How Does Breast Cancer Start
All cancers start the same way, when cells grow faster than they should. Normally, your cells divide and make new cells to replace old cells that die off.
But cancer cells have changes in their DNA that let off uncontrolled cell growth. You may have inherited these faulty genes from your parents. Or you could have been exposed to things in the environment that damaged the DNA.
In breast cancer, the abnormal cells grow in the small tubes that carry milk to the nipples or in the glands that make milk inside your breasts. These growths are called tumors.
Stelara And Other Medications Or Therapies
Below are lists of medications and therapies that can interact with Stelara. These lists do not contain all the drugs that may interact with Stelara.
Before taking Stelara, talk with your doctor and pharmacist. Tell them about all prescription, over-the-counter, and other drugs you take. Also tell them about any vitamins, herbs, and supplements you use. Sharing this information can help you avoid potential interactions.
If you have questions about drug interactions that may affect you, ask your doctor or pharmacist.
Stelara and vaccines
You shouldnt get a live vaccine when youre using Stelara. Getting a live vaccine during Stelara treatment increases your risk of getting the condition the vaccine is meant to prevent.
This is because Stelara suppresses your immune systems ability to fight infections. Receiving a live vaccine during Stelara treatment increases your risk of serious infections.
Examples of live vaccines that you should avoid during Stelara treatment include:
You should also avoid getting the Bacillus Calmette-Guérin vaccine for 1 year before you start using Stelara, during your Stelara treatment, and for 1 year after you stop using Stelara. The BCG vaccine is meant to prevent tuberculosis . Its more commonly given to people who live outside of the United States.
Stelara and allergy shots
Stelara and warfarin
If youre taking these drugs together, your doctor may need to adjust your dosage of either Stelara or warfarin.
- everolimus
- sirolimus
Cancer And Treatments May Weaken Immunity
Cancer can weaken the immune system by spreading into the bone marrow. The bone marrow makes blood cells that help to fight infection. This happens most often in leukaemia or lymphoma, but it can happen with other cancers too. The cancer can stop the bone marrow from making so many blood cells.
Certain cancer treatments can temporarily weaken the immune system. This is because they can cause a drop in the number of white blood cells made in the bone marrow. Cancer treatments that are more likely to weaken the immune system are:
- chemotherapy
You can find information about the different types of cancer treatments.
Recommended Reading: How To Cure Breast Cancer
Drug Forms And Strengths
Stelara comes as a liquid solution that contains the active drug ustekinumab.
Its available as:
- a single-dose, prefilled syringe that holds 0.5 mL of solution and contains 45 mg of ustekinumab
- a single-dose, prefilled syringe that holds 1 mL of solution and contains 90 mg of ustekinumab
- a single-dose vial that holds 0.5 mL of solution and contains 45 mg of ustekinumab
Stelara is given as a subcutaneous injection. It can be given in your upper arms, thighs, belly, or buttocks.
Your healthcare professional may give you Stelara injections at a medical clinic. They may also show you how to self-inject Stelara at home.
Note: Stelara also comes in a vial that contains 130 mg of ustekinumab. This vial is used for a one-time intravenous infusion of Stelara. Its used to give the first dose of the drug to people with Crohns disease or ulcerative colitis. This one-time infusion is called a loading dose or an induction dose. This IV infusion will take place over at least 1 hour. Each dose of Stelara after the IV infusion is given as a subcutaneous injection.
In Built Immune Protection

This is also called innate immunity. These mechanisms are always ready and prepared to defend the body from infection. They can act immediately . This in built protection comes from:
- a barrier formed by the skin around the body
- the inner linings of the gut and lungs, which produce mucus and trap invading bacteria
- hairs that move the mucus and trapped bacteria out of the lungs
- stomach acid, which kills bacteria
- helpful bacteria growing in the bowel, which prevent other bacteria from taking over
- urine flow, which flushes bacteria out of the bladder and urethra
- white blood cells called neutrophils, which can find and kill bacteria
Different things can overcome and damage these natural protection mechanisms. For example:
- something may break the skin barrier, such as having a drip in your arm or a wound from surgery
- a catheter into your bladder can become a route for bacteria to get inside the bladder and cause infection
- anti acid medicines for heartburn may neutralise the stomach acid that kills bacteria
Certain cancer treatments can also overcome these protection mechanisms. Chemotherapy can temporarily reduce the number of neutrophils in the body, making it harder for you to fight infections. Radiotherapy to the lung can damage the hairs and mucus producing cells that help to remove bacteria.
Also Check: Cancer In Both Breasts Survival Rate
How Do Breast Cancer Treatments Help
Doctors can pick from several treatment options. Your therapy will depend on your type of breast cancer and how far it has spread. You may get more than one treatment.
Surgery removes as much of the cancer as possible. If the cancer is small, your doctor might take out just the part of the breast where the cancer is . For a larger cancer, the surgeon might remove the whole breast or both breasts . The surgeon can also take out nearby lymph nodes.
Chemotherapy uses strong medicine that travels through your bloodstream to kill cancer cells or to stop them from dividing. You can have this treatment after surgery to get rid of any remaining cancer cells, or if your cancer has spread.
Radiation zaps cancer cells with high-energy rays. You get it after surgery to kill any leftover cancer, or to treat cancer that has spread to areas like your bones or brain.
Hormone therapy treats breast cancers that respond to estrogen and/or progesterone. It lowers the amount of estrogen in your body or blocks the effects of estrogen so that it can’t help your cancer grow.
Targeted therapy works against breast cancers that use proteins such as HER2 to help them grow.
Immunotherapyboosts your immune system to help it find and destroy breast cancer cells. Some of these treatments take the brakes off your immune cells so they can attack the cancer.
Immune System Takes Long Time To Recover After Breast Cancer Chemo
New research that looks at the long-term effects of chemotherapy on breast cancer survivors finds it weakens parts of the immune system for at least 9 months after treatment. This could leave patients with insufficient resilience to common infections, such as pneumonia and tetanus, even if they were immunized previously, say the researchers.
The study published in the journal Breast Cancer Research comes from the University of Leeds and Leeds Teaching Hospitals NHS Trust in the UK.
One of the senior authors, Thomas Hughes, an associate professor in the Faculty of Medicine at Leeds, says:
We were surprised that the impact of chemotherapy is so long lived.
He and his colleagues suggest the findings indicate breast cancer survivors who have undergone chemotherapy would likely benefit from post-treatment monitoring.
Breast cancer is the most common cancer in women and claims over half a million lives worldwide every year, note the authors.
Typical treatment for primary tumors involves surgery to remove the tumor, combined with other therapies, such as hormone therapy, radiotherapy and/or chemotherapy to kill any remaining cancer cells. Around 30% of breast cancer patients receive chemotherapy.
Chemotherapy drugs work by attacking cells that divide quickly, which is what cancer cells do. But other cells such as those in the bone marrow where white blood cells are made also divide quickly and are likely to be affected by chemotherapy.
Don’t Miss: Estrogen Positive Progesterone Negative Breast Cancer
Other Chemos Other Cancers
Researchers found that the type of chemo used did seem to make a difference in the recovery of patientsâ immune systems.
For instance, lymphocyte levels in patients treated with certain anthracycline-based regimens followed by the taxane docetaxel âremained significantly depressed,â measuring at 64 percent of pre-chemo levels.
Dr. Julie Gralow â a breast cancer oncologist at SCCA, Fred Hutch’s treatment arm â said she thought patients would be very interested in the study, but she felt the âclinical implications of the finding remain to be seen,â noting that the study looked at chemo agents that may not be commonly used in the U.S.
At the SCCA, for example, âWe donât use epirubicin as the anthracycline, we use doxorubicin,â she said. âAnd when we give anthracyclines, we generally favor taxol over taxotere as the taxane. So we donât give the same chemo.â
She also suggested that while the study showed the immune system was impacted by chemo, the study didnât prove that patients were more at risk for infection.
âMost of the effect has recovered within nine months, if you donât smoke,â she said. â it seems that smoking has a big effect, and we always encourage patients to stop smoking.â
While the researchers did not investigate this effect in other cancers, they said patients treated with the same chemotherapy agents would most likely experience the same thing.
Understanding Your Cancer And Treatment
Not all breast cancers are alike. Someone elses experience with their treatment may be completely different from yours. Understanding your type and stage can help make sense of your doctors recommendations. This may help you feel better about your treatment choices.
A big part of cancer treatment is the relationship between you and your oncology team. Here are some things youll want to know about early on so youre well informed about your specific type of breast cancer:
Oncologists meet with cancer patients every day and its their job to see you as a whole person. Express your wants and needs. Rest assured that no question is too insignificant to ask.
Read Also: Breast Cancer Stage 3 Symptoms
Does My Cancer Treatment Weaken My Immune System
Chemotherapy affects the whole body, including the immune system. These medications that kill cancer cells also lower your number of white blood cells, which fight infection. There are times in your treatment cycle when your white blood cell counts are lowest this is when youâre at highest risk for infection. Your blood counts are checked often during treatment. So your treatment team can tell you when youâre at greatest risk. Still, do what you can to help prevent infection all the time.
Other types of cancer treatment — such as radiation, immunotherapy, targeted therapy, and surgery — can affect your immune system, too. Talk to your cancer care team about your treatment plan, how it impacts your risk for infection, and what you need to do during the coronavirus pandemic.
Immunologic Consequences Of Conventional Breast Cancer Treatment
Immunologic Effects of Chemotherapy and Radiotherapy
Cyclophosphamide-methotrexate-5-fluorouracil chemotherapy regimens have been shown to significantly decrease both spontaneous and IFN-stimulated NK cell activities. NK cell activity against the K562 cell line in patients who had received adjuvant chemotherapy combined with radiotherapy was significantly lower than that of patients after radiotherapy alone or that of healthy controls.96 Tsavaris and colleagues studied the immunologic effects of taxane-based chemotherapy on 30 women with advanced breast cancer.6 Sera were collected before the start of chemotherapy and after the last treatment cycle and were compared with those from healthy controls. Compared with healthy controls, these breast cancer patients had depressed. NK cell LAK cytotoxicity and depressed GM-CSF, IL-2, IL-6, and TNF-. Both paditaxel and docetaxel increased NK and LAK cell activity and increased IL-6, GM-CSF, and IFN- levels while decreasing IL-1 and TNF- levels. A better clinical response in these metastatic breast cancer patients was associated with greater increases in serum IFN-, IL-2, IL-6, and GM-CSF cytokine levels and enhancement of peripheral blood mononuclear cell NK and LAK cell activity.
Immunologic Disorders Associated with Breast Cancer Treatment
Also Check: Stage-three Cancer
Financial And Insurance Assistance
If you need financial support to pay for Stelara, or if you need help understanding your insurance coverage, help is available.
Janssen Biotech, Inc., the manufacturer of Stelara, offers a program called Janssen CarePath. For more information and to find out if youre eligible for support, call 877-CAREPATH or visit the program website.
Your doctor will recommend if you need to take other drugs with Stelara to treat your condition.
What The Immune System Does
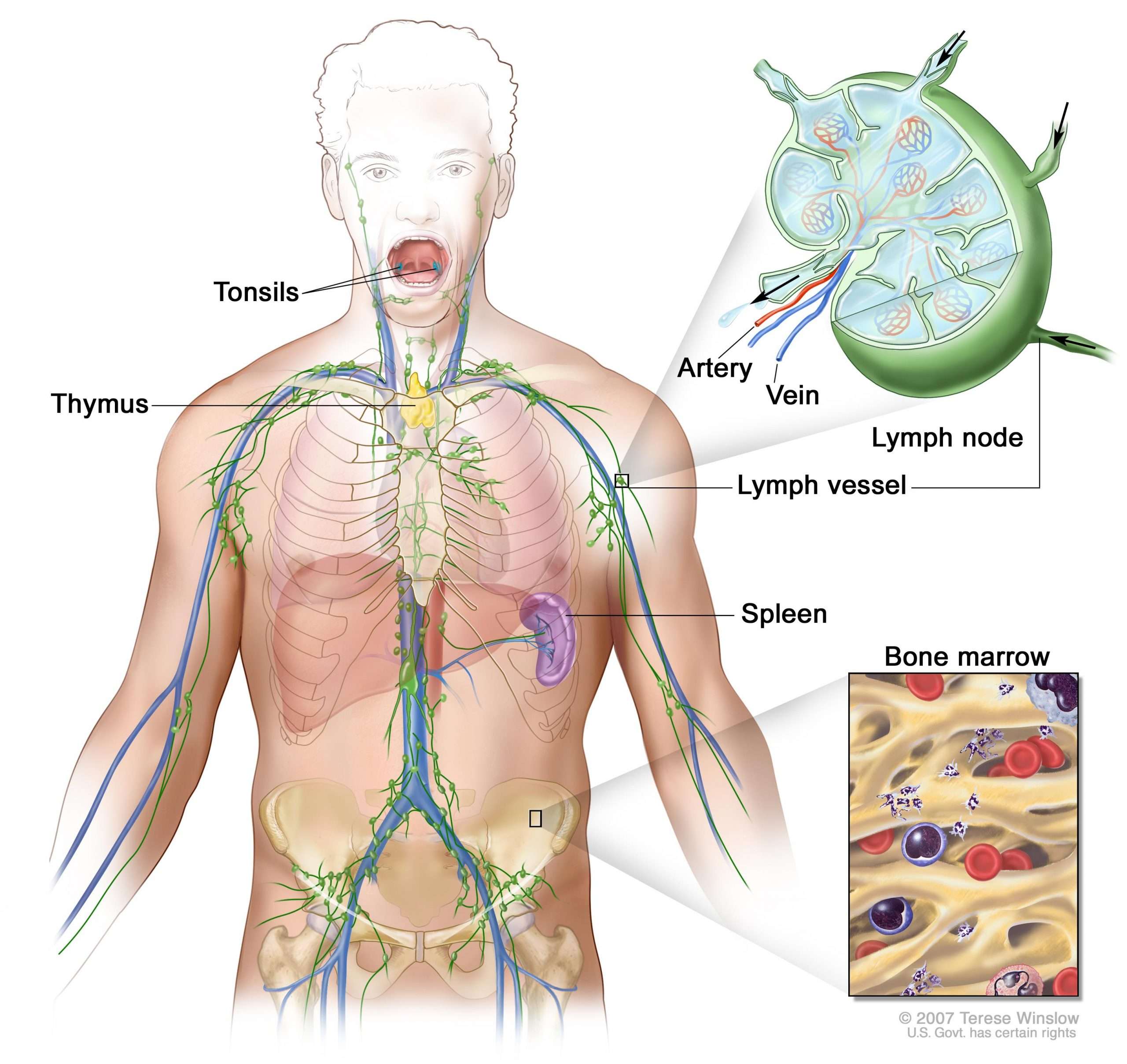
The immune system protects the body against illness and infection that bacteria, viruses, fungi or parasites can cause. It is a collection of reactions and responses that the body makes to damaged cells or infection. So it is sometimes called the immune response.
The immune system is important to people with cancer because:
- cancer can weaken the immune system
- cancer treatments might weaken the immune system
- the immune system may help to fight cancer
Don’t Miss: Baking Soda And Breast Cancer
Exposure To Certain Chemicals
Being exposed to large amounts of arsenic increases the risk of developing skin cancer. Arsenic is an element found naturally in well water in some areas. Its also used in making some pesticides and in some other industries.
Workers exposed to coal tar, paraffin, and certain types of petroleum products may also have an increased risk of skin cancer.
The Immune System Can Help To Fight Cancer
Some cells of the immune system can recognise cancer cells as abnormal and kill them. But this may not be enough to get rid of a cancer altogether.
Some treatments aim to use the immune system to fight cancer.
There are 2 main parts of the immune system:
- the protection we have from birth
- the protection we develop after having certain diseases
Don’t Miss: Stage 4 Breast Cancer Cure
Alternatives For Plaque Psoriasis
Examples of other drugs that may be used to treat plaque psoriasis include:
- topical therapies, such as oils containing vitamin D
- methotrexate
- acitretin
- moderate to severe Crohns disease in adults
- moderate to severe ulcerative colitis in adults
Stelara is also approved to treat moderate to severe plaque psoriasis in children ages 6 years and older.
Humira is also approved to treat Crohns disease in children ages 6 years and older. And its approved to treat ulcerative colitis in children ages 5 years and older.
Additionally, Humira is also approved to treat:
- moderate to severe rheumatoid arthritis in adults
- uveitis in adults and children ages 2 years and older
- juvenile idiopathic arthritis in children ages 2 years and older
- hidradenitis suppurativa in adults and children ages 12 years and older
If I Take Stelara For A Long Time Will I Have Withdrawal Symptoms When I Stop Using It
Its possible that your condition may return or worsen if you stop taking Stelara. This can lead to symptoms that may be confused with withdrawal symptoms.
Dont stop taking Stelara unless your doctor recommends that you stop treatment. Once you stop taking Stelara, your doctor will monitor you closely to determine if you can safely remain off the medication.
Recommended Reading: Can Stage 3 Breast Cancer Be Cured
Hair And Skin Changes
Chemotherapy, or âchemo,â can make your hair fall out, not only on your head but also all over your body. Chemo also can turn your skin dry, itchy, and flaky. Radiation might cause your skin to look and feel like sunburn around the treatment spot.
These effects may change how you feel about yourself. Some people might react visibly. Consider telling your loved ones and others beforehand about what youâre going through. Sometimes it may help to talk to a mental health counselor.
The good news is that after treatment, your skin returns to normal and your hair usually grows back. Itâs possible that your hair could grow back with a slightly different feel and texture.
How Breast Cancer Treatments Can Affect The Immune System
While breast cancer treatments can be very effective, one of the unwanted side effects, primarily of chemotherapy, is harm to a womans immune system.
Treatment for breast cancer is highly effective. Five-year survival rates for breast cancer have increased dramatically in recent decades, and much of that success can be credited to cancer researchers and campaigns designed to inform women about the importance of screenings.
Breast cancer is highly treatable, but treatment typically leads to some unwanted side effects. According to Johns Hopkins Medicine, women undergoing treatment for breast cancer may experience a host of side effects, including fatigue, pain, headaches, and dental issues. Cancer treatments, most notably chemotherapy, also can take a toll on womens immune systems.
Why does chemotherapy affect the immune system?
Cancer is caused by an uncontrolled division of abnormal cells in the body. According to Breastcancer.org, chemotherapy targets these abnormal cells, but also can affect fast-growing cells that are healthy and normal. So chemotherapy can damage cells throughout the body, including those in bone marrow. When bone marrow is damaged, its less capable of producing sufficient red blood cells, white blood cells and platelets. Breastcancer.org notes that the body is more vulnerable to infection when it does not have enough white blood cells.
Does chemotherapy always weaken the immune system?
Other treatments
Don’t Miss: Whats The Youngest You Can Get Breast Cancer
Less Common Treatment Effects
Radiation therapy. In some cases it can cause pulmonary fibrosis, which scars your lung tissue. You might notice:
- Dry cough
- Chest pain
These symptoms typically show up 2-3 months after your treatment ends. It may first look like pneumonia, but antibiotics wonât help. Your doctor may prescribe steroids to treat your symptoms.
Chemotherapy. Certain chemo drugs can lead to heart problems, especially if you had existing heart problems. Other possible side effects of chemo include:
- Hot flashes and irregular or missed periods
- Foggy thinking
- Consistent numbness, pain, or tingling in fingers or toes
- Weight gain
Hormone therapy. If you have a type of tumor called estrogen receptive, you might get hormone therapy drugs. Many of them can lead to weaker bones . One drug, tamoxifen, may raise your risk for serious medical issues like stroke, blood clots, and uterine cancer. Tamoxifen also may cause:
- Vaginal discharge
- Weight gain
- Hot flashes
Each woman responds differently to their breast cancer and treatments. Itâs a good idea to keep track of your experience and update your doctors about your side effects. The sooner theyâre aware, the better they can help you get your symptoms under control.