Tnbc Chemotherapy Drugs And Efficacy Evaluation
Compared to other types of breast cancer, TNBC has limited treatment options, is prone to recurrence and metastasis, and has a poor prognosis. The main reason is that the expression of ER, PR, and HER2 are all negative, making specific endocrine therapies and targeted therapies ineffective. Therefore, chemotherapy has become the main approach for the treatment of TNBC. In recent years, a large body of literature has shown that the use of neoadjuvant chemotherapy regimens in the treatment of TNBC has a significantly higher pathological remission rate than for hormone receptor-positive breast cancer and can significantly improve the prognosis of TNBC patients. The national comprehensive cancer network guidelines recommend using combination regimens based on taxane, anthracycline, cyclophosphamide, cisplatin, and fluorouracil. At present, taxel/docetaxel + adriamycin + cyclophosphamide , docetaxel + cyclophosphamide , adriamycin + cyclophosphamide , cyclophosphamide + methotrexate + fluorouracil , cyclophosphamide + adriamycin + fluorouracil , and cyclophosphamide + epirubicin + fluorouracil + paclitaxel/docetaxel are the preferred adjuvant regimens for TNBC. Therefore, the selection of appropriate chemotherapy drugs and the optimization of chemotherapy regimens are important for ensuring good treatment outcome and prognosis of TNBC patients.
Also Check: Do People Survive Stage 4 Breast Cancer
A New Era Of Hope For Patients With Triple
Triple-negative breast cancer is a particularly devastating subtype of breast cancer, as it is often diagnosed in young women and is associated with an exceptionally poor prognosis. The triple-negative designation indicates that the three key features driving most breast cancers are lacking, but it provides no clues as to potential biologic drivers. In the absence of any biologic insights, tailored, targeted treatment decisions have historically not been possible.
Consequently, until as recently as 2018, we have relied exclusively on nonselective cytotoxic agents, with modest success. For example, conventional neoadjuvant chemotherapy confers a pathologic complete response in just 50% to 55% of patients with early-stage triple-negative breast cancer,1-4 and among those who do not achieve a pathologic complete response, approximately one-third will die within 3 years.5 Moreover, patients with metastatic triple-negative breast cancer treated with conventional chemotherapeutics have a median survival of 12 to 18 months and an estimated 5-year overall survival of 11%.6 Thus, therapeutic innovation for early and late triple-negative breast cancer has been desperately needed.
Biologic Insight Leads to Therapies
From biologic insight springs hope for therapeutic innovation. Heather L. McArthur, MD, MPHTweet this quote
Immune Modulation Via Checkpoint Blockade
Antibody-Drug Conjugates
Forecast Finally Changing in Triple-Negative Disease
REFERENCES
Transcription Factors: Cebpb And En1
The CCAAT enhancer-binding protein beta is a TF regulating the expression of genes involved in inflammatory responses. High CEBPB has been correlated with expression of the chromosome 19 miRNA cluster , the expression of which has been linked to TNBC . Due to this association, it may also be worthwhile to compare C19MC expression in QNBC versus TNBC. The fact that CEBPB is induced under hypoxic conditions further emphasizes the need to determine the role of hypoxia in QNBC.
Don’t Miss: How To Cure Breast Cancer With Baking Soda
What Is Estrogen Receptor
Breast cancer cells sometimes have what are called receptors, which are tiny molecules of protein. Hormones may attach to specific receptors and trigger actions within the cell. Some types of cancerous, or malignant, breast tumors have cell receptors to which the hormoneestrogen attaches, stimulating the cells to grow. In the case of estrogen receptor-negative breast cancer, or ER-negative breast cancer, the cells do not have hormone receptors for estrogen. The presence or absence of estrogen receptors makes a difference to breast cancer treatment, because, with estrogen receptor-positive tumors, hormone therapies can be used which block the receptors, slowing breast cell growth.
A number of different hormone receptors may be found on breast cancer cells. As well as receptors specific to estrogen, other receptors may be present for the hormone progesterone or for a protein known as HER2. When receptors are found, treatments may be given using drugs which target those receptors and act against cancer growth. Some tumors will not show any of the receptors, in which case they are described as triple negative. As estrogen receptor-negative breast cancer does not respond to the body’s progesterone or estrogen levels, it is not usually possible to treat it using hormone therapies.
Immunophenotypic Features Of Blbc And Tn3bke
Cell cycle regulators and cell proliferation. A panel of eight cell cycle-associated proteins was analyzed. A significant association was found between BLBC and elevated levels of both p53 and p16 . When compared with TN3BKE- tumors, BLBC showed a positive association with the nuclear expression of c-Myc and high mitotic index as defined by phospho-histone 3 , indicating an association between BLBC and a growth fraction.
Luminal epithelial cell markers and other biomarkers. BLBC was associated with more frequent expression of luminal CK19 . Although BLBC showed lower levels of expression of CK18, this association was not significant . BLBC showed a positive association with the expression of neuroendocrine differentiation markers , hypoxia-associated factor , FHIT protein , and ER-1 . BLBC showed an association of borderline significance with the expression of P-cadherin .
Immunologic markers. BLBC showed a positive association with the expression of MHC class I polypeptide-related sequence A and HC10 . BLBC also showed an association of borderline significance with the expression of MUC2 .
Table 3.
Recommended Reading: What Are The Chances Of Getting Breast Cancer Twice
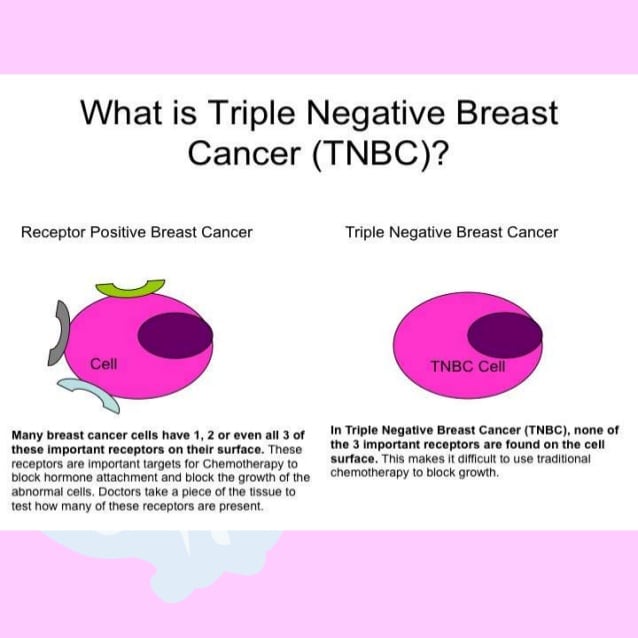
What Is Triple Negative Breast Cancer
Triple negative breast cancer is a rare cancer that affects about 13 in 100,000 women each year. It represents about 15 % of all invasive breast cancers. Triple negative breast cancer is one of three types of breast cancer. It is called as triple negative because it doesnt have three markers associated with other types of breast cancer, which is important for prognosis and treatment. Its one of the more challenging breast cancers to treat. But researchers are making steady progress toward more effective treatments. Overall, 77% of women who have triple negative breast cancer are alive five years after diagnosis.
Survival Rates And Prognosis
The outlook for breast cancer is often described in terms of relative survival rates.
Relative survival rates are an estimate of the percentage of people who will survive their cancer for a given period of time after diagnosis. Survival among people with cancer is compared to survival among people of the same age and race who have not been diagnosed with cancer.
Five-year relative survival rates tend to be lower for triple-negative breast cancer than for other forms of breast cancer.
According to the American Cancer Society, the overall 5-year relative survival rate for TNBC is 77 percent. However, an individuals outlook depends on many factors, including the stage of the cancer and the grade of the tumor.
Your healthcare professional will be able to give you a more precise outlook based on:
- the stage of your TNBC
- your age
Recommended Reading: Can Asbestos Cause Breast Cancer
Risk Factors And Epidemiologic Features
In addition to a distinct molecular and pathologic profile, the epidemiology and risk factors associated with triple-negative breast cancer are distinct, especially when compared with endocrine-sensitive luminal breast tumors. The Carolina Breast Cancer Study, a population-based, case-control study aimed at determining clinical associations and distributions across distinct breast cancer subtypes, has refined our understanding of the epidemiologic and risk factors associated with triple-negative breast cancer. In the initial study of women diagnosed with invasive breast cancer, the prevalence of breast cancer subtypes within racial and menopausal subsets were determined. Immunohistochemical staining was used to classify specific subtypes in approximately 500 tumors, and basal-like tumors were defined as triple negative and cytokeratin 5/6 positive and/or HER1 positive. Results indicated that those with basal-like tumors were more likely to be African American compared with nonAfrican American and premenopausal compared with postmenopausal . There was a particularly high prevalence of basal-like tumors among premenopausal African American women compared with postmenopausal African American women and nonAfrican American women of any age . The observation that triple-negative breast cancers more commonly arise in younger African American women has been confirmed in several additional studies, although the exact cause for this association is not yet fully understood.,
Nitrofen Reduces In Vitro Invasive Activity Of Breast Cancer Cells
Using an in vitro Matrigel invasion assay, we observed that TNBC cell lines showed higher invasive potential than non-TNBC cell lines . Further, nitrofen treatment reduced invasive potential of TNBC lines to a greater extent than non-TNBC lines . We further determined the effect of nitrofen on the invasive potential of the luciferase expressing MDA-MB-231 cell line . Accordingly, we used MDA-MB-231-luc-D3H2LN cells to carry out in vitro cell invasion assays in the presence and absence of 1 and 10 M nitrofen. We observed significant reduction in invasive potential of MDA-MB-231-Luc cells in the presence of 1 and 10 M nitrofen relative to untreated control . AlamarBlue assay done under the same conditions shows that there is no change in relative viability of cells upon any treatments .
Figure 1
Quantification of Matrigel invasion assay demonstrating that nitrofen significantly reduces the invasive potential of MDA-MB-231-Luc cells. Invasion assay was carried out using 40,000 cells/well, incubated for 24 h. Nitrofen was dissolved in Ethanol to prepare the stock concentration of 100 mM and diluted in DMSO to a final concentration of 1 uM and 10 uM. AlamarBlue cell viability assay done under the same conditions shows that there is no change in relative viability of cells upon treatments. Data representative of 6 separate experiments each done in triplicate. **significantly altered from untreated control p< 0.01.
Recommended Reading: Does Getting Hit In The Breast Cause Cancer
Is Triple Negative Breast Cancer An Aggressive Form Of Cancer
Its true that triple negative breast cancers can grow quickly. But your prognosis or expected outcome depends on more factors than your cancer subtype. Healthcare providers will also consider your tumors size and whether it has spread to your lymph nodes and other parts of your breast. Its also helpful to know researchers are focusing on ways to slow the spread of TNBC.
How Is Tnbc Diagnosed
Imaging tests are usually the first tests done:
- Mammography, the most common screening tool for breast cancer, uses X-rays to take images of the breast and can uncover tumors that may be too small to feel.
- MRI uses a magnet, radio waves and a computer to make detailed images of the breast with a much greater resolution than a mammogram offers.
The next step is a biopsy to remove a sample of suspicious cells from the breast to analyze them. Techniques include:
The appropriate type of biopsy for you depends on factors such as the size and location of the tumor. You may also have a biopsy of your underarm lymph nodes at the same time to see if any cancer is there.
You May Like: Did Anne Hathaway Have Breast Cancer
Advanced Cancer That Progresses During Treatment
Treatment for advanced breast cancer can often shrink the cancer or slow its growth , but after a time, it tends to stop working. Further treatment options at this point depend on several factors, including previous treatments, where the cancer is located, and a womanâs age, general health, and desire to continue getting treatment.
What Is The Prognosis For Triple Negative Breast Cancer
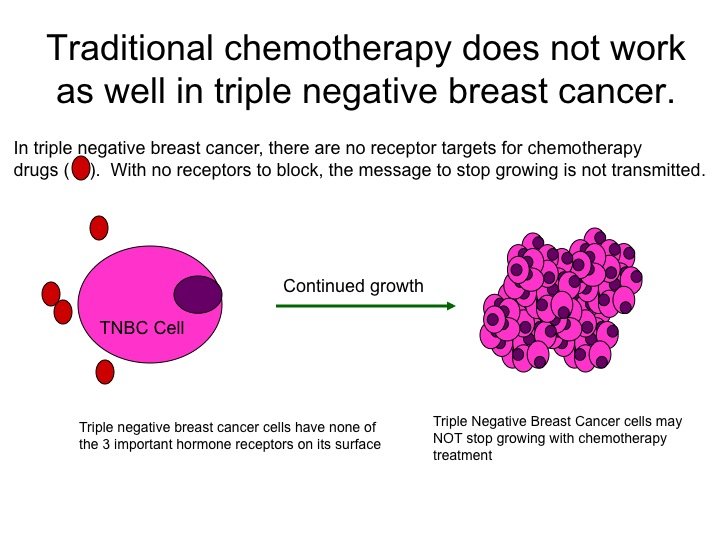
Triple negative breast cancer can be more aggressive and difficult to treat. Also, the cancer is more likely to spread and recur. The stage of breast cancer and the grade of the tumor will influence your prognosis. Research is being done currently to create drug therapies that are specific for triple negative breast cancer.
Interested in learning more? i3Health is hosting an upcoming webinar Metastatic Triple-Negative Breast Cancer: Applying Treatment Advances to Personalized Care. Learn more here.
Material on this page courtesy of Johns Hopkins Medicine
Recommended Reading: Is Breast Cancer Curable In The 3 Stage
Having Dense Breast Tissue
Breasts are made up of fatty tissue, fibrous tissue, and glandular tissue. Breasts appear denser on a mammogram when they have more glandular and fibrous tissue and less fatty tissue. Women with dense breasts on mammogram have a risk of breast cancer that is about 1 1/2 to 2 times that of women with average breast density. Unfortunately, dense breast tissue can also make it harder to see cancers on mammograms.
A number of factors can affect breast density, such as age, menopausal status, the use of certain drugs , pregnancy, and genetics.
To learn more, see our information on breast density and mammograms.
Mercks Keytruda Plus Chemotherapy Reduced Risk Of Death By 27% Versus Chemotherapy As First
First Anti-PD-1 Therapy in Combination With Chemotherapy to Demonstrate Statistically Significant Overall Survival for These Patients
Data From Phase 3 KEYNOTE-355 Trial Presented at ESMO Congress 2021
KENILWORTH, N.J.â-Merck , known as MSD outside the United States and Canada, today announced the final overall survival results from the pivotal Phase 3 KEYNOTE-355 trial investigating KEYTRUDA, Mercks anti-PD-1 therapy, in combination with chemotherapy for the first-line treatment of patients with metastatic triple-negative breast cancer . KEYTRUDA is the first anti-PD-1 therapy in combination with chemotherapy to demonstrate a statistically significant and clinically meaningful improvement in OS for these patients.
In this study, KEYTRUDA plus chemotherapy reduced the risk of death by 27% in patients with mTNBC whose tumors expressed PD-L1 , as compared to chemotherapy alone. There was an increase of 6.9 months in median OS with KEYTRUDA plus chemotherapy compared to chemotherapy alone . Although the trial was not powered to compare efficacy between treatment groups by different chemotherapy regimens, the increase in OS was observed for KEYTRUDA plus chemotherapy across the three chemotherapy choices. These data were presented today in an oral presentation at the European Society for Medical Oncology Congress 2021 .
About KEYNOTE-355
About KEYTRUDA® Injection, 100 mg
Selected KEYTRUDA® Indications in the U.S.
Melanoma
Read Also: Can Stage 3 Breast Cancer Be Cured
What Is Invasive Lobular Carcinoma
Invasive lobular carcinoma is a cancer that starts in the breasts lobules and invades surrounding tissue. ILC is the second most common form of invasive breast cancer, accounting for 10 to 15% of breast cancer cases. ILC doesnt always form a lump, but women who have it may notice a thick or full area that doesnt feel like the rest of the breast.
Risk Factors For Triple
Doctors aren’t sure what makes you more likely to get triple-negative breast cancer. Not many women do — it only affects up to 20% of those who have breast cancer. You’re most at risk for triple-negative breast cancer if you:
- Are African-American or Latina
- Are under 40
- Have what your doctor will call a BRCA mutation , especially the gene BRCA1
Also Check: Did Anne Hathaway Have Breast Cancer
When Should I Go To The Emergency Room
You might also have unusually strong side effects from your cancer treatment. While your healthcare provider likely gave you medication to help control your side effects, you should go to the emergency room if your side effects continue despite medication.
Many cancer treatments affect your immune system, increasing the chance you will develop infections. Symptoms that might require an emergency room visit during treatment are:
- Fever of 100.5 and above.
- Chills.
- Persistent nausea and vomiting.
Research Into Triple Negative Breast Cancer
Researchers are working to find new treatments for triple negative breast cancer. Much of this research involves looking for molecules in the body that are involved with cancer growth, and formulating a drug that will disable how that molecule works.
Clinical trials are in progress to determine whether these new drugs are better than the current standard treatment. If you would like more information on clinical trials, visit the clinical trials section of our website.
Recommended Reading: Why Is Left Breast Cancer More Common
Trials For Advanced Triple Negative Breast Cancer
Trials are comparing different types of chemotherapy to see which are better at treating advanced disease. For example, researchers are waiting for the results of the Triple Negative Trial to find out whether it is better to use carboplatin or docetaxel.
Research is looking at using targeted cancer drugs alongside other treatments. For example, a trial is using a drug called atezolizumab in combination with chemotherapy. Some trials are testing a drug called pembrolizumab. Researchers think that these targeted drugs on their own might help to control the growth of the cancer.
-
National Institute for Health and Care Excellence , July 2018
-
Biology and management of patients with triple negative breast cancerP SharmaThe Oncologist. 2016, Volume 21, Issue 9
-
4th ESOESMO International Consensus Guidelines for Advanced Breast CancerF Cardoso and othersAnnals of Oncology,2018, Volume 29, pages 16341657
-
Early breast cancer: ESMO Clinical Practice Guidelines for diagnosis, treatment and follow-upF Cardoso and others
What Is Metaplastic Carcinoma
Also known as metaplastic breast cancer, metaplastic carcinoma is a rare type of invasive breast cancer with a unique characteristic: It contains a mix of two or more types of breast cancer cells, usually carcinoma combined with sarcoma. Metaplastic means that one form is turning into another. Various leading-edge techniques are used to analyze the exact genetics and biology of these confused cancers to find out if the tumor is more similar to carcinoma or sarcoma, since these two types of cancer have very different treatments.
Also Check: Baking Soda And Honey For Cancer
Cutting Both Ways: The Role Of Ar In Tnbc
AR is a transcription factor belonging to the nuclear steroid hormone receptor family. AR-mediated signaling plays a critical role in the development of breast tissue . There is also accumulating evidence supporting the role of AR in BC development and progression . Nonetheless, the role of AR signaling in TNBC remains unclear. In TNBC, AR is reported to interact with androgen response elements and stimulate tumor cell growth in an androgen-dependent manner. In TNBC patients, clinical trial focused on testing the anti-androgen therapies in combination with chemotherapy in TNBC patients have yielded positive results . Currently, the efficacy of various drug combinations such as pembrolizumab and enobosarm, palbociclib and avelumab, and taselisib and enzalutamide is being evaluated in patients with metastatic TNBC . In addition, the ongoing MDACC ARTEMIS trial is a neoadjuvant study that is focused on women with stage IIII TNBC and modifies therapy based on molecular profiling. For example, if AR is expressed, then enzalutamide along with paclitaxel is administered .
Table 1 QNBC biomarkers and therapeutic targets, based upon differences in tumor biology between AR-negative and AR-positive TNBCs, and suggested therapeutic interventionsFig. 1