Special Invasive Breast Cancers And Carcinoma In Situ
Inflammatory breast cancer is an aggressive locally advanced breast cancer.
The main symptoms of IBC are swelling and redness in the breast. Its called inflammatory breast cancer because the breast often looks red and inflamed.
About 1-5 percent of breast cancers are IBC .
Learn more about IBC.
Paget disease of the breast is a rare carcinoma in situ in the skin of the nipple or in the skin closely surrounding the nipple. Its usually found with an underlying breast cancer.
About 1-4 percent of breast cancers also involve Paget disease of the breast .
|
Susan G. Komen® Support Resources |
|
What Is Inflammatory Breast Cancer
As its name suggests, inflammatory breast cancer often causes the breast to become red, swollen, and inflamed. Some women with IBC also notice thickened or discolored breast skin with tiny dimples, puckers, or ridges that make it look like an orange peel. While the symptoms may sound like an infection, the real culprit is cancer that is blocking lymphatic vessels in the skin and breast tissue, causing a buildup of fluid and, in some cases, pain, discoloration, and sudden swelling of the breast. Also called inflammatory breast carcinoma or locally advanced breast cancer, IBC can spread quickly, making prompt diagnosis and treatment essential.
Breast Cancer Cell Lines
Part of the current knowledge on breast carcinomas is based on in vivo and in vitro studies performed with cell lines derived from breast cancers. These provide an unlimited source of homogenous self-replicating material, free of contaminating stromal cells, and often easily cultured in simple standard media. The first breast cancer cell line described, BT-20, was established in 1958. Since then, and despite sustained work in this area, the number of permanent lines obtained has been strikingly low . Indeed, attempts to culture breast cancer cell lines from primary tumors have been largely unsuccessful. This poor efficiency was often due to technical difficulties associated with the extraction of viable tumor cells from their surrounding stroma. Most of the available breast cancer cell lines issued from metastatic tumors, mainly from pleural effusions. Effusions provided generally large numbers of dissociated, viable tumor cells with little or no contamination by fibroblasts and other tumor stroma cells.Many of the currently used BCC lines were established in the late 1970s. A very few of them, namely MCF-7, T-47D, MDA-MB-231 and SK-BR-3, account for more than two-thirds of all abstracts reporting studies on mentioned breast cancer cell lines, as concluded from a Medline-based survey.
Metabolic markers
Read Also: Stage 3 Cancer In Lymph Nodes
Estrogen And Breast Cancer
The molecular form for one type of estrogenA female sex hormone that is primarily produced by the ovaries. Its primary function is to regulate the menstrual cycle and assist in the production of secondary sex characteristics such as breasts. It may even play a role in the production of cancer cells in the breast tissue. called estriol. High levels of estrogen in the body have been shown to be a risk factorAnything that increases or decreases a persons chance of developing a disease. for breast cancer.
High estrogen levels in the body are believed to dramatically increase our risk of breast cancer. It is therefore worth understanding what estrogen is and how you can control your estrogen level at the same time as other breast cancer risk factors.
Ductal Carcinoma In Situ
DCIS is the most common type of noninvasive breast cancer, with about 60,000 new cases diagnosed in the United States each year. About one in every five new breast cancer cases is ductal carcinoma in situ.
Also called intraductal carcinoma or stage 0 breast cancer, its considered a noninvasive breast cancer. With DCIS, abnormal and cancerous cells havent spread from the ducts into nearby breast tissue nor anywhere else, such as the lymph nodes.
DCIS is divided into several subtypes, mainly according to the appearance of the tumor. These subtypes include micropapillary, papillary, solid, cribriform and comedo.
Patients with ductal carcinoma in situ are typically at higher risk for seeing their cancer return after breast cancer treatment, although the chance of a recurrence is less than 30 percent. Most recurrences occur within five to 10 years after the initial breast cancer diagnosis and may be invasive or noninvasive. DCIS also carries a heightened risk for developing a new breast cancer in the other breast. A recurrence of ductal carcinoma in situ would require additional treatment.
The type of therapy selected may affect the likelihood of recurrence. Treating DCIS with a lumpectomy , and without radiation therapy, carries a 25 percent to 35 percent chance of recurrence. Adding breast cancer radiation therapy to the treatment decreases this risk to about 15 percent. Currently, the long-term survival rate for women with ductal carcinoma in situ is nearly 100 percent.
Recommended Reading: Honey And Baking Soda Cancer Treatment
Signs And Symptoms Of Breast Cancer
In its early stages, breast cancer may not cause any symptoms. In many cases, a tumor may be too small to be felt, but an abnormality can still be seen on a mammogram.
If a tumor can be felt, the first sign is usually a new lump in the breast that was not there before. However, not all lumps are cancer.
Each type of breast cancer can cause a variety of symptoms. Many of these symptoms are similar, but some can be different. Symptoms for the most common breast cancers include:
- a breast lump or tissue thickening that feels different than surrounding tissue and has developed recently
- breast pain
- changes to the appearance of the skin on your breasts
- a lump or swelling under your arm
If you have any of these symptoms, it doesnt necessarily mean you have breast cancer. For instance, pain in your breast or a breast lump can be caused by a benign cyst.
Still, if you find a lump in your breast or have other symptoms, you should see your doctor for further examination and testing.
Expert Review And References
- American Cancer Society. Breast Cancer. 2015: .
- Foxson SB, Lattimer JG & Felder B. Breast cancer. Yarbro, CH, Wujcki D, & Holmes Gobel B. . Cancer Nursing: Principles and Practice. 7th ed. Sudbury, MA: Jones and Bartlett 2011: 48: pp. 1091-1145.
- Martini FH, Timmons MJ, Tallitsch RB. Human Anatomy. 7th ed. San Francisco: Pearson Benjamin Cummings 2012.
- Morrow M, Burstein HJ, and Harris JR. Malignant tumors of the breast. DeVita VT Jr, Lawrence TS, & Rosenberg SA. Cancer: Principles and Practice of Oncology. 10th ed. Philadelphia: Wolters Kluwer Health/Lippincott Williams & Wilkins 2015: 79: 1117-1156.
Don’t Miss: Metastatic Breast Cancer Mbc
Occupational Exposure And Safe Handling
In the 1970s, antineoplastic drugs were identified as hazardous, and the has since then introduced the concept of after publishing a recommendation in 1983 regarding handling hazardous drugs. The adaptation of federal regulations came when the U.S. first released its guidelines in 1986 and then updated them in 1996, 1999, and, most recently, 2006.
The has been conducting an assessment in the workplace since then regarding these drugs. Occupational exposure to antineoplastic drugs has been linked to multiple health effects, including infertility and possible carcinogenic effects. A few cases have been reported by the NIOSH alert report, such as one in which a female pharmacist was diagnosed with papillary transitional cell carcinoma. Twelve years before the pharmacist was diagnosed with the condition, she had worked for 20 months in a hospital where she was responsible for preparing multiple antineoplastic drugs. The pharmacist didn’t have any other risk factor for cancer, and therefore, her cancer was attributed to the exposure to the antineoplastic drugs, although a cause-and-effect relationship has not been established in the literature. Another case happened when a malfunction in biosafety cabinetry is believed to have exposed nursing personnel to antineoplastic drugs. Investigations revealed evidence of genotoxic biomarkers two and nine months after that exposure.
How Much Do Tamoxifen And Raloxifene Lower The Risk Of Breast Cancer
Multiple studies have shown that both tamoxifen and raloxifene can reduce the risk of developing estrogen receptor-positive breast cancer in healthy postmenopausal women who are at high risk of developing the disease. Tamoxifen lowered the risk by 50 percent. Raloxifene lowered the risk by 38 percent. Overall, the combined results of these studies showed that taking tamoxifen or raloxifene daily for five years reduced the risk of developing breast cancer by at least one-third. In one trial directly comparing tamoxifen with raloxifene, raloxifene was found to be slightly less effective than tamoxifen for preventing breast cancer.
Both tamoxifen and raloxifene have been approved for use to reduce the risk of developing breast cancer in women at high risk of the disease. Tamoxifen is approved for use in both premenopausal women and postmenopausal women . Raloxifene is approved for use only in postmenopausal women.
Less common but more serious side effects of tamoxifen and raloxifene include blood clots to the lungs or legs. Other serious side effects of tamoxifen are an increased risk for cataracts and endometrial cancers. Other common, less serious shared side effects of tamoxifen and raloxifene include hot flashes, night sweats, and vaginal dryness.
Don’t Miss: How Bad Is Stage 3 Cancer
How Is Breast Cancer Treated
If the tests find cancer, you and your doctor will develop a treatment plan to eradicate the breast cancer, to reduce the chance of cancer returning in the breast, as well as to reduce the chance of the cancer traveling to a location outside of the breast. Treatment generally follows within a few weeks after the diagnosis.
The type of treatment recommended will depend on the size and location of the tumor in the breast, the results of lab tests done on the cancer cells, and the stage, or extent, of the disease. Your doctor will usually consider your age and general health as well as your feelings about the treatment options.
Breast cancer treatments are local or systemic. Local treatments are used to remove, destroy, or control the cancer cells in a specific area, such as the breast. Surgery and radiation treatment are local treatments. Systemic treatments are used to destroy or control cancer cells all over the body. Chemotherapy and hormone therapy are systemic treatments. A patient may have just one form of treatment or a combination, depending on her individual diagnosis.
Life Style And Dietary Cause
Sedentary life style, high dietary intake of fat obesity particularly in postmenopausal women may cause breast cancer. The use of alcohol is also another one cause of breast cancer. The risk increases with the amount of alcohol consumed. Women who consume two to five alcoholic beverages per day have a risk about one and a half times that of nondrinkers for the development of breast cancer.
Don’t Miss: Stage 3 Aggressive Breast Cancer
Low Expression Of Brca1 In Breast And Ovarian Cancers
BRCA1 expression is reduced or undetectable in the majority of high grade, ductal breast cancers. It has long been noted that loss of BRCA1 activity, either by germ-line mutations or by down-regulation of gene expression, leads to tumor formation in specific target tissues. In particular, decreased BRCA1 expression contributes to both sporadic and inherited breast tumor progression. Reduced expression of BRCA1 is tumorigenic because it plays an important role in the repair of DNA damages, especially double-strand breaks, by the potentially error-free pathway of homologous recombination. Since cells that lack the BRCA1 protein tend to repair DNA damages by alternative more error-prone mechanisms, the reduction or silencing of this protein generates mutations and gross chromosomal rearrangements that can lead to progression to breast cancer.
Mutations And Cancer Risk
Certain variations of the BRCA1 gene lead to an increased risk for breast cancer as part of a hereditary breastovarian cancer syndrome. Researchers have identified hundreds of mutations in the BRCA1 gene, many of which are associated with an increased risk of cancer. Females with an abnormal BRCA1 or BRCA2 gene have up to an 80% risk of developing breast cancer by age 90 increased risk of developing ovarian cancer is about 55% for females with BRCA1 mutations and about 25% for females with BRCA2 mutations.
These mutations can be changes in one or a small number of DNA base pairs , and can be identified with PCR and DNA sequencing.
In some cases, large segments of DNA are rearranged. Those large segments, also called large rearrangements, can be a deletion or a duplication of one or several exons in the gene. Classical methods for mutation detection are unable to reveal these types of mutation. Other methods have been proposed: traditional quantitative PCR,multiplex ligation-dependent probe amplification , and Quantitative Multiplex PCR of Short Fluorescent Fragments . Newer methods have also been recently proposed: heteroduplex analysis by multi-capillary electrophoresis or also dedicated oligonucleotides array based on comparative genomic hybridization .
Some results suggest that hypermethylation of the BRCA1 promoter, which has been reported in some cancers, could be considered as an inactivating mechanism for BRCA1 expression.
Recommended Reading: Invasive Ductal Carcinoma Symptoms
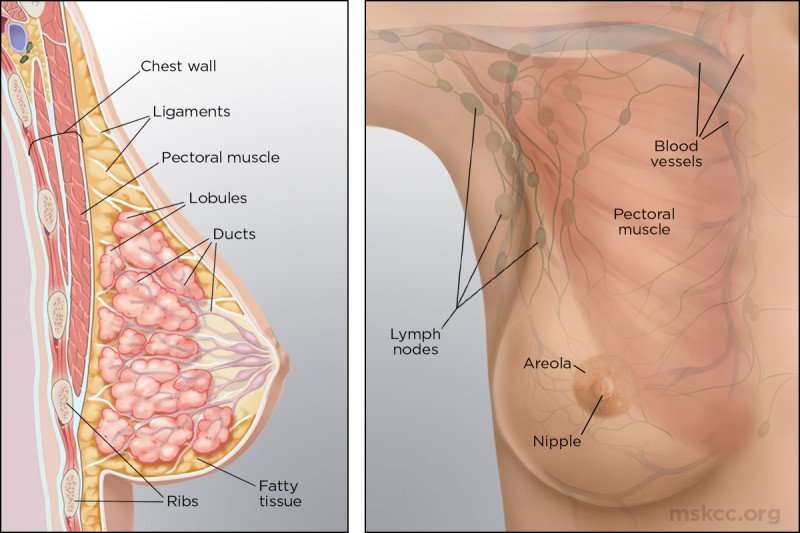
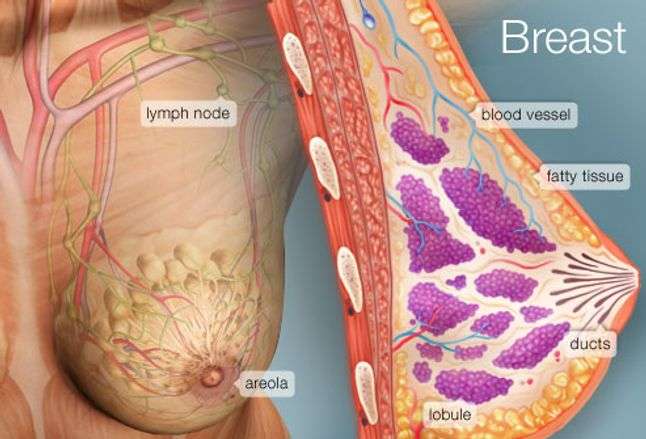
What Does A Breast Look Like On The Inside
Breasts are made up of lobules and ducts surrounded by fatty and connective tissue:
- lobules produce breast milk
- ducts carry milk to the nipple.
| Illustration of a woman’s breast including showing ductal carcinoma in situ & invasive breast cancer |
Close to the breasts are a number of lymph nodes. These are part of the lymphatic system and help to protect the body from infection. The closest lymph nodes to the breast are in the armpit . There are also lymph nodes under the breastbone and in the neck .
Different Types Of Aggressive Breast Cancer Identified
Media Inquiries
Vanderbilt-Ingram Cancer Center researchers have identified six subtypes of an aggressive and difficult-to-treat form of breast cancer, called triple-negative breast cancer .
In the July issue of the Journal of Clinical Investigation, Cancer Center Director Jennifer Pietenpol, and colleagues describe the molecular features of these six distinct subtypes and identify chemotherapies to which the different subtypes respond in cultured cells and animal tumor models. Knowing the specific subtype could help physicians determine which therapies would work best in patients with TNBC and also inform the discovery and development of new drugs to treat this form of breast cancer, the authors suggest.
You May Like: What Stage 3 Cancer Means
What Is Stage 3 Breast Cancer
Also known as locally advanced breast cancer, the tumor in this stage of breast cancer is more than 2 inches in diameter across and the cancer is extensive in the underarm lymph nodes or has spread to other lymph nodes or tissues near the breast. Stage 3 breast cancer is a more advanced form of invasive breast cancer. At this stage, the cancer cells have usually not spread to more distant sites in the body, but they are present in several axillary lymph nodes. The tumor may also be quite large at this stage, possibly extending to the chest wall or the skin of the breast.
Stage 3 breast cancer is divided into three categories:
Stage 3A: One of the following is true:
- No tumor is found in the breast, but cancer is present in axillary lymph nodes that are attached to either other or other structures, or cancer may be found in the lymph nodes near the breast bone, or
- The tumor is 2 cm or smaller. Cancer has spread to axillary lymph nodes that are attached to each other or other structures, or cancer may have spread to lymph nodes near the breastbone, or
- The tumor is 2 cm to 4 cm in size. Cancer has spread to axillary lymph nodes that are attached to each other or to other structures, or cancer may have spread to lymph nodes near the breast bone, or
- The tumor is larger than 5 cm. Cancer has spread to axillary lymph nodes that may be attached to each other or to other structures, or cancer may have spread to lymph nodes near the breastbone.
Stage 3C:
What Is Invasive Lobular Carcinoma
Invasive lobular carcinoma is a cancer that starts in the breasts lobules and invades surrounding tissue. ILC is the second most common form of invasive breast cancer, accounting for 10 to 15% of breast cancer cases. ILC doesnt always form a lump, but women who have it may notice a thick or full area that doesnt feel like the rest of the breast.
You May Like: Difference Between Stage 3 And 4 Cancer
Brain And Spinal Cord Tumors
There are different types of brain and spinal cord tumors. These tumors are named based on the type of cell in which they formed and where the tumor first formed in the central nervous system. For example, an astrocytic tumor begins in star-shaped brain cells called astrocytes, which help keep nerve cells healthy. Brain tumors can be benign or malignant .