Some Risk Factors For Breast Cancer
The following are some of the known risk factors for breast cancer. However, most cases of breast cancer cannot be linked to a specific cause. Talk to your doctor about your specific risk.
Age. The chance of getting breast cancer increases with age. Nearly 80 percent of breast cancers are found in those over the age of 50.
Personal history of breast cancer. An individual who has had breast cancer in one breast is at an increased risk of developing cancer in the other breast.
Family history of breast cancer. A higher risk of breast cancer is associated with having an immediate relative with breast cancer, especially at a young age . Having other relatives with breast cancer may also raise the risk.
Genetic factors. Certain genetic mutations, including changes to the BRCA1 and BRCA2 genes, are associated with a higher risk of developing breast cancer at some point. Other gene changes may raise breast cancer risk as well. For more information, ask your doctor about comprehensive biomarker testing, which may include genetic testing for inherited cancer risk.
Childbearing and menstrual history. Research suggests a link between reproductive and menstrual history and the risk of breast cancer. Higher risk factors include:
- Early onset menstruation
- Late onset menopause
- Never having children, childbirth later in life or not breastfeeding
Hormone use. Menopausal hormone therapy and certain types of birth control may have hormones that are risk factors for breast cancer.
Biomarkers For Breast Cancer Detection
presents numerous markers used for breast cancer detection . DNA biomarkers provide useful information on the process of tumor growth but they are associated with poor early detection due to low concentrations of cancer markers . Protein biomarkers are the major indicator of breast cancer, which can be classified as predictive and prognostic markers . Predictive protein markers provide information of the particular therapeutic intervention, while prognostic protein markers offer the overall information of the subjects.
How Does A Radiologist See Breast Cancer On Mammography & Ultrasound
When you look at mammography or ultrasound images, you might wonder how radiologists make any sense of them. How can they identify potential cancers in those Rorschach tests of gray and white? While even the most advanced imaging technology doesnt allow radiologists to identify cancer with certainty, it does give them some strong clues about what deserves a closer look. Today well discuss a few things that radiologists are on the lookout for when examining mammography and breast ultrasound images.
When radiologists look at a mammogram, theyre looking for three primary things:
- Changes from what is seen in previous images
- Calcifications
- Masses
If youve had a mammogram before, it is helpful to give your current radiologist access to your previous mammography images. Anytime you visit a new mammography clinic, let them know where youve had breast imaging done in the past so they are able to note any changes over time.
Masses comprise a variety conditions, including cysts, benign solid tumors, and malignancies. Their size, shape, borders, and internal composition can give insight into whether they represent cancer. Cancerous tumors often appear as white masses with blurry or spiked borders, which indicate infiltration into the surrounding tissue. Cysts are often indistinguishable from solid tumors on a mammogram, so ultrasound is often used to determine whether a mass is solid or fluid filled .
You May Like: How To Cure Breast Cancer With Baking Soda
What To Expect At The Breast Clinic
Your visit to the breast clinic may take several hours.
You can take a partner, close friend or relative with you for company or support. Some people prefer to go on their own.
A doctor or specialist nurse will ask you about your symptoms
You may be asked to fill in a short questionnaire including questions about any family history of breast problems and any medication youre taking.
You will have an examination
The doctor or nurse will check the breast tissue on both sides. As part of the examination its usual to examine the lymph nodes under your arm and around your neck.
You may need further tests
These will usually include one or more of the following:
- A mammogram
- A core biopsy of the breast tissue and sometimes lymph nodes
- A fine needle aspiration of the breast tissue and sometimes lymph nodes
How To Make Breast Self

Make it routine. The more you examine your breasts, the more you will learn about them and the easier it will become for you to tell if something has changed. Try to get in the habit of doing a breast self-examination once a month to familiarize yourself with how your breasts normally look and feel. Examine yourself several days after your period ends, when your breasts are least likely to be swollen and tender. If you are no longer having periods, choose a day that’s easy to remember, such as the first or last day of the month.
Get to know your breasts’ different neighborhoods. The upper, outer area near your armpit tends to have the most prominent lumps and bumps. The lower half of your breast can feel like a sandy or pebbly beach. The area under the nipple can feel like a collection of large grains. Another part might feel like a lumpy bowl of oatmeal.
Start a journal where you record the findings of your breast self-exams. This can be like a small map of your breasts, with notes about where you feel lumps or irregularities. Especially in the beginning, this may help you remember, from month to month, what is normal for your breasts. It is not unusual for lumps to appear at certain times of the month, but then disappear, as your body changes with the menstrual cycle .
Learn more about Breastcancer.org’s recommendations on when to begin annual mammograms.
Also Check: Did Anne Hathaway Have Breast Cancer
Why Is The Mortality Rate Of Breast Cancer Higher For Black Women
While Black women and White women get breast cancer at about the same rate, Black women are 40% more likely to die from the disease. There are many factors that contribute to breast cancer disparities, ranging from social determinants to genetics to tumor biology, but one mysterious phenomenon stands out: Black women are twice as likely to have triple-negative breast cancer, a rarer but more aggressive form that does not respond to hormonal treatment, making it difficult to treat.
Whether A Woman Should Be Screened For Breast Cancer And The Screening Test To Use Depends On Certain Factors
Women with risk factors for breast cancer, such as certain changes in the BRCA1 or BRCA2 gene or certain genetic syndromes may be screened at a younger age and more often.
Women who have had radiation treatment to the chest, especially at a young age, may start routine breast cancer screening at an earlier age. The benefits and risks of mammograms and MRIs for these women have not been studied.
Breast cancer screening has not been shown to benefit the following women:
- Elderly women who, if diagnosed with breast cancer through screening, will usually die of other causes. Screening mammograms for those aged 66 to 79 years may find cancer in a very small percentage of women, but most of these cancers are low risk.
- In women with an average risk of developing breast cancer, screening mammography before age 40 has not shown any benefit.
- In women who are not expected to live for a long time and have other diseases or conditions, finding and treating early stage breast cancer may reduce their quality of life without helping them live longer.
You May Like: Is Stage 3 Breast Cancer Curable
Effect On Black Women
Black women are dying from breast cancer at an alarming rate and the following conclusions from the ACS’s Breast Cancer Facts and Figures 20192020 may provide some insight on the crisis at hand:
The lack of diversity in breast cancer research means that some of the recommendations, such as the USPSTF’s breast cancer screening guidelines, are not best practices for Black women. This can be a tough pill for Black women to swallow as they often must overcome medical mistrust and systemic problems.
Mammogram And Breast Ultrasound
If you have symptoms and have been referred to a specialist breast unit by a GP, you’ll probably be invited to have a mammogram, which is an X-ray of your breasts. You may also need an ultrasound scan.
If cancer was detected through the NHS Breast Screening Programme, you may need another mammogram or ultrasound scan.
Your doctor may suggest that you only have a breast ultrasound scan if you’re under the age of 35. This is because younger women have denser breasts, which means a mammogram is not as effective as ultrasound in detecting cancer.
Ultrasound uses high-frequency sound waves to produce an image of the inside of your breasts, showing any lumps or abnormalities.
Your breast specialist may also suggest a breast ultrasound if they need to know whether a lump in your breast is solid or contains liquid.
Find out more about breast screening.
You May Like: Is Breast Cancer Curable
What Women Under 40 Should Be Doing To Detect Breast Cancer
Only weeks after having a clean physical, Trish Gauthier put her hands on her chest after coughing and discovered a lump. She was 37 at the time.
I have no family history … but I knew immediately that it was not right, Gauthier, now 40, told TODAY.
Knowing her body is exactly what led Gauthier to aggressively pursue a diagnosis after discovering her lump. She said her doctor was doubtful, suggesting there was nothing there, but she insisted on getting a mammogram. Once a mammogram confirmed the lump, a subsequent biopsy confirmed that it was cancer.
I remember that day, she said. You always remember diagnosis day.
Gauthier went through a lumpectomy, where doctors discovered the cancer had spread and was at stage 3. She went through five months of chemotherapy, five weeks of radiation and a hysterectomy before entering remission. She has since joined The Breasties, a group for women facing breast cancer or in remission to support one another.
You know your body better than anyone, Gauthier said. If something feels off, investigate it.
Microwave Breast Imaging Methods And Measurement Systems
MI techniques can be grouped as passive and active, and active approaches can be sub-grouped into two major groups: microwave tomographic and radar-based MI. Passive MI uses radiometry to measure the temperature differences between normal and malignant tissues. Active MI measures the dielectric properties contrast between healthy tissue and malignant tissue in the high-MHz to low-GHz regime. Active MI is an emerging mammography technique for diagnosing breast cancer.
Read Also: Chances Of Getting Breast Cancer Twice
Breast Cancer: How To Detect And Prevent It Early
Breast cancer: how to detect and prevent it early? Data from the International Agency for Research on Cancer of the World Health Organization in 2020 show that breast cancer has become the most common cancer in the world and the number one killer that seriously harms womens health.
Early detection and early treatment of breast cancer are very important for patients. With the increasing incidence of breast cancer today, the majority of female friends must pay attention to the prevention of breast cancer in order to detect breast cancer in advance and adopt targeted treatment measures.
How Should I Prepare For The Procedure
PET is usually done on an outpatient basis. Your doctor will give you detailed instructions on how to prepare for your examination. You should wear comfortable, loose-fitting clothes. You should not eat for four hours before the scan. You will be encouraged to drink water. Your doctor will instruct you regarding the use of medications before the test.
Note: Diabetic patients should ask for any specific diet guidelines to control glucose levels during the day of the test.
A nurse or technologist will take you into a special injection room, where the radioactive substance is administered as an intravenous injection . It will then take approximately 30 to 90 minutes for the substance to travel through your body and accumulate in the tissue under study. During this time, you will be asked to rest quietly and avoid significant movement or talking, which may alter the localization of the administered substance. After that time, scanning begins. This may take 30 to 45 minutes.
Some patients, specifically those with heart disease, may undergo a stress test in which PET scans are obtained while they are at rest and again after undergoing the administration of a pharmaceutical to alter the blood flow to the heart.
Usually, there are no restrictions on daily routine after the test, although you should drink plenty of fluids to flush the radioactive substance from your body.
What will I experience during the procedure?
Who interprets the results and how do I get them?
Don’t Miss: Is Breast Cancer Curable In The 3 Stage
Who Should Have A Regular Screening Mammogram
The biggest risk factors for developing breast cancer are being a woman and getting older. BreastScreen Australia targets women aged 50 to 74, as 75% of all breast cancers occur in women over the age of 50.
- Screening mammograms are often less reliable for women under 40 years of age. The density of breast tissue in younger women often makes it difficult to detect cancers on mammograms.
- All women aged 40 to 49 years who have no breast symptoms also have free access to the BreastScreen Australia program should they choose to a have a screening mammogram.
- All women aged 50 to 74 years are encouraged to have a free mammogram every two years through BreastScreen Australia.
- Women aged 75 and over who have no breast symptoms also have free access to the BreastScreen Australia program. They should discuss whether to have a mammogram with their doctor.
When To See Your Gp
See your GP if you have:
- a lump in your breast
- any other worrying symptoms, such as nipple discharge
- a history of breast cancer in members of your family and youâre worried about your chances of getting it
Itâs very unlikely you have cancer, but itâs best to get your symptoms checked. Your GP will examine your breast and can refer you for tests and scans for breast cancer if needed.
If you do not have symptoms but have a clear family history of breast cancer, your GP may refer you to a genetic specialist to discuss your risk of getting it.
There are some inherited genes that increase your risk of cancer and a blood test can be done to check for these. Read about testing for cancer risk genes.
You May Like: Can You Get Rid Of Breast Cancer
How To Do A Breast Self Exam
This article was co-authored by Carrie Noriega, MD. Dr. Noriega is a Board Certified Obstetrician & Gynecologist and medical writer in Colorado. She specializes in womens health, rheumatology, pulmonology, infectious disease, and gastroenterology. She received her MD from the Creighton School of Medicine in Omaha, Nebraska and completed her residency at the University of Missouri – Kansas City in 2005.There are 10 references cited in this article, which can be found at the bottom of the page. This article has been viewed 201,827 times.
Breast self-exams are an optional screening tool to check for early signs of breast cancer. Performing these exams monthly can help you familiarize yourself with the look and feel of your breasts so that you can more easily detect changes.XResearch source Though breast self-exams were once thought to be essential to screening for breast cancer, they are now considered a helpful, optional tool.
How To Detect Breast Cancer In Early Stage
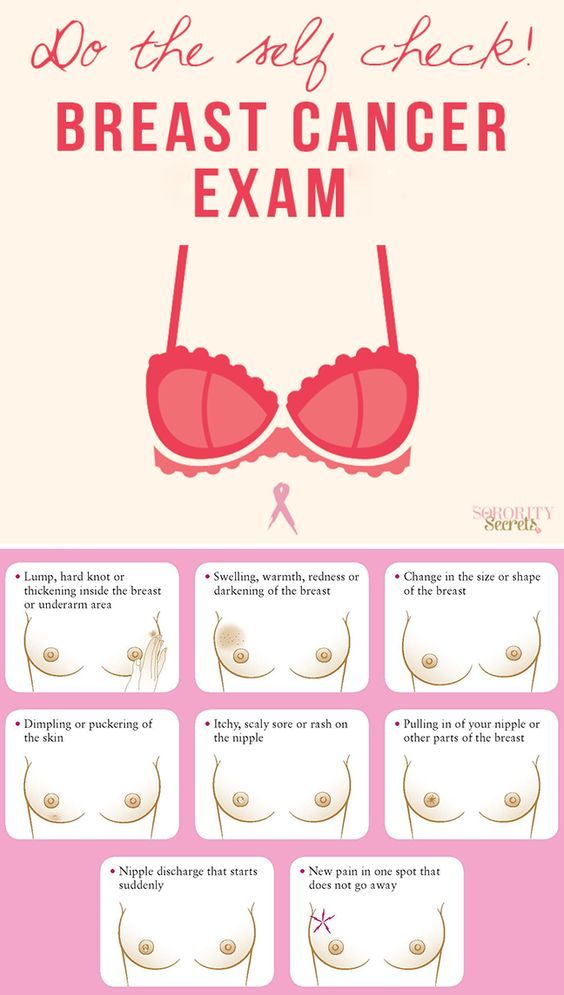
From person to person warning signs and symptoms can vary greatly, but there are some common signs they are:
- Swelling of all or part of a breast.
- Lump inside the breast or underarm area.
- Skin irritation or dimpling.
- Change in breast size and shape.
- Nipple pain or breast pain.
- Sore or rash on the nipple.
- Swelling, redness or darkening of the breast.
- Prominent veins on the surface of the breast.
- Nipple discharge that starts suddenly.
- Pulling in of the nipple or the other parts of the breast.
If these signs or symptoms do occur, it does not necessarily mean that cancer is present. It can often the result of benign breast conditions. Benign means it is not cancer and changes in the breast can be caused because of the factors like puberty, pregnancy, and menopause.
You May Like: Did Anne Hathaway Have Breast Cancer
Inflammatory Breast Cancer Symptoms
Unlike other breast cancers, inflammatory breast cancer rarely causes breast lumps and may not appear on a mammogram. Inflammatory breast cancer symptoms include:
- Red, swollen, itchy breast that is tender to the touch
- The surface of the breast may take on a ridged or pitted appearance, similar to an orange peel
- Heaviness, burning, or aching in one breast
- One breast is visibly larger than the other
- Inverted nipple
- No mass is felt with a breast self-exam
- Swollen lymph nodes under the arm and/or above the collarbone
- Symptoms unresolved after a course of antibiotics
Unlike other breast cancers, inflammatory breast cancer usually does not cause a distinct lump in the breast. Therefore, a breast self-exam, clinical breast exam, or even a mammogram may not detect inflammatory breast cancer. Ultrasounds may also miss inflammatory breast cancer. However, the changes to the surface of the breast caused by inflammatory breast cancer can be seen with the naked eye.
Symptoms of inflammatory breast cancer can develop rapidly, and the disease can progress quickly. Any sudden changes in the texture or appearance of the breast should be reported to your doctor immediately.
For women who are pregnant or breast-feeding, redness, swelling, itchiness and soreness are often signs of a breast infection such as mastitis, which is treatable with antibiotics. If you are not pregnant or nursing and you develop these symptoms, your doctor should test for inflammatory breast cancer.