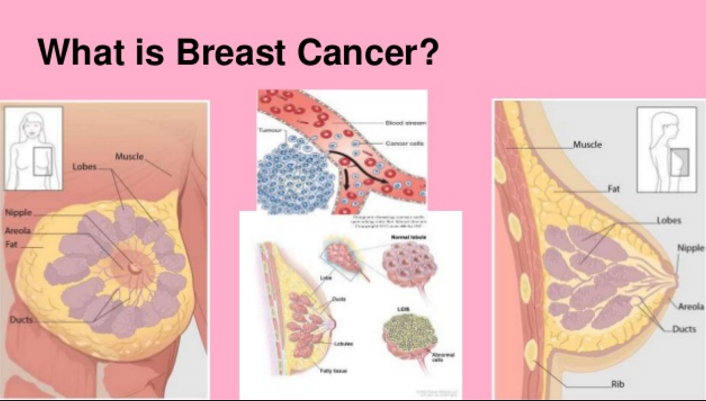
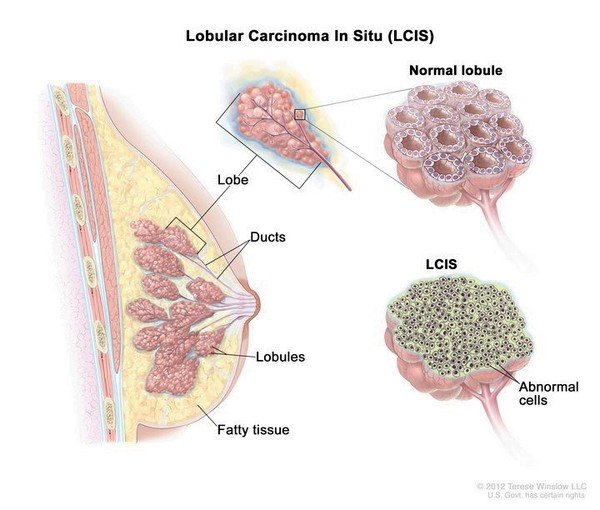
What Are Breast Lobes And Breast Ducts
Each female breast contains 15-20 sections called lobes. Each lobe is made up of many smaller sacs called lobules . It is these lobules that produce milk in breastfeeding women. The lobes and lobules are connected to the nipple by tubes called ducts, which carry milk to the nipple. Milk flows through the nipple to the outside during breastfeeding.
Why Is Inflammatory Breast Cancer So Deadly
Because of the tendency for misdiagnosis. IBC is often mistaken for mastitis, or sometimes even shingles. On other occasions, IBC may be mistaken for a different type of locally advanced breast cancer and not given the right treatment.
The difficulty of diagnosis in combination with the fast growth of cancer often means IBC is at an advanced stage at diagnosis.
The First Record Of A Mastectomy Offered For Breast Cancer Was Over 1500 Years Ago
The first record of a breast mastectomy was in A.D. 548 on Theodora, Empress of Byzantine. Significant progress in our understanding and treatment of breast cancer in recent decades has seen a dramatic reduction in the use of radical mastectomy , which was the standard surgical approach to breast cancer right up until the 1960s.
Fact 5
You May Like: Can Breast Cancer Be Cured
Benefits Of Mammography For Women Ages 40
Mammography in women ages 40-49 may lower the risk of dying from breast cancer, but the benefit is less than for older women .
The U.S. Preventive Services Task Force meta-analysis combined the results from 8 randomized controlled trials. It found no clear difference in the risk of dying from breast cancer for women ages 39-49 who got mammograms on a regular basis and their peers who did not get mammograms . If there was a difference, it was likely very small.
There are a few reasons why theres less benefit from mammography for younger women than for older women :
- Women ages 40-49 have a lower risk of breast cancer than older women.
- Younger women tend to have dense breast tissue, which can make abnormal findings hard to see on a mammogram.
- Breast cancers in younger women tend to grow faster than breast cancers in older women. This means mammography every 1-2 years may be less likely to find breast cancers in younger women early, when the chances of survival are highest.
For younger women, there are also some drawbacks of screening mammography.
Receptors For Secondary Breast Cancer

Breast cancer cells may have receptors . Hormones, or a protein called HER2, can attach to the receptors and encourage the cells to grow. A doctor called a pathologist tests cancer cells taken during a biopsy or surgery for these receptors. Your doctor uses the results of these tests to help plan your treatment.
If you have had primary breast cancer before, the receptors may not be the same as when you were first diagnosed. This may mean different treatments are useful. Your doctor may be able to diagnose a secondary cancer from your scan results. But they may still recommend a biopsy to find out more about the cancer cell receptors.Cancer that does not have receptors for either hormones or HER2 is called triple negative breast cancer.
Read Also: What Happens If Breast Cancer Is Not Treated
Risk Factors You Can Change
- Not being physically active. Women who are not physically active have a higher risk of getting breast cancer.
- Being overweight or obese after menopause. Older women who are overweight or obese have a higher risk of getting breast cancer than those at a normal weight.
- Taking hormones. Some forms of hormone replacement therapy taken during menopause can raise risk for breast cancer when taken for more than five years. Certain oral contraceptives also have been found to raise breast cancer risk.
- Reproductive history. Having the first pregnancy after age 30, not breastfeeding, and never having a full-term pregnancy can raise breast cancer risk.
- Drinking alcohol. Studies show that a womans risk for breast cancer increases with the more alcohol she drinks.
Research suggests that other factors such as smoking, being exposed to chemicals that can cause cancer, and changes in other hormones due to night shift working also may increase breast cancer risk.
Integrative Subtypes And Late Recurrence
Researchers recently developed a model to identify 11 integrative subtypes of breast cancer with different risks and timing of recurrence, according to the findings of a 2019 study published online in Nature.
Four integrative subtypes were identified that were associated with a high risk of late recurrence . Altogether, these four subtypes accounted for roughly 26% of breast cancers that were estrogen receptor-positive and HER2 negative.
These subtypes included tumors that had an enriched copy number alterations in genes that are thought to drive the growth of cancer , including:
- CCND1
- RPS6KB1
- MYC
They were also able to identify a subgroup of triple-negative tumors that were unlikely to recur after five years as well as a subgroup in which people continue to be at risk of late recurrence. A Breast Cancer Recurrence Calculator including integrative subtypes has been developed but, at the current time, this is meant for research purposes alone.
Read Also: Estrogen Dependent Breast Cancer
Removal Of The Breast Without Cancer
Certain women with breast cancer have a high risk of developing breast cancer in their other breast . Doctors may suggest that these women have that breast removed before cancer develops. This procedure is called contralateral prophylactic mastectomy. This preventive surgery may be appropriate for women with any of the following:
-
An inherited genetic mutation that increases the risk of developing breast cancer
-
At least two close, usually first-degree relatives who have had breast or ovarian cancer
-
Radiation therapy directed at the chest when women were under 30 years old
-
Lobular carcinoma in situ
In women with lobular carcinoma in situ in one breast, invasive cancer is equally likely to develop in either breast. Thus, the only way to eliminate the risk of breast cancer for these women is to remove both breasts. Some women, particularly those who are at high risk of developing invasive breast cancer, choose this option.
Advantages of contralateral prophylactic mastectomy include the following:
-
Longer survival for women with breast cancer and a genetic mutation that increases risk and possibly for women who are under 50 years old when they are diagnosed with breast cancer
-
For some women, decreased anxiety
Disadvantages of this procedure include the following:
-
Twice the risk of complications
Instead of having a contralateral prophylactic mastectomy, some women may choose to have their doctor monitor the breast closely for cancerfor example with imaging tests.
How Does Cancer Spread Beyond The Breast
Breast cancer can invade through nearby tissue, or spread through the body via the lymphatic system and blood.
- Tissue: the cancer spreads from the original site and grows into nearby areas .
- Lymphatic system: breast cancer cells break away from the original site and can enter nearby lymph tubes , grow in nearby lymph nodes or travel through lymph vessels to other parts of the body.
- Blood: breast cancer cells break away from the original site and can enter and travel through nearby blood vessels to other parts of the body.
You May Like: Do You Gain Weight With Breast Cancer
Read Also: How Breast Cancer Affects The Body
Normal Breast Changes Through Life
The female breast will go through various normal changes over the course of a lifetime. Many of these changes are driven by hormones. They can be related to the menstrual cycle, pregnancy or the normal aging process. Most breast changes are not cancer, however, if you do notice an unusual breast change, it is important that you speak with your doctor so that it can be checked as soon as possible.
Normal breast changes throughout life include:
Talking To Other People
Talking about how youre feeling can often help you cope in the early days. You may be able to do this with family and friends, but many people find this very difficult.
Talking with a specialist nurse can often help. You can ask to be put in contact with one if you havent already.
Breast Cancer Now is also here to help. Through our services you can:
Read Also: How To Cure Breast Cancer With Baking Soda
Gurugram Hospital Removes Worlds Largest Chest Tumour At 1385 Kgs
A team of doctors at Fortis Memorial Research Institute successfully removed the worlds largest chest tumour weighing 13.85 kgs from the chest of a 25-year-old male patient.
As per the available medical literature and published papers, the largest chest tumour removed till date, prior to this case, was in Gujarat in 2015 weighing 9.5 kgs, the hospital said in a statement on Thursday.
Patient Devesh Sharma came to Fortis with breathlessness and extreme uneasiness in the chest. He wasnt able to sleep straight on the bed due to breathing trouble since the last 2-3 months.
An earlier CT scan at another hospital in the city indicated the presence of a massive tumour in the chest. It occupied more than 90 per cent of the chest area, engulfing the heart and displacing both lungs which led to only 10 per cent of the lungs functioning.
In addition, the patient had a very rare blood group, AB negative.
Due to the vast size of the tumour, it could not be removed through minimal invasive surgery. Thus, the Fortis doctors, in a 4-hour long surgery, opened both the sides of the chest and cut the chest bone in between.
Post the surgery, the patient was shifted to the ICU, and was initially kept on ventilation and later weaned off.
However, the carbon dioxide in his blood started rising owing to which his lungs which had initially contracted started expanding leading to Re-expansion Pulmonary Edema .
Factors That Affect The Risk Of Breast Cancer Recurrence Following A Mastectomy
Your individual risk for breast cancer recurrence after receiving a mastectomy will depend on several factors, including the type of breast cancer you have and whether it is affected by hormones, the size and location of your tumor, how quickly the cancer cells grew and the stage of cancer at the time of treatment. In particular, if breast cancer has spread to nearby lymph nodes, such as those in the underarm area, the likelihood of recurrence may be higher.
You May Like: What Is The Worst Stage Of Breast Cancer
Treatment Of Cancer That Has Spread
Breast cancer that has spread beyond the lymph nodes is rarely cured, but most women who have it live at least 2 years, and a few live 10 to 20 years. Treatment extends life only slightly but may relieve symptoms and improve quality of life. However, some treatments have troublesome side effects. Thus, deciding whether to be treated and, if so, which treatment to choose can be highly personal.
Choice of therapy depends on the following:
-
Whether the cancer has estrogen and progesterone receptors
-
How long the cancer had been in remission before it spread
-
How many organs and how many parts of the body the cancer has spread to
-
Whether the woman is postmenopausal or still menstruating
If the cancer is causing symptoms , women are usually treated with chemotherapy or hormone-blocking drugs. Pain is usually treated with analgesics. Other drugs may be given to relieve other symptoms. Chemotherapy or hormone-blocking drugs are given to relieve symptoms and improve quality of life rather than to prolong life.
The most effective chemotherapy regimens for breast cancer that has spread include capecitabine, docetaxel, doxorubicin, gemcitabine, paclitaxel, and vinorelbine.
Hormone-blocking drugs are preferred to chemotherapy when the cancer has the following characteristics:
-
The cancer is estrogen receptorpositive.
-
Cancer has not recurred for more than 2 years after diagnosis and initial treatment.
-
Cancer is not immediately life threatening.
What Are Breast Cancer Symptoms And Signs
The most common sign of breast cancer is a new lump or mass in the breast. In addition, the following are possible signs of breast cancer:
- Thickening or lump in the breast that feels different from the surrounding area
- Inverting of the nipple
- Nipple discharge or redness
- Breast or nipple pain
Also Check: Breast Cancer Under 40 Prognosis
Where Does Breast Cancer Recur
Breast cancer recurrence can be categorized by where in the body it occurs when it returns. These categories include:
- Local recurrence This type of recurrence describes breast cancer that develops in or near the same area where it originally developed, such as scar tissue, the chest wall or other nearby tissue.
- Regional recurrence Breast cancer that returns in a nearby region, such as the lymph nodes in the armpit or collar bone, is known as a regional recurrence.
- Distant recurrence Also called metastatic recurrence, this type of recurrence describes breast cancer that returns in a distant area of the body, such as the bones, lungs or liver.
Who Provides Breast Cancer Treatment
A medical team may involve several different health professionals. It may include a GP, a radiologist, an oncologist, a breast care nurse, a surgeon and other allied health professionals such as counsellors and therapists. Having a multi-disciplinary team means a patient can receive the best care possible.
Recommended Reading: Breast Cancer Treatment Stage 2
How Breast Cancer Spreads
Breast cancer can spread through the lymphatic system, the bloodstream, or by local invasionfor instance, when cancer cells actually invade nearby tissues, such as the chest wall or ribs.
When breast cancers spread and enter the lymphatic system, they usually first arrive at nearby lymph nodes and may still be early-stage.
Metastatic breast cancer is the same thing as stage 4 breast cancer and is considered the most advanced stage. It refers to breast cancers that have spread beyond the breast and nearby lymph nodes to other regions of the body, which are called distant metastases.
While treatment options for metastatic breast cancer are similar no matter where cancer has spread, some treatments are used for specific sites of metastasis as well .
Future Research On Inflammatory Breast Cancer
Recent research on inflammatory breast cancer has focused on the work on genetic determinants that underlie the inflammatory breast cancer phenotype.
Indeed, scientists have already identified some of the genes that are present in the development and progression of this disease. However, there has been no real genetic breakthrough in the treatment of the disease.
For the most part, inflammatory breast cancer has a distinct molecular profile, though it does share some genetic changes with other breast cancers.
Read Also: Estrogen Positive Breast Cancer Survival
Should I Have Regular Routine Scans Or Blood Tests To Check For Distant Breast Cancer Recurrence
No. Routine scans to check for the presence of distant disease recurrence are not recommended in the absence of symptoms
Given the ominous nature of stage 4 disease, the obvious question is, why dont we scan for spread regularly after a first diagnosis, so that we can detect it early if it does return? The reason we dont scan or test for metastasis is that there really is no early stage 4 disease, and thus no real opportunity to intervene earlier and increase the chance of cure. Its also important to know that with recurrence, one does not progress from one stage to the next: a woman who was originally diagnosed with stage 1 breast cancer does not recur as stage 2, because once cells have taken up residence elsewhere, she is immediately considered to have stage 4 disease. And with stage 4 disease, either you respond well to treatment and the disease regresses, or you dont and it doesnt. Studies have shown that getting frequent scans after a first cancer diagnosis does not lead to improved survival, which is why we dont scan for stage 4even if we wish we could.
Current guidelines and evidence therefore recommend against routine CT or bone scans, or blood tests, to look for recurrence of cancer in patients who do not have any symptoms or other concerns that need to be followed up on.
If you do have concerning symptoms , then you should bring them to the attention of your healthcare team to be checked out.
Next Steps For Breast Cancer Survivors
Following a diagnosis of breast cancer, I always tell my patients to pace themselves. The journey after treatment can be long and challenging. The late, great Maya Angelou gave sage advice when she stated, My mission in life is not merely to survive, but to thrive, and to do so with some passion, some compassion, some humor, and some style.
These 5 steps can help you thrive in your overall health and cancer survivorship:
Take care of yourself emotionally. Seeking social support, developing strong personal relationships, accessing mental health services, and having a solid spiritual foundation are effective steps to manage lifes stressors and especially those unique to cancer survivorship.
Eat a healthy diet. Good nutrition supports overall health, such as eating a diet rich in fresh fruits, vegetables, and lean meats.
Maintain a healthy weight. Research shows that maintaining a healthy weight through a healthy diet and moderate physical activity lowers the risk of developing diabetes, high blood pressure, and other cancers and chronic diseases.
Stick with your follow-up care and other health screenings. Your routine oncology appointmentis a good time to talk about any concerns. If you notice any changes or new symptoms before your scheduled appointment, be sure to alert your health care provider. Also, take care of your entire body, including other recommended health screenings, such as Pap tests, general blood tests, blood pressure checks, and colonoscopy.
Recommended Reading: Stage 3c Breast Cancer
Mammography: Screening For Breast Cancer
Mammography is one of the best ways to detect breast cancer early. Mammography is designed to be sensitive enough to detect the possibility of cancer at an early stage, sometimes years before it can be felt. Because mammography is so sensitive, it may indicate cancer when none is presenta false-positive result. About 85 to 90% of abnormalities detected during screening are not cancer. Typically, when the result is positive, more specific follow-up procedures, usually a breast biopsy, are scheduled to confirm the result. Mammography may miss up to 15% of breast cancers. It is less accurate in women with dense breast tissue.
Breast tomosynthesis may be used with mammography to produce a clear, highly focused 3-dimensional picture of the breast. This technique makes it somewhat easier to detect cancer, especially in women with dense breast tissue. However, this type of mammography exposes women to almost twice as much radiation as traditional mammography.
Recommendations for routine screening with mammography vary. Experts disagree about
-
When it should start
When a lump or another abnormality is detected in the breast during a physical examination or by a screening procedure Screening Breast cancer occurs when cells in the breast become abnormal and divide uncontrollably. Breast cancer usually starts in the glands that produce milk or the tubes that carry… read more , other procedures are necessary.