Who Might Get A Mastectomy
Many women with early-stage cancers can choose between breast-conserving surgery and mastectomy. You may prefer mastectomy as a way to “take out all the cancer as quickly as possible.” But the fact is that in most cases, mastectomy does not give you any better chance of long-term survival compared to BCS. Studies of thousands of women over more than 20 years show that when BCS is done along with radiation, the outcome is the same as having a mastectomy.
Mastectomy might be recommended if you:
- Are unable to have radiation therapy
- Would prefer more extensive surgery instead of having radiation therapy
- Have had the breast treated with radiation therapy in the past
- Have already had BCS with re-excision that did not completely remove the cancer
- Have two or more areas of cancer in different quadrants of the same breast that are not close enough to be removed together without changing the look of the breast too much
- Have a tumor larger than 5 cm across, or a tumor that is large relative to your breast size
- Are pregnant and would need radiation therapy while still pregnant
- Have a genetic factor such as a BRCA mutation, which might increase your chance of a second cancer
- Have a serious connective tissue disease such as scleroderma or lupus, which may make you especially sensitive to the side effects of radiation therapy
- Have inflammatory breast cancer
For Women At Very High Risk Of Breast Cancer
For women in this group, removing both breasts before cancer is diagnosed can greatly reduce the risk of getting breast cancer.
Unfortunately theres no way to know for sure ahead of time if a woman will benefit from this surgery. Most women with a BRCA1 or BRCA2 gene mutation will develop breast cancer at some point. Having a prophylactic mastectomy before the cancer develops might add many years to their lives. But not all women with BRCA1 or BRCA2 mutations develop breast cancer. For some women the surgery might not have been helpful. Although they might still get some important benefits from the surgery such as peace of mind, they would also have to deal with its aftereffects, which might include physical and emotional side effects.
Are You Facing A Decision About Surgery For Dcis Or Breast Cancer
Do you have ductal carcinoma in situ or breast cancer that can be removed with surgery? If so, you may be able to choose which type of breast surgery to have. Often, your choice is between breast-sparing surgery and a mastectomy .
Once you are diagnosed, treatment will usually not begin right away. There should be enough time for you to meet with breast cancer surgeons, learn the facts about your surgery choices, and think about what is important to you. Learning all you can will help you make a choice you can feel good about.
You May Like: What Is The Most Common Treatment For Breast Cancer
Surgery To Remove Just The Area Of Cancer
Surgery to remove the area of cancer in the breast is called breast conserving surgery or a wide local excision.
The surgeon takes away the cancer and a border of healthy tissue all around it. They leave behind as much healthy breast tissue as possible.
You usually have radiotherapy to the breast after this type of surgery.
Nursing Allied Health And Interprofessional Team Monitoring
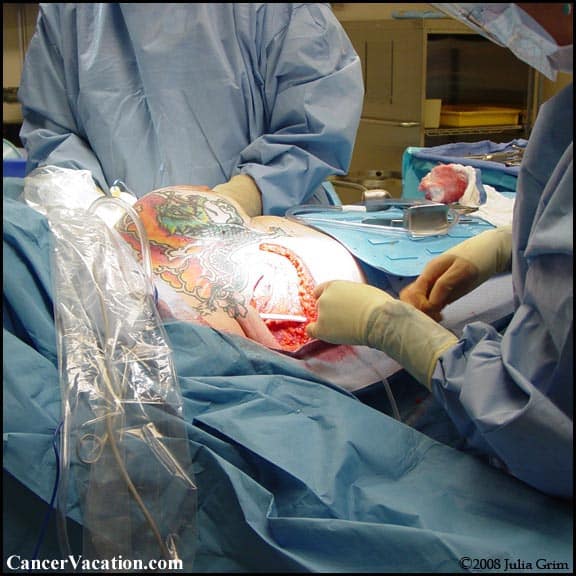
Nurses must be aware of the potential complications of these procedures to properly monitor patients in the postoperative period. In particular, monitoring the incision for any hematoma or seroma formation to let the surgeon know of any complications that may occur. Also, if drains are present, monitoring the quality and quantity of output is essential.
You May Like: Are There Different Types Of Breast Cancer
Sentinel Lymph Node Removal
Doctors frequently perform a sentinel lymph node removal during breast-conserving surgery for invasive breast cancer. Lymph nodes are part of the lymphatic system, which consists of organs and vessels that drain excess fluid from tissues and help the body fight infections.
Before surgery, doctors inject a radioactive tracer. During surgery, they may inject a blue dye. The tracer travels through the breast tissue to nearby lymph nodes under the arm. The first several nodes to absorb the tracer are called the sentinel nodes because if cancer spreads outside the breast, it is likely to spread to these nodes first.
Doctors can find this node or nodes using a gamma probe, a device that can detect the radioactive tracer. This helps doctors determine where to make an incision. The blue dye further helps them identify the correct node or nodes to remove during surgery.
Doctors remove the sentinel nodes through a small incision under the arm to see if they contain cancer. If they dont, then no further lymph nodes need to be removed.
If cancer is found in the sentinel nodes, your surgeon may discuss with you whether another procedure, called axillary lymph node dissection, is needed to remove additional nodes where cancer may have spread.
Should I Consider Surgery To Lower My Risk Of Breast Cancer
You might consider preventive surgery if you:
- Have a mutation in the BRCA1 or BRCA2 gene that is found by genetic testing
- Have a strong family history of breast cancer
- Had radiation therapy to the chest before age 30
- Have cancer in one breast
Like any type of surgery, a mastectomy can have risks and side effects, some of which could affect your quality of life. Because of this, preventive surgery is not usually a good option for women who are at average risk of breast cancer, or for those who are at only slightly increased risk.
For women who are known to have a BRCA1 or BRCA2 gene mutation, a prophylactic oophorectomy might be recommended as well.
You May Like: How Effective Is Radiation Therapy For Breast Cancer
Which Women Might Consider Having Surgery To Reduce Their Risk Of Breast Cancer
Women who inherit a deleterious mutation in the BRCA1 gene or the BRCA2 gene or mutations in certain other genes that greatly increase the risk of developing breast cancer may consider having bilateral prophylactic mastectomy and/or bilateral prophylactic salpingo-oophorectomy to reduce this risk.
In two studies, the estimated risks of developing breast cancer by age 70 years were 55 to 65 percent for women who carry a deleterious mutation in the BRCA1 gene and 45 to 47 percent for women who carry a deleterious mutation in the BRCA2 gene . Estimates of the lifetime risk of breast cancer for women with Cowden syndrome, which is caused by certain mutations in the PTEN gene, range from 25 to 50 percent or higher , and for women with Li-Fraumeni syndrome, which is caused by certain mutations in the TP53 gene, from 49 to 60 percent .
Other women who are at very high risk of breast cancer may also consider bilateral prophylactic mastectomy, including:
- those with a strong family history of breast cancer
- those with lobular carcinoma in situ plus a family history of breast cancer
- those who have had radiation therapy to the chest before the age of 30 yearsâfor example, if they were treated with radiation therapy for Hodgkin lymphoma
What Kinds Of Surgery Can Reduce The Risk Of Breast Cancer
Two kinds of surgery can be performed to reduce the risk of breast cancer in a woman who has never been diagnosed with breast cancer but is known to be at very high risk of the disease.
A woman can be at very high risk of developing breast cancer if she has a strong family history of breast and/or ovarian cancer, a deleterious mutation in the BRCA1 gene or the BRCA2 gene, or a high-penetrancemutation in one of several other genes associated with breast cancer risk, such as TP53 or PTEN.
The most common risk-reducing surgery is bilateral prophylactic mastectomy . Bilateral prophylactic mastectomy may involve complete removal of both breasts, including the nipples , or it may involve removal of as much breast tissue as possible while leaving the nipples intact . Subcutaneous mastectomies preserve the nipple and allow for more natural-looking breasts if a woman chooses to have breast reconstruction surgery afterward. However, total mastectomy provides the greatest breast cancer risk reduction because more breast tissue is removed in this procedure than in a subcutaneous mastectomy .
Even with total mastectomy, not all breast tissue that may be at risk of becoming cancerous in the future can be removed. The chest wall, which is not typically removed during a mastectomy, may contain some breast tissue, and breast tissue can sometimes be found in the armpit, above the collarbone, and as far down as the abdomenâand it is impossible for a surgeon to remove all of this tissue.
Recommended Reading: Stefanie Spielman Fund For Breast Cancer Research
Surgery And Drug Therapies
The choice of surgery does not affect whether you will need chemotherapy, hormone therapy, HER2-targeted therapy and/or other drug therapies. Drug therapies are given based on the characteristics of the tumor, not the type of surgery you have.
For example, whether or not you will need hormone therapy depends on hormone receptor status. Hormone receptor status is a biomarker.
Learn more about .
How Long Is The Recovery From Breast Cancer Surgery
You may be sore and have limited movement in your chest and arms for a few weeks afterward. Youll have painkillers to take home with you. Youll also be given arm and shoulder exercises to practice daily. These are important to prevent stiffness. You may feel tired for a while. It can take several weeks to regain your former energy levels. You may need someone to help you around the house. Most people are able to resume their normal activities within about a month.
You May Like: How To Tell If Breast Cancer
Questions About The Effectiveness Of Breast Cancer Surgery
Which type of breast cancer surgery is best for my cancer?
| Lumpectomy or other breast-sparing surgery | Most women with DCIS or breast cancer can choose to have breast-sparing surgery, usually followed by radiation therapy. |
|---|---|
| Mastectomy | Most women with DCIS or breast cancer can choose to have a mastectomy.A mastectomy may be a better choice for you if
|
| Mastectomy with reconstruction |
If you have a mastectomy, you might also want breast reconstruction surgery.You can choose to have reconstruction surgery at the same time as your mastectomy or wait and have it later. Your surgeon can talk with you about how much skin, including the nipple and areola, might be preserved for reconstruction. |
Will the type of breast cancer surgery I have affect how long I live?
No. Research shows that women who have breast-sparing surgery live as long as women who have a mastectomy. This does not change if you also have reconstruction.
What are the chances that my breast cancer will return in the same area?
Think About What Is Important To You

After you have talked with a breast cancer surgeon and learned the facts, you may also want to talk with your spouse or partner, family, friends, or other women who have had breast cancer surgery.
Surgery Choices: Theresa, Cindy, Paula
Three women describe how they decided which type of breast cancer surgery was right for them.
Then, think about what is important to you. Thinking about these questions and talking them over with others might help:
Recommended Reading: Can Breast Cancer Cause Arm Pain
Cosmetic Concerns After Mastectomy
Patients undergoing mastectomy may have concerns about the appearance oftheir breast after the procedure. Fortunately, breast reconstruction ispossible for the majority of patients after mastectomy. Your doctor willdiscuss with you your options regarding reconstructive surgery. Alternativesolutions to reconstruction after mastectomy include the use of an externalprosthesis or a special mastectomy bra.
Reconstruction after Breast Cancer | Pam’s Story
After turning to Johns Hopkins for a second opinion after her breast cancer diagnosis, Pam Vierra says her reconstruction changed her life, leaving her in better shape than ever.
Mastectomy And Breast Reconstruction
A breast reconstruction is surgery to make a new breast after removal of the breast tissue. The surgeon creates a new breast shape using tissue from another part of your body, or an implant, or both.
Your surgeon will talk to you before the operation about the options for breast reconstruction.
It is your choice whether you have breast reconstruction or not but you should be offered one. Some women choose not to have reconstruction.
You might be able to have breast reconstruction at the same time as the mastectomy . Or you might have it some months or years afterwards . Whenever possible you should be able to choose when you have a reconstruction operation. Everyone is different and some women prefer to have it at the same time as the mastectomy while others prefer to delay it.
You will have time to talk to your surgeon or specialist nurses and ask any questions you have. They may have photographs to show you of women who have had a breast reconstruction.
If you aren’t having an immediate breast reconstruction, your nurse will show you artificial breast shapes . They are also called softies or cumfies.
You put these prostheses inside your bra to create a breast shape. Your nurse will help you find the right size and shape.
Don’t Miss: What Is Her3 Breast Cancer
Are Lymph Nodes Removed During A Lumpectomy
Women with invasive breast cancer typically have one or more lymph nodes taken from the underarm area during a lumpectomy. These nodes, called the sentinel nodes, are the first lymph nodes to which cancer cells would travel if they were to leave the breast. This is done so that your doctor can check to see if the cancer has spread.
Women with DCIS undergoing lumpectomy do not need to have lymph nodes removed.
Read Also: How Can I Tell If I Have Breast Cancer
Assessing Lymph Nodes During Surgery
Some hospitals are set up to assess the lymph nodes during breast surgery. The removed nodes will be looked at by a pathologist, who will tell the surgeon the result during the operation.
The most common test used is called One Step Nucleic Acid Amplification .
If the sentinel node contains cancer cells, the surgeon may then remove more lymph nodes.
Having lymph nodes assessed during surgery avoids a second operation.
Also Check: Metastatic Triple Negative Breast Cancer Treatment
What Support Does Msk Offer To Women Recovering From A Lumpectomy
MSKs quality-of-life specialists provide comprehensive follow-up care to help you recover from a lumpectomy. Many services are available at our New Jersey, Long Island, and Westchester County locations as well as at our Evelyn H. Lauder Breast Center in Manhattan.
- Wellness therapies from integrative medicine specialists can relieve emotional or physical symptoms after surgery or for potential side effects.
- Rehabilitation and exercise therapies can help you heal and recover your strength, flexibility, and stamina.
- Find emotional support through our Counseling Center, online support groups, or patient-to-patient support program, which connects you with other breast cancer survivors who understand your challenges and concerns. Our social workers are available across our treatment locations to provide emotional support and guidance. They can also help with some of the practical aspects of having cancer, such as transportation assistance and the impact on your job.
Will Insurance Cover The Surgery
If you have health insurance, surgery for breast cancer is typically covered.
You may need to meet a deductible before your insurance pays for surgery. Your deductible may be as low as $0 or as high as $7,500 per year.
You may also need to pay coinsurance or copays depending on your plan.
You can contact your insurance provider to learn about your plan.
The Womens Health and Cancer Rights Act requires all group health plans that cover mastectomy to also cover breast reconstruction.
Medicare covers breast reconstruction.
Also Check: Common Symptoms Of Breast Cancer
Possible Side Effects Of Mastectomy
Bleeding and infection at the surgery site are possible with all operations. The side effects of mastectomy can depend on the type of mastectomy you have . Side effects can include:
- Pain or tenderness at the surgery site
- Swelling at the surgery site
- Buildup of blood in the wound
- Buildup of clear fluid in the wound
- Limited arm or shoulder movement
- Numbness in the chest or upper arm
- Neuropathic pain in the chest wall, armpit, and/or arm that doesnt go away over time. It is also called post-mastectomy pain syndrome or PMPS.
- If axillary lymph nodes are also removed, other side effects such as lymphedema may occur.
What To Expect After A Lumpectomy For Breast Cancer
Heres how many days you should set aside for recovery.
Surgery is just one treatment option for breast cancer, but its a common one: Most people I diagnose with breast cancer will have surgery at some point during their treatment, says Jaime Alberty-Oller, MD, breast cancer oncologist and surgeon at Dubin Breast Center, Mount Sinai Hospital in New York City.
Its common for women to have many questions when a lumpectomy for breast cancer is recommended, according to Dr. Alberty-Oller. Many women are curious about how the surgery treats the cancer, how the breasts will look afterward, and the expected recovery time.
What Is a Lumpectomy?
Lumpectomies are a type of breast surgery where, instead of removing all of the breast tissue , a portion of the breast is removed. The surgeon will remove the cancer, as well as a rim of normal tissue surrounding it, which is called the margin. A lumpectomy may also be called breast-conserving surgery, quadrantectomy, partial mastectomy, or segmental mastectomy. Learn more about types of breast cancer surgery here.
The goal of lumpectomy surgery is to take the cancer out and do the safest operation that we can, says Dr. Alberty Oller. The amount of breast tissue thats removed during a lumpectomy depends on the size and location of the tumor, your breast size, and other factors.
Lumpectomy Surgery: What to Expect
Side effects: Common side effects after a lumpectomy may include:
Don’t Miss: When You Have Breast Cancer Does It Hurt