Benefits Of Extending Therapy
One popular option is to change from tamoxifen to an aromatase inhibitor when menopause is reached . Read more about aromatase inhibitors in our article on post-menopausal early stage breast cancer.
Extending tamoxifen for an additional 5 years can also decrease a womans chances of breast cancer recurrence by about 4% in the 10 years after surgery if her cancer had spread to her lymph nodes prior to surgery. However, women who had early-stage breast cancer that did not spread to their lymph nodes did not benefit from more than 5 years of tamoxifen.
In addition to reducing recurrence, the studies also found that taking tamoxifen for 10 years instead of 5 years reduced the chances of dying from breast cancer within those 10 years from about 15% to about 12%. These differences are small and disappear for women with the earliest stage breast cancers. Even more important, overall survival how long a woman lives after her initial diagnosis of breast cancerwas not significantly affected by taking tamoxifen for more than 5 years. In other words, even if a woman taking tamoxifen for 10 years was less likely to die of breast cancer within those 10 years, she was not less likely to die from any cause.
Hormonal Therapies Slow Or Stop Breast Cancers Growth By Changing The Hormonal Milieu
For early stage cancer, these treatments include tamoxifen and a class of drugs called aromatase inhibitors . Three aromatase blocking drugs are available clinically. Anastrozole and letrozole work by reversibly blocking this enzyme, while exemestane binds to the enzyme and inactivates it permanently. Studies suggest that all three are equally effective. Women with metastatic breast cancer also have other hormone therapy options, including fulvesrant , megestrol acetate , and tormifene .
Hormone Therapy Drugs For Metastatic Breast Cancer
Some hormone therapy drugs are pills and some are given by injection under the skin .
|
Figure 5.8: Hormone therapies for metastatic breast cancer |
||
|
Drug |
Used in pre- or postmenopausal women? |
Injection or pill? |
|
Postmenopausal |
Pill |
To learn more about a specific hormone therapy, visit the National Institutes of Healths Medline Plus website.
Recommended Reading: Is Stage 4 Breast Cancer Survivable
How Is Hormone Therapy Given
Hormone therapy is most often used to treat breast and prostate cancers. Research is being done to see if hormonal therapy could be used to treat other cancer types. Hormone therapy can be given in a few ways:
- Oral medication Taken by mouth.
- Injection Given by an injection under the skin or in the muscle .
- Surgical intervention Removal of the ovaries in women, or testicles in men, causes lower levels of hormones being made.
Hormone therapy is a “systemic” therapy, meaning that it travels throughout the body. Surgery and radiation therapy are “local” treatments.
What Should Women Do If They Have Menopausal Symptoms But Are Concerned About Taking Mht
Women who are seeking relief from hot flashes and vaginal dryness should talk with their health care provider about whether to take MHT, the possible risks of using MHT, and what alternatives may be appropriate for them. FDA currently advises women to use MHT for the shortest time and at the lowest dose possible to control menopausal symptoms. The FDA provides additional information about the risks and benefits of MHT use for menopausal symptoms on its Menopause & Hormones: Common Questions fact sheet.
Also Check: How Long Does Breast Cancer Last
Symptom Burden And Quality
In order to appreciate the relative toxicities observed in SOFT/TEXT, it is important to consider the safety profiles of single agent tamoxifen and AI. Common adverse effects of endocrine therapies can be divided into 1) symptoms that are bothersome but impact QOL and compliance and 2) serious toxicities that can impact morbidity and mortality but do not necessarily cause symptoms. It is important to recognize and attempt to treat the bothersome symptoms, as early discontinuation of these medications is common, is often attributed to adverse effects, and likely leads to worse outcomes3537.
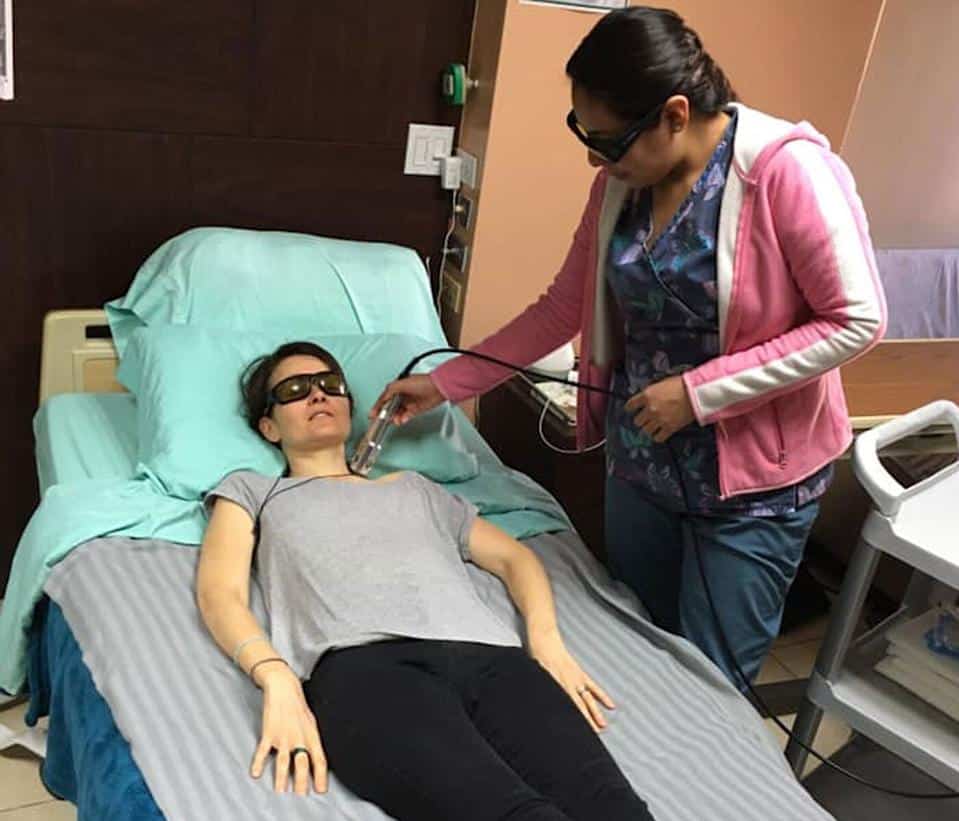
Treatments For Vaginal Dryness
Vaginal dryness and discomfort can be bothersome menopausal symptoms for some women.
Devices that use lasers or other forms of energy to ‘rejuvenate’ vaginal tissue are now being studied as well, although it’s not yet clear how helpful they might be. It’s important to discuss the possible risks and benefits of these treatments with your doctor before deciding if one is right for you.
Also Check: Care Strategies For Breast Cancer
Treatment Side Effects And Complications
Menopause-like symptoms can be difficult for young women being treated for breast cancer. Rather than the gradual onset of natural menopause, hot flashes and other symptoms tend to come on quickly and harshly soon after treatment starts.
Sexual side effects are common with lower estrogen levels, and these can be particularly bothersome for young women as well.
Breast Cancer Doctor Discussion Guide
Get our printable guide for your next doctor’s appointment to help you ask the right questions.
Which Patients Benefit From The Inclusion Of Ovarian Function Suppression As Part Of The Adjuvant Endocrine Therapy Regimen
Given the added toxicity and relatively modest benefit in distant DFS,7,21 subset analyses are being used to determine which patients benefit most from the addition of ovarian function suppression to endocrine therapy. In the SOFT trial,7,21 patients who received chemotherapy were noted to have improved DFS with ovarian function suppression with either tamoxifen or exemestane compared with tamoxifen alone. This difference was especially notable in the small number of patients younger than 35 years of age, where the rate of freedom from breast cancer differed markedly for tamoxifen alone versus tamoxifen plus ovarian function suppression versus exemestane plus ovarian function suppression .
Moreover, in the planned subset analysis of SOFT/TEXT trials for patients receiving adjuvant chemotherapy, there was evidence of benefit for tamoxifen plus ovarian function suppression versus tamoxifen alone in terms of reduction of breast cancer recurrences at 5 years , with a further improvement among those receiving exemestane plus ovarian function suppression .21 However, the receipt of chemotherapy among patients was high , especially among younger women.
Recommended Reading: Where To Check For Breast Cancer Lumps
Are There Alternatives For Women Who Choose Not To Take Menopausal Hormone Therapy
Women who are concerned about the changes that occur naturally with the decline in hormone production that occurs during menopause can make changes in their lifestyle and diet to reduce the risk of certain health effects. For example, eating foods that are rich in calcium and vitamin D or taking dietary supplements containing these nutrients may help to prevent osteoporosis. FDA-approved drugs such as alendronate , raloxifene , and risedronate have been shown in randomized trials to prevent bone loss.
Medications approved by the FDA for treating depression and seizures may help to relieve menopausal symptoms such as hot flashes . Drugs that have been shown in randomized clinical trials to be effective in treating hot flashes include venlafaxine , desvenlafaxine , paroxetine , fluoxetine , citalopram , gabapentin , and pregabalin.
Side Effects Of Tamoxifen And Toremifene
The most common side effects of tamoxifen and toremifene are:
- Vaginal dryness or discharge
- Changes in the menstrual cycle
When tamoxifen treatment starts, a small number of women with cancer that has spread to the bones might have a tumor flare which can cause bone pain. This usually decreases quickly, but in some rare cases a woman may also develop a high calcium level in the blood that is hard to control. If this happens, the treatment may need to be stopped for a time.
Rare, but more serious side effects are also possible:
Recommended Reading: What Do Breast Cancer Patients Need
Preventing Breast Cancer In The Opposite Breast
About 1 in 20 women diagnosed with breast cancer will develop breast cancer in the opposite breast within the 10 years after first breast cancer diagnosis. A 2017 study in the prestigious medical journal JAMA found that taking tamoxifen can reduce the percentage of those women from developing cancer in the opposite breast within 10 years, from about 5% to 2%. Unfortunately, the study authors did not report on breast cancer deaths or deaths for any other reason. Therefore, we do not know whether tamoxifens reduction of cancer in the opposite breast had any impact on the womens longevity.
What Are Hormones And How Are They Used As Therapy
Hormones are chemicals that are made by the organs of the body’s endocrine system . These chemicals move through the body in the bloodstream. They help each organ do its job. Hormones regulate almost every cell in the body. Some examples of hormones are estrogen, testosterone, insulin, thyroid hormone, cortisol, and epinephrine.
Some cancers need hormones in order to grow. Blocking the action of these hormones might stop the cancer from growing. There are a few ways this happens:
- Block the hormones from acting: Cells have “receptors” on their surface that certain hormones connect to and trigger activity inside the cells. By blocking the receptor, the hormone is not able to connect to its receptor.If the hormone’s normal spot on the cell is already taken, the hormone cannot attach to and activate the cell.
- Prevent the body from making the hormone: This can be done with medication to block the production of the hormone, or with surgery to remove the organ that makes it. For example, removing the ovaries decreases the amount of estrogen being made.
- Remove the hormone receptors on cells or change their shape: The hormone then cannot attach itself to the cell receptor to activate it, making the hormone unable to work.
Also Check: Does Beer Cause Breast Cancer
Risk Of Late Relapse In Hr+ Breast Cancer
The risk of relapse in breast cancer varies over time and is dependent on a number of prognostic features including stage, histopathology, and HR status. Distinct from HR-negative breast cancer that typically has the highest relapse rates early after diagnosis, HR+ breast cancer has a unique predilection for late relapses23. Based on Surveillance, Epidemiology, and End Results data, HR+ breast cancer has an estimated annual hazard rate for relapse of approximately 12% that plateaus and persists through years 101524.
Hormone Therapy For Breast Cancer Pros And Cons
One main use of hormone therapy is, it lowers the risk of breast cancer reappearance in persons suffering from early-stage hormone-sensitive breast cancers. It can even effectively lower the risk of metastatic breast cancer growth and development in people with hormone-sensitive tumors.
Coming to the side effects of breast cancer hormone therapy, it depends on the medication type and as such varies.
SERMs
Tamoxifen and other SERMs can lead to
- Vaginal discharge
- Vaginal dryness
These medications may even increase the risk of endometrial cancer and blood clots. In a few cases, tamoxifen can lead to stroke and can enhance the risks of a heart attack.
Side effects for AIs consist of
- Joint stiffness
On the whole keeping in view, the hormone therapy for breast cancer pros and cons Hormone therapy is a good treatment option and the need for refusing hormone therapy for breast cancer is very less.
Sudheendra is a passionate blogger for 8 years and holds a Degree in Journalism & Mass Communications. His writings particularly focus on health, medicine, diet & lifestyle. For him, everything that interlinks and relates to health & medical world entices him. His write-ups aim at educating people not by just giving facts but by infusing human touch.
You May Like: How Can You Avoid Breast Cancer
Hormone Therapy For Breast Cancer
Some types of breast cancer are affected by hormones, like estrogen and progesterone. The breast cancer cells have receptors that attach to estrogen and progesterone, which helps them grow. Treatments that stop these hormones from attaching to these receptors are called hormone or endocrine therapy.
Hormone therapy can reach cancer cells almost anywhere in the body and not just in the breast. It’s recommended for women with tumors that are hormone receptor-positive. It does not help women whose tumors don’t have hormone receptors .
Menopausal Status And Chemotherapy
Menopause has been broadly defined as age > 60, having undergone bilateral oophorectomy , or having amenorrhea for at least 12 months in the absence of factors potentially influencing menstruation 13. Confirming menopausal status can pose a challenge in women either who have undergone hysterectomy without BSO or who develop chemotherapy-induced ovarian failure . Women under age 60 with HR+ breast cancer who have undergone hysterectomy without BSO and who will be receiving chemotherapy should have ovarian function assessed prior to chemotherapy initiation in order to determine pre-chemotherapy menopausal status. This information helps inform choice of endocrine therapy and potential need for monitoring of ovarian function.
Women with CIOF can experience reactivation of ovarian function during AI therapy despite having estradiol concentrations in the postmenopausal range at the time of AI initiation14,15. Importantly, estradiol levels can increase even though menses do not resume. Notably, younger age at the time of chemotherapy is independently associated with a higher chance of ovarian function recovery following AI therapy, and no upper age limit has yet been identified15.
Read Also: Is The Lump In My Breast Cancer
Overall Survival And The Role Of Soft/text In The Contemporary Era
In the SOFT and TEXT trials, no improvement in overall survival was seen with the addition of OS. However, given the few events observed in this cohort, the overall excellent prognosis , and the long natural history of HR+ breast cancer, the absence of an overall survival difference is likely due to insufficient follow up and long-term results are eagerly awaited. The worse overall survival with AI plus OS in ABCSG-12 has not yet been replicated in SOFT/TEXT follow-up is ongoing.
How Is Hormone Therapy Used To Treat Breast Cancer
There are three main ways that hormone therapy is used to treat hormone-sensitive breast cancer:
Adjuvant therapy for early-stage breast cancer:Tamoxifen is FDA approved for adjuvant hormone treatment of premenopausal and postmenopausal women with ER-positive early-stage breast cancer, and the aromatase inhibitorsanastrozole, letrozole, and exemestane are approved for this use in postmenopausal women.
Research has shown that women who receive at least 5 years of adjuvant therapy with tamoxifen after having surgery for early-stage ER-positive breast cancer have reduced risks of breast cancer recurrence, including a new breast cancer in the other breast, and reduced risk of death at 15 years .
Until recently, most women who received adjuvant hormone therapy to reduce the chance of a breast cancer recurrence took tamoxifen every day for 5 years. However, with the introduction of newer hormone therapies , some of which have been compared with tamoxifen in clinical trials, additional approaches to hormone therapy have become common .
Some premenopausal women with early-stage ER-positive breast cancer may have ovarian suppression plus an aromatase inhibitor, which was found to have higher rates of freedom from recurrence than ovarian suppression plus tamoxifen or tamoxifen alone .
Men with early-stage ER-positive breast cancer who receive adjuvant therapy are usually treated first with tamoxifen. Those treated with an aromatase inhibitor usually also take a GnRH agonist.
Read Also: Will Blood Work Show Breast Cancer
Randomized Trials Exploring Benefit Of Ovarian Suppression Alone
Although early trials showed a clear benefit1 for the use of ovarian suppression as a treatment for breast cancer, the use of purely ovarian suppressive strategies declined with the widespread use of chemotherapy. With the publication of the meta-analysis which demonstrated that, for premenopausal women, there was a clear benefit of OA/OS as compared to no adjuvant therapy, there was a resurgence of interest in this strategy.11 The Early Breast Cancer Trialists Collaborative Group published a meta-analysis which examined the previous smaller trials evaluating the benefits of ovarian ablative therapy in 1995.12 The meta-analysis included eight trials encompassing 3456 women who were less than 50 years of age and did not receive chemotherapy. There was a clear benefit of ovary-targeted therapy, demonstrating a relative reduction of 25% in recurrence and 24% in mortality as compared to no treatment. This was seen despite lack of knowledge regarding the tumor estrogen receptor status in two-thirds of the trials examined and was not affected by nodal status. In the most recent EBCTCG update, similar benefits were seen in the < 40 year old age group as well as the 40â49 year old group . There were similar benefits for OS therapy with GHRH agonists and OA approaches with oophorectomy or ovarian radiation.13
Hormones And Postmenopausal Breast Cancer
Despite the negative results of the WHI study, the relationship between hormones, breast cancer, and other health indicators is far from conclusive. Prior to the use of tamoxifen, estrogen therapy was actually the standard for the treatment of breast cancer . Early comparisons of estrogen vs. tamoxifen treatment revealed that the synthetic estrogen DES provided as much protection as tamoxifen treatment . In addition, more recent analyses of the Womens Health Initiative data have shown that in hysterectomized women, estrogen replacement therapy alone actually seemed to decrease the incidence and mortality rate of breast cancer 70075-X/abstract” rel=”nofollow”> Anderson et al., 2012).
Due to the confusion related to hormone therapy and breast cancer, meta-analyses of multiple studies have been conducted. In 2006, such an analysis indicated that hormone replacement therapy taken after breast cancer was related to a decreased risk of breast cancer deaths . Creasman reviewed studies on hormone replacement therapy after cancer, finding that case-control and cohort studies found no risk or even less risk of recurrence of breast cancer in women taking estrogen therapy. He concluded that hormone therapy has little if any risk to women who have had breast cancer.
Recommended Reading: Celebrities With Breast Cancer 2021