What Should I Expect Before During And After The Magnetic Resonance Imaging Exam
Before the exam
- If you have been given an implant card to carry in your wallet, be sure to bring it with you to your MRI appointment.
- Personal items such as your watch, wallet — including any credit cards with magnetic strips — and jewelry/body piercing jewelry should be left at home if possible, or removed prior to the MRI scan. Secured lockers are available to store personal possessions. Other metal objects that need to be left at home or stored in the locker include dentures/partial plants, eyeglasses, hearing aids, hair pins/barrettes, keys, cell phones and beepers.
- You will be required to change into a hospital gown for the MRI scan.
- Your breast MRI exam requires an injection of a contrast material called gadolinium. The contrast improves the quality of the scan images. The contrast material will be injected into an IV line that has been inserted into your hand or arm.
During the exam
After the exam
- Generally, you can resume your usual activities and normal diet immediately. However, if your exam was an MRI breast biopsy, please follow your home-going instruction given to you after the procedure. If you received anesthesia, please follow the home-going instructions given to you by the radiologist .
- The results of your MRI should be available to your physician within 24 hours after your test, Monday through Friday.
- Your physician will discuss the test results with you.
Keep in mind. . .
Last reviewed by a Cleveland Clinic medical professional on 10/29/2019.
References
What Can I Expect After A Breast Mri
A breast MRI is usually an outpatient procedure. You can go home and resume your normal activities right away unless your doctor tells you otherwise.
The results of your breast MRI will determine your next steps. Benign results mean there is no cancer and no further treatment may be necessary. If the results indicate a problem, you may need more imaging exams, additional diagnostic tests , or treatment.
How Does Mri Work
An MRI scanner is a long cylinder or tube that holds a large, very strong magnet. You lie on a table that slides into the tube, and the machine surrounds you with a powerful magnetic field. The machine uses a powerful magnetic force and a burst of radiofrequency waves to pick up signals from the nuclei of hydrogen atoms in your body. A computer converts these signals them into a black and white picture.
Contrast materials can be put into the body through a vein to clearer images. Once absorbed by the body, the contrast speeds up the rate at which tissue responds to the magnetic and radio waves. The stronger signals give clearer pictures.
Also Check: Signs Of Breast Cancer Metastasis
What Happens After A Breast Mri
You should move slowly when getting up from the scanner table to avoid any dizziness or lightheadedness from lying prone for the length of the procedure.
If any sedatives were taken for the procedure, you may be required to rest until the sedatives have worn off. You will also need to avoid driving.
If contrast was used during your procedure, you may be monitored for a period of time for any side effects or reactions to the contrast, such as itching, swelling, rash, or difficulty breathing.
If you notice any pain, redness, and/or swelling at the IV site after you return home following your procedure, you should notify your health care provider, as this could indicate an infection or other type of reaction.
Nursing mothers may choose not to breastfeed for 12 to 24 hours after a breast MRI with contrast.
Generally, there is no special type of care required after a breast MRI scan. You may resume your usual diet and activities, unless your health care provider advises you differently.
Your health care provider may give you additional or alternate instructions after the procedure, depending on your particular situation.
The Many Shades Of Breast Imaging Studies: A Comparison Of Mammogram Vs Ultrasound Vs Breast Mri
Breast radiologists the physicians who specialize in screening and diagnosing women with breast cancer are used to seeing shades of black, white, and grey all day long. But what does that mean when it comes to breast imaging?
Color, or the absence of color, means everything in imaging studies. Breast abnormalities such as calcifications, lesions, or masses may show up differently or not at all depending on the imaging modality being used.
While most patients are familiar with mammography, radiologists also use ultrasound and magnetic resonance imaging to evaluate breast tissue in an effort to detect breast cancer as early as possible. With that said, patients may wonder what the differences are between these techniques and how to know which study might be best for them.
In most cases, the answer to which study is best isnt a simple or straightforward decision, explains Raleigh Radiology fellowship-trained interventional breast radiologist Dr. Svati Singla Long: Due to the complexities around breast imaging, your OB/GYN or primary care doctor will work with your radiologist to determine which imaging tool is best for you based upon your overall risk of breast cancer and/or your current breast complaint.
Dr. Long continues by explaining that among the three modalities: mammography, ultrasound, and MRI. None are necessarily better than the other, but instead, they work together as needed to give the radiologist a full picture of your breast tissue.
Don’t Miss: What Does Her2 Negative Mean In Breast Cancer
How Is The Term High Risk Defined Specifically Regarding Women And Breast Cancer
High risk defines when radiologists use breast MRIs. Several risk models use modeling techniques to predict risk for breast cancer. Each of these risk models has benefits and drawbacks, with factors such as age, race, BMI, parity, age at first menstrual cycle, and personal and family history of breast cancer.
In addition, women with BRCA1 or BRCA2 gene mutations, untested women who have a first degree family member with a known BRCA1 or BRCA2 mutation, and women with a history of chest radiation between the ages of 10 and 30 are considered high risk and are recommended for annual screening MRI.
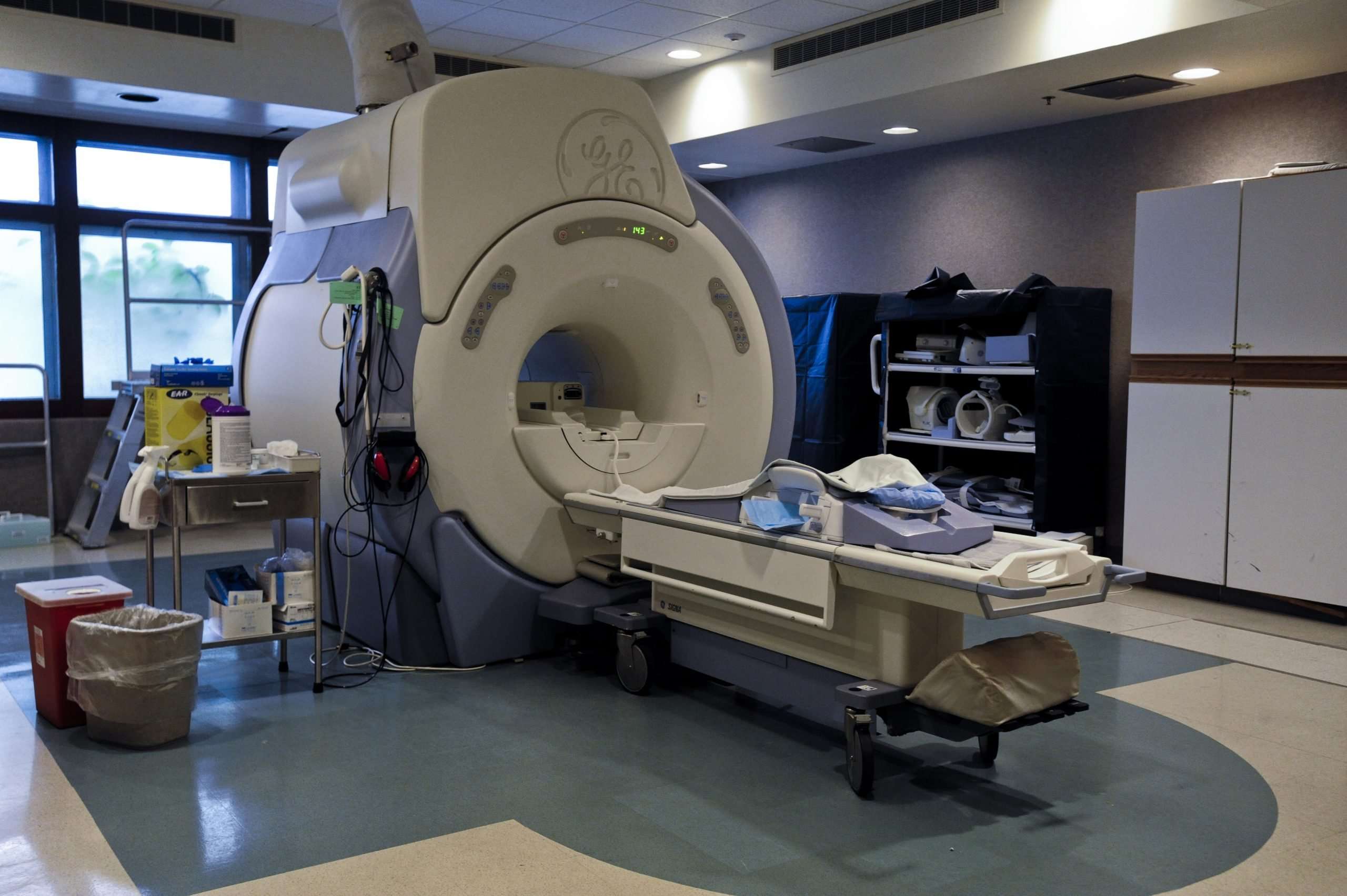
What Does The Equipment Look Like
The traditional MRI unit is a large cylinder-shaped tube surrounded by a circular magnet. You will lie on a table that slides into a tunnel towards the center of the magnet.
Some MRI units, called short-bore systems, are designed so that the magnet does not completely surround you. Some newer MRI machines have a larger diameter bore, which can be more comfortable for larger patients or those with claustrophobia. “Open” MRI units are open on the sides. They are especially helpful for examining larger patients or those with claustrophobia. Open MRI units can provide high quality images for many types of exams. Open MRI may not be used for certain exams. For more information, consult your radiologist.
Read Also: Stage 3a Breast Cancer
Continue Learning About Breast Cancer Diagnosis
Important: This content reflects information from various individuals and organizations and may offer alternative or opposing points of view. It should not be used for medical advice, diagnosis or treatment. As always, you should consult with your healthcare provider about your specific health needs.
What Are The Possible Complications Of An Mri
People can be hurt in MRI machines if they take metal items into the room or if other people leave metal items in the room.
Some people become very uneasy and even panic when lying inside the MRI scanner.
Some people react to the contrast material. Such reactions can include:
- Nausea
- Pain at the needle site
- A headache that develops a few hours after the test is over
- Low blood pressure leading to a feeling of lightheadedness or faintness
Be sure to let your health care team know if you have any of these symptoms or notice any other changes after you get the contrast material.
Gadolinium, the contrast material used for MRI, can cause a special complication when its given to patients on dialysis or who have severe kidney problems, so its rarely given to these people. Your doctor will discuss this with you if you have severe kidney problems and need an MRI with contrast.
Small amounts of gadolinium can stay in the brain, bones, skin and other parts of your body for a long time after the test. Its not known if this might have any health effects, but so far, studies havent found any harmful effects in patients with normal kidneys.
Don’t Miss: How Quickly Can Breast Cancer Grow
What Is It Like To Have A Magnetic Resonance Imaging Scan
Many people are nervous about a magnetic resonance imaging test because they fear being enclosed in a tight space. Its true that the older machines were narrow with the tight head-to-ceiling space. However, newer machines have greatly improved patients comfort. The newer machines are open bore, meaning they are open at both ends. The newer MRI machines also have wider openings, shorter total length, better interior lightening, more head-to-ceiling space, more arm/body room, and are fully ventilated . In some cases, if only a lower body scan is needed, a patients head and torso can remain outside the machine.
If you are nervous about the MRI test or fear closed spaces, talk to your doctor. If needed, your doctor will discuss options for medicine or even anesthesia if necessary.
Conventional Vs Fast Breast Mri
Women who have dense breasts are at an increased risk of developing breast cancer, and dense breasts make mammograms less sensitive. In some states, women who are found to have dense breasts on mammography are now required to be informed of the diagnosis and may wish to undergo additional testing.
Combining mammography and breast ultrasound has been found to improve detection to some degree, but with an increased risk of false positives.
A newer MRI technique referred to as fast breast MRI or abbreviated MRI may be combined with mammography in this situation. Unlike conventional MRI, a fast MRI takes only around 10 minutes, and unlike the high cost of conventional MRI, fast MRI costs roughly the same as a mammogram.
In studies thus far, the combination of mammography with fast MRI detected significantly more breast cancers than mammography alone , especially aggressive breast cancers. Since the technique is relatively new, it is not yet available at all breast cancer screening centers.
Don’t Miss: Hormone Therapy For Breast Cancer Stage 4
Johns Hopkins Medicines Mammogram Guidelines
We strongly recommend that women begin screening mammography at the age of 40 and continue annually until their life expectancy is less than five years due to comorbid disease. In the United
States, a woman is diagnosed with breast cancer every three minutes, and 12% of those women are in their 40s. A woman dies of breast cancer in the United States every 13 minutes. Screening and early detection can help us provide better care for breast cancer patients in the United States.
Importance Of Breast Mri
Breast MRI with dedicated breast coils uses strong magnets instead of radiation to make very detailed, cross-sectional pictures of the inside of the breast. Breast MRI scanner takes pictures from several angles in order to produce the imaging results with high level of accuracy. Breast MRI creates pictures of soft tissue parts that would sometimes be difficult to see when using other imaging tests. Benefits of breast MRI classified by different groups of patients include:
1.) For breast cancer screening: To screen for breast cancer, based on risk levels, women are grouped into:
High risk group: Women who fall into high risk group possess a lifetime risk of breast cancer of about 20%, or greater, compared to normal population. High risk is defined as below:
- Having first degree relatives diagnosed with breast cancer e.g. mother, grandmother, daughter and sibling with similar mother
- Having genetic mutations of BRCA1 or BRCA2
- Receiving previous radiation treatments to the chest when aged between 10-30 and
- Being diagnosed with certain diseases that increase chances of developing breast cancer e.g. Li-Fraumeni Syndrome, Cowden Syndrome or Bannayan-Riley-Ruvalcaba syndrome.
Recommendations for high risk group: For women at high risk for breast cancer, a screening MRI is highly recommended along with a yearly mammogram, staring at age 25-30.
Recommendations for intermediate risk group: For women at intermediate risk for breast cancer, MRI is recommended once a year.
Also Check: Triple Positive Breast Cancer Stage 4
Why Is A Breast Mri Needed
This test has many uses:
-
Screen for breast cancer in people who are at a high risk for the disease or have a personal history of breast cancer.
-
Diagnose and evaluate breast tumors. An MRI may identify a small mass within a breast better than a mammogram or ultrasound. This is particularly true for very dense, non-fatty breast tissue.
-
Learn more about a tumor that a doctor feels in the breast but cannot see on a mammogram or ultrasound.
-
Determine the size of the tumor after an initial breast cancer diagnosis.
-
Monitor how well chemotherapy is working to treat the cancer by checking to see if the cancer is shrinking.
-
Find a rupture of a breast implant.
How Is The Procedure Performed
MRI exams may be done on an outpatient basis.
The technologist will position you on the moveable exam table. They may use straps and bolsters to help you stay still and maintain your position.
For an MRI of the breast, you will lie face down on a platform specially designed for the procedure. The platform has openings to accommodate your breasts and allow them to be imaged without compression. The electronics needed to capture the MRI image are actually built into the platform. It is important to remain very still throughout the exam. This is best accomplished by making sure you are comfortable and can relax rather than trying to actively hold still tensing your muscles. Be sure to let the technologist know if something is uncomfortable, since discomfort increases the chance that you will feel the need to move during the exam.
If MRI of the breast is being performed for the sole purpose of determining if you have a ruptured breast implant, you will not be given contrast material. If the exam is being performed for any other reason, you will need to have a contrast material injected intravenously. MRI of the breast without contrast material is inadequate for identifying breast cancers.
If your exam uses a contrast material, a doctor, nurse, or technologist will insert an intravenous catheter into a vein in your hand or arm. They will use this IV to inject the contrast material.
Don’t Miss: Stage 3 Lymphatic Cancer
Why You Might Have It
For women with lobular breast cancer a breast MRI scan might be used to see the cancer. This is because lobular breast cancer doesn’t show up well on a mammogram or breast ultrasound. A breast MRI scan might also be used to assess the size of the cancer to check which kind of surgery is possible.
MRI scan is also used in breast screening for young women who are at higher risk of developing cancer. They might be at higher risk due to having family members with cancer or because they have certain gene abnormalities .
You might have an MRI scan if you have chemotherapy before surgery . You have this before and after your chemotherapy. This shows how well the chemotherapy is working.
Recommendations By The Study
An annual MRI should be done on women at high risk who have a strong family history of breast cancer as an alternative to surgical breast removal.
The paper points out that the combination of mammography and ultrasound cannot detect all types of breast cancer.
Women with dense breasts DO have the option to request an MRI and will likely have to pay out of pocket for it.
Dr. Mendi has published several articles in radiology journals and has expertise in MRI, womens imaging, musculoskeletal, neurological and body imaging.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. Shes also a former ACE-certified personal trainer.
Top image: cancer.gov/ Bruce Wetzel and Harry Schaefer
Read Also: Anne Hathaway’s Breasts
What Are The Most Common Uses For A Breast Mri
The most common use for breast MRI is high risk screening, which is indicated annually to supplement a mammogram for women who have a 20% or greater lifetime risk of breast cancer.
The 20% or greater lifetime risk is determined by one of multiple risk models. They are found online for example, on the National Cancer Institute website.
Recent literature supports the use of screening MRI for women with a personal history of breast cancer and dense breast tissue, as well as when a woman has a recent diagnosis of breast cancer.
Of the breast imaging modalities, MRIs have been shown to demonstrate the most accurate extent of disease of any of the breast imaging modalities. Our breast imaging specialists also look at the contralateral breast when there is a new breast cancer diagnosis. The data demonstrates that 3% to 5% of women will have asynchronous contralateral breast cancer, which is critical to diagnose at the time of breast cancer treatment.
The breast MRI can also identify the extent of the cancer that has been biopsied by determining if cancer is in more than one quadrant, and if the chest wall or the skin and nipple are involved. The MRI can help breast surgeons determine whether a lumpectomy or mastectomy should be planned.
Difficult imaging problem: Occasionally, when a definitive lesion cannot be identified by mammography or ultrasound, a breast MRI can help sort out the findings that are confusing on previous imaging.
Before The Breast Mri
A breast MRI can be done in a hospital or outpatient clinic. A radiologist or radiology technologist may perform the test. A radiologist is a medical doctor who performs and interprets imaging tests to diagnose disease. A radiology technologist is specially trained and certified to perform MRI scans but not interpret them.
You will need to remove all jewelry or other metal objects before the exam. You also may need to change into a hospital gown.
A nurse or doctor will give you gadolinium through an intravenous line. They will insert a small needle into a vein in your arm or hand. This needle connects to a tube. At first, saline solution flows through the IV line and then gadolinium dye. The dye travels through your bloodstream and helps create a clearer picture of your breasts.
People having a breast MRI for a ruptured implant do not need the dye. For some people, the dye causes allergic reactions. It may also cause complications in people with kidney or liver problems. So, be sure to tell your doctor about any health conditions you may have before the test.
A breast MRI is not painful. But if you receive an IV, the needle injection can be uncomfortable. The saline solution in the IV may cause a cool feeling at the injection site.
You May Like: Estrogen And Progesterone Positive Breast Cancer Prognosis