Surgical Removal Of The Ovaries
The operation to remove the ovaries is called oophorectomy. Surgical removal of the ovaries is a permanent way to reduce the levels of oestrogen.
It is a very effective treatment to stop early breast cancer returning or to slow the progress of metastatic cancer. This can also reduce the risk of developing ovarian cancer.
Surgery to remove the ovaries can be done with keyhole surgery or with an open operation .
Your surgeon will discuss with you the pros and cons of these different techniques. Oophorectomy is done under a general anaesthetic .
Usually the fallopian tubes are also removed but the uterus is left intact. After oophorectomy, the symptoms of menopause may come on suddenly. This is different to turning off the ovaries with medication which brings menopausal symptoms on gradually
What Is The Life Expectancy For Each Cancer Stage
Your outlook depends on the stage of your cancer when its discovered. Cancer is staged by number, starting with 0 and going to 4. Stage 0 is the very beginning and stage 4 is the last stage, also called the metastatic stage because its when cancer has spread to other areas in the body.
Each number reflects different characteristics of your breast cancer. These include the size of the tumor and whether cancer has moved into lymph nodes or distant organs, like the lungs, bones, or brain.
The cancer subtype doesnt play a role in staging, only in treatment decisions.
Survival statistics of women with the major subtypes of breast cancer such as ER-positive, HER2-positive, and triple-negative are grouped together. With treatment, most women with very early stage breast cancers of any subtype can expect a normal life span.
Survival rates are based on how many people are still alive years after they were first diagnosed. Five-year and 10-year survival are commonly reported.
According to the
- stage 3 72 percent
- stage 4 22 percent
One thing to note is that these statistics also included women with the more aggressive HER2-positive and triple-negative cancers. And it takes five years to get to a five-year statistical survival rate, so newer therapies are not included in these numbers.
Its likely that a woman with ER-positive breast cancer diagnosed today may have a higher chance of survival.
When Is Hormone Therapy Used
Hormone therapy is only effective for HR-positive tumors. If your breast cancer tumor is , your oncologist will recommend other treatments.
Hormone therapy can be used in pre- or postmenopausal people with any stage of HR-positive breast cancer.
Hormone therapy that starts before surgery or radiation treatment is called neoadjuvant therapy. This can help shrink the tumor and make surgery easier.
When you begin hormone therapy treatment after surgery or radiation, its called adjuvant therapy. The goal here is to lower the risk that cancer will spread or come back.
According to the American Cancer Society, hormone therapy usually lasts at least .
Recommended Reading: Stage Iv Breast Cancer Symptoms
What Are Hormone Inhibitors And How Do They Work
Hormone inhibitors also target breast cancer cells with hormone receptors, but unlike hormone blockers, they work by reducing the bodys hormone production. When breast cancer cells are cut off from the food supply the tumor begins to starve and die.Generally, the benefits of using hormone therapy and chemotherapy together have a much greater combined effect than using either alone. If your breast cancer is positive for hormone receptors, your doctor may recommend both therapies.
Hormone Therapy For Breast Cancer
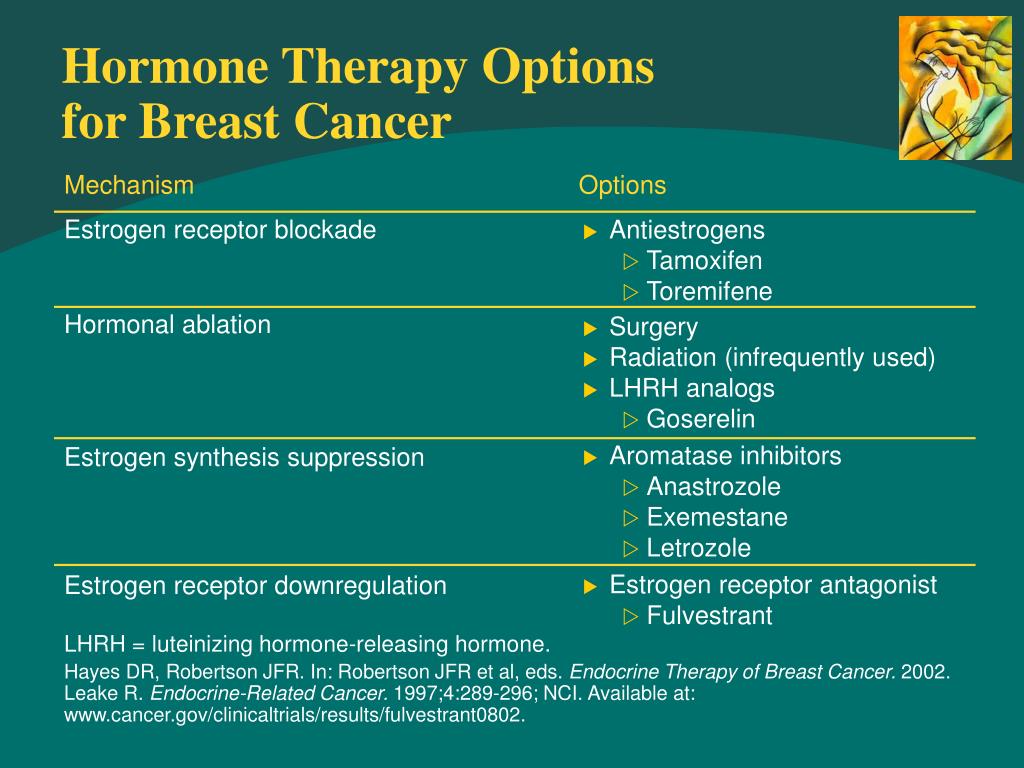

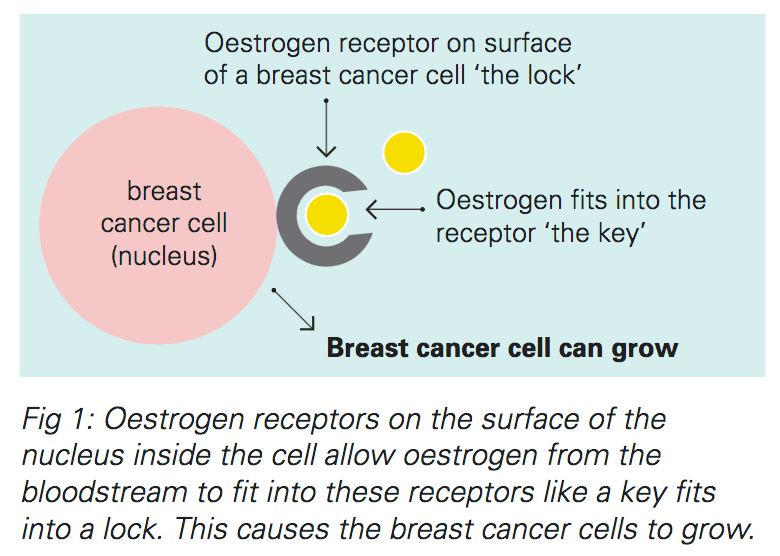
Some types of breast cancer are affected by hormones, like estrogen and progesterone. The breast cancer cells have receptors that attach to estrogen and progesterone, which helps them grow. Treatments that stop these hormones from attaching to these receptors are called hormone or endocrine therapy.
Hormone therapy can reach cancer cells almost anywhere in the body and not just in the breast. It’s recommended for women with tumors that are hormone receptor-positive. It does not help women whose tumors don’t have hormone receptors .
Recommended Reading: Breast Cancer Age Of Onset
What Is A Hormone Receptor
In breast cancer, hormone receptors are the proteins located in and around breast cells. These receptors signal cells both healthy and cancerous to grow. In the case of breast cancer, the hormone receptors tell the cancer cells to grow uncontrollably, and a tumor results.
Hormone receptors can interact with estrogen or progesterone. Estrogen receptors are the most common. This is why ER-positive is the most common form of breast cancer.
Some people are diagnosed with progesterone receptor-positive breast cancer. The key difference is whether cancerous cells are getting growth signals from estrogen or progesterone.
Testing for hormone receptors is important in treating breast cancer. In some cases, there are no hormone receptors present, so hormone therapy isnt a good treatment option. This is called hormone receptor-negative breast cancer.
According to
Treating Stage Iii Breast Cancer
In stage III breast cancer, the tumor is large or growing into nearby tissues , or the cancer has spread to many nearby lymph nodes.
If you have inflammatory breast cancer: Stage III cancers also include some inflammatory breast cancers that have not spread beyond nearby lymph nodes. These cancers are treated slightly different from other stage III breast cancers. You can find more details in Treatment of Inflammatory Breast Cancer.
There are two main approaches to treating stage III breast cancer:
Read Also: Cancer Is Fungus And Curable With Baking Soda
How Hormone Therapy Is Given
Hormone therapy may be given in many ways. Some common ways include:
- Oral. Hormone therapy comes in pills that you swallow.
- Injection. The hormone therapy is given by a shot in a muscle in your arm, thigh, or hip, or right under the skin in the fatty part of your arm, leg, or belly.
- Surgery. You may have surgery to remove organs that produce hormones. In women, the ovaries are removed. In men, the testicles are removed.
Does Insurance Cover Tamoxifen
While costs vary, tamoxifen is usually less expensive than an aromatase inhibitor because it is a generic medicine. If you have health insurance, check with your insurance company to see if and how much of the cost of tamoxifen is covered. If you don’t have health insurance or your insurance doesn’t cover the cost of tamoxifen, ask your doctor or nurse about programs in your area that may be able to help.
Soltamox is available to patients who qualify at the same co-pay cost as generic tamoxifen. Patients can download a $10 co-pay per prescription card for unlimited use.
You can also read Breastcancer.org’s Paying for Your Care section for information on additional types of financial assistance and cost-lowering tips.
Read Also: Malignant Neoplasm Of Breast Meaning
Survival Rates For Her2
Cancer survival statistics are typically reported using a 5-year survival rate. This is the percentage of individuals that are still living 5 years after their diagnosis.
Survival rates can vary based off of the subtype of breast cancer that you have. A publication from the reports 5-year survival rates for HER2-negative breast cancers as:
- 92 percent for HER2-negative, HR-positive breast cancer
- 77 percent for triple-negative breast cancer
Keep in mind that HER2 and HR status arent the only factors that can influence outlook. Other important factors at diagnosis include:
- the stage of the cancer
- the specific type of breast cancer
- your age and overall health
Less Common Types Of Hormone Therapy
Some other types of hormone therapy that were used more often in the past, but are rarely given now include:
- Megestrol acetate , a progesterone-like drug
- Androgens , like testosterone
- Estradiol
These might be options if other forms of hormone therapy are no longer working, but they can often cause side effects.
Read Also: Symptoms Of Late Stage Breast Cancer
Can Other Drugs Interfere With Hormone Therapy
Certain drugs, including several commonly prescribed antidepressants , inhibit an enzyme called CYP2D6. This enzyme plays a critical role in the body’s use of tamoxifen because CYP2D6 metabolizes, or breaks down, tamoxifen into molecules, or metabolites, that are much more active than tamoxifen itself.
The possibility that SSRIs might, by inhibiting CYP2D6, slow the metabolism of tamoxifen and reduce its effectiveness is a concern given that as many as one-fourth of breast cancer patients experience clinical depression and may be treated with SSRIs. In addition, SSRIs are sometimes used to treat hot flashes caused by hormone therapy.
Many experts suggest that patients who are taking antidepressants along with tamoxifen should discuss treatment options with their doctors, such as switching from an SSRI that is a potent inhibitor of CYP2D6, such as paroxetine hydrochloride , to one that is a weaker inhibitor, such as sertraline or citalopram , or to an antidepressant that does not inhibit CYP2D6, such as venlafaxine . Or doctors may suggest that their postmenopausal patients take an aromatase inhibitor instead of tamoxifen.
Other medications that inhibit CYP2D6 include the following:
- Quinidine, which is used to treat abnormal heart rhythms
What Is The Role Of Hormone Therapy In The Treatment Of Metastatic Breast Cancer
For patients who have hormone receptor positive disease without a life-threatening component or systemic symptoms requiring immediate palliation for comfort, in general, hormone manipulation is the initial treatment of choice. Response rates are higher with chemotherapy, but so is the incidence of potentially dangerous toxicity, and there is no evidence that patients live longer as a result of receiving initial chemotherapy.
For ERpositive metastatic breast cancer, the American Society of Clinical Oncology recommends using endocrine therapy rather than chemotherapy as first-line treatment, except in patients with immediately life-threatening disease or if there are concerns about endocrine resistance. The recommendation is part of an ASCO clinical practice guideline on the use of chemotherapy and targeted therapy for women with human epidermal growth factor 2 -negative advanced breast cancer, with recommendations based on a systematic review of 79 studies.
A trial of hormone manipulation alone can assess whether hormone therapy is effective, which is impossible to determine if it is given together with cytotoxic chemotherapy. This is especially important when the patient has relapsed disease, because the benefit of second-line hormone manipulation is nearly 50%, and failure to benefit from an initial trial with endocrine therapy correlates with second-line failure. Common hormone therapies and dosages are listed in Table 5, below.
References
Recommended Reading: Breast Cancer Stage 3 Treatment
Types Of Studies Of Hormone Therapy And Cancer Risk
Different types of studies can be used to look at cancer risk from menopausal hormone therapy .
Randomized controlled trials: In this kind of study, a group of patients get the drug being studied , and another group gets a placebo . Results from this kind of study are powerful because which group a patient is in is based on chance. This helps assure that the groups are similar in all ways, such as risk for cancer, except for the drug thats being studied. This is the best way to see the effects of a drug. These types of studies can also be double-blinded, which means neither the people in the study nor their doctors know which group they are in. This lowers the chance that thoughts or opinions about treatment could affect the study results. Unfortunately, these kinds of studies are costly, which limits the number of people in the study, how long the study can continue, and the number of studies done.
A major drawback of observational studies is that the people getting the treatment being studied may have different cancer risk factors than the people who arent. Plus, the treatment can differ between the people being studied. This makes it less clear that the differences seen are only due to the drug being studied and not other factors.
When observational studies and randomized controlled trials have different results, most experts give more weight to the results of the randomized controlled trial.
Taking Estrogen With A Progestin Vs Estrogen Alone
Treating menopausal symptoms with estrogen and progestin together is known as estrogen-progestin therapy or combined hormone therapy. Although estrogen alone improves the symptoms of menopause, it increases the risk of cancer of the uterus . Adding a progestin to the estrogen lowers the risk of endometrial cancer back to normal. Because of this, EPT is given to women who still have a uterus . EPT can be given 2 ways:
- Continuous EPT means the same dose of estrogen and progestin is taken each day. Women often prefer continuous EPT because it rarely leads to menstrual-like bleeding.
- Sequential EPT means different amounts of each hormone are taken on specific days. There are different ways to do this. For example, estrogen can be taken by itself for 14 days, then estrogen plus progestin for 11 days, then neither hormone for 3 to 5 days. Other schedules involve taking progestin only every few months. This lowers the amount of progestin that you are exposed to. Monthly regimens are also thought to result in hormone levels that are more like the natural menstrual cycle. Cyclical EPT can produce bleeding like a menstrual period, but it can occur less often than monthly.
Read Also: Estrogen Positive Metastatic Breast Cancer
How To Tell If Hormone Therapy Is Working
If you are taking hormone therapy for prostate cancer, you will have regular PSA tests. If hormone therapy is working, your PSA levels will stay the same or may even go down. But, if your PSA levels go up, this may be a sign that the treatment is no longer working. If this happens, your doctor will discuss treatment options with you.
If you are taking hormone therapy for breast cancer, you will have regular checkups. Checkups usually include an exam of the neck, underarm, chest, and breast areas. You will have regular mammograms, though you probably wont need a mammogram of a reconstructed breast. Your doctor may also order other imaging procedures or lab tests.
Estrogen Therapy And Cancer Risk
Endometrial cancer
In women who still have a uterus, using systemic ET has been shown to increase the risk of endometrial cancer . The risk remains higher than average even after ET is no longer used. Although most studies that showed an increased risk were of women taking estrogen as a pill, women using a patch or high-dose vaginal ring can also expect to have an increased risk of endometrial cancer.
Because of this increased cancer risk, women who have gone through menopause and who still have a uterus are given a progestin along with estrogen. Studies have shown that EPT does not increase the risk for endometrial cancer.
Long-term use of vaginal creams, rings, or tablets containing topical estrogen doses may also increase the levels of estrogen in the body. Its not clear if this leads to health risks, but the amounts of hormone are much smaller than systemic therapies.
Breast cancer
ET is not linked to a higher risk of breast cancer. In fact, certain groups of women taking ET, such as women who had no family history of breast cancer and those who had no history of benign breast disease, had a slightly lower risk of breast cancer.
Ovarian cancer
The WHI study of ET did not report any results about ovarian cancer.
To put the risk into numbers, if 1,000 women who were 50 years old took estrogen for menopause for 5 years, one extra ovarian cancer would be expected to develop.
Colorectal cancer
Lung cancer
ET does not seem to have any effect on the risk of lung cancer.
You May Like: Signs Of Stage 4 Breast Cancer
Can Hormone Therapy Be Used To Prevent Breast Cancer
Yes. Most breast cancers are ER positive, and clinical trials have tested whether hormone therapy can be used to prevent breast cancer in women who are at increased risk of developing the disease.
A large NCI-sponsored randomized clinical trial called the Breast Cancer Prevention Trial found that tamoxifen, taken for 5 years, reduces the risk of developing invasive breast cancer by about 50% in postmenopausal women who were at increased risk . Long-term follow-up of another randomized trial, the International Breast Cancer Intervention Study I, found that 5 years of tamoxifen treatment reduces the incidence of breast cancer for at least 20 years . A subsequent large randomized trial, the Study of Tamoxifen and Raloxifene, which was also sponsored by NCI, found that 5 years of raloxifene reduces breast cancer risk in such women by about 38% .
As a result of these trials, both tamoxifen and raloxifene have been approved by the FDA to reduce the risk of developing breast cancer in women at high risk of the disease. Tamoxifen is approved for this use regardless of menopausal status. Raloxifene is approved for use only in postmenopausal women.
Who Should Use Tamoxifen
Tamoxifen can help women and men with hormone receptor-positive breast cancer. The drug can lower the risk of breast cancer in:
- Women who are high-risk of breast cancer due to a family history of disease or mutated breast cancer genes.
- Women and men who have already been diagnosed with breast cancer to prevent recurrence of cancer, including:
- Development of breast cancer in the opposite, untreated breast.
- American Cancer Society. Breast Cancer Hormone Receptor Status. Accessed 11/18/2021.
- American Cancer Society. Hormone Therapy for Breast Cancer. Accessed 11/18/2021.
- American Cancer Society. Tamoxifen and Raloxifene for Lowering Breast Cancer Risk. Accessed 11/18/2021.
- BreastCancer.org. Low-Dose Tamoxifen May Be an Option to Reduce Risk of Recurrence, Invasive Disease After Non-Invasive Breast Cancer. Accessed 11/18/2021.
- BreastCancer.org. Tamoxifen . Accessed 11/18/2021.
- National Breast Cancer Foundation. Hormone Therapy. Accessed 11/18/2021.
- National Cancer Institute. Hormonal Therapy. Accessed 11/18/2021.
- Susan G. Komen. Side Effects of Tamoxifen. Accessed 11/18/2021.
- Susan G. Komen. Tamoxifen. Accessed 11/18/2021.
- Susan G. Komen. Tamoxifen and Raloxifene to Reduce Breast Cancer Risk. Accessed 11/18/2021.
- Susan G. Komen. Tumor Characteristics: Hormone Receptor Status. Accessed 11/18/2021.
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services.Policy
You May Like: Does Having Breast Cancer Shorten Life Expectancy