman has some risk of breast cancer. In the U.S., 1 in 8 women will be diagnosed with invasive breast cancer over the course of her lifetime. This means the average womans breast cancer risk is 12-13%. A mans lifetime risk, by comparison, is much lower at 1 in 833 far less than 1%.
Just as there are factors that INCREASE the risk of breast cancer, there are ways to REDUCE your risk.
The starting point can be assessing YOUR PERSONAL RISK of breast cancer. Thankfully, there is a survey tool that can calculate a womans risk of developing breast cancer in her lifetime.
There are two breast cancer risk assessment tools that doctors use to calculate a womans risk of breast cancer:
- breast ultrasound
Recommendations For Women Based On Their Risk Assessment
With the goal of providing personalized medicine, Providence Imaging Center has added the Tyrer-Cuzick risk assessment tool as a complementary addition to our array of breast cancer screening and diagnostic services.
The Tyrer-Cuzik model incorporates a comprehensive set of variables to assess a womans lifetime risk of breast cancer. It identifies women at greater than average risk of breast cancer who could benefit from supplemental screening with breast MRI or breast ultrasound. The data collected also identifies families at high risk of hereditary cancer who could benefit from a genetics consultation.
The patients lifetime risk calculation will be documented on the mammogram report. Breast cancer screening recommendations for each risk category are listed below:
Average Risk less than 15%Continued annual screening mammography is recommended. Screening with tomosynthesis is preferred for women with heterogeneously dense or extremely dense breast tissue.
Intermediate Risk 15 to 19%Supplemental screening could be considered for women that fall in this risk category with heterogeneously dense or extremely dense breast tissue, after discussion regarding the risks of false positive and insurance issues. This risk group has insufficient evidence to recommend for or against supplemental screening. Screening breast MRI or ultrasound may be appropriate for selected patients.
Also Check: Ct Simulation For Breast Cancer
What Gets Stored In A Cookie
This site stores nothing other than an automatically generated session ID in the cookie no other information is captured.
In general, only the information that you provide, or the choices you make while visiting a web site, can be stored in a cookie. For example, the site cannot determine your email name unless you choose to type it. Allowing a website to create a cookie does not give that or any other site access to the rest of your computer, and only the site that created the cookie can read it.
Recommended Reading: Are There Different Types Of Chemotherapy For Breast Cancer
American Society Of Clinical Oncology
- For premenopausal with increased risk for breast cancer, offer tamoxifen to reduce the risk of invasive estrogen receptor positive breast cancer
- In postmenopausal women, endocrine therapy options include anastrozole , exemestane , raloxifene , or tamoxifen .
- Health care providers should discuss pharmacologic breast cancer risk reduction with women aged 35 years or older without a personal history of breast cancer who are at increased risk of developing invasive breast cancer.
Tamoxifen
ASCO guidelines recommend discussing use of tamoxifen, 20 mg per day orally for 5 years, as an option to reduce the risk of invasive breast cancer, specifically ER-positive breast cancer, in women 35 years of age or older who are premenopausal or postmenopausal and have a 5-year projected absolute breast cancer risk 1.66% or have LCIS. Risk reduction benefit continues for at least 10 years.
ASCO guidelines advise that tamoxifen not be used in the following cases :
- In women with a history of deep vein thrombosis, pulmonary embolus, stroke, or transient ischemic attack or during prolonged immobilization
- In combination with hormone therapy
- In women who are pregnant, may become pregnant, or are nursing mothers
Raloxifene
ASCO guidelines advise that raloxifene not be used in the following cases :
- For breast cancer risk reduction in premenopausal women
- In women with a history of deep vein thrombosis, pulmonary embolus, stroke, or transient ischemic attack or during prolonged immobilization
Recommended Reading: Does Breast Cancer Start In The Armpit
Which Risk Model To Use Clinical Implications Of The Acs Mri Screening Guidelines
Corresponding Author:Corresponding Author:
Elissa M. Ozanne, Brian Drohan, Phil Bosinoff, Alan Semine, Michael Jellinek, Claire Cronin, Frederick Millham, Dana Dowd, Taryn Rourke, Caroline Block, Kevin S. Hughes Which Risk Model to Use? Clinical Implications of the ACS MRI Screening Guidelines. Cancer Epidemiol Biomarkers Prev 1 January 2013 22 : 146â149.
Factors That Affect Your Risk Of Breast Cancer
The following factors can affect your personal risk of breast cancer. Your physician will ask about these factors in helping you gauge your risk.
- Your age and family history of cancer
- Your personal history of breast cancer
- Prior radiation to chest or face
- Certain breast changes
- If and when you were pregnant and how many children you had
- Breastfeeding history
- Menstrual history, starting age and menopause age
- Using hormone replacements
Don’t Miss: Can An Xray Show Breast Cancer
National Comprehensive Cancer Network
The NCCN guidelines recommend that SLNB should be performed and is the preferred method of axillary lymph node staging if the patient is an appropriate candidate for SLNB. Candidates include patients who are clinically node negative at the time of breast cancer diagnosis, with or without 12 suspicious nodes on imaging, and for whom no preoperative systemic therapy is planned.
If the sentinel lymph node is negative, no further axillary surgery is a category 1 recommendation. The NCCN recommends axillary dissection level I/II if the sentinel node is not identified or if the sentinel node is positive but the patient fails to meet all the following criteria:
- Whole-breast radiation therapy planned
- No preoperative chemotherapy
The NCCN recommends fine needle aspiration or core biopsy for patients whose breast cancer has any of the following characteristics:
- Clinically node positive at time of diagnosis or
- T2 or N1 and with preoperative systemic therapy planned or
If FNA or core biopsy results are negative, the NCCN recommends SLNB. For those with positive results, the NCCN recommends axillary dissection I/II, although SLNB may be considered in selected cases .
The NCCN guidelines state that lymph node dissection is optional in the following cases: