Consume Alcohol Less In 7 Days
The tools Georgia Foster offers you will certainly help you drink less, no issue how much you drink. With the tools of 7 Days To Drink Less, you will not only learn to drink less, but develop new healthier coping strategies without using so any crutch. The 7 Days to Drink Less program will work with you to help identify the pain points in your life and the personality trains that lead you to drinking a little more than you should.
Breast Cancer Risk Factors
Family history of breast cancer, ovarian cancer, or other hereditary breast and ovarian syndrome- associated cancer
Known deleterious gene mutation
Prior breast biopsy with specific pathology
Atypical hyperplasia
Lobular carcinoma in situ
Prolonged interval between menarche and first pregnancy
Menopausal hormone therapy with estrogen and progestin
Not breastfeeding
Certain ethnicities
Higher body mass index
Prior exposure to high-dose therapeutic chest irradiation in young women
The Odds Of Developing Cancer
Receiving a cancer diagnosis or watching a loved one struggle with the disease can be a terrifying experience. According to MetLife, 41 percent of adults in the U.S. reportedly feared developing cancer during their lifetime.;
But what are the chances of getting cancer? Statistics from the American Cancer Society suggest men have a 40.14 percent chance of getting the disease, while womens odds are 38.7 percent. As for specifics, prostate cancer is ranked highest for men, with an 11.6 percent risk.;
For women, its breast cancer, carrying a 12.83 percent risk. However, the ACS has recently revealed lung cancer has overtaken breast cancer as the leading cause of cancer in women living in developed nations.
What about the odds of dying from cancer? Despite the alarming figures, dying from cancer has a slightly more optimistic outlook. Men have a 21.34 percent risk of dying from cancer throughout a lifetime, while women have an approximately 18.33 percent risk.;
These encouraging statistics result from screening programs with early detection rates and significant advancements in cancer therapy treatments.
Recommended Reading: What Stage Is Breast Cancer Spread To Lymph Nodes
Who Is Most At Risk Of Developing Breast Cancer
1. The strongest risk factor for breast cancer is age. Therefore, older women are at a higher risk of developing breast cancer than younger women.
2. Another significant risk factor is carrying a gene that predisposes to the development of breast cancer, such as the BRCA 1 and 2 genes. Related to carrying a gene that causes breast cancer, having a strong family history of breast cancer also increases a persons risk. Women who carry a gene that causes breast cancer or women who have a strong family history of breast cancer are at higher risk than women who do not.;
3. Another risk factor for breast cancer is having a history of a breast biopsy that showed atypical cells, such as atypical ductal hyperplasia or lobular carcinoma in situ.;
4. Lastly, there are several risk factors associated with a woman’s exposure to hormones throughout her lifetime, such as early menarche, number of pregnancies, whether or not a woman has breastfed, late menopause, that impact breast cancer risk. The more a woman has been exposed to estrogen and the more menstrual cycles she has experienced, the higher her risk of developing breast cancer.;
What Are The Benefits Of Genetic Testing For Brca1 And Brca2 Variants
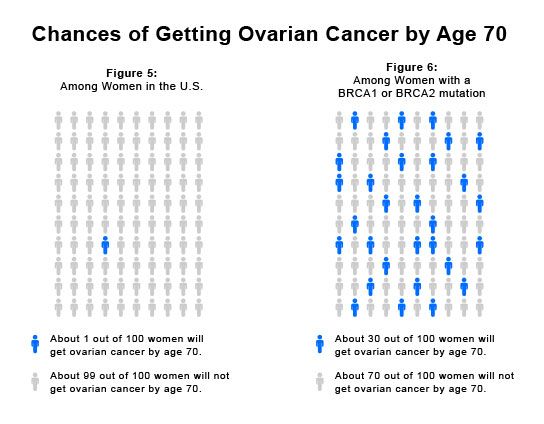
There can be benefits to genetic testing, regardless of whether a person receives a positive or a negative result.
The potential benefits of a true negative result include a sense of relief regarding the future risk of cancer, learning that one’s children are not at risk of inheriting the family’s cancer susceptibility, and the possibility that special check-ups, tests, or risk-reducing;surgeries may not be needed.
A positive test result may;allow people to make informed decisions about their future health care, including taking steps to reduce their cancer risk.;
Don’t Miss: What Age Should You Get Checked For Breast Cancer
Breast Cancer: Risk Factors And Prevention
Have questions about breast cancer? Ask here.
ON THIS PAGE: You will find out more about the factors that increase the chance of developing breast cancer. Use the menu to see other pages.
A risk factor is anything that increases a persons chance of developing cancer. Although risk factors often influence the development of cancer, most do not directly cause cancer. Some people with several risk factors never develop cancer, while others with no known risk factors do. Knowing your risk factors and talking about them with your doctor may help you make more informed lifestyle and health care choices.
Most breast cancers are sporadic, meaning they develop from damage to a persons genes that occurs by chance after they are born. There is no risk of the person passing this gene on to their children, as the underlying cause of sporadic breast cancer is environmental factors.
Inherited breast cancers are less common, making up 5% to 10% of cancers. Inherited breast cancer occurs when gene changes called mutations are passed down within a family from parent to child. Many of those mutations are in tumor suppressor genes, such as BRCA1, BRCA2, and PALB2. These genes normally keep cells from growing out of control and turning into cancer. But when these cells have a mutation, it can cause them to grow out of control.
The following factors may raise a womans risk of developing breast cancer:
Does Health Insurance Cover The Cost Of Genetic Testing For Brca1 And Brca2 Variants
People considering BRCA1 and BRCA2 variant testing may want to confirm their insurance coverage for genetic counseling and testing. Genetic counselors can often help answer questions about insurance coverage for genetic testing.
Some genetic testing companies may offer testing for inherited BRCA1 and BRCA2 variants at no charge to patients who lack insurance and meet specific financial and medical criteria.
Read Also: How Do Doctors Treat Breast Cancer
Clinical Considerations And Recommendations
How should individual breast cancer risk be assessed?
Health care providers periodically should assess breast cancer risk by reviewing the patients history. Breast cancer risk assessment is based on a combination of the various factors that can affect risk Box 1610111213. Initial assessment should elicit information about reproductive risk factors, results of prior biopsies, ionizing radiation exposure, and family history of cancer. Health care providers should identify cases of breast, ovarian, colon, prostate, pancreatic, and other types of germline mutation-associated cancer in first-degree, second-degree, and possibly third-degree relatives as well as the age of diagnosis. Women with a potentially increased risk of breast cancer based on initial history should have further risk assessment. Assessments can be conducted with one of the validated assessment tools available online, such as the Gail, BRCAPRO, Breast and Ovarian Analysis of Disease Incidence and Carrier Estimation Algorithm, International Breast Cancer Intervention Studies , or the Claus model 34.
Is screening breast self-examination recommended in women at average risk of breast cancer, and what should women do if they notice a change in one of their breasts?
Should practitioners perform routine screening clinical breast examinations in average-risk women?
When should screening mammography begin in average-risk women?
How frequently should screening mammography be performed in average-risk women?
What Causes Breast Cancer In Your 20s And 30s
Breast cancer happens when cells in the breast begin to grow and multiply abnormally. Changes in DNA can cause normal breast cells to become abnormal.
The exact reason why normal cells turn into cancer is unclear, but researchers know that hormones, environmental factors, and genetics each play a role.
Roughly 5 to 10 percent of breast cancers are linked to inherited gene mutations. The most well-known are breast cancer gene 1 and breast cancer gene 2 . If you have a family history of breast or ovarian cancer, your doctor may suggest testing your blood for these specific mutations.
Breast cancer in your 20s and 30s has been found to differ biologically in some cases from the cancers found in older women. For example, younger women are more likely to be diagnosed with triple negative and HER2-positive breast cancers than older women.
Here are some statistics about breast cancer in women under 40:
You May Like: How Do Women Get Breast Cancer
Using Your Family History
You should certainly share your family history with your medical team. Your doctors might advise genetic counseling or genetic testing if your family history suggests that you could be carrying a breast cancer gene.
Some red flags include:
- Cancer of;any;kind before the age of 50
- More than one relative with the same type of cancer
- One family member who has more than one type of cancer
- A family member who has cancer not typical for that gender, such as breast cancer in a male
- Certain combinations of cancer, such as the combination of breast cancer with ovarian cancer, uterine cancer, colon cancer, prostate cancer, pancreatic cancer, or melanoma
- Cancer in both of one organ, for example, bilateral breast or ovarian cancer
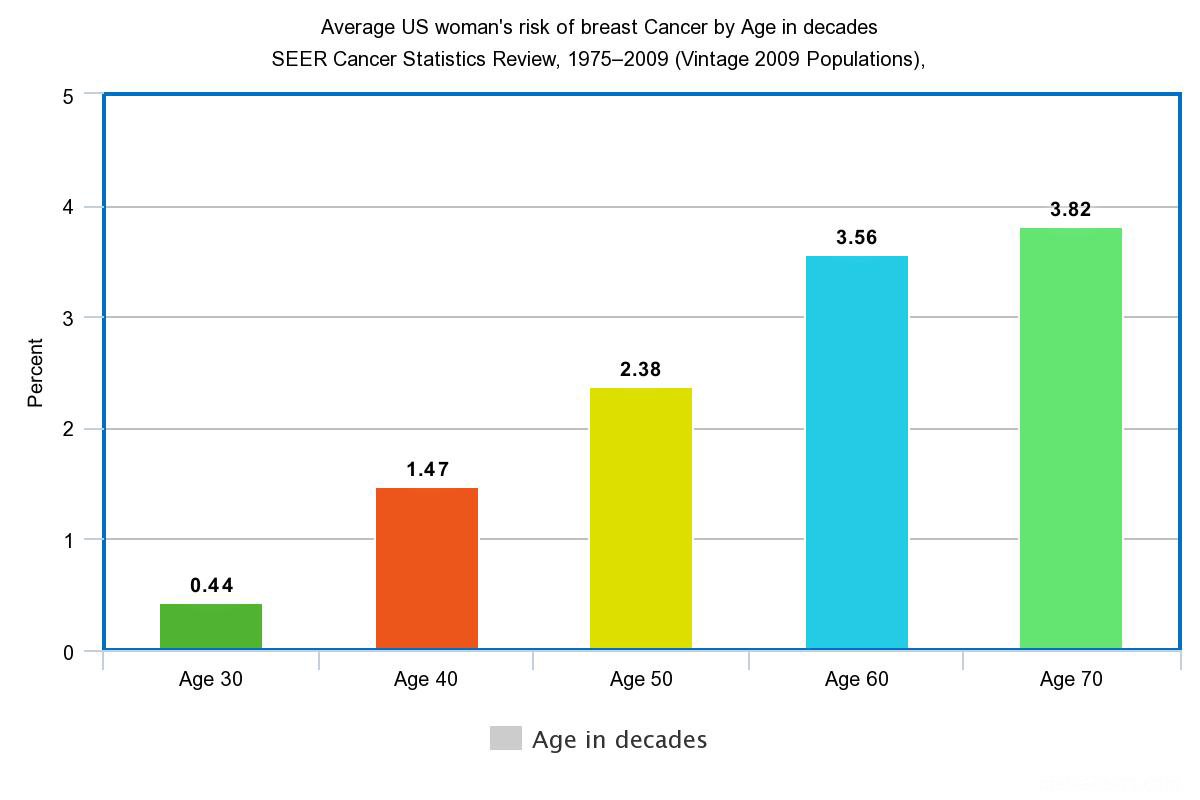
The Importance Of Age And The Lifetime Risks For Breast Cancer
In 1989, a womans lifetime risks for breast cancer was about 1 in 10. That risk increased to about 1 in 7 by 2003 and is currently 1 in 8 in the US over an 80-year lifespan.
Even though it may seem that breast cancer risk has increased in recent years, the actual risk of dying from breast cancer has decreased significantly.
As we can see from the graph above, the likelihood of being diagnosed with breast cancer increases as a woman ages.
The percentages on the graph can also be translated to the following risks for breast cancer listed below:-
- Age 30: 1 in 227
- At age 40: 1 in 68
- Age 50: 1 in 42
- Age 60: 1 in 28
- At Age 70: 1 in 26
What jumps out at you from the above table is the exponential increase in probability between age 30 and 40 years.
A woman is around 3.5 times more likely to get breast cancer at age 40 than she was aged 30. In addition, between the ages of 40 and 50, there is another increase in probability.
Recommended Reading: How Old To Get Breast Cancer
Understanding The Risk Of Late Recurrence Of Breast Cancer
Even as a young child, Crystal Moore, MD, PhD, FCAP, knew she wanted to be a physician. For her, medicine is not just a profession but also a calling. She received her MD/PhD at the Medical College of Virginia. Her PhD was awarded by the Department of Biochemistry and Molecular Biophysics. She completed her residency training in Anatomic and Clinical Pathology at Duke University and is a board-certified fellow of the College of American Pathologists. Follow Dr. Moore at www.DrCrystalMoore.com and on Twitter .
An astonishing 15 years after her initial diagnosis and treatment, my mothers breast cancer unexpectedly recurred. Eventually, it claimed her life. As a daughter, I felt blindsided. But as a physician, I grew determined to help all people with breast cancer understand the risk of late recurrence.
From surgery and reconstruction to radiation therapy, chemotherapy, adjuvant hormone therapy, and follow-up doctor visits, the road back to health after a breast cancer diagnosis can be long and difficult to navigate. Patients anxiously await the day when theyll hear that seemingly magical word: remission.
Once there has been a diagnosis of breast cancer, the risk of a recurrence is never zero.
Next Steps For Breast Cancer Survivors
Following a diagnosis of breast cancer, I always tell my patients to pace themselves. The journey after treatment can be long and challenging. The late, great Maya Angelou gave sage advice when she stated, My mission in life is not merely to survive, but to thrive, and to do so with some passion, some compassion, some humor, and some style.
These 5 steps can help you thrive in your overall health and cancer survivorship:
Take care of yourself emotionally. Seeking social support, developing strong personal relationships, accessing mental health services, and having a solid spiritual foundation are effective steps to manage lifes stressors and especially those unique to cancer survivorship.
Eat a healthy diet. Good nutrition supports overall health, such as eating a diet rich in fresh fruits, vegetables, and lean meats.
Maintain a healthy weight. Research shows that maintaining a healthy weight through a healthy diet and moderate physical activity lowers the risk of developing diabetes, high blood pressure, and other cancers and chronic diseases.
Stick with your follow-up care and other health screenings. Your routine oncology appointmentis a good time to talk about any concerns. If you notice any changes or new symptoms before your scheduled appointment, be sure to alert your health care provider. Also, take care of your entire body, including other recommended health screenings, such as Pap tests, general blood tests, blood pressure checks, and colonoscopy.
Recommended Reading: How You Know If You Have Breast Cancer
What Do Brca1 And Brca2 Genetic Test Results Mean
BRCA1 and BRCA2 mutation testing can give several possible results: a positive result, a negative result, or a variant of uncertain significance result.
Positive result. A positive test result indicates that a person has inherited a known harmful variant in BRCA1 or BRCA2 and has an increased risk of developing certain cancers. However, a positive test result cannot tell whether or when the tested individual will develop cancer. Some people who inherit a harmful BRCA1 or BRCA2 variant never develop cancer.
A positive test result may also have important implications for family members, including future generations.
- Both men and women who inherit a harmful BRCA1 or BRCA2 variant, whether or not they develop cancer themselves, may pass the variant to their children. Each child has a 50% chance of inheriting a parents variant.
- All blood relatives of a person who has inherited a harmful BRCA1 or BRCA2 variant are at some increased risk of having the variant themselves. For example, each of that persons full siblings has a 50% chance of having inherited the variant as well.
- Very rarely, an individual may test positive for a harmful variant not inherited from either parent. This is called a de novo variant. Such a variant is one that arose in a germ cell of one of the parents and is present in all the cells of the person who grew from that cell. The children of someone with a de novo variant are at risk of inheriting the variant.
How Cancer Risk Is Determined
Determining what is the probability of getting cancer comes from studies focusing on large groups of people, allowing researchers to identify environmental factors such as smoking for lung cancer and sunlight or skin cancer that contribute to cancer.;
In cancers with more subtle risks, researchers have used observational techniques to determine what types of people develop the disease, what those people have in common, and how they differ from those who are yet to develop the disease.;Cancer Risk And You
Risk statistics can be frustrating because they cannot necessarily answer the question: What are the chances of me getting cancer? Just because theres a 40 percent chance of developing cancer, it doesnt necessarily mean you are in that 40 percent.;
Your risk is determined by several factors, including age, lifestyle habits, family history and genetics, and your living environment. Even then, this may not affect your chances of having cancer.;
Your doctor will discuss your chances of developing cancer and propose ways to reduce the risk. However, its not a sure guarantee that you wont develop cancer at some point in your lifetime.
Read Also: What Is Er Pr Positive Breast Cancer
Reproductive History Estrogen Is The Main Hormone Associated With Breast Cancer Estrogen Affects The Growth Of Breast Cells Experts Believe That It Plays An Important Role In The Growth Of Breast Cancer Cells As Well The Type Of Exposure And How Long Cells Are Exposed To Estrogen Affects The Chances That Breast Cancer Will Develop
Early menarche
The start of menstruation is called menarche. Early menarche is when menstruation starts at an early age . Starting your period early means that your cells are exposed to estrogen and other hormones for a greater amount of time. This increases the risk of breast cancer.
Late menopause
Menopause occurs as the ovaries stop making hormones and the level of hormones in the body drops. This causes a woman to stop menstruating. If you enter menopause at a later age , it means that your cells are exposed to estrogen and other hormones for a greater amount of time. This increases the risk for breast cancer. Likewise, menopause at a younger age decreases the length of time breast tissue is exposed to estrogen and other hormones. Early menopause is linked with a lower risk of breast cancer.
Late pregnancy or no pregnancies
Pregnancy interrupts the exposure of breast cells to circulating estrogen. It also lowers the total number of menstrual cycles a woman has in her lifetime.
Women who have their first full-term pregnancy after the age of 30 have a slightly higher risk of breast cancer than women who have at least one full-term pregnancy at an earlier age. Becoming pregnant at an early age reduces breast cancer risk.
The more children a woman has, the greater the protection against breast cancer. Not becoming pregnant at all increases the risk for breast cancer.
Risk Of Developing Breast Cancer
The term risk is used to refer to a number or percentage that describes how likely a certain event is to occur. When we talk about factors that can increase or decrease the risk of developing breast cancer, either for the first time or as a recurrence, we often talk about two different types of risk: absolute risk and relative risk.
Don’t Miss: Can Birth Control Cause Breast Cancer