Clinical Breast Exams And Regular Breast Self
Routine examination of the breasts by health care providers or by women themselves has not been shown to reduce deaths from breast cancer. However, if a woman or her health care provider notices a lump or other unusual change in the breast, it is important to get it checked out. For more information, see the PDQ® Breast Cancer Screening summary.
What Are The Risks Of A Mammogram
You may want to ask your health care provider about the amount ofradiation used during the procedure and the risks related to yourparticular situation. It is a good idea to keep a record of your pasthistory of radiation exposure, such as previous scans and other typesof X-rays, so that you can inform your health care provider. Risksassociated with radiation exposure may be related to the cumulativenumber of X-ray examinations and/or treatments over a long period oftime.
If you are pregnant or suspect that you may be pregnant, you shouldnotify your health care provider. Radiation exposure during pregnancymay lead to birth defects. If it is necessary for you to have amammogram, special precautions will be made to minimize the radiationexposure to the fetus.
Some discomfort may be felt as the breast is compressed against theX-ray plate during the procedure. This compression will not harm thebreast, however.
There may be other risks depending on your specific medical condition.Be sure to discuss any concerns with your health care provider prior tothe procedure.
Certain factors or conditions may interfere with a mammogram. Theseinclude, but are not limited to, the following:
Lets Talk Mammograms
Recommended Reading: How To Cure Breast Cancer With Baking Soda
A Word About Minimizing Radiation Exposure
Doctors take special care during x-ray exams to use the lowest radiation dose possible while producing the best images for evaluation. National and international radiology protection organizations continually review and update the technique standards radiology professionals use.
Modern x-ray systems minimize stray radiation by using controlled x-ray beams and dose control methods. This ensures that the areas of your body not being imaged receive minimal radiation exposure.
Don’t Miss: Do Nipple Piercings Cause Breast Cancer
How Does One Properly Screen For Breast Cancer When You Have Dense Breast Tissue
Brown mentions that this is still an area of research. There are no guidelines on what to do with the information on increased breast density. There are currently studies looking at whether 3-D mammography is better than 2-D in saving lives. But in most cases, ultrasound and breast MRI are recommended to further assess the situation, she explains. Dr. Johnson advises talking with your physician about additional imaging, perhaps especially if theres a family history of cancer.
Further, the American College of Obstetricians and Gynecologists say that screening mammography remains the most useful tool for breast cancer detection and consistently has demonstrated a reduction in breast cancer mortality.
Dr. Johnson also reminds us of the bottom line, which is that early detection matters. While several guideline groups mention that the decision to start getting regular mammograms between the ages of 40 to 49 is a personal choice, Dr. Johnson advises making an appointment, especially if you are at an increased risk.
To get more stories about health and wellness delivered to your inbox, sign up for the Healthy Living newsletter
What To Do If You Find A Lump

Dont panic if you think you feel a lump in your breast. Most women have some lumps or lumpy areas in their breasts all the time, and most breast lumps turn out to be benign . There are a number of possible causes of non-cancerous breast lumps, including normal hormonal changes, a benign breast condition, or an injury.
Dont hesitate to call your doctor if youve noticed a lump or other breast change that is new and worrisome. This is especially true for changes that last more than one full menstrual cycle or seem to get bigger or more prominent in some way. If you menstruate, you may want to wait until after your period to see if the lump or other breast change disappears on its own before calling your doctor. The best healthcare provider to call would be one who knows you and has done a breast exam on you before for example, your gynecologist, primary care doctor, or a nurse practitioner who works with your gynecologist or primary care doctor.
Make sure you get answers. Its important that your doctor gives you an explanation of the cause of the lump or other breast change and, if necessary, a plan for monitoring it or treating it. If youre not comfortable with the advice of the first doctor you see, dont hesitate to get a second opinion.
You May Like: How Long Does Breast Cancer Take To Kill
What Are The Different Types Of Mammograms
According to the National Cancer Institute:
-
Screening mammogram. A screening mammogram is an X-ray of the breast used to detect breast changes in women who have no signs or symptoms of breast cancer. It usually involves 2 X-rays of each breast. Using a mammogram, it is possible to detect a tumor that cannot be felt.
-
Diagnostic mammogram. A diagnostic mammogram is an X-ray of the breast used to diagnose unusual breast changes, such as a lump, pain, nipple thickening or discharge, or a change in breast size or shape. A diagnostic mammogram is also used to evaluate abnormalities detected on a screening mammogram. It is a basic medical tool and is appropriate in the workup of breast changes, regardless of a womans age.
Find an Imaging Location
How Breast Mri Is Performed
Unlike a mammogram, which uses X-rays to create images of the breast, breast MRI uses magnets and radio waves to produce detailed 3-dimensional images of the breast tissue. Before the test, you may need to have a contrast solution injected into your arm through an intravenous line. Because the dye can affect the kidneys, your doctor may perform kidney function tests before giving you the contrast solution. The solution will help any potentially cancerous breast tissue show up more clearly. Some people experience temporary discomfort during the infusion of the contrast solution.
Cancers need to increase their blood supply in order to grow. On a breast MRI, the contrast tends to become more concentrated in areas of cancer growth, showing up as white areas on an otherwise dark background. This helps the radiologist determine which areas could possibly be cancerous. More tests may be needed after breast MRI to confirm whether or not any suspicious areas are actually cancer.
Because the technology uses strong magnets, it is essential that you remove anything metal jewelry, snaps, belts, earrings, zippers, etc. before the test. The technologist also will ask you if you have any metal implanted in your body, such as a pacemaker or artificial joint.
Its important to have breast MRI done at a facility with:
Recommended Reading: Stage 2 Triple Positive Breast Cancer
Radiation Therapy To The Chest
Women who received radiation to their chest as part of treatment for another type of cancer are at an increased risk for breast cancer.
The risk is highest for those who received treatment as teenagers or during their twenties. Radiation treatments to the chest in women over 40 dont appear to increase the risk for breast cancer.
Importance Of Early Detection
Prompt detection of breast cancer is important to find breast cancer in its earliest and most treatable stage. This may be before the person has any noticeable symptoms, so regular screening may be the most important tool for this early detection.
One notes that breast cancer is the second most common cause of death from cancer among women worldwide. Screening can help reduce this risk.
Research from 2016 notes that standard procedures for breast cancer screening can lead to a roughly in deaths from breast cancer.
The also notes that increasing screening practices for eligible people could:
- increase life expectancy
You May Like: Hormone Receptor Positive Breast Cancer Prognosis
How A Breast Ultrasound Works
A breast ultrasound uses sound waves to create a computer picture of the inside of the breast. The test is simple, non-invasive and there is no radiation. An ultrasound technician performs the screening by putting a gel on the breast and then moving a wand-like tool called a transducer over the skin. The transducer sends out sound waves which then bounce off tissues.
Ultrasound imaging can provide additional information to doctors if a suspicious spot is found on a mammogram or a lump can be felt but not seen with mammogram screening. It can help detect breast lesions in women with dense breast tissue.
Who Is At Risk For Developing Breast Cancer
Anyone can develop this cancer. Indeed, 75 percent of women who receive a breast cancer diagnosis have no family history of the disease. Doctors dont consider these women high risk, either because of their clean family history.
Anyone who is considered high-risk must take extra precautions. Thats because their likelihood of developing cancer outweighs the risks of others. Those who are regarded as high risk include:
- Those with a history of breast cancer in their family
- Women who are 50 years of age or older
While this disease is thought to only occur in women, men have a small chance of developing cancer, as well. Doctors may not recommend regular breast screenings for them, but they should still do self-exams at home and tell their doctor if they feel any changes or other lumps.
Read Also: Stage 4 Breast Cancer Cure
Finding Hard Lumps Around The Collarbone Are Always Frightening But What About On The Collarbone
Do you regularly feel your collarbone smack on it with your probing fingertips as well as right above it and right below it?
Lymphoma is a type of malignancy where the cancer cells originate from the lymphatic system, says John-Paul H. Rue, MD, orthopedic sports medicine surgeon with Orthopedics and Joint Replacement at Mercy Medical Center in Baltimore, MD.
Lymphomas may present as painless swelling in the lymph nodes of the neck and collarbone region, or the armpits or groin, continues Dr. Rue.
How To Check Your Breasts

Theres no special way to check your breasts and you do not need any training.
Checking your breasts is as easy as TLC:
- Touch your breasts: can you feel anything new or unusual?
- Look for changes: does anything look different to you?
- Check any new or unusual changes with a GP
Everyone will have their own way of touching and looking for changes.
Get used to checking regularly and be aware of anything thats new or different for you.
Check your whole breast area, including up to your collarbone and armpits.
Also Check: First Stage Of Breast Cancer Symptoms
Reasons For A Mammogram
A mammogram is a useful tool in detecting breast cancer because it can show abnormalities, such as a tumor, in the breast tissue long before they can be felt. Both screening and diagnostic mammography can help diagnose breast diseases, lumps, cysts and benign and malignant tumors. These procedures can also detect calcium deposits that may indicate breast cancer.
It is recommended that women older than 40 have mammograms annually. Patients with the following risk factors should take extra care to be screened regularly:
- Personal or family history of breast cancer
- Abnormal changes in the breast
- Long-term use of hormone therapy
How Does The Procedure Work
X-rays are a form of radiation like light or radio waves. X-rays pass through most objects, including the body. The technologist carefully aims the x-ray beam at the area of interest. The machine produces a small burst of radiation that passes through your body. The radiation records an image on photographic film or a special detector.
Different parts of the body absorb the x-rays in varying degrees. Dense bone absorbs much of the radiation while soft tissue allow more of the x-rays to pass through them. As a result, bones appear white on the x-ray, soft tissue shows up in shades of gray, and air appears black.
Most x-ray images are electronically stored digital files. Your doctor can easily access these stored images to diagnose and manage your condition.
In conventional film and digital mammography, a stationery x-ray tube captures an image from the side and an image from above the compressed breast. In breast tomosynthesis, the x-ray tube moves in an arc over the breast, capturing multiple images from different angles.
Recommended Reading: Breast Cancer Growth Rate
American Cancer Society Screening Recommendations For Women At High Risk
Women who are at high risk for breast cancer based on certain factors should get a breast MRI and a mammogram every year, typically starting at age 30. This includes women who:
- Have a lifetime risk of breast cancer of about 20% to 25% or greater, according to risk assessment tools that are based mainly on family history
- Have a known BRCA1 or BRCA2 gene mutation
- Have a first-degree relative with a BRCA1 or BRCA2 gene mutation, and have not had genetic testing themselves
- Had radiation therapy to the chest when they were between the ages of 10 and 30 years
- Have Li-Fraumeni syndrome, Cowden syndrome, or Bannayan-Riley-Ruvalcaba syndrome, or have first-degree relatives with one of these syndromes
The American Cancer Society recommends against MRI screening for women whose lifetime risk of breast cancer is less than 15%.
Theres not enough evidence to make a recommendation for or against yearly MRI screening for women who have a higher lifetime risk based on certain factors, such as:
- Having a personal history of breast cancer, ductal carcinoma in situ , lobular carcinoma in situ , atypical ductal hyperplasia , or atypical lobular hyperplasia
- Having extremely or heterogeneously dense breasts as seen on a mammogram
If MRI is used, it should be in addition to, not instead of, a screening mammogram. This is because although an MRI is more likely to detect cancer than a mammogram, it may still miss some cancers that a mammogram would detect.
Converting A Classifier From Recognizing Patches To Whole Images
Figure 1
Converting a patch classifier to an end-to-end trainable whole image classifier using an all convolutional design. The function f was first trained on patches and then refined on whole images. We evaluated whether removing the heatmap improved information flow from the bottom layers of the patch classifier to the top convolutional layers in the whole image classifier. The magnifying glass shows an enlarged version of the heatmap. This figure is best viewed in color.
The function h accepts whole images as input and produces labels at the whole image level. Therefore, it is end-to-end trainable, providing two advantages over the two-step approach. First, the entire network can be jointly trained, avoiding sub-optimal solutions from each step Second, the trained network can be transferred to another dataset without explicit reliance on ROI annotations. Large mammography databases with ROI annotations are rare and expensive to obtain. The largest public database with ROI annotations for digitized film mammograms DDSM contains several thousand images with pixel-level annotations, which can be exploited to train a patch classifier f. Once the patch classifier is converted into a whole image classifier h, it can be fine-tuned on other databases using only image-level labels. This approach allows us to significantly reduce the requirement for ROI annotations, and has many applications in medical imaging in addition to breast cancer detection on screening mammograms.
Also Check: Invasive Adenocarcinoma Breast Cancer
What This Means For You
While itll be a some time until youre scheduling a pap smear to detect breast cancer, the results suggest that cancer screenings could become more accurate and convenient in the future. For now, youll want to make sure you attend all your cancer screening appointments. People should start getting breast cancer screenings every one to two years, beginning at age 40. Pap smears are recommended for people with uteruses starting at age 21.
Tests To Stage Breast Cancer
After youre diagnosed with breast cancer, the next step is identifying your stage. Knowing the stage is how your doctor determines the best course of treatment. Staging depends on the size and location of the tumor and whether it has spread outside your breast to nearby lymph nodes and other organs. The speed of growth and the likelihood that the growth will spread is another component of staging.
Cancer cells that spread to lymph nodes can travel to different parts of your body. During the staging process, your doctor may order a complete blood panel including, liver function and kidney function tests, and a mammogram of your other breast to check for signs of a tumor. A doctor may also test for breast cancer tumor markers, CA 27-29 and CA 15-3.
Your doctor may also use any of the following tests to determine the extent of your cancer and assist with diagnosis :
Don’t Miss: Is Breast Cancer Curable
How Well Do Mammograms Work
These imaging tests help doctors diagnose about 75% to 85% of breast cancers. Detection rates get better as a woman ages, because breasts become less dense with age. This makes tissue easier to see through on mammograms.
Advancing technology raises detection rates. One study showed that using 3D mammography along with digital mammograms improved detection rates and lowered the number of women who had to return for more tests because of a suspicious finding.
Can An Ultrasound Detect Breast Cancer
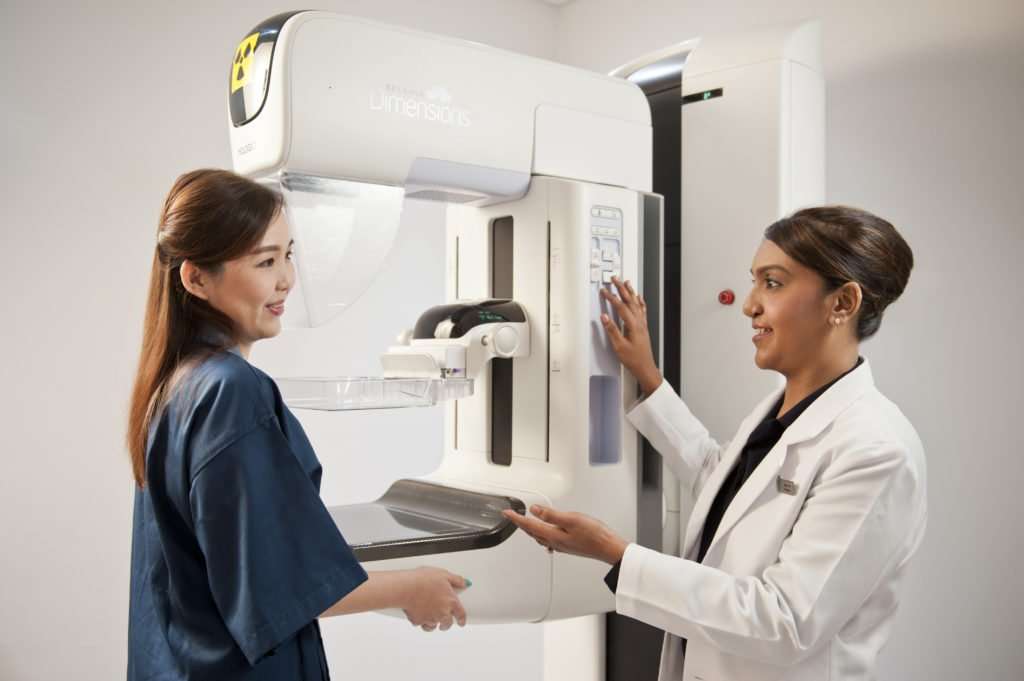
Mammography is your best defense against breast cancer. According to the American Cancer Society, screening mammograms can reduce breast cancer deaths by approximately 20% to 40%. After you get a mammogram, your doctor may call you back for additional testing. This doesnt always mean theres bad news. It could just be that your breast tissue is dense or there is a calcification or benign mass.
Your next test will likely be a diagnostic mammogram and an ultrasound to get better images of the inside of your breast.
Thank you for requesting an appointment with us!
You will receive an email from us in the next 24 hours.
If you do not see our email please check your Spam folder. For assistance, please call us at
Breast ultrasounds are used to create sonograms, which are detailed pictures that can show areas inside the breast. Ultrasounds are just one imaging method used to detect breast cancer. Others include:
- Mammograms
- Magnetic resonance imaging
- PET/CT scans
Breast ultrasounds are typically used early on in the detection process. In some cases a biopsy may be necessary and this can often be done with ultrasound or mammographic guidance.
Read Also: Treatment For Malignant Neoplasm Of Breast