What Is Breast Screening
Cancer screening involves testing apparently healthy people for signs that could show that a cancer is developing.
Breast screening uses a test called mammography which involves taking x-rays of the breasts. Screening can help to find breast cancers early when they are too small to see or feel. These tiny breast cancers are usually easier to treat than larger ones.
It is important to remember that screening will not prevent you from getting breast cancer but aims to find early breast cancers.
Overall, the breast screening programme finds cancer in around 9 out of every 1,000 women having screening.
Breast Cancer Screening: Ages 50 To 74
Breast cancer causes approximately 42,000 deaths in the United States each year. The U.S. Preventive Services Task Force recommends that women between the ages of 50 to 74 undergo mammography screening once every two years. Early detection via mammography screening and subsequent treatment can reduce breast cancer mortality for women in this age range.
Explore the percentage of women ages 50 to 74 who had a mammogram to screen for breast cancer in each state. Higher rates are better on this measure.
The purple dashed line represents the median, or middle, of all values reported.
This measure reports state performance on the percentage of women ages 50 to 74 who received a mammogram to screen for breast cancer during the measurement year or two years prior to the measurement year.
States voluntarily report on Breast Cancer Screening as part of the Core Set of Adult Health Care Quality Measures. These data show performance rates for states that voluntarily reported the measure using Adult Core Set measure specifications.
Source: Mathematica analysis of Medicaid and CHIP Program System reports for the Federal Fiscal Year reporting cycle as of June 18, 2021 see 2020 Child and Adult Health Care Quality Measures. For more information on the Breast Cancer Screening measure, visit Adult Health Care Quality Measures.
Notes:
Unless otherwise specified:
Breast Cancer Screening Among Hispanic/latina Women By Group
Mammography screening among Hispanic/Latina women varies by group. For example, women of Central/South American origin have higher screening mammography rates than Mexican American women .
Compared to Hispanic women who have lived in the U.S. for a short period of time, those who have lived in the U.S. for a long period of time may be more likely to get mammograms .
Recommended Reading: Metastatic Triple Negative Breast Cancer Treatment
Black Women In The Us
Black women have had similar rates of screening mammography as white women, Hispanic women and Asian American women in recent years .
Overall, the breast cancer incidence rate is lower among Black women than among white women .
However, the breast cancer mortality rate is higher in Black women .
For example, the breast cancer mortality rate from 2016-2020 was about 39 percent higher for Black women than white women .
Permission To Use This Summary
PDQ is a registered trademark. The content of PDQ documents can be used freely as text. It cannot be identified as an NCI PDQ cancer information summary unless the whole summary is shown and it is updated regularly. However, a user would be allowed to write a sentence such as NCIs PDQ cancer information summary about breast cancer prevention states the risks in the following way: .
The best way to cite this PDQ summary is:
PDQ® Screening and Prevention Editorial Board. PDQ Breast Cancer Screening. Bethesda, MD: National Cancer Institute. Updated < MM/DD/YYYY> . Available at: . Accessed < MM/DD/YYYY> .
Images in this summary are used with permission of the author, artist, and/or publisher for use in the PDQ summaries only. If you want to use an image from a PDQ summary and you are not using the whole summary, you must get permission from the owner. It cannot be given by the National Cancer Institute. Information about using the images in this summary, along with many other images related to cancer can be found in Visuals Online. Visuals Online is a collection of more than 3,000 scientific images.
Don’t Miss: Breast Cancer Deaths Per Year
Talk With Your Health Care Provider About Breast Cancer Screening
- If youâre at higher risk of breast cancer, talk with your health care provider about when to start breast cancer screening. You may need to be screened earlier and more often than other women. You may also benefit from other imaging, such as breast MRI.
- If youâre 40 or older , talk with your health care provider about breast cancer screening. Discuss when and how often you should get a mammogram.
Komen believes all women should have access to regular screening mammograms when they and their health care providers decide itâs best based on their risk of breast cancer.
Learn more about talking with your health care provider.
Schedule A Breast Cancer Screening Today
Adult women of all ages should receive regular breast cancer screenings. Consult with your doctor to determine the best diagnostic screenings to monitor your breast health. Health Images is here to help with advanced imaging services and a compassionate staff to guide you through the process. We offer mammograms, ultrasounds and MRIs with rapid results to give you peace of mind.
Early detection can save your life. Find a location near you to schedule a breast cancer screening today.
Also Check: What Causes Breast Cancer In Men
Clinical Breast Exam And Breast Self
Research has not shown a clear benefit of regular physical breast exams done by either a health professional or by women themselves . There is very little evidence that these tests help find breast cancer early when women also get screening mammograms. Most often when breast cancer is detected because of symptoms , a woman discovers the symptom during usual activities such as bathing or dressing. Women should be familiar with how their breasts normally look and feel and should report any changes to a health care provider right away.
While the American Cancer Society does not recommend regular clinical breast exams or breast self-exams as part of a routine breast cancer screening schedule, this does not mean that these exams should never be done. In some situations, particularly for women at higher-than-average risk, for example, health care providers may still offer clinical breast exams, along with providing counseling about risk and early detection. And some women might still be more comfortable doing regular self-exams as a way to keep track of how their breasts look and feel. But its important to understand that there is very little evidence that doing these exams routinely is helpful for women at average risk of breast cancer.
If You Have A Family History Of Breast Cancer
UK guidelines recommend that women with a moderate or high risk of breast cancer because of their family history should start having screening mammograms every year in their forties.
If you are younger than 40 and have an increased risk of breast cancer, you should be offered yearly MRI scans from the age of 30 or 40. This depends on your level of risk.
Recommended Reading: Can You Get Breast Cancer If Someone Hits You
Choosing Not To Be Screened
If you decide not to take the test, you should let the screening centre know in plenty of time.
You’ll be invited for screening again in 3 years. If you don’t want to be invited again, ask the screening centre for a disclaimer form so that your name can be removed from the system.
If you’ve completed a disclaimer or decided not to be screened at this time, but change your mind later, you can arrange an appointment by contacting your local screening centre.
Screening Information For Breast Cancer
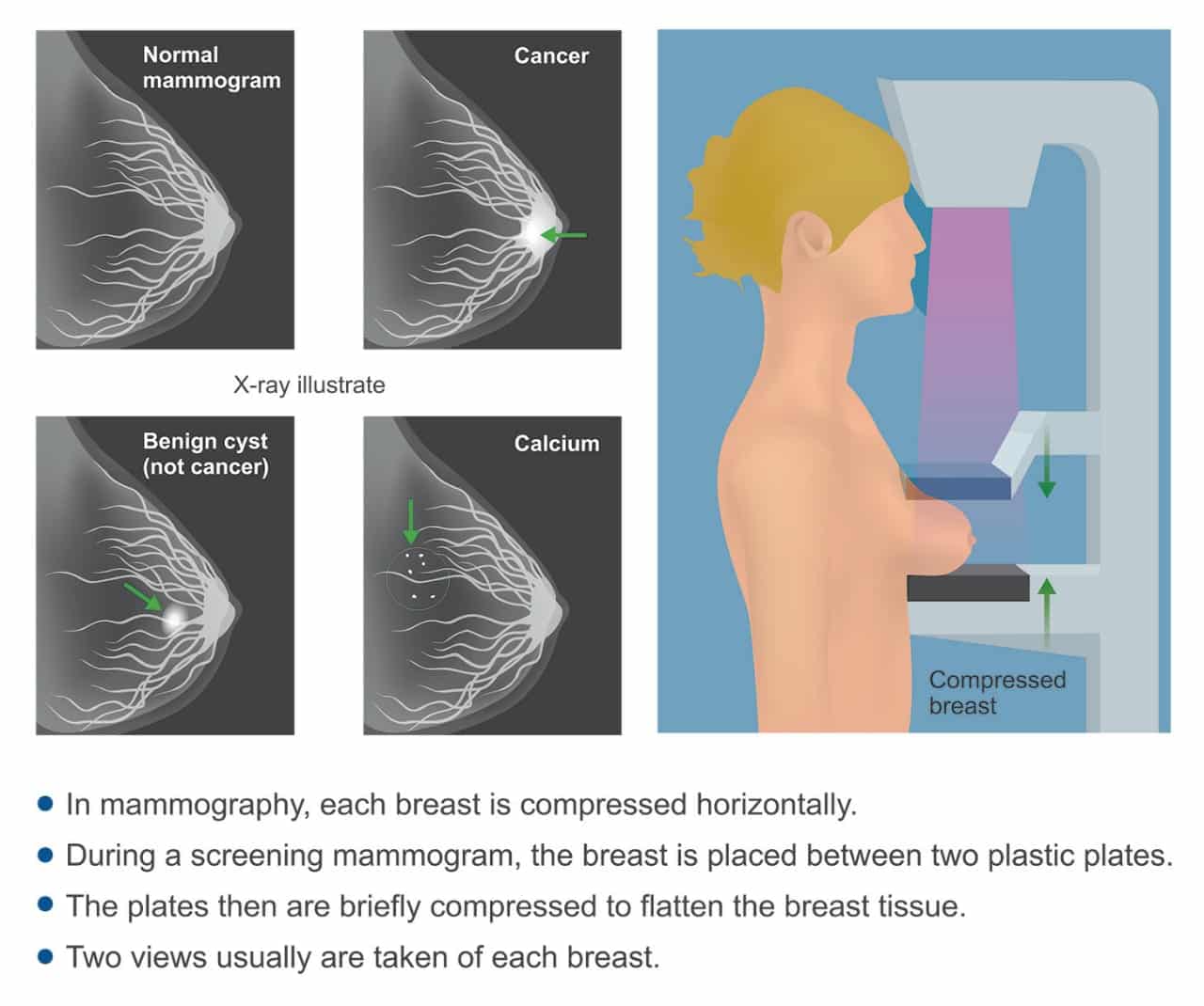
Mammography
Mammography is the best tool doctors have to screen healthy people for breast cancer, as it has been shown to lower deaths from the disease. Like any medical test, mammography involves risks, such as the possibility of additional testing and anxiety if the test falsely shows a suspicious finding, called a “false-positive” result. Up to 10% to 15% of the time, mammography will not show an existing cancer, called a “false-negative” result.
Digital mammography may be better able to find breast cancers, particularly in dense breasts. A newer type of mammogram is called tomosynthesis or 3D mammography. It may improve the ability to find small cancers and reduce the need to repeat tests due to false-positives. However, there is also the risk of diagnosing problems in the breast that would otherwise go unnoticed and would not lead to any negative consequences. This is called “overdiagnosis” and may lead to overtreatment with a potential for harm. This method is approved by the U.S. Food and Drug Administration , though research on it is ongoing.
Other breast cancer screening methods
According to the American Cancer Society , women who have BRCA gene mutations, who have a very strong family history of breast cancer, or who had prior radiation therapy to the chest should consider mammography and MRI each year.
Talk with your doctor about the method of screening recommended for you and how often screening is needed.
Don’t Miss: Is Stage 3 Breast Cancer Metastatic
Breast Cancer Is The Second Leading Cause Of Death From Cancerin American Women
Women in the United States get breast cancer more than any othertype of except for .
Breast cancer is more likely to occur as a woman ages. It occurs more often in White women than in Black women, but Black women die from breast cancer more often than White women.
Breast cancer rarely occurs in men. Because men with breast cancer usually have a lump that can be felt, tests are not likely to be helpful.
Susan G Komen Breast Self
1. Know your risk
- Talk with a health care providerabout your risk of breast cancer
2. Get screened
- Talk with a health care provider aboutwhich screening tests are right for you if youre at higher risk
- Have amammogramevery year starting at age 40 if youre at average risk
- Have aclinical breast examat least every 3 years starting at age 20, and every year starting at age 40
- Sign up for your screening reminder atkomen.org/reminder
3. Know what is normal for you and see a health care provider if you notice any of these breast changes :
- Lump, hard knot or thickening inside the breast or underarm area
- Swelling, warmth, redness or darkening of the breast
- Change in the size or shape of the breast
- Dimpling or puckering of the skin
- Itchy, scaly sore or rash on the nipple
- Pulling in of the nipple or other parts of the breast
- Nipple discharge that starts suddenly
- New pain in one spot that doesnt go away
4. Make healthy lifestyle choices
Recommended Reading: Can 15 Year Olds Get Breast Cancer
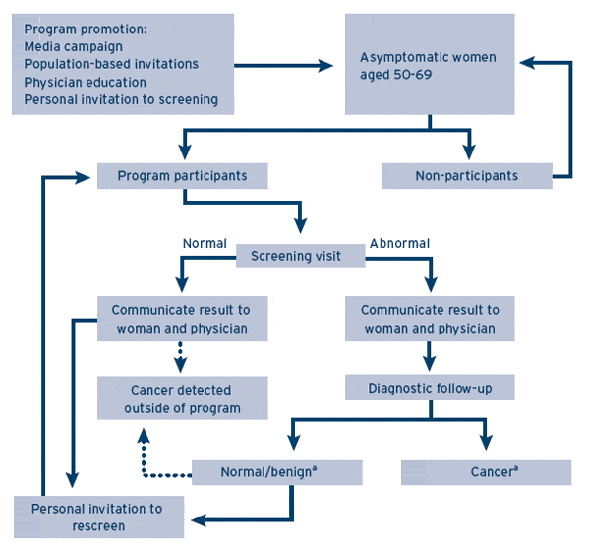
Example Of Breast Cancer Screening
Incidence and Mortality
The American Cancer Society estimated that, in 2004, 215,990 women would be newly diagnosed with breast cancer 40,110 would die of this disease.20 About 59,390 women will be diagnosed with carcinoma in situ of the breast, primarily by mammography.20 From 1996 to 2000, the age-adjusted incidence in nine Surveillance, Epidemiology, and End Results registries was about 137 per 100,000 women the age-adjusted mortality during this period was about 28 per 100,000.21 The probability at birth of being diagnosed with breast cancer in 80 years of life is about 11% the probability at birth of dying of breast cancer by age 80 is about 2%.21 Breast cancer incidence for all women increased from 1980 to 2000, although the increase slowed considerably in the late 1990s. Between 1990 and 2000, breast cancer mortality for all women decreased by about 2.3% per year.22,68 The reasons for this decrease are not clear and may be due to a combination of screening and improved treatment.69
What Are Screening Tests
Screening refers to tests and exams used to find a disease in people who dont have any symptoms. The goal of screening tests for breast cancer is to find it early, before it causes symptoms . Early detection means finding and diagnosing a disease earlier than if youd waited for symptoms to start.
Breast cancers found during screening exams are more likely to be smaller and less likely to have spread outside the breast. The size of a breast cancer and how far it has spread are some of the most important factors in predicting the prognosis of a woman with this disease.
Read Also: Can Hormones Cause Breast Cancer
Breast Cancer Is A Disease In Which Malignant Cellsform In The Tissues Of The Breast
The is made up of and . Each breast has 15 to 20 sections calledlobes, which have many smaller sections called . Lobules end in dozens of tiny bulbs thatcan produce milk. The lobes, lobules, and bulbs are linked by thin tubes calledducts.
Anatomy of the female breast. The nipple and areola are shown on the outside of the breast. The lymph nodes, lobes, lobules, ducts, and other parts of the inside of the breast are also shown.
Each breast also has and . The lymph vessels carry an almost colorless, watery called . Lymphvessels carry lymph between . Lymph nodes are small, bean-shaped structures that lymph and store that help fight and disease. Groups of lymph nodes are found near the breast in the , above the, and in the chest.
See the following summaries for more information about :
American Cancer Society Screening Recommendations For Women At High Risk
Women who are at high risk for breast cancer based on certain factors should get a breast MRI and a mammogram every year, typically starting at age 30. This includes women who:
- Have a lifetime risk of breast cancer of about 20% to 25% or greater, according to risk assessment tools that are based mainly on family history
- Have a known BRCA1 or BRCA2 gene mutation
- Have a first-degree relative with a BRCA1 or BRCA2 gene mutation, and have not had genetic testing themselves
- Had radiation therapy to the chest when they were between the ages of 10 and 30 years
- Have Li-Fraumeni syndrome, Cowden syndrome, or Bannayan-Riley-Ruvalcaba syndrome, or have first-degree relatives with one of these syndromes
The American Cancer Society recommends against MRI screening for women whose lifetime risk of breast cancer is less than 15%.
Theres not enough evidence to make a recommendation for or against yearly MRI screening for women who have a higher lifetime risk based on certain factors, such as:
- Having a personal history of breast cancer, ductal carcinoma in situ , lobular carcinoma in situ , atypical ductal hyperplasia , or atypical lobular hyperplasia
- Having extremely or heterogeneously dense breasts as seen on a mammogram
If MRI is used, it should be in addition to, not instead of, a screening mammogram. This is because although an MRI is more likely to find cancer than a mammogram, it may still miss some cancers that a mammogram would find.
Also Check: What Is The Prognosis For Stage 4 Breast Cancer
The Importance Of Breast Cancer Screenings
Breast cancer screenings are the most reliable way to detect the disease as soon as possible. The technology can discover breast cancer before any symptoms appear, while its small and easier to treat successfully. Nearly 13% of women in the U.S. will develop invasive breast cancer within their lifetime. Breast cancer screenings can help save their lives.
Early detection is crucial for preventing deaths from breast cancer. One study showed that women with breast cancer who participated in regular screenings had a 60% lower risk of dying within 10 years of their diagnosis and a 47% lower risk within 20 years. Breast cancer screenings are the first line of defense against the disease to significantly improve the odds of successful treatment and recovery.
The Harms Of Mammography Include The Following:
False-positive test results can occur.
Screening test results may appear to be abnormal even though no cancer is present. A false-positive test result is usually followed by more tests , which also have risks.
When a breast biopsy result is abnormal, getting a second opinion from a different pathologist may confirm a correct breast cancer diagnosis.
Most abnormal test results turn out not to be cancer. False-positive results are more common in the following:
- Younger women .
- Women who have had previous breast biopsies.
- Women with a family history of breast cancer.
- Women who take hormones for menopause.
False-positive results are more likely the first time screening mammography is done than with later screenings. For every ten women who have a single mammogram, one will have a false-positive result. The chance of having a false-positive result goes up the more mammograms a woman has. Comparing a current mammogram with a past mammogram lowers the risk of a false-positive result.
The skill of the radiologist also can affect the chance of a false-positive result.
False-positive results can lead to extra testing and cause anxiety.
If a mammogram is abnormal, more tests may be done to diagnose cancer. Women can become anxious during the diagnostic testing. Even if it is a false-positive test and cancer is not diagnosed, the result can lead to anxiety anywhere from a few days to years later.
False-negative test results can delay diagnosis and treatment.
Read Also: What Age Does Breast Cancer Start
Breast Cancer Screening Essay Example
Breast cancer is a common disease that is claiming lives at a very alarming rate, women being the most vulnerable population. A distinctive character of this disease is that it is hereditary, so some of these cases are unavoidable, and it is essential for all people to stay alert to any changes in their breasts. Screening is checking for any abnormalities with the breast like lumps, discharge from the nipples and nipple tenderness among others. Testing helps to detect the disease early, and this provides higher chances of controlling the infirmity through the appropriate medical measures. It is cheaper and simpler to prevent the disease than to cure, since it proves a costly and rather a complex disease to deal with once it develops to the later stages.
If the illness is detec
ted early, the patient will not undergo chemotherapy or mastectomy . Some of its symptoms are not easily noticeable, and for that reason, it is advisable to go for screening to ensure that one is on the safe side. In the case of abnormalities after the screening, one is advised to do the diagnostic test but does not mean that one has the breast cancer.
Due to the high turnover, I had an arrangement with
see a healthy nation free of breast cancer was beginning to come true. In future, I plan to have campaigns to create awareness to all women and educate them about the benefits of early breast cancer screening.