Recurrent Breast Cancer: Facts And Figures
Breast cancer can return at any point after the initial diagnosis and treatment. This is one of the most anxiety-provoking factors for many women after breast cancer diagnosis and treatment.
There are 3 types of cancer recurrence:-
It is very difficult to predict how many breast cancers of all stages recur, at local, regional and distant sites.
Indeed, breast cancer incidence and mortality rates are documented over the years. However, data on most cancer registries do not document the incidence of recurrence.
Furthermore, a local or regional recurrence does not have the same prognostic impact as distant metastasis. Even more difficult to handle, is that cancer can recur at any given point in time.
How Common Is Tnbc
About 15-20 percent of all breast cancers are TNBC or basal-like tumors .
TNBC tends to occur more often in :
- Younger women
- People with an BRCA1 inherited gene mutation
- Black, non-Hispanic Black and African American women
TNBC may also be more common among Hispanic women compared to non-Hispanic white women .
Targeting Homologous Recombination Deficiency In Tnbc
PARPi offer a biologically appealing treatment for patients with intrinsic HRD. HRD renders cells vulnerable to neoplastic transformation. However, this vulnerability to neoplastic changes also renders tumour cells vulnerable to genotoxic cell death via PARP inhibition as cells are reliant on base excision repair by PARP so it represents an Achilles Heel. By inhibiting two pathways of DNA repair, the tumour cells have impaired DNA replication. The combination of PARP inhibition and BRCA1/BRCA2 mutations is termed synthetic lethality.
Also Check: Stage Four Breast Cancer Symptoms
What Is The Risk For Triple
The disease can affect anyone, but is more likely to show up in those who are:
- Younger than age 50 .
- Black or Latinx.
- Living with a genetic condition called BRCA mutation that increases the risk for breast cancer and other forms of cancer. Most cancers diagnosed in people with the BRCA1 mutation are triple negative.
Triple Negative Metastatic Breast Cancer
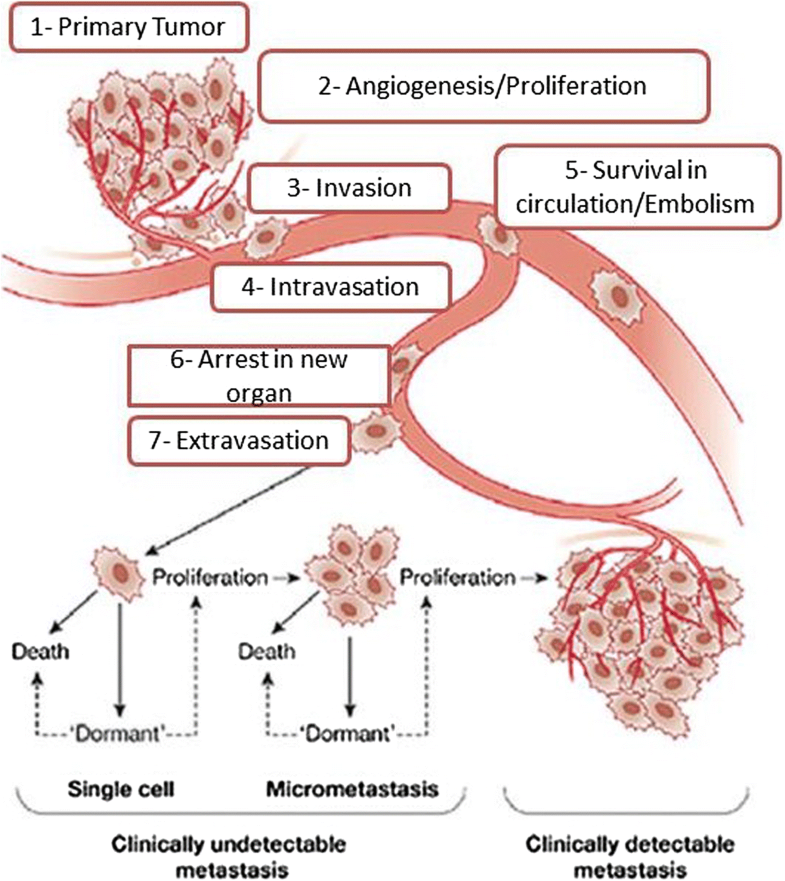
Triple negative metastatic breast cancer is a heterogeneous disease, chemotherapy remains the mainstay of treatment, however, new treatments based on identifying molecular subtypes, stratifying TNBC based on gene expression assays with subsequent specific targeted therapy is an area of intense clinical research. In this post, I will review our current standard clinical practice and explore ongoing and future clinical directions.
Metastatic TNBC is very heterogenous, and while Basal type is most common, it only account for nearly 80% of all cases.
- Metastatic TNBC is more common in younger patients and premenopausal African American patients.
- Metastatic TNBC more commonly affecting the brain, and visceral organs, and less commonly affecting bones.
- Metastatic TNBC is more common in BRCA1 mutation patient, all TNBC younger than 60 should be screened for BRCA mutations.
- In a patient with a history of TNBC and now presenting with metastatic disease, a re-biopsy is recommended since there is reported discordance between primary tumor and metastatic disease hormone receptor status in up to 5% of cases.
A. gBRCA mutated metastatic TNBC
PARP inhibitors: the use of Olaparib in this patients subsets is clearly validated by the OlympiAD trial, where patients who are metastatic TNBC, and germline BRCA mutation treated with Olaparib was shown to have higher response rate and PFS compared to standard therapy. As of to date, Olaparib is not yet FDA approved for BRCA mutated metastatic TNBC.
Don’t Miss: Red Mill Baking Soda Cancer
Cell Lines And Culture Conditions
Cell lines used were: MCF7, T47D, SKBr3, MDA-MB-468, MDA-MB-436, SUM 149 and DU145 MDA-MB-231 MDA-MB-231-luc-D3H2LN . The MDA-MB-231-luc-D3H2LN cell line was derived from a tumor isolated from the lymph node of a mouse after mammary fat pad injection with a luciferase-expressing MDA-MB-231 human breast cancer cell line. STR profiling done on the MDA-MB-231-luc D3H2LN cell line matched MDA-MB-231 in the ATCC STR database. All cell lines were cultured in Dulbeccos modified Eagles , supplemented with 10% fetal bovine serum , 100 U/ml penicillin, 100 U/ml streptomycin , 2 mM L-glutamine, incubated at 37ºC and 95% O2 / 5% CO2. Insulin 0.01 mg/ml was added to medium for MCF7. Nitrofen treatment in vitro was carried out at 1 µM and 10 µM concentrations for 24 h in culture medium containing 1% FBS. This was the effective dose of nitrofen reported in two previous studies using cell culture assays without causing cell death,.
Phase Iii Keynote 355 Trial
The much anticipated KEYNOTE-355 trial was presented at the inaugural virtual ASCO annual meeting in June 2020. This trial investigated pembrolizumab/chemo vs chemo in patients with treatment-naïve, metastatic TNBC. Patients were excluded if they had active brain metastases or recurrence of disease < 6 mo prior to primary treatment. PD-L1 was assessed with the IHC 22C3 pharmDx CPS assay in a central laboratory. The primary outcome measure was pre-defined as OS and PFS in the PD-L1 positive population and the ITT population. In this trial, a hierarchial statistical testing method involved statistical testing of OS and PFS in the CPS > 10 group initially, followed by CPS > 1 and then the ITT population. The trial included 566 patients in the chemotherapy/IO arm vs 281 in the chemotherapy arm. In patients with a CPS score of 10 or greater, the median PFS favoured pembrolizumab with a PFS of 9.6 mo vs 5.6 mo . In patients with a CPS score of 1 or greater, the median PFS favoured the pembrolizumab arm with a PFS of 7.6 mo vs 5.6 mo . This was not statistically significant. This was similar to the ITT population where the PFS was 7.5 mo in the pembrolizumab arm and 5.6 mo in the placebo arm . OS data is awaited. This progression free survival improvement led to accelerated FDA approval for pembrolizumab in combination with chemotherapy in the first-line setting in November of 2020.
Recommended Reading: Symptoms Of Stage 2 Breast Cancer
Treating Metastatic Breast Cancer
If you receive a diagnosis of breast cancer thats spread to your colon, your doctor will likely order additional tests to see whether the cancer has spread to other parts of your body.
Once you know exactly whats going on, you and your doctor can discuss the best options for treatment. This may include one or more of the following therapies.
What Is The Treatment For Triple
Chemotherapy.Chemotherapy is almost always called for, Sun says. Chemo can downstage tumors . While Sun says the chemotherapy for triple-negative breast cancer can be intense, she adds that regimen can be tailored to the individual and adjusted for older or frailer patients.
In those cases where we get complete response, we know we gave you the right medicine and your prognosis is good, Sun says.
Surgery can remove more of the tumor. Surgery for triple-negative breast cancer does not always have to be a mastectomy, Sun says. Effective chemotherapy done first opens up the possibility of less-invasive surgical options that are less of an ordeal for the patient. If the tumor is small enough after chemo, outpatient procedures or a lumpectomy may be possible.
Surgical samples of the cancerous tissues taken from surgery can provide more information on the cancer and how it is behaving so chemotherapy can be tailored accordingly.
Radiation therapy involves the use beams of radiation to destroy cancer cells, using various techniques to prevent damage to healthy surrounding tissue.
Medical treatments are being tested on triple-negative breast tumors in clinical trials.
Immunotherapy and PARP inhibitors are very exciting and theres lots of research going on, including here at Johns Hopkins, Sun says.
Recommended Reading: Stage 3 Her2 Positive Breast Cancer
What Role Do Genetic Mutations Play
One way to find and treat TNBC earlier is to identify those at greater risk of getting breast cancer. To do this, researchers are studying the inherited gene mutations that can increase a womanâs risk of getting breast cancer.
Inheriting variants of two genes — breast cancer gene 1 and breast cancer gene 2 — increases your chance of getting breast and ovarian cancers and certain other types of cancer. If you have one of these variants and do get breast cancer, youâre more likely to get it at a younger age.
Learning more about the other genetic variants linked to breast cancer may lead to better treatment of TNBC. Most breast cancers with the BRCA1 mutation are triple-negative, but other genes can also be targeted for treatment in TNBC. Studies show that some drug therapies may be more effective in treating BRCA-related and other genetic variants in breast cancers.
Some doctors recommend that everyone with TNBC be tested for gene mutations linked to breast cancer, including BRCA1 and BRCA2. If you were diagnosed with TNBC at 60 or younger, or if you have a relative with TNBC, your doctor may recommend genetic testing. Knowing your status may be helpful to you both when it comes to selecting effective therapies. For example, TNBC patients with certain variants may be more likely to respond to some treatments.
Survival Rates For Triple
Triple-negative breast cancer is considered an aggressive cancer because it grows quickly, is more likely to have spread at the time its found, and is more likely to come back after treatment than other types of breast cancer. The outlook is generally not as good as it is for other types of breast cancer.
Survival rates can give you an idea of what percentage of people with the same type and stage of cancer are still alive a certain amount of time after they were diagnosed. They cant tell you how long you will live, but they may help give you a better understanding of how likely it is that your treatment will be successful.
Keep in mind that survival rates are estimates and are often based on previous outcomes of large numbers of people who had a specific cancer, but they cant predict what will happen in any particular persons case. These statistics can be confusing and may lead you to have more questions. Talk with your doctor about how these numbers may apply to you, as he or she is familiar with your situation.
Recommended Reading: Did Anne Hathaway Have A Nose Job
A New Era Of Hope For Patients With Triple
Triple-negative breast cancer is a particularly devastating subtype of breast cancer, as it is often diagnosed in young women and is associated with an exceptionally poor prognosis. The triple-negative designation indicates that the three key features driving most breast cancers are lacking, but it provides no clues as to potential biologic drivers. In the absence of any biologic insights, tailored, targeted treatment decisions have historically not been possible.
Consequently, until as recently as 2018, we have relied exclusively on nonselective cytotoxic agents, with modest success. For example, conventional neoadjuvant chemotherapy confers a pathologic complete response in just 50% to 55% of patients with early-stage triple-negative breast cancer,1-4 and among those who do not achieve a pathologic complete response, approximately one-third will die within 3 years.5 Moreover, patients with metastatic triple-negative breast cancer treated with conventional chemotherapeutics have a median survival of 12 to 18 months and an estimated 5-year overall survival of 11%.6 Thus, therapeutic innovation for early and late triple-negative breast cancer has been desperately needed.
Biologic Insight Leads to Therapies
From biologic insight springs hope for therapeutic innovation. Heather L. McArthur, MD, MPHTweet this quote
Immune Modulation Via Checkpoint Blockade
Antibody-Drug Conjugates
Forecast Finally Changing in Triple-Negative Disease
REFERENCES
Drug And Gene Delivery For Treatment Of Breast Cancer Metastasis
Combinatorial delivery by liposomes of gefitinib and small interfering RNA targeted to EGF receptors for treatment of TNBC
Small interfering RNA represents an attractive tool for inhibition of a specific mRNA and corresponding protein. In our lab, we used siRNA targeted to EGFR receptors in combination with gefitinib for the effective treatment of TNBCs. Both the siRNA and gefitinib were delivered by cationic and neutral liposomes, respectively. The toxicity of this combination for sensitive MCF-7 and triple-negative MDA-MB-231 human breast cancer cells was studied with appropriate controls .
The cellular internalization of siRNA delivered by liposomes. Representative images of human breast cancer cells incubated within 24 h with liposomes containing siRNA . Cell nuclei were stained with nuclear-specific dye . Superimposition of red and green colors gives yellow color
The expression of EGFR mRNA. The relative quantity of EGFR gene expression in MCF-7 and MDA-MB-231 human breast cancer cells was calculated by the 2 method using quantitative PCR. The levels of gene expression were represented as a fold change. Means±SD are shown. a Expression of EGFR in MCF-7 and MDA-MB-231 cells incubated with media . b MDA-MB-231 cells before and after treatment. Cells were incubated within 24 h with liposomal siRNA targeted to EGFR mRNA
Recommended Reading: 4th Stage Breast Cancer Life Expectancy
What Makes Breast Cancer Hard To Treat
The most successful treatments control the way breast cancer cells grow. Breast cancer is divided into three subtypes based on how cells respond to these types of treatment:
- Hormone receptor positive cancer has the estrogen receptor and/or progesterone receptor and responds to hormone therapies.
- HER2-positive cancer has high amounts of the HER2/neu protein and is treated with therapies that target HER2 receptors.
- Triple-negative breast cancer does not contain estrogen or progesterone receptors or the HER2 receptor. Between 10-20 percent of all breast cancer cases fall into this subtype.
Treatments that are most effective for other types of breast cancer donât work for TNBC. Since there are no hormone receptors, hormone therapy isnât effective. And drugs that target HER2 aren’t helpful, either. At the same time, TNBC tends to be more aggressive than other types of breast cancer. By the time itâs diagnosed, the cancer often has spread to other parts of the body. It also differs from patient to patient and can even change over time to resist certain drugs.
Survival Rates And Prognosis
The outlook for breast cancer is often described in terms of relative survival rates.
Relative survival rates are an estimate of the percentage of people who will survive their cancer for a given period of time after diagnosis. Survival among people with cancer is compared to survival among people of the same age and race who have not been diagnosed with cancer.
Five-year relative survival rates tend to be lower for triple-negative breast cancer than for other forms of breast cancer.
According to the American Cancer Society, the overall 5-year relative survival rate for TNBC is . However, an individuals outlook depends on many factors, including the stage of the cancer and the grade of the tumor.
Your healthcare professional will be able to give you a more precise outlook based on:
- the stage of your TNBC
- your age
Also Check: Breast Cancer Tumor Growth Rate
Breast Cancers Survival Is Influenced By Tumor Grade
Grade identifies the size and shape of the malignant breast cancer cells. At the event the breast cancer cells look very different than normal breast tissue cells, and random in appearance, they can be called, that was badly differentiated and described as âhigh gradeâ. Higher level breast cancer cells tend to really have a poorer prognosis.
Treatment For Triple Negative Breast Cancer
The main treatments for triple negative breast cancer are surgery, chemotherapy and radiotherapy. The treatment you need depends on:
- where the cancer is
- the size of the cancer and whether it has spread
- how abnormal the cells look under the microscope
- your general health
You might have surgery to remove:
- an area of the breast
- the whole breast
When you have your surgery, the surgeon usually takes out some of the lymph nodes under your arm. They test these nodes to see if they contain cancer cells. The surgeon might check the lymph nodes closest to the breast using a procedure called sentinel lymph node biopsy. Testing the lymph nodes helps to find the stage of the cancer and decide on further treatment.
After breast conserving surgery you usually have radiotherapy to the rest of the breast tissue.
Also Check: Tamoxifen Metastatic Breast Cancer
Circulating Tumor Cells And Lymphovascular Invasion
Circulating tumor cells are rare malignant cells that resulted or originated from the primary site. These cells circulate in the peripheral blood and can work as independent predictive and prognosis factor of early and advanced stage of breast cancer. The presence of more than five CTCs/7.5 ml of blood in MBC patients or more than one CTCs/7.5 ml of blood in non-metastasis patients can be predictive of poor PFS and OSC. As a result, CTCs can give information about the efficacy of the treatment by drawing a blood sample from cancer patient multiple times during his/her illness . Figure Figure22 shows how CTCs works as prognosis factor for metastasis cells, treatment, and understanding drug resistance in breast cancer.
Role of CTCs in breast cancer in vitro and vivo. Modified and reproduced with permission from
Lymphovascular invasion involves both the lymphatic and blood vessel invasion lying within an endothelial-lined space in the area that surrounding the invasive tumor. LVI can be used as predictive factor for breast cancer patients. In addition, it is prognosis factor for lymph node, lymph node positive, and triple-negative breast cancer. About 23% of patients with early stage breast cancer showed vascular invasion .
Treatments Of Metastatic Breast Cancer
The goal of metastasis treatment is to prolong survival, palliate symptoms, and delay progression of the disease . Treatment of MBC varies with certain factors such as risk for toxicity, preferences of the patient, burden of the tumor, characterization of the tumor itself such as HER2 status and hormone receptor status, age, history of prior therapy, co-morbidities, degree of tumor-related symptoms, and metastasis sites. In fact, treatment of MBC can fall into three categories, such as surgery, chemotherapy, and hormonal therapy . Combination of two or more regimens of MBC therapy can improve the quality of life and decrease the side effects associated with using single treatment. The most common types of treatment of MBC are summarized in Fig. Fig.44.
The most common types of MBC treatment
Don’t Miss: What Stage 3 Cancer Means