Ovarian Ablation Or Suppression
In women who have not yet experienced the menopause, oestrogen is produced by the ovaries.
Ovarian ablation or suppression stops the ovaries working and producing oestrogen.
Ablation can be done using surgery or radiotherapy. It permanently stops the ovaries from working and means you’ll experience the menopause early.
Ovarian suppression involves using a medicine called goserelin, which is a luteinising hormone-releasing hormone agonist .
Your periods will stop while you’re taking it, although they should start again once your treatment is complete.
If you’re approaching the menopause , your periods may not start again after you stop taking goserelin.
Goserelin comes as an injection you have once a month.
What Is Her2 And What Does It Mean
HER2 is a protein that helps breast cancer cells grow quickly. Breast cancer cells with higher than normal levels of HER2 are called HER2-positive. These cancers tend to grow and spread faster than breast cancers that are HER2-negative, but are much more likely to respond to treatment with drugs that target the HER2 protein.
All invasive breast cancers should be tested for HER2 either on the biopsy sample or when the tumor is removed with surgery.
Her2 Breast Cancer Treatment
Targeted therapy is the hallmark of treatment for HER2-positive cancer. The drug used most often is trastuzumab . Trastuzumab interferes with HER2 production and slows or prevents the cancer cells from growing. It is often administered with the chemotherapy agent emtansine in a combined drug called T-DM1.
Another medication, pertuzumab , is sometimes prescribed with trastuzumab when the cancer has spread to other parts of the body or metastasized. Oncologists also may prescribe an aromatase inhibitor, such as lapatinib or neratinib to lower estrogen levels.
If the cancer is also HR-positive, oncologists often prescribe endocrine therapy after the completion of targeted therapy. Endocrine or hormone therapy helps prevent cancer from returning by suppressing estrogen production. Tamoxifen is a common form of endocrine therapy used primarily in premenopausal women. It belongs to a class of drugs called selective estrogen receptor modulators .
Postmenopausal women have the option instead of taking an aromatase inhibitor , such as anastrozole , exemestane , or letrozole to block estrogen production. Postmenopausal women who have completed a tamoxifen regimen may be encouraged to follow up with an AI for added benefit.
You May Like: Chest Cancer In Female
Mcandrew: No Reason Not To Start With Cdk4/6 Inhibitors In Metastatic Hr+ Her2
Nicholas McAndrew, MD, MSCE, a medical oncologist and breastcancer specialist at UCLA Health and assistant clinical professor of Medicine at UCLA in the Division of Hematology/Oncology, discusses the arrival of CDK4/6 inhibitors in the treatment landscape.
The American Journal of Managed Care
Do I Need Genetic Counseling And Testing
Your doctor may recommend that you see a genetic counselor. Thats someone who talks to you about any history of cancer in your family to find out if you have a higher risk for getting breast cancer. For example, people of Ashkenazi Jewish heritage have a higher risk of inherited genetic changes that may cause breast cancers, including triple-negative breast cancer. The counselor may recommend that you get a genetic test.
If you have a higher risk of getting breast cancer, your doctor may talk about ways to manage your risk. You may also have a higher risk of getting other cancers such as ovarian cancer, and your family may have a higher risk. Thats something you would talk with the genetic counselor about.
Links with this icon indicate that you are leaving the CDC website.
- The Centers for Disease Control and Prevention cannot attest to the accuracy of a non-federal website.
- Linking to a non-federal website does not constitute an endorsement by CDC or any of its employees of the sponsors or the information and products presented on the website.
- You will be subject to the destination website’s privacy policy when you follow the link.
- CDC is not responsible for Section 508 compliance on other federal or private website.
Also Check: Recurrent Breast Cancer Symptoms
Side Effects Of Her2 Targeted Drug Therapy
The side effects of HER2 targeted drugs are often mild, but some can be serious. Discuss what you can expect with your doctor. If you are pregnant, you should not take these drugs. They can harm and even cause death to the fetus. If you could become pregnant, talk to your doctor about using effective birth control while taking these drugs.
Monoclonal antibodies and antibody-drug conjugates can sometimes cause heart damage during or after treatment. This can lead to congestive heart failure. For most women, this effect lasts a short time and gets better when the drug is stopped. The risk of heart problems is higher when these drugs are given with certain chemo drugs that also can cause heart damage, such as doxorubicin and epirubicin . Other factors that can increase your risk of heart problems are being older than 50, being overweight or obese, having heart problems, and taking medicines for high blood pressure.
Because these drugs can cause heart damage, doctors often check your heart function before treatment, and regularly while you are taking the drug. Let your doctor know if you develop symptoms such as shortness of breath, a fast heartbeat, leg swelling, and severe fatigue.
Lapatinib, neratinib, tucatinib, and the combination of pertuzumab with trastuzumab can cause severe diarrhea, so its very important to let your health care team know about any changes in bowel habits as soon as they happen.
Targeted Therapy For Women With Brca Gene Mutations
Olaparib and talazoparib are drugs known as PARP inhibitors. PARP proteins normally help repair damaged DNA inside cells. The BRCA genes also help repair DNA , but mutations in one of those genes can stop this from happening. PARP inhibitors work by blocking the PARP proteins. Because tumor cells with a mutated BRCA gene already have trouble repairing damaged DNA, blocking the PARP proteins often leads to the death of these cells. These drugs are pills and are taken once or twice a day.
Olaparib and talazoparib can be used to treat advanced or metastatic, HER2-negative breast cancer in women with a BRCA mutation who have already had chemotherapy. If the cancer is hormone receptor-positive, olaparib can also be used in women who have already received hormone therapy.
Only a small portion of women with breast cancer are born with a mutated BRCA gene, which is in all the cells of the body. This is different from the gene change happening after you are born which is found only in the cancer cells. If you are not known to have a BRCA mutation, your doctor will test your blood to be sure you have one before starting treatment with these drugs.
Side effects can include nausea, vomiting, diarrhea, fatigue, loss of appetite, taste changes, low red blood cell counts , low platelet counts, and low white blood cell counts. Rarely, some people treated with a PARP inhibitor have developed a blood cancer, such as myelodysplastic syndrome or acute myeloid leukemia .
Recommended Reading: Invasive Ductal Carcinoma Survival Rate Stage 1
Tests On Your Breast Cancer Cells
After a biopsy or surgery to remove breast tissue, a sample of cells is sent to the laboratory. A doctor called a pathologist does various tests on the cells. This can diagnose cancer and also show which type of cancer it is.
Some tests can also show how well particular treatments might work, such as hormone therapies or targeted cancer drugs.
What Type Of Breast Cancer Do I Have
Breast cancers arent all the same. Doctors classify them in a number of different ways. The most basic place to start is where the cancer cells originate. Their origin is a key factor in whether or not your cancer may spread and helps dictate the kind of treatment youll get.
Most breast cancers 70% to 80% start in the milk ducts. Theyre known as infiltrating or invasive ductal carcinomas, meaning that theyve broken through the milk ducts wall and have proliferated into the breasts fatty tissue. Once there, its possible for the cancer cells to further spread to other parts of the body.
Another 10% of breast cancers start in the milk-producing glands, or lobules, and are called invasive lobular carcinomas. Theyre also capable of spreading.
Other rarer breast cancers may involve the nipple, the breasts connective tissue or the linings of blood vessels or lymph vessels.
Some breast cancers are non-invasive. They havent spread. Theyre contained within the milk ducts and are called ductal carcinoma in situ . Generally, the prognosis for patients with DCIS is very good, Dr. Abraham says.
You May Like: Estrace Breast Cancer
Should I Consider Participating In A Clinical Trial
Breast cancer treatment has improved tremendously. The reason for this progress is because patients have been willing to take part in tests of newer treatment options.
For any stage of breast cancer, a well done clinical trial could be your best treatment option, Dr. Abraham says. If you qualify for such a trial, your doctor can answer any questions you may have about participating so that you can determine if its a good fit for you.
Pyrotinib Os Benefit Confirmed In Her2
There were a lot of exciting breastcancer abstracts presented at the San Antonio meeting this month. One of the studies that I found most interesting is the PHOEBE trial. This is a phase III trial which demonstrated that pretreated metastatic HER2-positive breastcancer patients had an improved overall survival when treated with the new agent pyrotinib plus capecitabine as compared to lapatinib plus capecitabine.
MedPage Today
Recommended Reading: What Does Stage 3 Breast Cancer Mean
Other Types Of Breast Cancer
There are some other less common types of invasive breast cancer.
Invasive lobular breast cancer
About 1 in 10 invasive breast cancers start in the lobes of the breast. This type can sometimes be difficult to diagnose on a mammogrambecause of the way it grows. Some women may need an MRI scan.
Inflammatory breast cancer
This is when cancer cells grow along and block the tiny channels in the skin of the breast. The breast then becomes inflamed and swollen. Inflammatory breast cancer is rare.
Pagets disease of the breast
This is a condition that causes a red, scaly rash on the skin of the nipple. Women with Pagets disease of the breast may have DCIS or invasive breast cancer.
The Same But Different
The story of progress in beating breast cancer is a testament to decades of painstaking work by researchers around the world. Nearly eight in 10 women diagnosed today will still be going strong ten years later, compared to around half that number back in the 1970s.
But this broadly positive picture of breast cancer hides a complex biological tapestry: not all breast cancers are equal.
For starters, around three quarters of all breast tumours are whats called ER positive, meaning they carry oestrogen receptors and so respond to the female sex hormone oestrogen. About two thirds of these are also PR positive, bearing receptors for another female hormone called progesterone. These types of cancers usually respond well to hormone-blocking treatments, such as tamoxifen, and there is a very good chance of surviving for a decade or more.
Then there are the HER2 positive bunch around one in five breast cancers. These carry multiple copies of a molecule called HER2, and tend to grow more aggressively. But they can be targeted by the drug Herceptin , which has helped to boost survival.
By a process of elimination, triple negative cancers are those that are left ER negative, PR negative and HER2 negative, and these make up roughly 15 per cent of all breast cancers somewhere in the region of 7,500 cases every year in the UK. Younger women under 40 are more likely to have this type, as are black women, and the cancers tend to grow and spread aggressively.
Recommended Reading: Is Estrogen Positive Breast Cancer Hereditary
Different Drugs Same Target
Breast cancers that are HER2-positive tend to be aggressive, with the excess HER2 protein on tumor cells fueling the cancers growth. In the late 1990s, trastuzumab was among the first targeted cancer therapies to be approved by FDA, after trials showed it could improve survival in women with metastatic HER2-positive breast cancer.
Over time, other HER2-targeted therapies emerged, some with alternative mechanisms for disrupting HER2 activity in cancer cells. Drugs like trastuzumab and pertuzumab are monoclonal antibodies that bind to the HER2 protein above the cancer cells surface, preventing it from acting or enlisting the immune system to help destroy cells that produce it.
Tucatinib, on the other hand, is a member of a class of drugs known as tyrosine kinase inhibitors . These drugs work by binding to the part of the HER2 protein that is inside the cell and preventing it from sending signals that promote cell growth. Other HER2-targeted TKIs include neratinib and lapatinib .
Some TKIs have multiple targets. But, compared with other HER2-targeted drugs, tucatinib appears to be relatively selective for HER2that is, its less likely to bind to related proteins, explained Stanley Lipkowitz, M.D., Ph.D., chief of the Womens Malignancies Branch in NCIs Center for Cancer Research. That selectivity limits the risk of side effects seen with other HER2-targeted TKIs that inhibit other targets, Dr. Lipkowitz said.
What Are The Symptoms Of Breast Cancer
The most common symptom of most breast cancers is a lump in the breast. A painless, hard mass with irregular edges is most likely cancer, but breast cancers can also have a lump that is soft and tender to the touch. Other possible symptoms in the first three stages of breast cancer include:
- Change in the size and shape of the breast
- Asymmetry in the breast compared to the other
- Skin dimpling or other abnormal changes in the breastâs skin
Also Check: What Are The Odds Of Surviving Breast Cancer
Targeted Therapy For Her2
In about 1 in 5 women with breast cancer, the cancer cells make too much of a growth-promoting protein known as HER2 . These cancers, known as HER2-positive breastcancers, tend to grow and spread more aggressively than HER2-negative breast cancers. Different types of drugs have been developed that target the HER2 protein.
What Is A Hormone Receptor
In breast cancer, hormone receptors are the proteins located in and around breast cells. These receptors signal cells both healthy and cancerous to grow. In the case of breast cancer, the hormone receptors tell the cancer cells to grow uncontrollably, and a tumor results.
Hormone receptors can interact with estrogen or progesterone. Estrogen receptors are the most common. This is why ER-positive is the most common form of breast cancer.
Some people are diagnosed with progesterone receptor-positive breast cancer. The key difference is whether cancerous cells are getting growth signals from estrogen or progesterone.
Testing for hormone receptors is important in treating breast cancer. In some cases, there are no hormone receptors present, so hormone therapy isnt a good treatment option. This is called hormone receptor-negative breast cancer.
According to
Also Check: What Is Stage 3a Cancer
Treating Aggressive Breast Cancers
Women diagnosed with breast cancer undergo testing to determine the form of the disease and whats driving its growth. This information is key to developing an individualized treatment strategy. Choice of treatment also depends on how extensive the cancer is within the breast, whether it has metastasized, and whether the patient is menopausal.
When either HER2-positive or triple-negative breast cancer is diagnosed early, surgery is often performed to remove the tumor and its surrounding tissue or the entire breast . Nearby lymph nodes sometimes are removed as well.
Neoadjuvant therapy, a treatment given as a first step before the primary treatment, is standard for both HER2-positive and triple-negative breast cancers if the tumor can be surgically removed. Chemotherapy is often used as a neoadjuvant therapy before surgery to shrink the tumor. The goal is to reduce the area that needs to be removed so the surgery can be less extensive, possibly avoiding a mastectomy. For HER2-positive cancer, chemotherapy may be combined with targeted therapy, medication that acts on the specific cause of the cancer.
After neoadjuvant therapy and surgery, the treatment strategies for HER2 and triple-negative breast cancers differ.
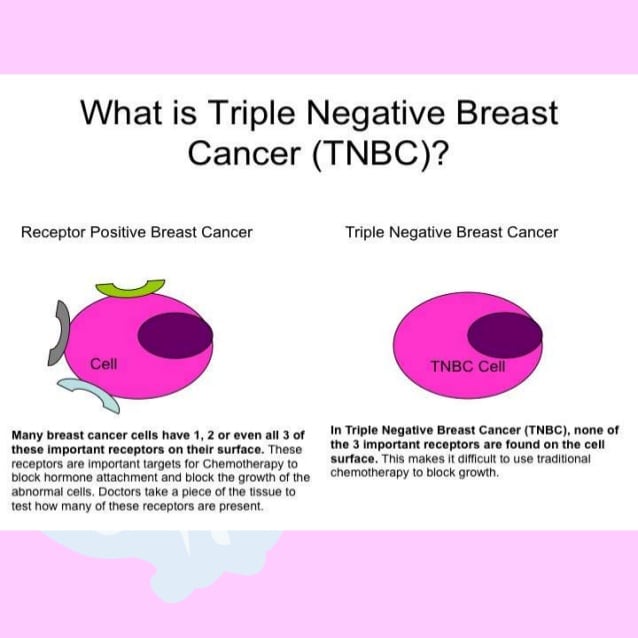
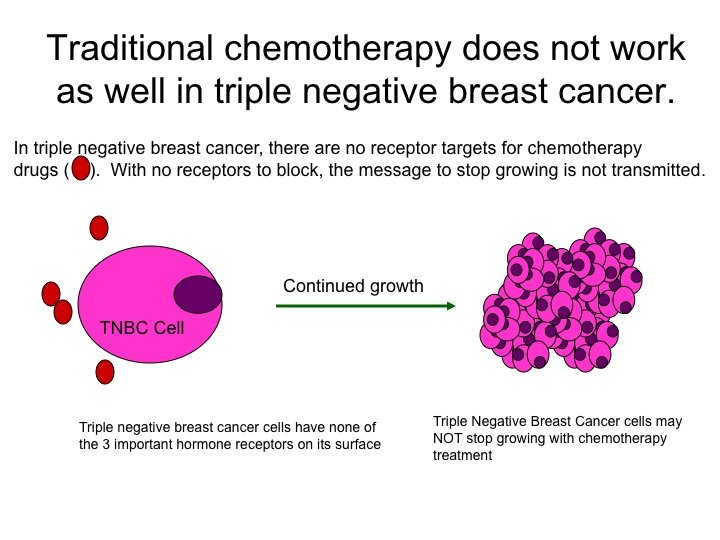
What Is Triple Negative Breast Cancer
In addition to being negative for estrogen and progesterone receptors, triple negative breast cancer cells also lack a protein known as HER2. Human epidermal growth factor receptor-2 is a protein that promotes cell growth and HER2 positive breast cancers have a higher than normal presence of these proteins, because of mutations in HER2 gene.
Triple negative cancers account for approximately 15% of breast cancers. Triple negative breast cancer more often occurs in African-American women younger than 40, or women who have an inherited mutation in BRCA1 gene, which normally is a tumor suppressor gene, which suppresses cell growth.
Read Also: Life Expectancy Of Breast Cancer Survivors
Targeted Drug Therapy For Breast Cancer
Targeted drug therapy uses medicines that are directed at proteins on breast cancer cells that help them grow, spread, and live longer. Targeted drugs work to destroy cancer cells or slow down their growth. They have side effects different from chemotherapy and can be given in the vein , as an injection under the skin, or as a pill.
Some targeted therapy drugs, for example, monoclonal antibodies, work in more than one way to control cancer cells and may also be considered immunotherapy because they boost the immune system.
Like chemotherapy, these drugs enter the bloodstream and reach almost all areas of the body, which makes them useful against cancers that have spread to distant parts of the body. Targeted drugs sometimes work even when chemo drugs do not. Some targeted drugs can help other types of treatment work better.
Several types of targeted therapy drugs can be used to treat breast cancer.