The Effects Of Serms And Serds On The Tumor Immune Microenvironment
SERMs and SERDs are currently the most important endocrine therapeutic regimens for BC. SERMs, represented by tamoxifen, toremifene and raloxifene, work through competitive blockage of the interaction between estrogen and ER. SERDs, such as fulvestrant, contribute to the downregulation and degradation of ER . Accumulating evidence from experimental and clinical studies has revealed the multifaceted immunomodulatory effects of SERMs and SERDs in particular, progress has been made to elaborate how SERMs and SERDs act upon the immune microenvironment of BC .
Table 1 The effects of different endocrine therapeutic strategies on immune cells
In addition to being effective for treating BC, tamoxifen and raloxifene have also been shown to reduce the risk of BC in highly susceptible women . Tamoxifen administration was found to upregulate IFN-related genes in normal human mammary epithelial cells from in vitro experiments, implying its positive effect on the immune surveillance of normal breast tissue . Moreover, tamoxifen and toremifene were also found to enhance TNF-R2 expression on activated T cells by inhibiting the activation of JNK and promoting TNF-R2-mediated T cell proliferation . These results might explain their BC-preventive effect.
E Combination Of Cdk4/6 With Immune Checkpoint Inhibitors
CDK4/6 inhibitors act as cell cycle checkpoint inhibitors and induce cell cycle arrest, senescence and immunogenicity in the TME. Studies have demonstrated an enhancement in the anti-tumor response upon treatment with CDK4/6 inhibitors due to an enhancement in interferon production, reduced T-regs and enhanced T cell activation . Addition of immune checkpoint inhibitors to CDK4/6 inhibitors holds promise by inhibiting the growth and proliferation of cancerous cells and, with this study as the background, a clinical trial has focused on studying the suitability and efficacy of using abemaciclib in combination with pembrolizumab in HR+/HER-2 negative metastatic BC patients . Another study is recruiting to study the response of fulvestrant and pembrolizumab as a combination therapy in HR+/HER-2 negative advanced or metastatic BC patients.
What Types Of Hormone Therapy Are Used For Breast Cancer
Several strategies are used to treat hormone-sensitive breast cancer:
Blocking ovarian function: Because the ovaries are the main source of estrogen in premenopausal women, estrogen levels in these women can be reduced by eliminating or suppressing ovarian function. Blocking ovarian function is called ovarian ablation.
Ovarian ablation can be done surgically in an operation to remove the ovaries or by treatment with radiation. This type of ovarian ablation is usually permanent.
Alternatively, ovarian function can be suppressed temporarily by treatment with drugs called gonadotropin-releasing hormone agonists, which are also known as luteinizing hormone-releasing hormone agonists. By mimicking GnRH, these medicines interfere with signals that stimulate the ovaries to produce estrogen.
Estrogen and progesterone production in premenopausal women. Drawing shows that in premenopausal women, estrogen and progesterone production by the ovaries is regulated by luteinizing hormone and luteinizing hormone-releasing hormone . The hypothalamus releases LHRH, which then causes the pituitary gland to make and secrete LH and follicle-stimulating hormone . LH and FSH cause the ovaries to make estrogen and progesterone, which act on the endometrium .
Examples of ovarian suppression drugs that have been approved by the U.S. Food and Drug Administration are goserelin and leuprolide .
Read Also: What Is The Probability Of Getting Breast Cancer
If Cancer Has Come Back Or Spread
Hormone therapy can be used to treat breast cancer that has come back or that has spread to another part of the body .
Its given either alone or with other treatments, depending on what treatments you had before.
If your breast cancer came back during or after treatment with hormone therapy, you may be offered a different type of hormone therapy.
Can Hormone Therapy Be Used To Prevent Breast Cancer

Yes. Most breast cancers are ER positive, and clinical trials have tested whether hormone therapy can be used to prevent breast cancer in women who are at increased risk of developing the disease.
A large NCI-sponsored randomized clinical trial called the Breast Cancer Prevention Trial found that tamoxifen, taken for 5 years, reduces the risk of developing invasive breast cancer by about 50% in postmenopausal women who were at increased risk . Long-term follow-up of another randomized trial, the International Breast Cancer Intervention Study I, found that 5 years of tamoxifen treatment reduces the incidence of breast cancer for at least 20 years . A subsequent large randomized trial, the Study of Tamoxifen and Raloxifene, which was also sponsored by NCI, found that 5 years of raloxifene reduces breast cancer risk in such women by about 38% .
As a result of these trials, both tamoxifen and raloxifene have been approved by the FDA to reduce the risk of developing breast cancer in women at high risk of the disease. Tamoxifen is approved for this use regardless of menopausal status. Raloxifene is approved for use only in postmenopausal women.
Also Check: Does Breast Cancer Make You Gain Weight
How To Choose The Best Kind Of Hormone Therapy
There are many hormone therapy types to cure breast cancer such as
Selective Estrogen Receptor Modulators
Even known as SERMs, these medications obstruct breast cancer cells from getting attached to estrogen. SERMs impede the effects of estrogen merely in breast tissue but not in other tissues within the body.
These drugs are traditionally only used in premenopausal women.
The commonly used SERMs consist
Tamoxifen
This medication stops estrogen from attaching to cells and thereby disables cancer from growing and dividing. People who have tamoxifen for a decade after breast cancer treatment are less supposed to see the cancer recurrence and more supposed to live longer in comparison to the ones who take the medicine for just 5 years.
Toremifene
This medication is approved only to cure breast cancer that has extended to other body parts and might not be useful in persons who have seen less success with tamoxifen.
Fulvestrant
This is an injected estrogen receptor-blocking medication that is usually used to cure advanced breast cancers. Different from other SERMs, it obstructs the effect of estrogen all through the total body.
Aromatase Inhibitors
AIs obstruct estrogen production from fat tissue, however, have no consequence on the estrogen made by the ovaries.
Common AIs consist
- Exemestane
Ovarian Ablation or Suppression
Surgical ablation is carried on by the removal of ovaries. Without the manufacturing of estrogen from the ovaries, one will move into permanent menopause.
The Effects Of Estrogen On The Immune System
Estrogen, an aromatized steroid hormone produced mainly in gonads and extraglandular tissues, participates in a wide range of physiological processes through the ER signaling pathway. Although the production of estrogen by ovaries ceases among postmenopausal women, estrogen is continually generated by the adipose tissue , of which both normal and tumor-bearing breasts are enriched. It has been estimated that the level of estradiol in breast tumor is 50100 fold higher than that in normal breast tissue or in circulation, indicating an in situ synthesis capacity of breast tumor cells . Indeed, acquired CYP19A1 amplification in BC cells has been found in 21.5% of relapsed AI-treated patients, and this alteration causes autonomous estrogen biosynthesis that activates ER . Moreover, the extensive expression of ER/ in immune cells further supports the abnormal regulatory action of estrogen on immune system elements involving their development and functional responses .
For a detailed description, please also read a review written by Segovia-Mendoza et al. on the immune modulatory effect of estrogen in different immune cells. To summarize as illustrated in Fig. , estrogen acts as an immune-suppressive factor in favor of tumor emergence and progression. As such, along with its direct killing effect on cancer cells, anti-estrogen therapy may orchestrate an antitumor/pro-immune surveillance TIM in BC.
Fig. 1
Recommended Reading: How Likely Is Breast Cancer
A New Generation Of Oral Serd: Elacestrant
Elacestrant is a new generation of selective estrogen receptor degrading agent, administered orally once a day.
This study included 57 patients with ER-positive, HER2-negative, postmenopausal metastatic breast cancer who failed multi-line treatment from 11 hospitals in the United States.
The results of the study show that: for such patients, the safety of oral Elacestrant once a day is tolerable , and the single agent has anti-cancer activity And achieve partial relief.
The objective response rate of Elacestrant was 19.4%, 15% in patients who had previously received SERD treatment , 16.7% in patients who had received CDK4/6i treatment , and ESR1 mutations ) Among patients, it was 33.3%.
The overall clinical benefit rate of Elacestrant was 42.6%, 56.5% in patients with ESR1 mutations, and 30.4% in patients who had previously received CDK4/6i treatment.
In addition, a phase III clinical trial comparing the efficacy of Elacestrant with standard endocrine therapy is underway and is worth looking forward to.
Experts remind: a new generation of oral SERD is of great significance to patients with metastatic ER-positive breast cancer, especially those who are resistant to endocrine therapy.
At present, in addition to Elacestrant, there are several oral SERDs under development, including: Giredestrant , SAR439859, AZD9833.
Looking forward to more new therapies coming out, bringing new treatment options for this type of breast cancer patients.
Who Gets Hormone Therapy For Breast Cancer
When youâre diagnosed with breast cancer, your doctor will test cells from your tumor to see if they have parts on their surfaces called receptors that use estrogen or progesterone. If they do, it means that they depend on these hormones to grow. In that case, your doctor will probably recommend hormone therapy as part of your treatment plan.
If youâve already been treated for breast cancer, you might use hormone therapy to help keep it from coming back. It also helps lower your odds of getting new cancers in the other breast.
Also, if you don’t have the disease but have a family history of it, or genes that raise your risk, your doctor may recommend hormone therapy to lower your chances of getting it.
You May Like: What To Wear During Radiation Treatment For Breast Cancer
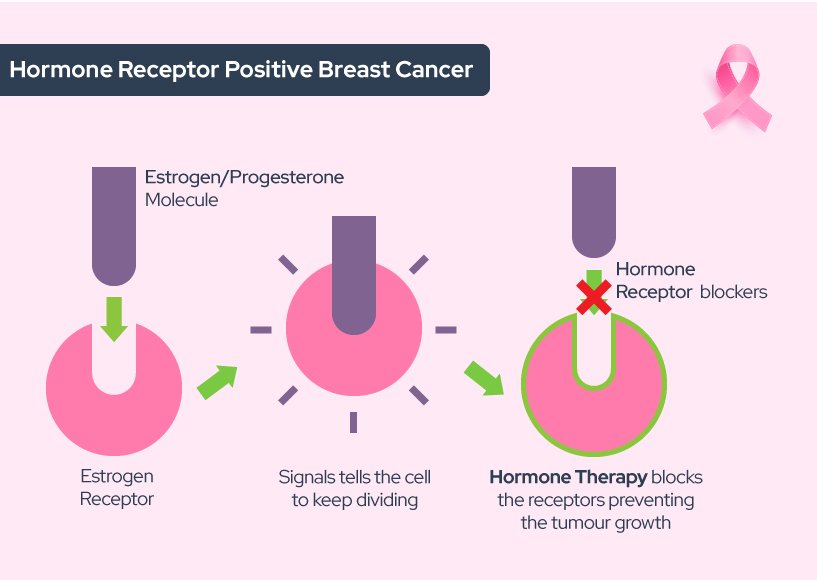
Estrogen Receptor Blockers Estrogen Receptor Blocker Drugs Attach Directly To And Block The Estrogen Receptors On Cancer Cells So That The Cancer Cells Cant Use Estrogen They Do Not Affect The Level Of Estrogen In The Body Estrogen Receptor Blockers Are Also Called Selective Estrogen Receptor Modulators
Tamoxifen
Tamoxifen is the most commonly used anti-estrogen drug. It is used in post-menopausal and premenopausal women. Tamoxifen is given by mouth as a pill.
Tamoxifen is the hormonal therapy drug used most often to lower the risk that DCIS or LCIS will lead to an invasive breast cancer.
Tamoxifen very slightly increases the risk for uterine cancer, deep vein thrombosis and stroke. Doctors will carefully weigh these risks against the benefits of giving this drug before they offer it to women who have a personal or a strong family history of these conditions. Usually the benefits of taking tamoxifen outweigh these risks.
Fulvestrant
Fulvestrant is an anti-estrogen drug that reduces the number of estrogen receptors on breast cancer cells. It is given as an injection into the muscles of the buttocks.
Fulvestrant is used in post-menopausal women if the breast cancer has grown after they were treated with tamoxifen. It is also used in postmenopausal women with locally advanced or metastatic breast cancer that have never been treated with hormonal therapy.
Other Factors And Proteins
There are several other transcription factors and proteins that determine cancer progression in the face of ongoing endocrine therapies, some known and many unknown. The EMT factors, Twist and Snail, have been implicated in endocrine resistance, with Twist downregulating ER by epigenetically regulating the promoter of ER . There are several other proteins and molecules that play a major role in endocrine resistance, including the NOTCH and WNT pathways described earlier. All these proteins and transcription factors function as individual molecules working together for/against the homeostasis of the human cells, to determine the fate of cancer cells.
Metabolic and oxidative stress are a few of the other factors affecting endocrine resistance. The mechanisms are elucidated in detail below for each of these factors. Recent publications have demonstrated that homeostasis in cell metabolism and cell proliferation is mediated by a few other transcription factors and pathways as well. Another mechanism for endocrine resistance that has been suggested relates to the ability of the metabolic enzymes to deliver the active compound. Some studies have reported lower concentrations of BC drugs at the site of the tumor when compared to levels in the plasma and an association with poor outcomes . Alternatively, a recent study demonstrated that an elevated concentration of tamoxifen metabolites at the site of the cancer, led to agonist effects .
Also Check: How Likely Am I To Get Breast Cancer
Can Other Drugs Interfere With Hormone Therapy
Certain drugs, including several commonly prescribed antidepressants , inhibit an enzyme called CYP2D6. This enzyme plays a critical role in the body’s use of tamoxifen because CYP2D6 metabolizes, or breaks down, tamoxifen into molecules, or metabolites, that are much more active than tamoxifen itself.
The possibility that SSRIs might, by inhibiting CYP2D6, slow the metabolism of tamoxifen and reduce its effectiveness is a concern given that as many as one-fourth of breast cancer patients experience clinical depression and may be treated with SSRIs. In addition, SSRIs are sometimes used to treat hot flashes caused by hormone therapy.
Many experts suggest that patients who are taking antidepressants along with tamoxifen should discuss treatment options with their doctors, such as switching from an SSRI that is a potent inhibitor of CYP2D6, such as paroxetine hydrochloride , to one that is a weaker inhibitor, such as sertraline or citalopram , or to an antidepressant that does not inhibit CYP2D6, such as venlafaxine . Or doctors may suggest that their postmenopausal patients take an aromatase inhibitor instead of tamoxifen.
Other medications that inhibit CYP2D6 include the following:
- Quinidine, which is used to treat abnormal heart rhythms
Acupuncture Against The Heat
Numerous menopausal symptoms can be alleviated by certain medications and herbal substances or by acupuncture and yoga. It is best to ask your doctor and/or a naturopath or homeopath. Systemic hormone replacement therapy is strongly discouraged.
Women can breathe easy. Acupuncture provides relief from hot flashes for breast cancer patients treated with tamoxifen after an estrogen brake. Acupuncture has two advantages over other hot flash treatments: it is affordable and does not cause harmful side effects.
These research results were presented at the 6th European Breast Cancer Congress in Berlin . The Norwegian physiotherapist and acupuncturist at Vestfold Central Hospital said at a press conference that hot flashes could be halved in women with breast cancer treated with traditional Chinese acupuncture. This effect applied both during the day and at night and persisted even after the end of acupuncture.
You May Like: Is There Financial Help For Breast Cancer Patients
Medications That Stop The Body From Making Estrogen After Menopause
Aromatase inhibitors are a class of medicines that reduce the amount of estrogen in your body, depriving breast cancer cells of the hormones they need to grow.
Aromatase inhibitors are only used in women who have undergone menopause. They cannot be used unless your body is in natural menopause or in menopause induced by medications or removal of the ovaries.
Aromatase inhibitors used to treat breast cancer include:
- Anastrozole . Anastrozole is used to reduce the risk of cancer recurrence in women who have been treated for early-stage breast cancer. It can also be used to treat advanced breast cancer.
- Exemestane . Exemestane is used to reduce the risk of cancer recurrence in women who have been treated for early-stage breast cancer. It’s sometimes used after taking tamoxifen for two or three years. It can also be used to treat advanced breast cancer in women for whom tamoxifen is no longer working.
- Letrozole . Letrozole is used to reduce the risk of cancer recurrence in women who have been treated for early-stage breast cancer. It can be used alone or given after completing tamoxifen treatment. Letrozole is also used to treat advanced breast cancer.
Aromatase inhibitors are given as pills you take once a day. All three aromatase inhibitors work the same and reduce the production of estrogen in your body.
The Effects Of Inhibiting Pi3k
PI3K-AKT-mTOR signaling is the most common aberrantly activated pathway in ER+BC, and this aberrant signaling has been acknowledged as the main cause of endocrine resistance . Various targeted drugs for inhibiting this pathway have been developed to reverse endocrine resistance and have shown promising results . In addition to staving tumor growth, inhibitors of this pathway also impact the functions of multiple immune cells . Therefore, the effects of these therapeutic strategies on the TIM deserve attention.
Fig. 3
Also Check: Can Breast Cancer Make You Nauseous
Endocrine Resistance In Hormone Receptor Positive Breast Cancerfrom Mechanism To Therapy
- 1School of Life Sciences, University of Westminster, London, United Kingdom
- 2Department of Surgery and Cancer, Imperial College London, London, United Kingdom
- 3Department of Biochemistry and Biomedicine, School of Life Sciences, University of Sussex, Brighton, United Kingdom
The importance and role of the estrogen receptor pathway has been well-documented in both breast cancer development and progression. The treatment of choice in women with metastatic breast cancer is classically divided into a variety of endocrine therapies, 3 of the most common being: selective estrogen receptor modulators , aromatase inhibitors and selective estrogen receptor down-regulators . In a proportion of patients, resistance develops to endocrine therapy due to a sophisticated and at times redundant interference, at the molecular level between the ER and growth factor. The progression to endocrine resistance is considered to be a gradual, step-wise process. Several mechanisms have been proposed but thus far none of them can be defined as the complete explanation behind the phenomenon of endocrine resistance. Although multiple cellular, molecular and immune mechanisms have been and are being extensively studied, their individual roles are often poorly understood. In this review, we summarize current progress in our understanding of ER biology and the molecular mechanisms that predispose and determine endocrine resistance in breast cancer patients.