Common Types Of Breast Cancer In Women
The most common type of breast cancer for individuals to be diagnosed with is invasive breast cancer . This means that the cancerous cells have grown within the duct linings which surround the breast tissue.
The NST is an acronym for no special type which means that breast cancer has no special features and there are no unique features displayed by the cancer cells when analysed under a microscope.
The second most common type of breast cancer is called invasive lobular breast cancer. Lobules are the physiological structures that are responsible for milk production during breastfeeding.
Invasive lobular breast cancer starts in the cells which line these glands and then spreads into the tissues surrounding the lobules.
Inflammatory breast cancer is a rare type of breast cancer that involves cancerous cells blocking the lymph channels within the breast.
The lymphatic system is highly important within the immune system and is responsible for the drainage of lymphatic fluid from organs and bodily tissues.
Due to the lymph channels being blocked, they are unable to function properly which causes the surrounding skin tissue to become inflamed, red, and irritated. Breast angiosarcomas are a group of cancers that are extremely rare.
This type of cancer originates in cells that make up the lining of the blood vessel walls and lymphatic vessels. Due to the physiological location of angiosarcomas, they can be difficult to treat as they are able to grow and divide rapidly.
Everything You Need To Know About Breast Cancer Screening
Information about breast cancer screenings can be confusing. It seems like new recommendations are coming out all the time, and each recommendation is different from the last one. Michelle Price, MD, co-medical director of the Fortunato Breast Health Center, helps us to understand some important breast health issues.
Understanding screening guidelines
Dr. Price says, think of it as an annual check-up. Unless there are other factors, women should begin screening mammography at age 40, and continue annual screening every year thereafter. Many professional societies involved with the diagnosis and treatment of breast cancer also continue to recommend annual screening mammography starting at age 40, including the Society for Breast Imaging, American College of Radiology and National Comprehensive Cancer Network.
According to Dr. Price, the Fortunato Breast Health Center also does not recommend a particular age for stopping screening. Some organizations suggest discontinuing mammography screening at age 75, but as long as you are in reasonably good health, you should continue to have your annual mammogram.
Michelle Price, MD,Fortunato Breast Health Center
Dense breasts what does that mean?
Risk Factors For Breast Cancer
- A family history of breast cancer .
- Previous chest or thoracic radiation therapy history before the age of 30 years.
- Family history of BRCA1 and BRCA2gene variants.
- First pregnancy at 30 years of age or older.
- Late menopause.
- More than four years of hormone replacement therapy .
Early detection with the most appropriate treatment is the most effective strategy to reduce breast cancer mortality.
Mammography screening for breast cancer is not only expensive but involves substantial manpower and financial resources. It is not a feasible approach in developing countries.
Studies on the efficacy of early detection programs, based on clinical breast examination and breast self-examination remain inconclusive and rather controversial.
You May Like: 18004cancer
American Cancer Society Screening Recommendations For Women At Average Breast Cancer Risk
The COVID-19 pandemic has resulted in many elective procedures being put on hold, and this has led to a substantial decline in cancer screening. Health care facilities are providing cancer screening during the pandemic with many safety precautions in place. Learn how you can talk to your doctor and what steps you can take to plan, schedule, and get your regular cancer screenings in Cancer Screening During the COVID-19 Pandemic.
These guidelines are for women at average risk for breast cancer. For screening purposes, a woman is considered to be at average risk if she doesnt have a personal history of breast cancer, a strong family history of breast cancer, or a genetic mutation known to increase risk of breast cancer , and has not had chest radiation therapy before the age of 30.
Women between 40 and 44 have the option to start screening with a mammogram every year.
Women 45 to 54 should get mammograms every year.
Women 55 and older can switch to a mammogram every other year, or they can choose to continue yearly mammograms. Screening should continue as long as a woman is in good health and is expected to live at least 10 more years.
All women should understand what to expect when getting a mammogram for breast cancer screening what the test can and cannot do.
Clinical breast exams are not recommended for breast cancer screening among average-risk women at any age.
Screening Recommendations For Breast Cancer
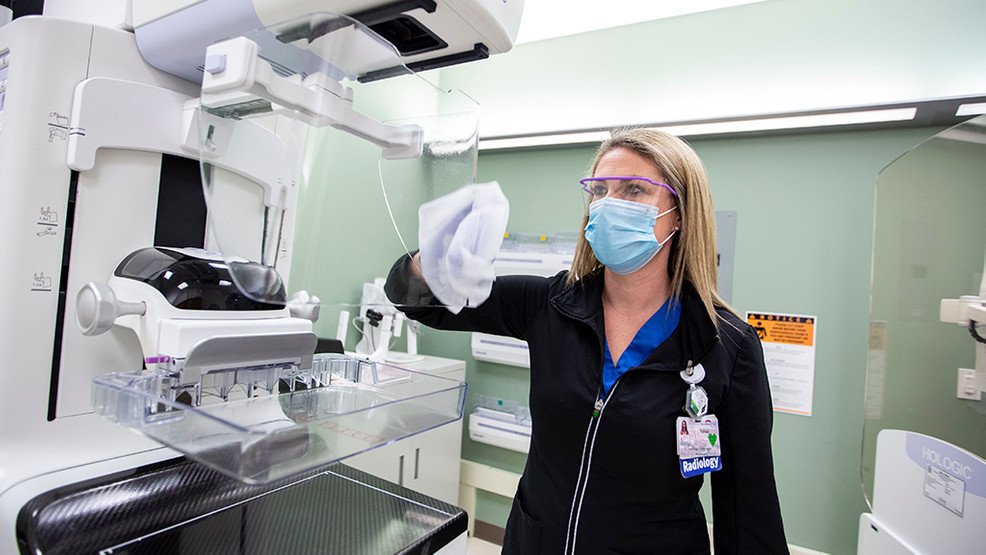
Detecting breast cancer early reduces the chance of death from breast cancer. Breast cancer is much easier to treat and has much better survival rates when caught in its early stages. Thats why getting regular screenings is an important part of womens healthcare.
According to the American Cancer Society, women at average risk for breast cancer should follow these screening guidelines:
| Age | |
| are strongly encouraged to have an annual mammogram | |
| over 55 | are encouraged to have a mammogram every 2 years, but can choose to still have an annual mammogram |
Women at an above average risk of breast cancer are strongly encouraged to have screenings more often and possibly begin earlier than age 40.
Screenings should include both mammograms and breast MRIs. Talk with a doctor about your individual risk factors and determine an appropriate screening plan for you.
Don’t Miss: Did Anne Hathaway Have Breast Cancer
What Is Breast Screening
Cancer screening involves testing apparently healthy people for signs that could show that a cancer is developing.
Breast screening uses a test called mammography which involves taking x-rays of the breasts. Screening can help to find breast cancers early when they are too small to see or feel. These tiny breast cancers are usually easier to treat than larger ones.
It is important to remember that screening will not prevent you from getting breast cancer but aims to find early breast cancers.
Overall, the breast screening programme finds cancer in around 9 out of every 1,000 women having screening.
Why Breast Cancer Screening Is More Important Than Ever
Breast Cancer Awareness Month is an opportune time to highlight the importance of understanding breast cancers impact, undergoing breast screening tests, and conducting breast self-exams.
Compared to the five-year averages before the COVID-19 pandemic, breast cancer screening tests declined by 87% in April 2020. Unfortunately, screening delays may lead to later-stage diagnoses, poor health consequences, and increased cancer disparities among women and men already experiencing health inequities.1Breast Cancer Awareness Month is a good time for employees to remember why breast cancer screening is so important, especially during a pandemic.
Also Check: Can Getting Hit In Your Breast Cause Cancer
What Is The Purpose Of Mammography
Regular mammogram screening is a vital tool in detecting breast cancer in its earliest stages. The goal is to find breast cancer before a woman notices any symptoms. The earlier a malignancy is detected, the better the chances of curing the disease before it spreads throughout the body and requires more invasive therapies with harmful side effects.
The American Cancer Society recommends all women over 40, even those with no family history of the disease, get a yearly mammogram.
Breast Cancer Is The Second Leading Cause Of Death From Cancer In American Women
Women in the United States get breast cancer more than any other type of cancer except for skin cancer.
Breast cancer is more likely to occur as a woman ages. It occurs more often in White women than in Black women, but Black women die from breast cancer more often than White women.
Breast cancer rarely occurs in men. Because men with breast cancer usually have a lump that can be felt, screening tests are not likely to be helpful.
Also Check: Is Breast Cancer Curable
Breast Cancer During Pregnancy
Breast cancer can occur and be diagnosed while a woman may be pregnant. This unfortunate situation requires a careful review with a specialized team consisting of the mothers gynecologist, oncologist, surgeon, pediatrician, pharmacologist and with adequate mental health support.
Due to the risk of cancer treatments on the growing fetus, there has to be a careful review of options on the best possible therapy and timing to minimize any fetal risks.
Most centers rely on surgical treatments to decrease the size or remove as much of the cancer tissue first, if detected early.
Hormonal therapy for the breast cancer may be used as its effect on the pregnancy is deemed less risky than cancer medications
* You Are At Average Risk If You Have:
- no symptoms of breast cancer
- no history of invasive breast cancer
- no history of ductal or lobular carcinoma in situ
- no history of atypia
- no family history of breast cancer in a first-degree relative
- no suggestion or evidence of a hereditary syndrome such as a BRCA mutation
- no history of mantle radiation
Don’t Miss: Can Asbestos Cause Breast Cancer
When To Get Screened
Breast cancer was expected to be the most common cancer diagnosed in Ontario women in 2018. Screening mammography can find breast cancers when they are small, less likely to have spread and more likely to be treated successfully. Your age and family medical history help determine when you should get screened:
- If you are age 50 to 74, the Ontario Breast Screening Program recommends that most women in your age group be screened every 2 years with mammography. Find your nearest OBSP site by calling 1-800-668-9304 or visiting Ontario Breast Screening Program locations.
- If you are age 30 to 69 and meet any of the following requirements, talk to your doctor about referral to the High Risk Ontario Breast Screening Program:
- You are known to have a gene mutation that increases your risk for breast cancer
- You are a first-degree relative of someone who has a gene mutation that increases their risk for breast cancer
- You have a personal or family history of breast or ovarian cancer
- You have had radiation therapy to the chest to treat another cancer or condition before age 30 and at least 8 years ago
For every 200 women screened in the Ontario Breast Screening Program, about 18 are referred for further tests and 1 will have breast cancer.
Can Telemedicine Consults Help Breast Cancer Patients Get The Right Help
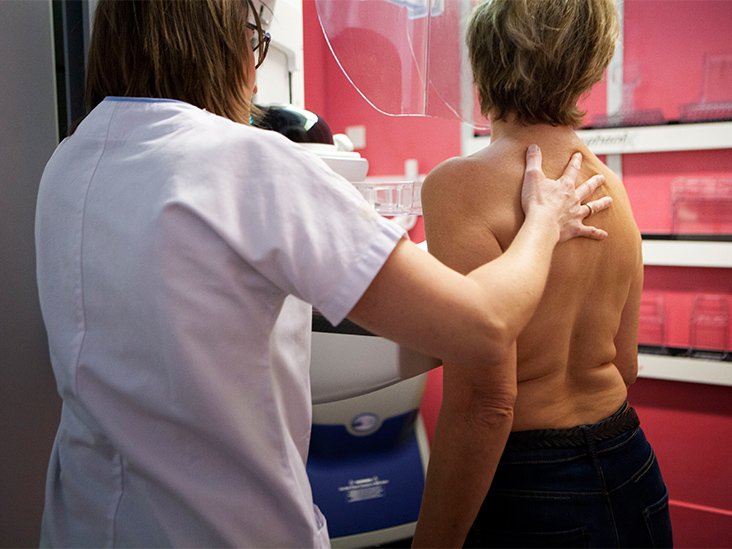
Telemedicine can help cancer patients seeking expert medical second opinions, counselling on the diagnosis and guidance on navigating the complex healthcare needs for the next best step for their management, that is deemed most appropriate for their cancer stage.
The difficulty in consulting a cancer specialist is often a challenging factor facing patients, regardless of their insurance coverage. Even patients with adequate funds to cover out-of-pocket access, often face the issue of connecting with a credible healthcare provider.
Many tertiary level healthcare facilities have telemedicine booking facilities for remote care appointments with their medical staff. Patients may be able to inquire about available facilities, coverage and the credibility of the clinical staff and their success rates with similar breast cancer patients.
- In some cases there may be further challenges even with remote care access such as:
- A difficult booking process
- Unclear process in follow up or referrals
Read Also: Is Breast Cancer Curable In The 3 Stage
What Laboratory Tests Are Needed To Diagnose Breast Cancer
Specific blood tests for measuring certain hormone receptors for estrogen and progesterone, and a specific cancer protein known as HER2/neu, are needed to guide the treatment plan.
If a breast cancer patient has high amounts of hormone receptors ie the cancer cells have a lot of these receptors on them, then it is possible to have a good response with hormone therapy. Chemotherapy that blocks hormone production or the receptors themselves may turn off the signals to these cancers to multiply.
If these hormone receptors are not present then hormone therapy will not be appropriate. Such test results are known as hormone-receptor-negative
HER2/neu Protein Tests
This protein is usually found in high numbers in aggressively invasive breast cancers or in recurrent cases.
This test is useful as a prognostic test, meaning a measurement of how well a treatment in removing cancer cells from the patient or of the actual mass is decreasing in size and activity.
If You Have A Normal Result
You will receive a letter to let you know your mammogram does not show any signs of cancer. Your next screening appointment will be in 3 years time. Do contact your GP or local screening unit if you havent received an appointment and think you are due one.
It is important to see your GP If you notice any symptoms between your screening mammograms.
You May Like: How To Cure Breast Cancer With Baking Soda
Risks Of Breast Cancer
The risks of breast cancer are for women who:-
- Have a lifetime risk of breast cancer of about 20% to 25% or greater, according to risk assessment tools that are based mainly on family history .
- Carry the BRCA1 or BRCA2 gene mutation.
- Have a first-degree relative with a BRCA1 or BRCA2 gene mutation, and have not had genetic testing themselves.
- Had radiation therapy to the chest when they were between the ages of 10 and 30 years.
- Have Li-Fraumeni syndrome, Cowden syndrome, or Bannayan-Riley-Ruvalcaba syndrome, or have first-degree relatives with one of these syndromes.
- The American Cancer Societyrecommends against MRI screening for women whose lifetime risk of breast cancer is less than 15 %.
Screening Information For Breast Cancer
Mammography
Mammography is the best tool doctors have to screen healthy women for breast cancer, as it has been shown to lower deaths from the disease. Like any medical test, mammography involves risks, such as the possibility of additional testing and anxiety if the test falsely shows a suspicious finding, called a “false-positive” result. Up to 10% to 15% of the time, mammography will not show an existing cancer, called a “false-negative” result.
Digital mammography may be better able to find breast cancers, particularly in women with dense breasts. A newer type of mammogram is called tomosynthesis or 3D mammography. It may improve the ability to find small cancers and reduce the need to repeat tests due to false-positives. However, there is also the risk of diagnosing problems in the breast that would otherwise go unnoticed and would not lead to any negative consequences. This is called “overdiagnosis” and may lead to overtreatment with a potential for harm. This method is approved by the FDA, though research on it is ongoing.
Other breast cancer screening methods
According to the American Cancer Society , women who have BRCA gene mutations, who have a very strong family history of breast cancer, or who had prior radiation therapy to the chest should consider mammography and MRI each year.
Women at moderate risk of breast cancer, such as women with precancerous changes on a biopsy, can talk with their doctor about whether MRI screening should be considered.
Recommended Reading: United Breast Cancer Foundation Rating
Screening Guidelines For Women At Above
MSKs breast cancer experts have developed separate guidelines for women who have a higher-than-average breast cancer risk for the following reasons:
- family history of breast cancer in a first-degree relative
- history of atypical hyperplasia
- history of lobular carcinoma in situ
- history of mantle radiation before the age of 32
- genetic predisposition for breast cancer
If you have an above-average risk of breast cancer for the reasons listed above, MSK doctors recommend the guidelines below.
Why Is Breast Screening Important
Breast cancer is the second largest cause of cancer death in Australian women after lung cancer. It is the most common cancer diagnosed in Australian women .
Early detection and appropriate treatment can significantly improve breast cancer survival.
Cancer Council Australia recommends that eligible women participate in the BreastScreen Australia program by having a free mammogram every two years, provided they are aware of the benefits and the risks.
Recommended Reading: How To Cure Breast Cancer With Baking Soda
The Balance Of Benefit And Harm
The panel estimates that an invitation to breast screening delivers about a 20% reduction in breast cancer mortality. For the UK screening programmes, this currently corresponds to about 1300 deaths from breast cancer being prevented each year, or equivalently about 22000 years of life being saved. However, this benefit must be balanced against the harms of screening, especially the risk of overdiagnosis. In the panel’s view, overdiagnosed cancers certainly occur, but the frequency in a screening programme of 20 years duration is unknown. Estimates from trials of shorter duration suggest overdiagnosis of about 11% as a proportion of breast cancer incidence during the screening period and for the remainder of the woman’s lifetime, or equivalently about 19% as a proportion of cancers diagnosed during the screening period. Any excess mortality stemming from the investigation and treatment of breast cancer is considered by the panel to be small and considerably outweighed by the benefits of treatment. Some other harms, including increased anxiety and discomfort caused by screening, are also acknowledged.
Notionally, for 10000 women invited to screening, from age 50 for 20 years, it is estimated that 681 cancers will be diagnosed, of which 129 will represent overdiagnosis and 43 deaths from breast cancer will be prevented.
The Effect Of Breast Screening On Mortality

This section summarises the panel’s views of the effect of breast screening on mortality. Specifically, the aim is to estimate the effect of the current national screening programmes in the United Kingdom on breast cancer mortality. Estimates of relative risk reduction, absolute risk reduction, and increase in life expectancy are discussed.
You May Like: What Does Triple Negative Cancer Mean