What Happens If Something Is Detected On My Screening Exam
Lumps, other abnormalities or questionable findings in the breast are often detected by screening tests. However, it is not always possible to tell from these imaging tests whether a finding is benign or cancerous. To determine whether there is a cancer present, your doctor may recommend that one or more of the following imaging tests may be performed:
- diagnostic mammography
- breast ultrasound
- breast MRI
If a finding is proven to be benign by its appearance on these exams, no further steps may need to be taken. If these tests do not clearly show that the finding is benign, a biopsy may be necessary. In a biopsy, a small amount of tissue is removed under local anesthesia so that it can be examined in a laboratory. One of the following image-guided procedures is used during a breast biopsy:
A pathologist;examines the removed tissue specimen and makes a final diagnosis. Depending on the facility, the radiologist or your referring physician;will share the results with you.
With early detection and improved treatments, more women are surviving breast cancer. If cancer is diagnosed, your doctor will discuss your treatment options and together you will determine your course of treatment. Today, women have more treatment options than ever before. For more information on treatment, see the Breast Cancer Treatment page.
The Breast Cancer Risk Assessment Tool
The Breast Cancer Risk Assessment Tool allows health professionals to estimate a woman’s risk of developing invasive breast cancer over the next 5 years and up to age 90 .
The tool uses a womans personal medical and reproductive history and the history of breast cancer among her first-degree relatives to estimate absolute breast cancer riskher chance or probability of developing invasive breast cancer in a defined age interval.
The tool has been validated for white women, black/African American women, Hispanic women and for Asian and Pacific Islander women in the United States. The tool may underestimate risk in black women with previous biopsies and Hispanic women born outside the United States. Because data on American Indian/Alaska Native women are limited, their risk estimates are partly based on data for white women and may be inaccurate. Further studies are needed to refine and validate these models.
This tool cannot accurately estimate breast cancer risk for:
- Women carrying a breast-cancer-producing mutation in BRCA1 or BRCA2
- Women with a previous history of invasive or in situ breast cancer
What Are Genomic Tests
Genomic tests analyze a sample of a cancer tumor to see how active certain genes are. The activity level of these genes affects the behavior of the cancer, including how likely it is to grow and spread. Genomic tests are used to help make decisions about whether more treatments after surgery would be beneficial.
While their names sound similar, genomic testing and genetic testing are very different.
Genetic testing is done on a sample of your blood, saliva, or other tissue and can tell if you have a change in a gene that is linked to a higher risk of breast cancer. See the Genetic Testing pages for more information.
Also Check: Does Breast Cancer Show Up In Blood Work
Where Can I Go To Get Screened
You can get screened for breast cancer at a clinic, hospital, or doctors office. If you want to be screened for breast cancer, call your doctors office. They can help you schedule an appointment.
Most health insurance plans are required to cover screening mammograms every one to two years for women beginning at age 40 with no out-of-pocket cost .
Are you worried about the cost? CDC offers free or low-cost mammograms. Find out if you qualify.
Keeping Health Insurance And Copies Of Your Medical Records

Even after treatment, its very important to keep health insurance. Tests and doctor visits cost a lot, and even though no one wants to think of their cancer coming back, this could happen.
At some point after your treatment, you might find yourself seeing a new doctor who doesnt know about your medical history. Its important to keep copies of your medical records to give your new doctor the details of your diagnosis and treatment. Learn more in Keeping Copies of Important Medical Records.
Don’t Miss: Can Breast Cancer Spread To Bones
Should I Go For Breast Screening
Its important that you have access to enough information about the benefits and harms of breast screening to make the decision.
You can talk to your own doctor or nurse. Or you can contact the Cancer Research UK nurses on freephone 0808 800 4040. The lines are open from 9am to 5pm, Monday to Friday.
Benefits Of Mammographic Screening
The ACS systematic review also examined the effect of screening mammography on life expectancy. Although the review concluded that there was high-quality evidence that mammographic screening increases life expectancy by decreasing breast cancer mortality, the authors were not able to estimate the size of the increase 23.
You May Like: Does Having Breast Cancer Make You Tired
* You Are At Average Risk If You Have:
- no symptoms of breast cancer
- no history of invasive breast cancer
- no history of ductal or lobular carcinoma in situ
- no history of atypia
- no family history of breast cancer in a first-degree relative
- no suggestion or evidence of a hereditary syndrome such as a BRCA mutation
- no history of mantle radiation
If You Have Further Questions Contact Your Ob
Don’t have an ob-gyn? Search for doctors near you.
FAQ178
Copyright 2021 by the American College of Obstetricians and Gynecologists. All rights reserved. Read copyright and permissions information.
This information is designed as an educational aid for the public. It offers current information and opinions related to women’s health. It is not intended as a statement of the standard of care. It does not explain all of the proper treatments or methods of care. It is not a substitute for the advice of a physician. Read ACOGs complete disclaimer.
Also Check: How Do I Self Check For Breast Cancer
Screening Guidelines For Women At Average Breast Cancer Risk
MSK doctors recommend the following for women at average risk* of breast cancer:
- Women between the ages of 25 and 40 should have anannual clinical breast examination.
- Women 40 and older should have an annual mammogram in addition to anannual clinical breast examination.
- Ultrasound may be recommended for women with dense breast tissue.
- All women should consider performing a monthly self breast exam beginning at age 20 and become familiar with their breasts so they are better able to notice changes.
Genetic Screening Test For Breast Cancer: Starting This Year More Women Can Be Tested
2020-11-08T12:02:48.785Z
A new and important line following the expansion of the health services basket: starting in 2020, more women can be tested for a mutation in the BRCA gene. Get to know the life-saving screening test and find out what the BRCA1 and BRCA2 genes are, why they should be tested and what the “Julie Julie effect” is.
-
health
Read Also: Can Biting Breasts Cause Cancer
American Cancer Society Screening Recommendations For Women At Average Breast Cancer Risk
The COVID-19 pandemic has resulted in many elective procedures being put on hold, and this has led to a substantial decline in cancer screening. Health care facilities are providing cancer screening during the pandemic with many safety precautions in place. Learn how you can talk to your doctor and what steps you can take to plan, schedule, and get your regular cancer screenings in;Cancer Screening During the COVID-19 Pandemic.
These guidelines are for women at average risk for breast cancer. For screening purposes, a woman is considered to be at average risk if she doesnt have a personal history of breast cancer, a strong family history of breast cancer, or a genetic mutation known to increase risk of breast cancer , and has not had chest radiation therapy before the age of 30.
Women between 40 and 44 have the option to start screening with a mammogram every year.
Women 45 to 54 should get mammograms every year.
Women 55 and older can switch to a mammogram every other year, or they can choose to continue yearly mammograms. Screening should continue as long as a woman is in good health and is expected to live at least 10 more years.
All women should understand what to expect when getting a mammogram for breast cancer screening what the test can and cannot do.
Clinical breast exams are not recommended for breast cancer screening among average-risk women at any age.
Breast Cancer Screening Saves Lives
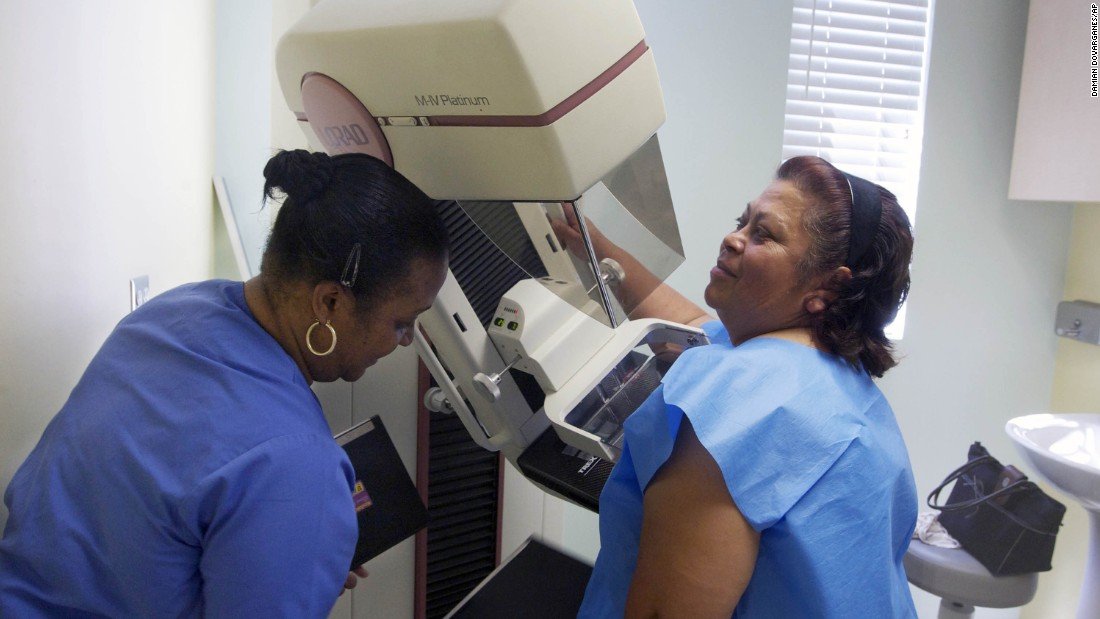
Screening tests can find breast cancer early, when the chances of survival are highest. Getting screened regularly means your doctor is likely to know sooner if theres a problem, so you can get effective treatment as early as possible. There are more than 3.5 million breast cancer survivors in the U.S. todaymore than any other group of cancer survivorslargely thanks to advances in screening and treatment.
You May Like: How To Help Breast Cancer Awareness
Mammography Is The Most Common Screening Test For Breast Cancer
A mammogram is a picture of the inside of the breast. Mammography may find tumors that are too small to feel. It may also find ductal carcinoma in situ . In DCIS, abnormalcells line the breast duct, and in some women may become invasive cancer.
There are three types of mammograms:
- Film mammography is an x-ray picture of the breast.
- Digital mammography is a computer picture of the breast.
- Digital breast tomosynthesis uses x-rays to take a series of pictures of the breast from many different angles. A computer is used to make 3-D pictures of the breast from these x-rays.
DBT was approved by the U.S. Food and Drug Administration in 2018 and is now used in 3 out of 4 facilities. One study found that DBT reduced false-positive test results and was likely to reduce breast cancer deaths. More studies are being done to provide information on digital mammography compared to DBT.
Mammography is less likely to find breast tumors in women with dense breast tissue. Because both tumors and dense breast tissue appear white on a mammogram, it can be harder to find a tumor when there is dense breast tissue. Younger women are more likely to have dense breast tissue.
Many factors affect whether mammography is able to detect breast cancer:
Women aged 50 to 69 years who have screening mammograms have a lower chance of dying from breast cancer than women who do not have screening mammograms.
Getting Your Screening Results
You usually get your breast screening results, in writing, about 2 to 3 weeks after your mammogram. A copy is also sent to your GP. If you have not heard anything after 3 weeks, call your breast screening unit and ask them to check your results.
Your results letter will tell you one of the following:
- Your mammogram is normal, and you will be invited again for screening in 3 years if you are still of screening age.;About 96 out of every 100 women who have breast screening have a normal result.
- You are invited for a repeat mammogram.;This can happen if the mammogram has missed part of the breast tissue, the x-ray picture is blurred or there is a problem with the equipment .
- You are invited to a breast assessment clinic for further tests.;This happens to about 4 out of every 100 women who have breast screening . But around 3 out of 4 women who have further tests do not have breast cancer.
Recommended Reading: Can You Get Breast Cancer At 20
Breast Cancer Is The Second Leading Cause Of Death From Cancer In American Women
Women in the United States get breast cancer more than any other type of cancer except for skin cancer.
Breast cancer is more likely to occur as a woman ages. It occurs more often in White women than in Black women, but Black women die from breast cancer more often than White women.
Breast cancer rarely occurs in men. Because men with breast cancer usually have a lump that can be felt, screening tests are not likely to be helpful.
If The Cancer Comes Back
If cancer does return, your treatment options will depend on where it comes back, what treatments you’ve had before, and your current health and preferences. For more information on how recurrent cancer is treated, see Treatment of Recurrent Breast Cancer.;
Its important to know that women who have had breast cancer can also still get other types of cancer. In fact, women who have had breast cancer are at higher risk for certain other cancers. Because of this, its important to follow the American Cancer Society guidelines for the early detection of cancer, such as those for colorectal cancer and cervical cancer. To learn more about the risks of second cancers and what you can do about them, see Second Cancers After Breast Cancer. ;
You May Like: Are Breast Cancer Lumps Hard Or Soft
Screening Vs Diagnostic Mammogram
The type of machine used and the process to get the first four images is the same for a screening or diagnostic mammogram. More images may need to be taken in a diagnostic mammogram to look at a specifici area more closely, and different types of tools may be used to compress the tissue in different ways.
Benefits & Potential Harms
There Are Three Screening Methods
There are three types of tests that may be used to screen for breast cancer.
Clinical Breast Exam A CBE is a physical exam of your breast and underarm area by a health care provider. Its often done during your regular medical check-up. A CBE should be performed by someone whos trained in the techniquenot all health care providers have this training. If your doctor doesnt offer you a CBE at your check-up and you would like one, ask if he or she can perform one or refer you to someone who can.
MammogramMammography uses X-rays to make images of the breast . While some tumors in the breast are aggressive and grow quickly, most grow slowly. In some cases a tumor may have been growing for as long as 10 years before it creates a lump large enough to feel. Mammography can find cancers early, before you would have noticed any signs or symptoms. Thats why its often used as a screening test. It can also be used as a follow-up test . If youve noticed a change in your breast and are getting a mammogram, tell the technologist what you noticed before your exam. If you evernotice a change in your breasteven if youve had a mammogram recently and had normal resultsget checked out by a doctor asap. And if youve never had a mammogram before, heres everything you wanted to know .
Recommended Reading: What Kind Of Doctor Do You See For Breast Cancer
General Considerations For Screening
The goal of screening for cancer is to detect preclinical disease in healthy, asymptomatic patients to prevent adverse outcomes, improve survival, and avoid the need for more intensive treatments. Screening tests have both benefits and adverse consequences .
Breast self-examination, breast self-awareness, clinical breast examination, and mammography all have been used alone or in combination to screen for breast cancer. In general, more intensive screening detects more disease. Screening intensity can be increased by combining multiple screening methods, extending screening over a wider age range, or repeating the screening test more frequently. However, more frequent use of the same screening test typically is associated with diminishing returns and an increased rate of screening-related harms. Determining the appropriate combination of screening methods, the age to start screening, the age to stop screening, and how frequently to repeat the screening tests require finding the appropriate balance of benefits and harms. Determining this balance can be difficult because some issues, particularly the importance of harms, are subjective and valued differently from patient to patient. This balance can depend on other factors, particularly the characteristics of the screening tests in different populations and at different ages.
Getting A Second Opinion

Getting a second opinion during your cancer care process is common. Its a good idea to get your second opinion before starting treatment, because a second opinion can alter your diagnosis and thus your treatment. However, you can get a second opinion at any point during treatment.
During your cancer care, consider asking for a second opinion in these instances:
- after your pathology report is complete
- before surgery
- after your staging work is complete, if you are uncomfortable with the treatment plan your doctor recommends
- while planning treatments following surgery
- during treatment, if you believe there may be a reason to change the course of your treatment
- after completing treatment, especially if you didnt ask for a second opinion prior to starting treatment
Recommended Reading: Does Breast Cancer Show Up In Blood Tests
Don’t Let Precious Samples Go Untested
Did you know that high sample input requirements significantly limit the usability of hybrid capture-based NGS tests? You might assume that all NGS tests are created equal. However, recent data from more than 20 US laboratories has shown that small biopsies and low-tumor content samples can pose significant challenges for some tests – some labs have test failure rates of 58%.
This means that less than half of all samples will be successfully sequenced. Not with Oncomine Solutions. You can experience a sequencing success rate of over 95% with only 10ng of nucleic acid input. Get NGS results for most of the precious samples you have.