Overcoming Therapeutic Resistance Of Triple Positive Breast Cancer With Cdk4/6 Inhibition
Elena Shagisultanova
1Young Womens Breast Cancer Translational Program, University of Colorado Denver, 13001 E 17th Pl, Aurora, CO 80045, USA
Academic Editor:
Abstract
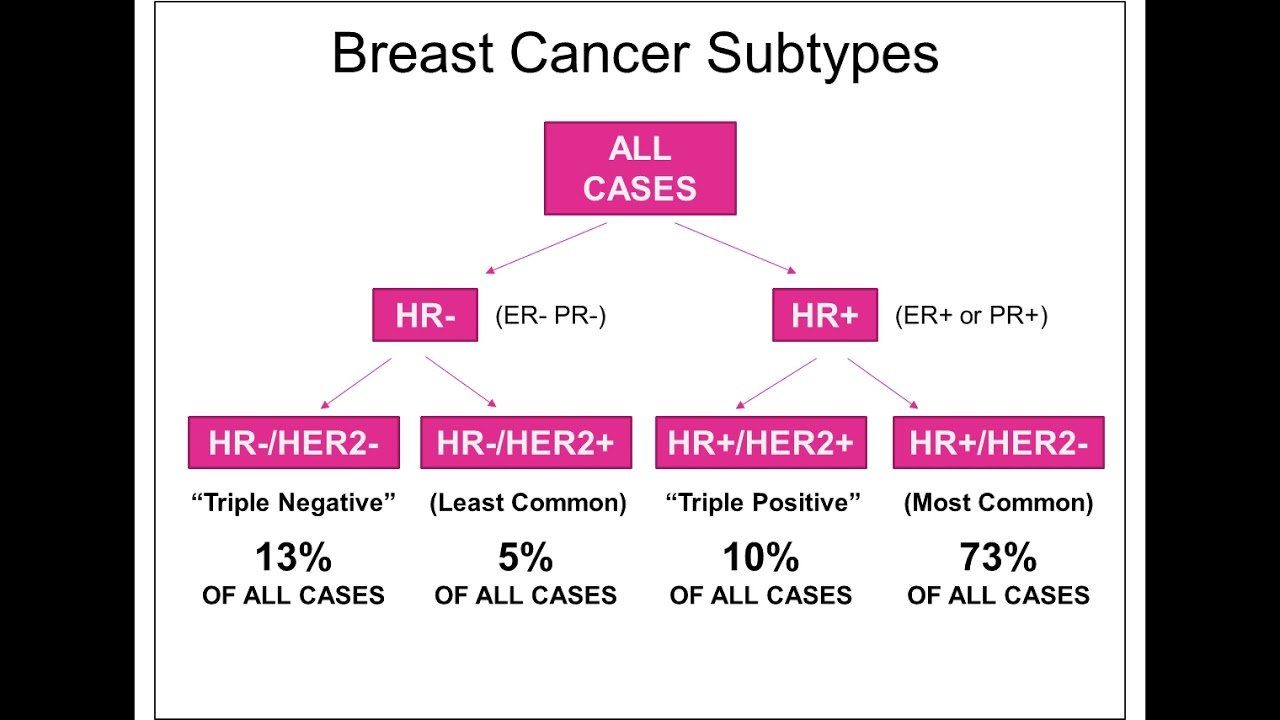
Triple positive breast cancers overexpress both the human epidermal growth factor receptor 2 oncogene and the hormonal receptors to estrogen and progesterone. These cancers represent a unique therapeutic challenge because of a bidirectional cross-talk between the estrogen receptor alpha and HER2 pathways leading to tumor progression and resistance to targeted therapy. Attempts to combine standard of care HER2-targeted drugs with antihormonal agents for the treatment of HR+/HER2+ breast cancer yielded encouraging results in preclinical experiments but did improve overall survival in clinical trial. In this review, we dissect multiple mechanisms of therapeutic resistance typical of HR+/HER2+ breast cancer, summarize prior clinical trials of targeted agents, and describe novel rational drug combinations that include antihormonal agents, HER2-targeted drugs, and CDK4/6 inhibitors for treatment of the HR+/HER2+ breast cancer subtype.
1. Triple Positive Breast Cancer Displays Increased Resistance to Targeted Therapy
| Clinical trial |
a b
Below we summarize current approaches to targeted therapy in HR+/HER2+ breast cancer, highlight drug resistance mechanisms, and focus on CDK4/6 inhibitors as promising agents that may counteract therapeutic resistance in patients with HR+/HER2+ breast cancer.
aba
References
Triple Positive Breast Cancer
Triple positive breast cancer
KR-Markham
Whitelilies
Could you, possibly, change it to 3? I believe 3 is the minimum to tag.
Perhaps do KR1.
I will send you a message still.
Whitelilies
Whitelilies
@KR Hello and welcome! I am sorry to hear of the diagnosis, of your wife.it is so very recent..glad you have reached out to us we are here to share and listen and support one another support for youand your wife. It is shocking to hear that word. .
Please meet, as you shared you wished to connect with others,
Thank you so much, if you could, share your experiences, here, to support our new member, as his wife, recently was diagnosed.similar path, as yourselves..he is wishing to connect..much appreciation.
Welcome again
Dakley
Thanks for tagging me.
I was diagnosed with stage 1 triple positive Dec 24th 2014, I was 50. Tumour under 2cm, lymph nodes clear . I did a lumpectomy . Because of my surgical choice I had to do radiation which I did after the 6 months of crappy chemo.
Because it is triple positive it is considered aggressive and fast growing therefore chemo even though I was only stage one and theoretically considered cancer free after surgery.
It is a crappy diagnosis. Long haul with treatment. But manageable and survivable.
Hang in there. Happy to support both you and wife via the many threads or private message.
Buffythevampire
With So Much At Stake Carol Seeks A Second Opinion
Dr. Dormady designed a personalized plan of treatment for her, but before beginning Carol sought a second opinion outside the El Camino Health network. She needed more assurance that she wasn’t going to be overtreated and left infertile. The second opinion concurred with Dr. Dormady’s recommended treatment plan.
“I had spoken with a couple other oncologists even before meeting Dr. Dormady,” shares Carol. “But I was really drawn to the level of care at El Camino Health. They deal with cancer every day, but instead of being jaded or callous, they are sincerely caring and personal.”
Also Check: How To Lower Your Risk Of Breast Cancer
Neoadjuvant And Adjuvant Systemic Therapy
For women who have a hormone receptor-positive breast cancer, most doctors will recommend hormone therapy as an adjuvant treatment, no matter how small the tumor is. Women with tumors larger than 0.5 cm across may be more likely to benefit from it. Hormone therapy is typically given for at least 5 years.
If the tumor is larger than 1 cm across, chemo after surgery is sometimes recommended. A woman’s age when she is diagnosed may help in deciding if chemo should be offered or not. Some doctors may suggest chemo for smaller tumors as well, especially if they have any unfavorable features .
After surgery, some women with HER2-positive cancers will be treated with trastuzumab for up to 1 year.
Many women with HER2-positive cancers will be treated with trastuzumab followed by surgery and more trastuzumab for up to 1 year. If after neoadjuvant therapy, residual cancer is found during surgery, trastuzumab may be changed to a different drug, called ado-trastuzumab emtansine, which is given every 3 weeks for 14 doses. If hormone receptor-positive cancer is found in the lymph nodes, your doctor might recommend one year of trastuzumab followed by additional treatment with an oral drug called neratinib for 1 year.
Facing Triple Positive Breast Cancer
My life changed forever once I received the phone call no one wants to get early one morning in March 2015. My surgeon was on the other line with the results from my recent biopsy. The lump that was supposed to be only a pesky cyst was indeed cancerous. The surgeon further explained my diagnosis. But the only thing I heard was that I had cancer. My world felt like it was spinning out of control.
How could this have happened to me? I was only 37 years old with a loving husband and three small daughters. I lived a relatively healthy lifestyle. Life was just starting for us. Unfortunately, I had to temporarily leave behind my teaching career, because life was being filled with MRIs, CT scans, bone scans, second-look biopsies, and appointments at the Saskatoon Cancer Centre and Breast Health Centre.
When I was diagnosed, I had no idea that there were different subtypes of breast cancer.
My type was triple positive, which meant that it was estrogen receptor positive, progesterone receptor positive, and HER2-positive.
HER2, which stands for human epidermal growth factor receptor 2, means that the cancer cells produce more of a certain protein. This type of breast cancer tends to grow and spread faster than others. It is particularly aggressive and requires additional treatment.
This regimen was a lot to chew for my husband and me, but we were willing to do what we needed so that I could watch my children achieve their milestones and grow old with my husband.
Don’t Miss: Can You Get Breast Cancer From Breast Implants
Rationale For Neoadjuvant Endocrine Therapy For Er
The PEPI score was also tested in the ACOSOG Z1031 trial to determine whether it could be used to assist decisions for neoadjuvant endocrine therapy vs. chemotherapy and identify patients with low risk of recurrence. The Z1031 trial tested 16 to 18 weeks of aromatase inhibitor in postmenopausal stage II or III ER-positive patients. Patients with a Ki67 of > 10% at 4 weeks of AI were declared endocrine therapy resistant and went on to neoadjuvant chemotherapy. Patients with a PEPI score of 0 exhibited a 5-year risk of relapse of 3.6% without chemotherapy, and confirmation is being sought in the ALTERNATE trial .
Prospective validation of the PEPI 0 and mPEPI 0 biomarker as a surrogate for 5-year RFS in the ALTERNATE trial would allow comparison of different NET strategies and agents and identify patients who do not need chemotherapy- a de-escalation strategy. Thus, neoadjuvant hormonal therapy is also a pathway to de-escalation because although higher-risk patients in the ALTERNATE trial were offered postoperative chemotherapy, many of these patients who received neoadjuvant hormonal therapy were able to avoid postoperative adjuvant chemotherapy. Therefore, in the ALTERNATE trial, postoperative chemotherapy served as a backstop for those patients who were candidates for it, whereas lower-risk patients avoided it.
Breast Cancer Cell Lines
Part of the current knowledge on breast carcinomas is based on in vivo and in vitro studies performed with cell lines derived from breast cancers. These provide an unlimited source of homogenous self-replicating material, free of contaminating stromal cells, and often easily cultured in simple standard media. The first breast cancer cell line described, BT-20, was established in 1958. Since then, and despite sustained work in this area, the number of permanent lines obtained has been strikingly low . Indeed, attempts to culture breast cancer cell lines from primary tumors have been largely unsuccessful. This poor efficiency was often due to technical difficulties associated with the extraction of viable tumor cells from their surrounding stroma. Most of the available breast cancer cell lines issued from metastatic tumors, mainly from pleural effusions. Effusions provided generally large numbers of dissociated, viable tumor cells with little or no contamination by fibroblasts and other tumor stroma cells.Many of the currently used BCC lines were established in the late 1970s. A very few of them, namely MCF-7, T-47D, MDA-MB-231 and SK-BR-3, account for more than two-thirds of all abstracts reporting studies on mentioned breast cancer cell lines, as concluded from a Medline-based survey.
Metabolic markers
Read Also: Does Having Breast Cancer Hurt
Types Of Breast Cancer
There are different types of breast cancer. Knowing the type of breast cancer you have helps your doctors decide on the best treatment for you.
On this page
There are different types of breast cancer. Knowing the type of breast cancer you have helps your doctor to plan the best treatment for you.
Breast cancer can be non-invasive or invasive.
Non-invasive breast cancer stays within the ducts or lobules and is called ductal carcinoma in situ .
Invasive breast cancer is when the cancer cells spread outside the milk ducts or lobules where they first started. Most breast cancers are invasive and can be grouped as:
- no special type
Other less common types of invasive breast cancer include:
- invasive lobular breast cancer
- inflammatory breast cancer
- Pagets disease of the breast.
Some breast cancers are also identified by whether or not the cancer cells have receptors for hormones or a protein called HER2 .
Breast cancer that does not have receptors for HER2 or hormones is called triple negative breast cancer.
This is the earliest form of breast cancer. In DCIS there are cancer cells in the ducts of the breast but these cells are contained . They have not spread into normal breast tissue.
DCIS may show up on a mammogram and is commonly diagnosed when women have breast screening.
Invasive breast cancer means the cancer cells have spread outside the lining of the ducts or lobes and into the surrounding breast tissue. There are different types of invasive breast cancer.
How Often Does Stage 1 Breast Cancer Come Back After Treatment
If stage 1 cancer is treated comprehensively, it rarely comes back. A new, unrelated breast cancer is more likely to emerge after stage 1 breast cancer is treated than a recurrence. Your healthcare provider will recommend a surveillance schedule for you so that new breast cancer or a recurrence can be identified and treated as quickly as possible.
Don’t Miss: How Serious Is Breast Cancer
Tumour Reviewtriple Positive Breast Cancer: A Distinct Subtype
HER-2, ER and PgR have a key role in treatment decision making in breast cancer.
-
Triple positive tumours exhibit a unique clinical and biological behavior.
-
TP breast cancer behavior might be also driven by HR status.
-
TP tumors with low disease burden and high HR expression resemble luminal tumours.
-
The identification and characterization of this subset may avoid overtreatment.
How Are Breast Tumors Tested For Her2
Women newly diagnosed with invasive breast cancers should be tested for HER2.
A biopsy or surgery sample of the cancer is usually tested with either immunohistochemical stains or Fluorescent in situ hybridization .
See Testing Biopsy and Cytology Specimens for Cancer and Understanding Your Pathology Report: Breast Cancerto get more details about these tests.
Also Check: Is Bilateral Breast Cancer Metastatic
What Type Of Drug Treatment Might I Get
Most women with breast cancer in stages I to III will get some kind of drug therapy as part of their treatment. This may include:
- Chemotherapy
- Hormone therapy
- HER2 targeted drugs, such as trastuzumab and pertuzumab
- Some combination of these
The types of drugs that might work best depend on the tumors hormone receptor status, HER2 status, and other factors.
Faith In The El Camino Health Cancer Care Team

Through it all, Carol drew strength from knowing she had an entire team in her corner fighting her cancer. In fact, she says she can’t begin to describe how much she has grown to love everyone at the El Camino Health Cancer Center.
“The whole team is amazing,” she says. “Dr. Dormady and nurse practitioner Katie are the best! They put up with my questions and quirks with the best humor and love. They understood my desire to be treated but not overtreated.”
“The nurses are like family. I have to give a shoutout to my nurse Hannah. We shared our lives together every week for a whole year. That was the biggest blessing ever. I still drop by with treats when Im in the area as an excuse to say hi.”
You May Like: What Does Stage 3 Breast Cancer Look Like
Where Do These Numbers Come From
The American Cancer Society relies on information from the SEER* database, maintained by the National Cancer Institute , to provide survival statistics for different types of cancer.
The SEER database tracks 5-year relative survival rates for breast cancer in the United States, based on how far the cancer has spread. The SEER database, however, does not group cancers by AJCC TNM stages . Instead, it groups cancers into localized, regional, and distant stages:
- Localized: There is no sign that the cancer has spread outside of the breast.
- Regional: The cancer has spread outside the breast to nearby structures or lymph nodes.
- Distant: The cancer has spread to distant parts of the body such as the lungs, liver or bones.
Purpose Of This Review
The purpose of this review is to critically evaluate the results of trials of neoadjuvant chemotherapy and neoadjuvant endocrine therapy for different breast cancer subtypes, discuss how neoadjuvant responses can inform adjuvant therapy, and highlight the importance of pathological complete response as a surrogate marker of distant disease-free survival , distant recurrence free survival , and event free survival which is interchangeable with disease-free survival , in the age of adaptive trial design. Notably, in contrast to overall survival , precise definitions of DFS and similar, related endpoints vary somewhat from trial to trial. pCR is generally a composite endpoint of primary tumor and lymph nodes. While pCR correlates with lower risk of recurrence, risk of recurrence still occurs and reduction of this risk remains an important goal. We also highlight functional and genomic predictive biomarkers in NET and their prediction of recurrence free survival , essentially equivalent to EFS.
Recommended Reading: Which Breast Implants Cause Cancer
Highlights And Future Directions
Another direction for progress will come from ongoing development of more effective strategies for de-escalation of therapy, particularly through measurement of pCR and MRI biomarkers in NAC. For example, improvements in HER2-targeted therapy may result in improved responses, measured by reduction of functional tumor volume and biopsy, such that anthracyclines may be deleted from neoadjuvant platform trial regimens that currently contain anthracyclines. Further progress will likely come from the use of functional biomarkers such as the mPEPI and PEPI score, and genomic assays, in NET. The process of answering these questions, through well designed trials will continue to add to the growing body of information on neoadjuvant strategies in breast cancer, where quantitatively measuring the effects of targeted drug therapy has added so much to what we can offer our patients.
Relative Survival Rates For Breast Cancer
The National Cancer Institute gives 5-year relative survival rates for breast cancer based on how far the disease had spread before a doctor found it.
- Localized : 99%
- Regional : 86%
- Distant : 28%
- Unknown stage: 55%
- All stages: 90%
While these numbers can give you a general idea, they are an average for women with any type of breast cancer. They arent specific to the HER2+ type. They also come from data that researchers collected from 2010 to 2016, so they dont reflect more recent treatment advances.
Read Also: Where Can Breast Cancer Lumps Be
More Information About The Tnm Staging System
The T category describes the original tumor:
- TX means the tumor can’t be assessed.
- T0 means there isn’t any evidence of the primary tumor.
- Tis means the cancer is “in situ” .
- T1, T2, T3, T4: These numbers are based on the size of the tumor and the extent to which it has grown into neighboring breast tissue. The higher the T number, the larger the tumor and/or the more it may have grown into the breast tissue.
The N category describes whether or not the cancer has reached nearby lymph nodes:
- NX means the nearby lymph nodes can’t be assessed, for example, if they were previously removed.
- N0 means nearby lymph nodes do not contain cancer.
- N1, N2, N3: These numbers are based on the number of lymph nodes involved and how much cancer is found in them. The higher the N number, the greater the extent of the lymph node involvement.
The M category tells whether or not there is evidence that the cancer has traveled to other parts of the body:
- MX means metastasis can’t be assessed.
- M0 means there is no distant metastasis.
- M1 means that distant metastasis is present.
Availability Of Data And Materials
The dataset analysed in the current study is not publicly available, but was obtained from the Cancer Registry of Norway under a specific ethical approval by the Regional Committee for Medical and Health Research Ethics in the South East Health Region of Norway. Researchers with appropriate approvals can apply for Norwegian health registry data from .
Also Check: How Did I Get Breast Cancer