How Does My Doctor Test For Ki
To test for Ki-67,* your doctor may send a sample of previously biopsied breast cancer tissue to a lab for analysis. You’ll receive the results in your pathology report, which will show what percentage of cancer cells express Ki-67. In the monarchE study, Ki-67 levels 20% indicated ‘high’ Ki-67. If levels of Ki-67 are high, that means cancer cells are quickly dividing and creating new cells.
How Often Does Stage 1 Breast Cancer Come Back After Treatment
If stage 1 cancer is treated comprehensively, it rarely comes back. A new, unrelated breast cancer is more likely to emerge after stage 1 breast cancer is treated than a recurrence. Your healthcare provider will recommend a surveillance schedule for you so that new breast cancer or a recurrence can be identified and treated as quickly as possible.
Neoadjuvant Chemotherapy Neoadjuvant Her2
With neoadjuvant chemotherapy, all the chemotherapy to treat the breast cancer is usually given before surgery . If the tumor doesnt get smaller with the first combination of chemotherapy drugs, other combinations can be tried.
If your tumor is HER2-positive, you may get neoadjuvant trastuzumab and neoadjuvant pertuzumab , but not at the same time as the chemotherapy drug doxorubicin .
If your tumor is estrogen receptor-negative, progesterone receptor-negative and HER2-negative with a high risk of recurrence, you may get neoadjuvant pembrolizumab . Pembrolizumab is an immunotherapy drug.
Don’t Miss: Breast Cancer Medications After Surgery
Playing An Active Role
You play an active role in making treatment decisions by understanding your breast cancer diagnosis, your treatment options and possible side effects.
Together, you and your health care provider can choose treatments that fit your values and lifestyle.
|
The National Academy of Sciences released the report, Delivering High-Quality Cancer Care: Charting a New Course for a System in Crisis in 2013. Susan G. Komen® was one of 13 organizations that sponsored this study. The report identified key ways to improve quality of care:
|
How Is A Local Recurrence After Lumpectomy Diagnosed

After a diagnosis of early stage breast cancer, any remaining breast tissue should be evaluated annually with scans .
Most local recurrences within the breast after lumpectomy are detected on routine annual breast imaging, which usually takes the form of mammography and ultrasound, and on occasions MRI.
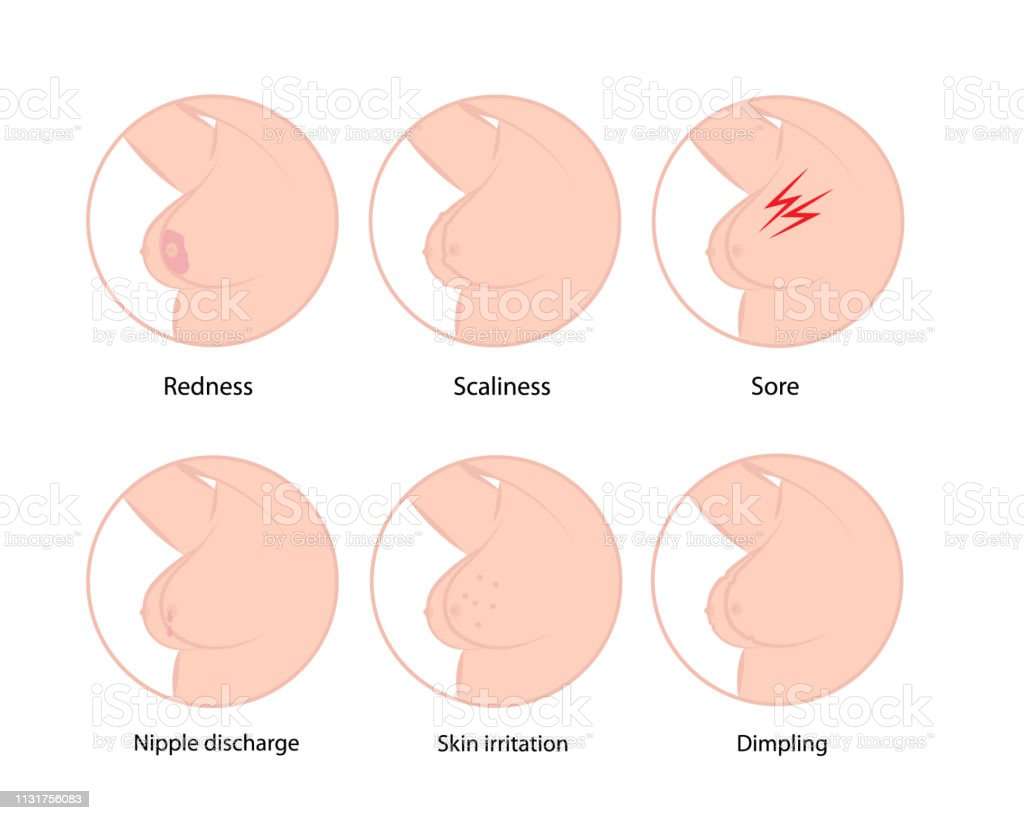
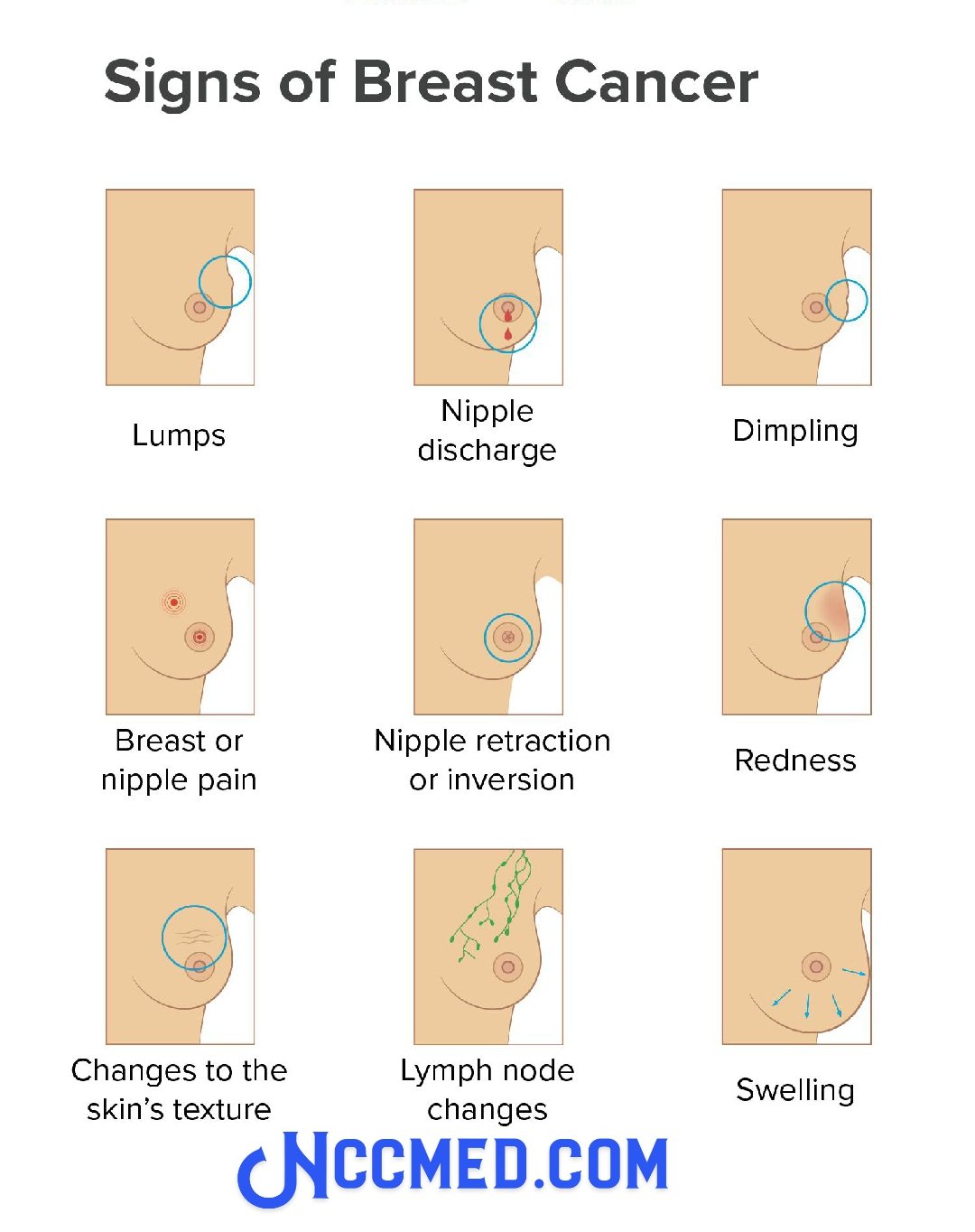
If you have a local recurrence or new primary breast cancer, you may find symptoms similar to an initial breast cancer. This includes:
- A new lump in the breast, armpit area or around the collarbone
- A change in breast size or shape
- Changes to the nipple, such as sores or crusting, an ulcer or inverted nipple
- Clear or bloody nipple discharge
- Changes to the skin including redness, puckering or dimpling
- Breast tenderness or pain
Once a local recurrence has been diagnosed, we do tests to see whether there are signs of cancer elsewhere in the body. These may include a chest X-ray, CT scan, bone scan or PET scan, and blood tests , then we have to figure out how best to treat the tumour in the breast. Usually in these cases we do a mastectomy, as the prior less drastic surgery and radiation didnt take care of it.
Read Also: Stage Iv Breast Cancer Symptoms
Also Check: Breast Cancer Age Of Onset
How Can I Protect Myself From Breast Cancer
Follow these three steps for early detection:
- Get a mammogram. The American Cancer Society recommends having a baseline mammogram at age 35, and a screening mammogram every year after age 40. Mammograms are an important part of your health history. Recently, the US Preventive Services Task Force came out with new recommendations regarding when and how often one should have mammograms. These include starting at age 50 and having them every two years. We do not agree with this, but we are in agreement with the American Cancer Society and have not changed our guidelines, which recommend yearly mammograms starting at age 40.
- Examine your breasts each month after age 20. You will become familiar with the contours and feel of your breasts and will be more alert to changes.
- Have your breast examined by a healthcare provider at least once every three years after age 20, and every year after age 40. Clinical breast exams can detect lumps that may not be detected by mammogram.
Diagnosis Of Breast Cancer
To determine if your symptoms are caused by breast cancer or a benign breast condition, your doctor will do a thorough physical exam in addition to a breast exam. They may also request one or more diagnostic tests to help understand whats causing your symptoms.
Tests that can help diagnose breast cancer include:
- Mammogram. The most common way to see below the surface of your breast is with an imaging test called a mammogram. Many women ages 40 and older get annual mammograms to check for breast cancer. If your doctor suspects you may have a tumor or suspicious spot, they will also request a mammogram. If an abnormal area is seen on your mammogram, your doctor may request additional tests.
- Ultrasound. A breast ultrasound uses sound waves to create a picture of the tissues deep in your breast. An ultrasound can help your doctor distinguish between a solid mass, such as a tumor, and a benign cyst.
Your doctor may also suggest tests such as an MRI or a breast biopsy.
If you dont already have a primary care doctor, you can browse doctors in your area through the Healthline FindCare tool.
You May Like: Breast Cancer Stage 4 Life Expectancy
The Stages Of Breast Cancer And Your Treatment Options
Compared to most other cancers, staging breast cancer is more complex. And when it comes to treating breast cancer, there isnt a one-size-fits-all approach. Your treatment plan should be created especially for you and be coordinated across specialists and thats where your cancer care team comes in.
At HealthPartners, we believe cancer treatment and care is best managed by a group of doctors and specialists in whats known as multidisciplinary conferences. This is where breast surgeons, oncologists, radiologists, pathologists and other members of your care team gather to discuss the best treatment sequence for you.
Below we dive into the treatment options your care team might recommend at various breast cancer stages.
What Is A Primary Tumor
The primary tumor refers to the original breast tumor. So, any metastases are either secondary tumors, or simply metastatic breast cancer.
Note, when breast cancer spreads to the bones, it is not bone cancer, it is metastatic breast cancer in the bones.
Metastatic describes a breast cancer that has already spread to distant areas and organs of the body. Metastatic cancer is the most advanced stage of breast cancer. Furthermore, the most common sites for breast cancer to metastasize to are the:-
- bones
- liver
- lungs.
Once breast cancer is at this most advanced metastatic stage, the odds of completely curing the breast cancer are quite low. .
The treatment of metastatic breast cancer, after a reasonable effort, will often focus on the quality of life and relieving symptoms rather than a cure.
Recommended Reading: Baking Soda And Honey Cancer
Who Gets Breast Cancer
Breast cancer is the most common cancer among women other than skin cancer. Increasing age is the most common risk factor for developing breast cancer, with 66% of breast cancer patients being diagnosed after the age of 55.
In the US, breast cancer is the second-leading cause of cancer death in women after lung cancer, and it’s the leading cause of cancer death among women ages 35 to 54. Only 5 to 10% of breast cancers occur in women with a clearly defined genetic predisposition for the disease. The majority of breast cancer cases are “sporadic, meaning there is no definitive gene mutation.
Inherited Breast Cancer And Risk Reduction
Family history is a known risk factor for breast cancer, with elevated risk due to both increasing number and decreasing age of first-degree relatives affected. For example, in a large, population-based study, risk of breast cancer was increased 2.9-fold among women whose relative was diagnosed prior to age 30, but the increase was only 1.5-fold if the affected relative was diagnosed after age 60 years. While twin studies indicate familial aggregation among women diagnosed with breast cancer, identification of true germline mutations, including BRCA1, BRCA2, p53 , PTEN , and STK11 , are quite rare, on the order of 5%-6%.- However, the management of young women at an increased risk of developing breast cancer via a germline mutation requires careful consideration, as screening, risk reduction, and implications for relatives are of upmost importance.
You May Like: Hormone Therapy For Breast Cancer Stage 4
Types Of Stage 1 And 2 Breast Cancer
The most common types of invasive breast cancers are named after the area of the breast where they begin. Types of early breast cancers include:
- Invasive ductal carcinoma IDC means that the cancer originated in the milk ducts of the breast, and has spread into the surrounding breast tissue. IDC is the most common type of breast cancer, accounting for 80% of all breast cancers.
- Invasive lobular carcinoma ILC means that the cancer originated in the milk-producing lobules of the breast, and has spread into the surrounding breast tissue. ILC is the second most common type of breast cancer, and accounts for 10% of breast cancers.
- There are also other less common forms of invasive breast cancer, such as inflammatory breast cancer and Pagets disease of the nipple. For more information on the various types of invasive breast cancer, including the less common forms, please visit Types of Breast Cancer page.
What Is Breast Cancer
Cancer occurs when changes called mutations take place in genes that regulate cell growth. The mutations let the cells divide and multiply in an uncontrolled way.
Breast cancer is cancer that develops in breast cells. Typically, the cancer forms in either the lobules or the ducts of the breast.
Lobules are the glands that produce milk, and ducts are the pathways that bring the milk from the glands to the nipple. Cancer can also occur in the fatty tissue or the fibrous connective tissue within your breast.
The uncontrolled cancer cells often invade other healthy breast tissue and can travel to the lymph nodes under the arms. The lymph nodes are a primary pathway that help the cancer cells move to other parts of the body.
You May Like: Tubular Breast Cancer Symptoms
About Those Lymph Nodes
A surgeon will usually take a lymph node biopsy to determine if the breast cancer has spread to the axillary lymph nodes. This is not always necessary, however. A lymph node biopsy is not usually necessary for DCIS. However, for invasive breast cancer, yes, they do need to check the lymph nodes.
Sometimes, doctors will perform a sentinel node biopsy, rather than a full lymph node excisional biopsy if the concerns about cancer spread are minimal. Cancer cells tend to appear first in the sentinel node before spreading to the other nodes, or other areas of the body.
Clinicopathologic Features Biology And Prognosis
The comparison of clinicopathologic and prognostic features of breast cancer arising in younger women with those in their older counterparts has been the subject of published studies for decades.- Traditionally, breast cancer arising in a younger host is characterized by a more aggressive phenotype. Among 185 premenopausal women carrying a diagnosis of invasive breast cancer, referred for surgery at the European Institute of Oncology from April 1997 to August 2000, those aged less than 35 years had a higher percentage of ER-negative , progesterone receptor -negative , vascular or lymphatic invasion and pathologic grade 3 tumors compared with women aged 35-50 years. Differences in tumor size, lymph node involvement, and Her2/neu status between younger and older women diagnosed with breast cancer have been less clear.-
Don’t Miss: Stage 3a Breast Cancer Treatment
How Can I Prevent Breast Cancer Recurrence
Healthcare providers dont know why some people experience breast cancer recurrence. A recurrence isnt your fault. You didnt do anything wrong to cause it or fail to do something more to prevent it.
Certain medications may reduce the risk of breast cancer recurrence in people who have early stage breast cancer. For estrogen-receptive breast cancer, hormonal therapies including tamoxifen or aromatase inhibitors block either the activity of estrogen or the bodys production of estrogen. Chemotherapy may also be recommended to reduce risk of breast cancer recurrence.
Early diagnosis may make it easier to treat a recurrence. Follow your healthcare providers recommendations for mammograms and other screenings. You should also perform regular breast self-exams. Get familiar with how your breasts look and feel so you can see your provider quickly if you notice changes. And remember that most breast changes occur for reasons other than cancer.
Breast Cancer Diagnosed During Or After Pregnancy
Being pregnant at the time of diagnosis of breast cancer has been associated with a worse outcome. In one study of 797 such cases, compared with 4,177 non-pregnancy-associated breast cancer controls, women diagnosed while pregnant had larger, more advanced tumors, a greater incidence of receptor-negative tumors, and a higher death rate . A smaller study found no association between pregnancy and increased mortality. In contrast, pregnancy and childbirth following a diagnosis of breast cancer do not increase mortality, and actually may improve survival. One study found that 438 women age < 45 years at diagnosis, who delivered a child 10 or more months following a diagnosis of breast cancer, had a decreased relative risk of death , compared to women who did not bear children following diagnosis. Women who were pregnant at the time they were diagnosed had a mortality rate similar to the latter group. This suggests that childbirth following breast cancer diagnosis does not increase mortality.
Recommended Reading: Milk Duct Cancer Symptoms
How Much Do Tamoxifen And Raloxifene Lower The Risk Of Breast Cancer
Multiple studies have shown that both tamoxifen and raloxifene can reduce the risk of developing estrogen receptor-positive breast cancer in healthy postmenopausal women who are at high risk of developing the disease. Tamoxifen lowered the risk by 50 percent. Raloxifene lowered the risk by 38 percent. Overall, the combined results of these studies showed that taking tamoxifen or raloxifene daily for five years reduced the risk of developing breast cancer by at least one-third. In one trial directly comparing tamoxifen with raloxifene, raloxifene was found to be slightly less effective than tamoxifen for preventing breast cancer.
Both tamoxifen and raloxifene have been approved for use to reduce the risk of developing breast cancer in women at high risk of the disease. Tamoxifen is approved for use in both premenopausal women and postmenopausal women . Raloxifene is approved for use only in postmenopausal women.
Less common but more serious side effects of tamoxifen and raloxifene include blood clots to the lungs or legs. Other serious side effects of tamoxifen are an increased risk for cataracts and endometrial cancers. Other common, less serious shared side effects of tamoxifen and raloxifene include hot flashes, night sweats, and vaginal dryness.
What Are The Different Grades Of Breast Cancer
There are three grades of invasive breast cancer:
- Grade 1 looks most like normal breast cells and is usually slow growing
- Grade 2 looks less like normal cells and is growing faster
- Grade 3 looks different to normal breast cells and is usually fast growing
Sometimes the grade given to a cancer after a biopsy can change after surgery. This is because after surgery theres more tissue for the pathologist to look at, which can give them more detailed information about the cancer.
Recommended Reading: Red Mill Baking Soda Cancer
N Categories For Breast Cancer
N followed by a number from 0 to 3 indicates whether the cancer has spread to lymph nodes near the breast and, if so, how many lymph nodes are involved.
Lymph node staging for breast cancer is based on how the nodes look under the microscope, and has changed as technology has gotten better. Newer methods have made it possible to find smaller and smaller groups of cancer cells, but experts haven’t been sure how much these tiny deposits of cancer cells influence outlook.
Its not yet clear how much cancer in the lymph node is needed to see a change in outlook or treatment. This is still being studied, but for now, a deposit of cancer cells must contain at least 200 cells or be at least 0.2 mm across for it to change the N stage. An area of cancer spread that is smaller than 0.2 mm doesn’t change the stage, but is recorded with abbreviations that indicate the type of special test used to find the spread.
If the area of cancer spread is at least 0.2 mm , but still not larger than 2 mm, it is called a micrometastasis . Micrometastases are counted only if there aren’t any larger areas of cancer spread. Areas of cancer spread larger than 2 mm are known to influence outlook and do change the N stage. These larger areas are sometimes called macrometastases, but are more often just called metastases.
NX: Nearby lymph nodes cannot be assessed .
N0: Cancer has not spread to nearby lymph nodes.
N1c: Both N1a and N1b apply.
N3: Any of the following:
N3a: either:
N3b: either:
Treatment Of Stage Iii Breast Cancers
Sometimes large breast cancers invade into muscles or attach to major arteries, veins or nerve trunks, which makes them impossible to surgically remove completely.
So, for these patients, the treatment usually starts with radiation or chemo to try to shrink it first, before surgery. But even a large tumor that has not attached itself onto muscle can, sometimes, be completely removed. There is no direct relationship between tumor size and whether or not it may be treated surgically or not.
Obviously, Stage 3 breast cancers that surgeons can completely remove do tend to have a significantly better prognosis than inoperable stage 3 breast cancers. However, some breast tumors, particularly those that are ER-positive, respond very well to chemotherapy. So well, in fact, that they actually downstage.
So, it is difficult to predict the overall prognosis for stage 3 breast cancer, as it will vary from individual to individual. If the response to chemotherapy is favorable, the overall survival rate is around 72%.
Read Also: Treatment For Stage 3 Breast Cancer