How To Care For Surgical Drains
When you wake up from surgery, your recovery room nurse will probably warn you that you need to be careful with your drains. Depending on the length of the tubes , it’s easy to get these tangled up with IV lines, your bedclothes, and anything else nearby.
Your nurse will periodically drain your bulbs and show you how it’s done. He or she will log the amount of drainage from each tube, and you will be instructed to continue the log on your own until your drains are removed.
Before you leave the hospital, your healthcare team will review drain management, tell you about symptoms that should prompt you to call, and schedule a follow-up visit to have them removed.
Who Might Get A Mastectomy
Many women with early-stage cancers can choose between breast-conserving surgery and mastectomy. You may prefer mastectomy as a way to “take out all the cancer as quickly as possible.” But the fact is that in most cases, mastectomy does not give you any better chance of long-term survival compared to BCS. Studies of thousands of women over more than 20 years show that when BCS is done along with radiation, the outcome is the same as having a mastectomy.
Mastectomy might be recommended if you:
- Are unable to have radiation therapy
- Would prefer more extensive surgery instead of having radiation therapy
- Have had the breast treated with radiation therapy in the past
- Have already had BCS with re-excision that did not completely remove the cancer
- Have two or more areas of cancer in different quadrants of the same breast that are not close enough to be removed together without changing the look of the breast too much
- Have a tumor larger than 5 cm across, or a tumor that is large relative to your breast size
- Are pregnant and would need radiation therapy while still pregnant
- Have a genetic factor such as a BRCA mutation, which might increase your chance of a second cancer
- Have a serious connective tissue disease such as scleroderma or lupus, which may make you especially sensitive to the side effects of radiation therapy
- Have inflammatory breast cancer
Simple Or Total Mastectomy
Your doctor removes your entire breast, including the nipple, in this procedure. They donât remove your lymph nodes, small glands that are part of your immune system.
Youâre most likely to have this procedure when the cancer isnât in your lymph nodes, or if youâre having a mastectomy to lower your risk of getting breast cancer.
Don’t Miss: Stage-three Cancer
Breast Reconstruction Surgery After Mastectomy
After having a mastectomy a woman might want to consider having the breast mound rebuilt to restore the breast’s appearance. This is called breast reconstruction. Although each case is different, most mastectomy patients can have reconstruction. Reconstruction can be done at the same time as the mastectomy or sometime later.
If you are thinking about having reconstructive surgery, its a good idea to discuss it with your surgeon and a plastic surgeon before your mastectomy. This allows the surgical teams to plan the treatment thats best for you, even if you wait and have the reconstructive surgery later. Insurance companies typically cover breast reconstruction, but you should check with your insurance company so you know what is covered.
Some women choose not to have reconstructive surgery. Wearing a breast prosthesis is an option for women who want to have the shape of a breast under their clothes without having surgery. Some women are also comfortable with just going flat.
Breast Cancer Surgery Options
Knowing your surgical options can help you face breast cancer head on
From the awkward excitement of putting on your first training bra to the profound tenderness of nursing your first baby, you have a deeply personal relationship with your breasts. But when women are diagnosed with breast cancer, that relationship is forever changed.
“Decisions about breast surgery can be very complicated and very emotional,” says Claudia Perez, DO, a breast surgeon at Rush. “It’s not just about cosmetics, it’s about your femininity and your sense of self.”
Surgery is considered the primary treatment for breast cancer the only women who may not typically have surgery are those who have metastatic breast cancer that has spread to places like the liver or bones.
However, breast cancer is unique compared to other cancers that are treated surgically because there are more surgical options for breast cancer. Your doctors will educate you about your options, and you will work together to make a shared decision about the best surgical option for you.
Making that decision with confidence starts with knowing what you’re up against and using that knowledge to make the best choice for yourself. These seven steps can help you get started.
Recommended Reading: Estrogen Receptive Breast Cancer Prognosis
Time To Treatment With Metastatic Breast Cancer
There is little research looking at the optimal time until treatment for metastatic breast cancer, though it appears that waiting more than 12 weeks has been linked with lower survival. In general, however, the goal of treatment with MBC is different than early stage disease. For most people, treatment for early-stage disease is aggressive, with the goal to reduce the risk of recurrence. With MBC, the goal is often to use the least amount of treatment necessary to control the disease.
Making Your Own Decision
Your breasts may be such an important part of your identity your sense of who you are that you’ll go to great lengths to preserve them. That’s a completely acceptable approach to take, no matter what your age or figure AS LONG AS it doesn’t endanger your overall health and chances for a full recovery.
You May Like: Baking Soda Honey Cancer
When To Call Your Healthcare Provider
You should call your surgeon if you have any concerns or questions at all, or if you develop any of the following problems:
- If your drainage is bright red for more than two or three days
- If you develop any signs or symptoms of an infection as noted above
- If a large amount of fluid is leaking from where the drain tubing is inserted into the surgical site
- If your drainage output suddenly decreases or stops abruptly
- If your drainage becomes thicker rather than thinner as time goes on
- If your bulb loses suction
- If your drain falls out
Why A Breast Lump Removal Is Performed
Breast lump removal is performed to prevent a cancerous tumor from spreading to other parts of your body. Whether a doctor can perform a lumpectomy depends on the size and stage of the tumor and certain patient characteristics such as the size of your breast.
Many doctors prefer this method over a mastectomy. A lumpectomy is less invasive that the entire removal of the breast. In a lumpectomy, your doctor takes a part of the breast, which leaves much of your breasts appearance and sensations intact. This allows for better breast symmetry. But you may need radiation or chemotherapy following a lumpectomy to ensure all cancer cells have been destroyed.
You May Like: 3a Breast Cancer
Why Might I Need A Mastectomy
A mastectomy may be done as part of treatment for breast cancer.
Your doctor will likely advise you to have a mastectomy if:
- The tumor is large
- The tumor involves more than 1 area of your breast
- Using radiation therapy is not advised
The size of your breast may also help determine the type of mastectomy thatis done.
In some cases, women with a high risk for breast cancer may want to have amastectomy before cancer develops. This includes women with genes linked tobreast cancer, such as the BRCA1 or BRCA2 gene. In these cases, amastectomy is done to try to keep breast cancer from occurring.
There may be other reasons for your doctor to recommend a mastectomy.
What Do Breast Look Like After Removal
As soon as you have removed your breast implants, your breasts will appear deflated. The breasts can take two to three weeks to regain their volume after they have been exposed to the sun. The appearance of your breasts wont be caved in if you had a breast lift after the breast implants were removed.
Recommended Reading: Malignant Breast Cancer Survival Rate
A Swollen Arm Or Hand
You are at risk of long term swelling in your hand and arm after surgery to remove your lymph nodes in the armpit. This is swelling caused by lymph fluid that can’t drain away. It can happen any time after surgery and radiotherapy to your armpit.
Not everyone will get this and it is less likely to happen if you only have a few nodes removed. But it is very important to speak to your specialist nurse or surgeon if you think your arm or hand may be swollen.
Unfortunately, once you have lymphoedema it cant be cured. But early treatment can help to control it. Your nurse will talk to you about ways of preventing lymphoedema.
How Long Does It Take To Recover From A Mastectomy
The bigger the operation, the longer the recovery time. Its typical to stay in the hospital for one day after a total mastectomy. Within about four weeks, youll probably be comfortable doing all of your regular daily activities.
You may need a longer hospital stay if the surgery you had was more involved, like a mastectomy with breast reconstruction using your own body tissue It can take a few months to feel fully recovered.
Recommended Reading: Will I Survive Breast Cancer
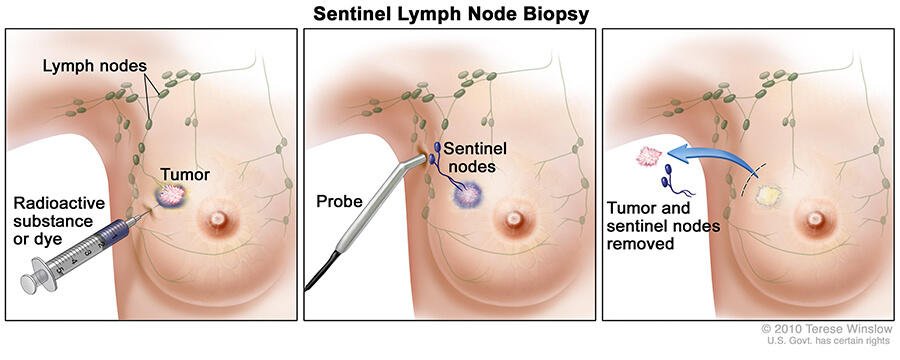
Getting The Results During Surgery
In some hospitals, the surgeon gets the results of the sentinel lymph node biopsy during the operation. This is called an intra operative assessment. They can remove the rest of the nodes if necessary. You then avoid having a second operation.
Your surgeon will explain this to you before your operation, so you know what to expect.
Scar Tissue In The Armpit
Some women develop scar tissue in the armpit after lymph node removal. The connective tissues in the armpit get inflamed, which forms one or more tight bands. This usually happens within the first few weeks or months after the operation.
The scar tissue is called cording or banding or axillary web syndrome. It can feel something like a guitar string. It can extend down the arm past the elbow, possibly as far as the wrist or thumb.
Cording is harmless but can be painful and can limit your arm movement. Massaging the area regularly can help. Tell your breast care nurse if you develop cording. They can refer you to a physiotherapist. They can show you how to massage the area and teach you stretching exercises. It usually gets better within a few months. Taking anti inflammatory painkillers may also help. Speak to your nurse or doctor about taking these.
-
Early Breast Cancer: ESMO Clinical Practice Guidelines 2019F Cardoso and others
-
Scottish Intercollegiate Guidelines Network, September 2013
-
A systematic review of axillary web syndrome WM Yeung and others
Also Check: Breast Cancer Type 3
Will A Prophylactic Mastectomy Prevent Breast Cancer
A prophylactic mastectomy removes the breast to prevent cancer. This is an option if breast cancer runs in your family. Through genetic testing, you can find out if you have inherited a higher risk of breast cancer. If so, you can discuss your options for high risk breast screening and may want to talk about prophylactic mastectomy with your healthcare provider. It reduces your risk of developing breast cancer by 85% to 100%.
Are Lymph Nodes Removed During A Lumpectomy
Women with invasive breast cancer typically have one or more lymph nodes taken from the underarm area during a lumpectomy. These nodes, called the sentinel nodes, are the first lymph nodes to which cancer cells would travel if they were to leave the breast. This is done so that your doctor can check to see if the cancer has spread.
Women with DCIS undergoing lumpectomy do not need to have lymph nodes removed.
Recommended Reading: Breast Cancer Stage 1 Grade 3
When Should I Call The Doctor
An infection near the incision site can be a serious health risk. You should call your healthcare provider right away if you have any of these symptoms in or near the affected breast:
- Swelling.
- Fluid that builds up in or around the breast.
- Redness.
- Pain that gets worse after surgery.
A note from Cleveland Clinic
Lumpectomy surgery can remove breast cancer while preserving natural breast tissue, which may help you feel more like yourself after cancer treatment. If retaining some of your breasts look and shape is important to you, ask your healthcare provider if a lumpectomy could benefit you. Certain factors may lead your provider to recommend a different treatment path. Your breast cancer treatment should be highly personalized to your needs.
Last reviewed by a Cleveland Clinic medical professional on 03/01/2021.
References
Tips For Mastectomy Recovery
Once youâre home, make sure you follow the plan your doctor gave you. Also make sure that you:
- Rest. Get plenty of it the first few weeks after surgery. It takes a lot out of you.
- Take your meds. Donât tough it out. Take the medication as prescribed. Youâll probably feel a mix of pain and numbness.
- Keep the site dry. Take sponge baths only until your drains and stitches are out.
- Do your exercises. Theyâll keep your arm from getting stiff.
- Ask for help. Donât be shy. It takes time to get better. Get all the help you can with meal prep, shopping, housework, child care, pet care, rides to doctorsâ appointments, and whatever else you arenât ready to take on by yourself.
Show Sources
American Cancer Society: “Surgery for Breast Cancer.” âMastectomy,â “Surgery for Breast Cancer in Men,” “Treatment of Breast Cancer in Men, by Stage.“
National Comprehensive Cancer Network: “Breast Cancer: Treatment Guidelines for Patients.”
Cancer Net: “Guide to Breast Cancer.”
BreastCancer.org: “What is Mastectomy?” âMastectomy: What to Expect,â “Rates of Preventive Double Mastectomy in Men Nearly Doubles.“
John Hopkins Medicine: âMastectomy.â
Manouras, A. Archives of Surgery, June 2008.
Mayo Clinic: “Modified Radical Mastectomy,â “Male breast cancer: Definition,” “Male breast cancer: Treatment and drugs.“
Townsend, C. Sabiston Textbook of Surgery, Saunders Elsevier, 2007.
Brunicardi, F. Schwartz’s Manual of Surgery, McGraw-Hill, 2006.
American Cancer Society:
Don’t Miss: Non Inflammatory Breast Cancer
What Is A Preventive Mastectomy
Women who have a high risk of breast cancer may choose to have a preventive mastectomy, also called prophylactic mastectomy.
Studies show that women with a high risk of breast cancer may be as much as 90% less likely to get the disease after preventive mastectomy.
Usually, doctors recommend a total mastectomy. In some cases, women have both breasts removed. This is called a double mastectomy.
Some women who’ve had breast cancer in one breast will have the other one removed to lower the chance of cancer coming back .
If you plan to have breast reconstruction, it can be done at the time of the preventive mastectomy or later on . During breast reconstruction, the surgeon may use synthetic implants or tissue flaps from another part of your body to create a breast.
Which Treatment Is Right For Me
Choosing the treatment that is right for you may be hard. Talk to your cancer doctor about the treatment options available for your type and stage of cancer. Your doctor can explain the risks and benefits of each treatment and their side effects. Side effects are how your body reacts to drugs or other treatments.
Sometimes people get an opinion from more than one cancer doctor. This is called a second opinion. Getting a second opinionexternal icon may help you choose the treatment that is right for you.
Links with this icon indicate that you are leaving the CDC website.
- The Centers for Disease Control and Prevention cannot attest to the accuracy of a non-federal website.
- Linking to a non-federal website does not constitute an endorsement by CDC or any of its employees of the sponsors or the information and products presented on the website.
- You will be subject to the destination website’s privacy policy when you follow the link.
- CDC is not responsible for Section 508 compliance on other federal or private website.
You May Like: Mayo Clinic Breast Cancer Stages
What Is A Nipple
You might also hear it called a total skin-sparing mastectomy. The doctor removes all the breast tissue, including the ducts going all the way up to the nipple and areola. But they save the skin of the nipple and areola and cut out tissues under and around them. If these areas are cancer-free, they can be saved. This method also calls for reconstruction right after the mastectomy.
What Should I Take With Me To Hospital
Your hospital team should provide you with information about your admission and hospital stay as well as what to take with you. Weve made some suggestions of what to take in our booklet Your operation and recovery, including what clothes and bra to wear after your surgery.
You will usually be given a telephone number at your pre-assessment appointment that you can call if you have any questions about preparing for surgery, or are unclear about any instructions you have been given .
Recommended Reading: Breast Cancer Weight Gain Before Diagnosis
Which Operation Should I Have
Some people will be offered a choice between breast-conserving surgery and a mastectomy.
Long-term survival is the same for breast-conserving surgery followed by radiotherapy as for mastectomy.
Studies show that women who have a wide local excision may be slightly more likely to have a local recurrence , which can be treated again. However, most people dont have a recurrence.
Insurance And Scheduling Problems
Some people find that the surgeon they’ve chosen under their insurance company isn’t available for longer than they would like to wait, or that it’s difficult to coordinate a surgeon and plastic surgeon on the same day in a reasonable amount of time. This can be more difficult some places than others. With the larger cancer centers, you may have a coordinator who will assist you in setting up appointments. In the community, you may need to do most of the legwork yourself.
Regardless, it’s important to be your own advocate. If you’re having difficulty, make sure to work with your insurance company. Sometimes they may cover a second or third tier provider if it’s the only option available for scheduling your surgery promptly . With some procedures, prior authorization is needed before scheduling can take place.
There are many breast cancer organizations that can assist you as well as help you make decisions. Support groups and online support communities are also an excellent option when it comes to questions and challenges along the way.
There are many options as well for those who are underinsured or uninsured, but again, it’s usually up to you to do the legwork. Programs such as the SAGE program are available, as well as many other assistance programs that can help with anything from transportation to childcare. Talking to a social worker at your cancer center can be invaluable in learning about your options.
You May Like: Hormone Receptor Positive Breast Cancer Prognosis